Research shows that symptoms of anxiety and depression are highly concordant (Reference Clark and WatsonClark & Watson, 1991). Also, there is a high comorbidity of anxiety and depression at the caseness level (Reference BarbeeBarbee, 1998, especially in late life (Reference Kirby, Bruce and RadicKirby et al, 1997). Among older persons about 50% of the clinically depressed suffer from comorbid anxiety disorders and 25% of patients with anxiety suffer from major depression (Reference Beekman, de Beurs and van BalkomBeekman et al, 2000). Current knowledge on the phenomenology of psychopathology in late life is limited, but the scarce data available do suggest that distinctive features of depression and anxiety become even less pronounced with rising age (Reference MacKinnon, Christensen and JormMacKinnon et al, 1994). However, an important aspect on which depression and anxiety in late life may be distinguished is the risk profiles for these conditions. Delineating risk profiles is crucial to the development of focused preventive measures aimed at emotional problems in late life. The present study sets out to compare risk profiles for anxiety and depression. Risk factors were organised according to the stress-vulnerability model (Reference Brown and HarrisBrown & Harris, 1978; Reference Goldberg and HuxleyGoldberg & Huxley, 1992), which states that destabilisation (getting symptoms) is the result of long-lasting vulnerability factors acting in concert with exposure to environmental stressors, usually one or more highly stressful events.
METHOD
Sample and procedure
To investigate risk profiles for developing depression and anxiety in older persons we used data from the Longitudinal Aging Study Amsterdam (LASA; Reference Deeg, Knipscheer and van TilburgDeeg et al, 1993). The LASA is a longitudinal study in a large representative sample aged 55-85 years. Data were collected by interviewing respondents in their homes by trained and intensively supervised interviewers. All interviews were audiotaped to allow random quality checks. The first cycle of LASA data collection (T 1) took place between the autumn of 1992 and the autumn of 1993; the second cycle (T 2) took place 3 years later (1995-1996). A random sample of older men and women, stratified for age and gender, was drawn from the population registers of 11 municipalities in three regions of The Netherlands. Older men initially were oversampled to ensure sufficient respondents in these strata for a later phase of the study. In the first cycle of LASA, 3107 respondents were interviewed. This sample has been described extensively in previous publications of LASA (Reference Beekman, Deeg and van TilburgBeekman et al, 1995; Reference de Beurs, Beekman and van Balkomde Beurs et al, 1999). Three years later the respondents were contacted again and 2302 (74%) were willing and still able to be interviewed again. Of the 805 non-participants, 417 (13.4% of the T 1 sample) had died, 253 (8.1%) were interviewed by telephone, which did not include the depression and anxiety assessment, 38 (1.2%) were too ill or cognitively impaired to be interviewed, 90 (2.9%) indicated that they were no longer interested in partaking in the study and 17 (0.5%) could not be contacted. Owing to item non-response on measures for depression and anxiety at T 1 or T 2, a further 139 respondents were lost, leaving 2163 subjects for whom depression and anxiety scores were available at both time points (69.6% of the T 1 respondents). The 944 non-participants were compared with the 2163 participants on key variables, to check for selective attrition. No significant difference was found between participants and non-participants regarding anxiety symptoms, but higher depression did make attrition more likely. For other variables we also found an association with attrition: non-participants were more likely to be male, unmarried, older, to be of lower socio-economic status and to have a chronic disease, more functional limitations and a lower score on the Mini-Mental State Examination (MMSE; Reference Folstein, Folstein and McHughFolstein et al, 1975). Thus, the subjects who were lost fromT 1 to T 2 comprised the less healthy and worse functioning part of the initial participants atT 1.
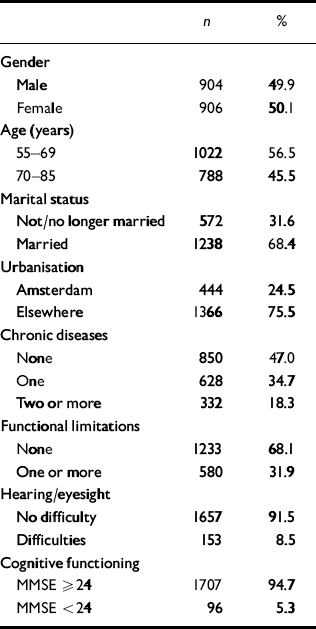
At T 1 120 respondents (5.5%) had depression symptoms, 84 (4.0%) had anxiety symptoms and 147 (6.8%) had both depression and anxiety symptoms. Because we aimed to investigate becoming depressed or anxious, respondents with symptoms were removed from the sample, leaving 1810 respondents. Descriptive statistics and data on health and functioning of the final study sample are presented in Table 1.
