Vertex/non-vertex presentation of twin pregnancies accounts for approximately 34.8% of twins (Chasen et al., Reference Chasen, Spiro, Kalish and Chervenak2005). The general consensus is that a trial of labor with the goal of vaginal delivery of vertex/vertex twins is appropriate at any gestational age (Cruikshank, Reference Cruikshank2007). Vaginal delivery of a non-vertex presenting twin is not recommended (Dodd & Crowther, Reference Dodd and Crowther2005). However, the optimal delivery route for vertex/non-vertex twins is controversial. Options for delivery of vertex/non-vertex twins include cesarean delivery of both twins, vaginal delivery with breech extraction of the second twin, and vaginal delivery with cephalic version of the second twin.
Several reports attest to the safety of vaginal delivery of second non-vertex twins who weigh more than 1,500 g (Blickstein et al., Reference Blickstein, Schwartz-Shoham, Lancet and Borenstein1987; Chervenak et al., Reference Chervenak, Johnson, Youcha, Hobbins and Berkowitz1985; Gocke et al., Reference Gocke, Nageotte, Garite, Towers and Dorcester1989). It was reported that vaginal delivery of the presenting twin followed by breech extraction of the second twin resulted in significantly shorter maternal and neonatal hospital stays, in part because vaginally extracted breech twins have less respiratory disease and fewer infections (Mauldin et al., Reference Mauldin, Newman and Mauldin1998). Therefore, the first twin presentation is important in choosing the mode of delivery, and it needs a practical and helpful study on longitudinal assessment of the first twin presentation to counsel the parents based on the data individually applicable. The aim of this study was to evaluate longitudinal changes of fetal presentation in twin pregnancies and to counsel parents based on this data.
Materials and Methods
Medical records of all twin pregnancies delivered between January 1999 and August 2009 were reviewed retrospectively. All patients were cared for from early-third trimester and delivered at the Seoul National University Hospital. Gestational age at assessment was divided into two intervals: early-third trimester (28–31 weeks) and mid-third trimester (32–35 weeks). Exclusion criteria were patients delivering prior to 36 weeks’ gestation, monochorionic monoamniotic twins, and intrauterine demise of the first twin. The first or presenting twin was defined as the fetus that was closer to the internal os of uterine cervix. Polyhydramnios was defined as a single deepest pocket of 8 cm or more in the sac of the first twin. Fetal presentation was categorized as vertex or non-vertex. Transverse or oblique lie and breech presentation were considered non-vertex. Longitudinal assessment of the first twin presentation was conducted during gestation and birth in all cases. We analyzed change of fetal presentation between antepartum intervals and at birth. The study population was divided into eight groups (groups A to H) according to spontaneous version of the first twin presentation longitudinally assessed (Table 1). ‘Version group’ was defined as a group that underwent one or more spontaneous versions of the first twin throughout the whole third trimester and birth. Patients’ information about maternal age, parity, chorionicity, pre-pregnancy body mass index (BMI), mode of conception, weight discordancy, fetal gender, amniotic fluid status, uterine fibroids, and birth weight was obtained from medical records. The protocol for the present study was approved by the Institutional Review Board of the Seoul National University Hospital.
TABLE 1 Presenting Part of First Twin

V = vertex; NV = non-vertex.
Continuous data are presented as mean ± standard deviation (SD), and dichotomous data as frequency and associated percentage. Comparison between the groups was performed by using the Mann–Whitey U test for continuous data and the chi-squared or Fisher exact test for categorical data. All statistical analyses were performed by using SPSS version 20.0 for Windows (IBM SPSS Statistics, Chicago, IL, USA), and p values of <.05 were considered statistically significant.