Table 1 Descriptive data at T 1 of the sample (n=1810)
| n | % | |
|---|---|---|
| Gender | ||
| Male | 904 | 49.9 |
| Female | 906 | 50.1 |
| Age (years) | ||
| 55-69 | 1022 | 56.5 |
| 70-85 | 788 | 45.5 |
| Marital status | ||
| Not/no longer married | 572 | 31.6 |
| Married | 1238 | 68.4 |
| Urbanisation | ||
| Amsterdam | 444 | 24.5 |
| Elsewhere | 1366 | 75.5 |
| Chronic diseases | ||
| None | 850 | 47.0 |
| One | 628 | 34.7 |
| Two or more | 332 | 18.3 |
| Functional limitations | ||
| None | 1233 | 68.1 |
| One or more | 580 | 31.9 |
| Hearing/eyesight | ||
| No difficulty | 1657 | 91.5 |
| Difficulties | 153 | 8.5 |
| Cognitive functioning | ||
| MMSE ≥ 24 | 1707 | 94.7 |
| MMSE < 24 | 96 | 5.3 |
Measures
Depression and anxiety
Depression was measured with the Center for Epidemiological Studies Depression scale (CES-D; Reference RadloffRadloff, 1977). Depressive symptoms were considered present if the CES-D score was ≥ 16. Anxiety was measured with the Anxiety sub-scale of the Hospital Anxiety and Depression Scale (HADS-A; Reference Zigmond and SnaithZigmond & Snaith, 1983). On the HADS-A the recommended cut-off of ≥ 7 was applied to decide whether a respondent developed symptoms of anxiety or not. However, merely crossing the cutoff on the CES-D or HADS-A at T 2 was deemed insufficient to consider a respondent changed or destabilised, because it can result from random fluctuations due to measurement error on the symptom scale. Therefore, the additional requirement of statistically reliable change was set. To be considered reliably changed, a respondent has to change beyond the standard error of the difference score from T 1 toT 2 (Reference SpeerSpeer, 1992). For our respondents this implied a change of at least seven scale points on the CES-D and four scale points on the HADS-A. Subjects who crossed the cut-off but failed to meet the requirement of statistically reliable change were considered unchanged and categorised as below threshold.
Vulnerability
The following four sets of variables, all measured atT 1, were selected as vulnerability factors for depression and anxiety: demographics, variables regarding health and functioning, personality characteristics and social functioning.
Demographic vulnerability factors included female gender, higher age, not/no longer married, living in Amsterdam and lower socio-economic status. We used a weighted score composed of level of education, occupation and income (range 0-100) as a measure of socio-economic status (Reference van Tilburg, Dykstra and Liefbroervan Tilburg et al, 1995).
Variables regarding health and functioning were included as a separate set of vulnerability factors. In the stress-vulnerability model, somatic illness usually is considered a stressor and is included as such among the stressful life events. However, in view of the fact that health declines during old age often are gradual, ill health and functional limitations also may act as age-specific vulnerability factors. Physical health status was determined in the interview and cross-checked with information from general practitioners (Reference Kriegsman, Penninx and van EijkKriegsman et al, 1996). Physical health includes the number of chronic diseases reported by the respondent, a self-rated health assessment using a single item (Centraal Bureau voor de Statistiek, 1989) and functional limitations, assessed with an adaptation of the Organisation of Economic Collaboration and Development (OECD) Questionnaire (Reference van Sonsbeekvan Sonsbeek, 1988; Reference Kriegsman, Deeg and van EijkKriegsman et al, 1997). Problems with perception (eyesight and hearing) were assessed in the interview by asking the respondent whether they could see/hear “well enough” on a four-point scale (“Yes, no difficulty” to “No, I cannot see/hear”; Centraal Bureau voor de Statistiek, 1989). Responses were recoded into one variable with two levels (no or minor problems v. much difficulty or inability with either eye-sight or hearing). Cognitive functioning was assessed with the MMSE.