Results
A total of 411 live-born twin pregnancies were identified with a gestational age at birth ≥36 weeks. In total, 332 (80.8%) were nulliparas. The mean maternal age was 32.2 years. Of the 411 pregnancies, 350 (85.2%) were dichorionic diamnionic, 50 (12.1%) were monochorionic diamnionic, and 11 (2.7%) were unknown chorionicity. The chorionicity was decided by early trimester ultrasound image, fetal sex, and pathologic findings except for 11 patients with no early ultrasound image, same-sex twins, and no pathology report. In total, 120 (29.2%) pregnancies were conceived naturally and the remaining 291 (70.8%) were by assisted reproductive technology, including in vitro fertilization.
Longitudinally assessed presentation of the first twin is described in Table 1. Most twin pregnancies showed that the first twin presentation was vertex during third trimester and birth. The first twin presentation did not change in 87.6% of cases between early-third trimester and birth. Those with vertex presentation at early-third trimester had the same presentation at birth in 95.6% of cases. Those with non-vertex presentation at early-third trimester had the same presentation at birth in 67.0% of cases. In total, 96% of twin pregnancies did not undergo spontaneous version between mid-third trimester and birth. During this interval, vertex was 98.4% and non-vertex was 88.5% of cases. When comparing vertex with non-vertex, vertex-presenting twins were very unlikely to undergo spontaneous version compared to non-vertex (p < .001). In contrast, more non-vertex presenting twins underwent spontaneous version into vertex (Table 2). Of 115 twin pregnancies with non-vertex presentation at early-third trimester, 38 (33.0%) delivered with vertex presentation at birth. Of 96 twin gestations with non-vertex presentation at mid-third trimester, only 11 (11.5%) delivered with vertex presentation at birth (Tables 1 and 2).
TABLE 2 The Rate of No Change in the Presenting Part of First Twin at Birth According to Presentation During Third Trimester

No correlation was found between spontaneous version of the first twin presentation during early-third trimester and maternal age, parity, chorionicity, mode of conception, pre-pregnancy BMI, birth weight, fetal gender, amniotic fluid status, uterine fibroids, and weight discordancy (Table 3). However, there were two factors affecting the first twin version since the mid-third trimester. The factors that contributed significantly to spontaneous version of the first twin presentation were lower birth weight of the first twin and the paired birth-weight differences between the first and the second twins, especially when the first twin was smaller than the second twin (Table 4). Table 5 describes factors affecting spontaneous version throughout the whole third trimester and birth. As mentioned in the methods section, ‘version group’ was defined as the presence of one or more spontaneous versions of the first twin presentation throughout the whole third trimester and birth. In comparing the ‘no version’ and ‘version’ group, there were no affecting factors except lower birth weight of the first twin compared with the second twin in the rate of spontaneous version of the first twins.
TABLE 3 Comparison of No Change Group and Change Group Between Early-third Trimester and Birth

BMI = body mass index. Values are presented as % (n) or mean ± standard deviation.
TABLE 4 Comparison of No Change Group and Change Group Between Mid-third Trimester and Birth
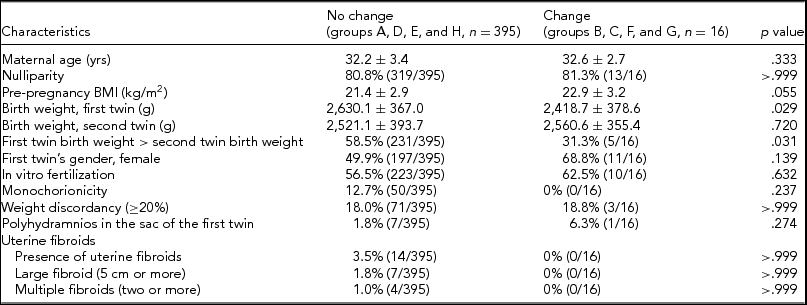
BMI = body mass index. Values are presented as % (n) or mean ± standard deviation.
TABLE 5 Comparison of No Version Group and Version Group Throughout Third Trimester and Birth

BMI = body mass index. ‘Version group’ was defined as one or more spontaneous versions of the first twin's presentation throughout third trimester and birth. Values are presented as % (n) or mean ± standard deviation.
Discussion
The present study provides longitudinally assessed presentation of the first twin and its spontaneous version between third trimester and birth. The data showing longitudinal change are useful for counseling patients about fetal presentation and mode of delivery in twin pregnancies. The results of this study, which are individually applicable to patients, make it possible for obstetricians to predict fetal presentation at birth of twin gestation using ultrasound during the third trimester. Based on our study, vertex-presenting twins are unlikely to change their presentation during the third trimester. In other words, vertex presentation in twins is stable and predictable, while in contrast, non-vertex presentation is relatively unstable.
As with our data, Chasen et al. (Reference Chasen, Spiro, Kalish and Chervenak2005) and Divon et al. (Reference Divon, Marin, Pollack, Katz, Henderson, Aboulafia and Merkatz1993) also reported that vertex presentation was most stable in twin gestations. In vertex-presenting first twins after 28 or 32 weeks of gestation, ultrasound can predict the first twin presentation at birth in 90% and 95% or more of cases respectively (Chasen et al., Reference Chasen, Spiro, Kalish and Chervenak2005; Divon et al., Reference Divon, Marin, Pollack, Katz, Henderson, Aboulafia and Merkatz1993; Fox et al., Reference Fox, Rebarber, Lesser, Roman, Klauser and Saltzman2013; Melamed et al., Reference Melamed, Wong, Asztalos, Rosen, Okby and Barrett2015; Schwartz et al., Reference Schwartz, Fuchs and Rosenn2012).
Although several studies have reported on the spontaneous version in twin gestations, their methods had one or more limitations, and their results were limited due to small sample sizes, inappropriate timing of enrollment, limited study population originating from secondary analysis of a previous large study, or cross-sectional analysis between only two time intervals (Chasen et al., Reference Chasen, Spiro, Kalish and Chervenak2005; Divon et al., Reference Divon, Marin, Pollack, Katz, Henderson, Aboulafia and Merkatz1993; Fox et al., Reference Fox, Rebarber, Lesser, Roman, Klauser and Saltzman2013; Melamed et al., Reference Melamed, Wong, Asztalos, Rosen, Okby and Barrett2015; Santolaya et al., Reference Santolaya, Sampson, Abramowicz and Warsof1992; Schwartz et al., Reference Schwartz, Fuchs and Rosenn2012). In 2015, Melamed et al. reported the secondary analysis of a previous large randomized controlled trial on the mode of delivery in twin pregnancies. The study enrolled only the women with vertex-presenting twins at the time of randomization and analyzed the spontaneous version of both of the first and second twins. Many women who had an estimated fetal weight less than 1,500 g, previous uterine scar by vertical uterine incision, two or more previous low-segment uterine incisions, presence of lethal fetal anomaly, or a second twin substantially larger than the first twin were also excluded. This point was an inherent weakness in the study design. Moreover, mean gestational age at randomization of 35 weeks was unfavorable for using the study results to predict fetal presentation at birth and to counsel the parents based on the data, because 35 weeks was the average timing of delivery in twin pregnancies (American College of Obstetricians and Gynecologists and Society for Maternal-Fetal Medicine, 2014).
In analyzing factors affecting spontaneous version of fetal presentation in twin pregnancies, the results of previous studies were controversial. Two studies found the correlation between the spontaneous version and specific factors (Fox et al., Reference Fox, Rebarber, Lesser, Roman, Klauser and Saltzman2013; Melamed et al., Reference Melamed, Wong, Asztalos, Rosen, Okby and Barrett2015) and two other studies did not (Chasen et al., Reference Chasen, Spiro, Kalish and Chervenak2005; Divon et al., Reference Divon, Marin, Pollack, Katz, Henderson, Aboulafia and Merkatz1993). In contrast to the results by Fox et al. (Reference Fox, Rebarber, Lesser, Roman, Klauser and Saltzman2013) and Melamed et al. (Reference Melamed, Wong, Asztalos, Rosen, Okby and Barrett2015), the present study showed that lower first twin birth weight and the paired birth-weight differences between the first and the second twins were associated with spontaneous version of the first twin presentation. Fox et al. (Reference Fox, Rebarber, Lesser, Roman, Klauser and Saltzman2013) found that higher estimation of fetal weight of the second twin was associated with the first twin version. Melamed et al. (Reference Melamed, Wong, Asztalos, Rosen, Okby and Barrett2015), whose study included only vertex-presenting twins, identified several independent factors associated with spontaneous version of the first twin presentation, including non-vertex second twin, lower weight of the second twin, change in the second twin presentation, and an interval to delivery of more than 4 weeks. In contrast, the first twin version was not affected by the second twin's size in our study. Moreover, Fox et al. (Reference Fox, Rebarber, Lesser, Roman, Klauser and Saltzman2013) found that prior term vaginal delivery and increased estimation of fetal weight in either twin were associated with spontaneous version of the first twin. The majority of the study population in our research was nulliparous (81%), and therefore we did not analyze factors associated with prior pregnancies. Interestingly, the paired birth-weight difference with a smaller first twin was associated with spontaneous version of the first twins between mid-third trimester and birth, but not between early-third trimester and birth. This factor was also correlated to the first twin version of one or more times throughout the whole third trimester and birth. It is supposed that spontaneous version of twin presentation is not affected by fetal size until the early-third trimester, when the intrauterine space is relatively ample for fetal movement, compared with the mid-third trimester or later. It is thought that paired birth-weight differences are not likely to be a critical factor for spontaneous version of the first twins because the fetuses move or rotate their position relatively freely at the earlier gestational period. However, it seems that paired birth-weight differences accompanied by increased fetal size may affect spontaneous version of twin presentation in the condition of a relatively confined space at the later gestational period. Several studies, mainly including singleton gestations, have mentioned uterine fibroids as a risk factor for fetal malpresentation and the rate of cesarean delivery (Ciavattini et al., Reference Ciavattini, Clemente, Carpini, Giuseppe, Giannubilo and Tranquilli2015; Vitale et al., Reference Vitale, Padula and Gulino2015). Therefore, we first analyzed and evaluated the relationship between the first twin's presentation and presence, size, or number of uterine fibroids. In our twin cohort, however, uterine fibroids were not related to fetal presentation in twin gestations.
The strength of the present study was the relatively large sample size and longitudinal assessment of the first twin presentation from early-third trimester to mid-third trimester to birth. The simple data model shown in Tables 1 and 2 may be useful for clinicians when counseling parents with twin gestations to determine the probability of final presentation and choose the mode of delivery. Moreover, the timing of enrollment of patients in this study was an appropriate period when clinicians usually discuss the route of delivery with their patients who have conceived twins.
The limitations of our study were to evaluate the first twin presentation only and that various types of non-vertex presentation, such as breech and transverse or oblique lie, were not distinguished. It may be found that different types of non-vertex first twin presentation are different in the rate of spontaneous version. For those with vertex/non-vertex twin pregnancies, the mode of delivery remains controversial. Although several studies have reported successful vaginal delivery of both twins using internal or external version of second twin or breech extraction of the second twin (Chauhan et al., Reference Chauhan, Roberts, McLaren, Roach, Morrison and Martin1995; Chervenak et al., Reference Chervenak, Johnson, Youcha, Hobbins and Berkowitz1985; Davison et al., Reference Davison, Easterling, Jackson and Benedetti1992), these require obstetricians experienced in intrauterine fetal manipulation. Nevertheless, longitudinally assessed data of spontaneous version of the first twins may be useful in informing patients of expected fetal presentation and to determine the mode of delivery in twin gestations when they want to attempt vaginal delivery. Future studies with a prospective design and much larger sample size using detailed affecting and confounding factors are needed.
In summary, twin gestations undergo spontaneous version during the third trimester. Based on our study, vertex-presenting first twins are unlikely to change their presentation during the third trimester. In contrast, non-vertex presentation of the first twin is relatively unstable.
Acknowledgments
This research was supported by the SNUH Research Fund funded by the Seoul National University Hospital (2520160070).