Three personality characteristics of the respondents were assessed: mastery, neuroticism and self-efficacy. Mastery was assessed in the interview with the abbreviated five-item locus of control scale (Reference Pearlin and ScoolerPearlin & Scooler, 1978). A higher score means a more external locus of control or less mastery. Neuroticism (15 items) was measured through the abbreviated sub-scale of the Dutch Personality Inventory (Reference Luteijn, Starren and van DijkLuteijnet al, 1985). This self-report scale was completed after the interview and mailed in by the respondent. Not all respondents complied: 540 of the 2163 respondents (25%) failed to return fully completed questionnaires. Non-response on the self-report data was not related to the gender of the respondent but was related to higher age (more non-response in older respondents). Finally, coping was measured in the interview with a 12-item version of the General Self-efficacy Scale (Reference Sherer, Maddux and MercandanteSherer et al, 1982; Reference Bosscher and SmitBosscher & Smit, 1998).
Social resources were assessed by estimating the size of the social network. Respondents were asked to name people they regularly socialised with and whom they deemed important in various domains of life (relatives, neighbours, work, church, etc). The validity of the network size index was supported in a previous study (Reference van Tilburgvan Tilburg, 1994). Also, respondents were questioned about the exchange of emotional support with key members of their social network. Because “emotional support received” could be an important protective factor for developing psychopathology, in particular depression, this variable was included in the analyses as well.
Life events
In the T 2 interview it was assessed retrospectively whether stressful life events had occurred in the time interval betweenT 1 and T 2. Regarding the question of why some people develop depression whereas others develop anxiety, Finley-Jones & Brown (Reference Finley-Jones and Brown1981) have suggested that the type of event may be a decisive factor: stressful life events involving loss (e.g. death of a loved one, retirement) are more likely to lead to depression, whereas stressful events involving threat (e.g. being a victim of crime) lead to anxiety. The following stressful events were assessed: illness of one's partner, death of one's partner, illness of a relative, death of a relative, a major conflict with others, income loss (of at least £30 a month), being a victim of crime and relocation. Life events were analysed individually and we also obtained a single composite score for stress by differentially weighting life events. Weights for various life events were derived from Tennant & Andrews (Reference Tennant and Andrews1976).
All assessment instruments used in the study had been validated previously in The Netherlands or their psychometric properties had been evaluated in LASA pilot studies (Reference Deeg, Knipscheer and van TilburgDeeg et al, 1993).
Statistical analyses
A series of multivariate logistic regression analyses were undertaken, each time comparing one of the symptom groups with the non-symptomatic controls. First, vulnerability factors were analysed in four sets of conceptually related variables: demographics, health and functioning, personality and social functioning as measured at T 1. Thus, variables could be found that were associated significantly with destabilisation, while controlling for the effect of other variables within the same set. This approach limits the number of predictor variables and decreases the risk of collinearity among predictors. Next, the association of each life event and destabilisation for each symptom group was analysed with multiple logistic regression analyses. Finally, in order to attain the most parsimonious set of predictors, we used only the variables that appeared to have predictive value in previous analyses and performed a series of stepwise logistic regression analyses using a forward inclusion criterion of P < 0.20 (Reference MenardMenard, 1995).
To test hypotheses regarding interaction of vulnerability and stress, the interaction term was added to the main effects for each of the three models (Reference Baron and KennyBaron & Kenny, 1986; Reference Hosmer and LemeshowHosmer & Lemeshow, 1989). In these analyses, we used the composite score for stressful life events.
RESULTS
Emergence of depression and anxiety symptoms
The 1810 respondents of the sample below threshold atT 1 were divided into four groups: 1642 (90.7%) respondents remained below threshold, 73 (4.0%) became depressed, 43 (2.4%) became anxious and 52 (2.9%) scored beyond threshold for both depression and anxiety. Inspection of the mean level of anxiety and depression in the three groups with symptoms revealed that the group with both anxiety and depression had the most serious condition because they suffered from more depression and anxiety compared with the groups with pure depression or pure anxiety. TheT 2 mean score on the CES-D was M=25.0 (s.d.=8.5) for both depressed and anxious subjects; M=20.6 (s.d.=4.9) for depressed subjects and M=11.5 (s.d.=4.9) for anxious subjects. Corresponding mean scores on the HADS-A were M=10.7 (s.d.=3.1),M=3.7 (s.d.=2.0) and M=8.7 (s.d.=2.7). All means were significantly different according to pairwise comparisons witht-tests.
Vulnerability to becoming depressed
Demographics, health and functioning personality and social functioning
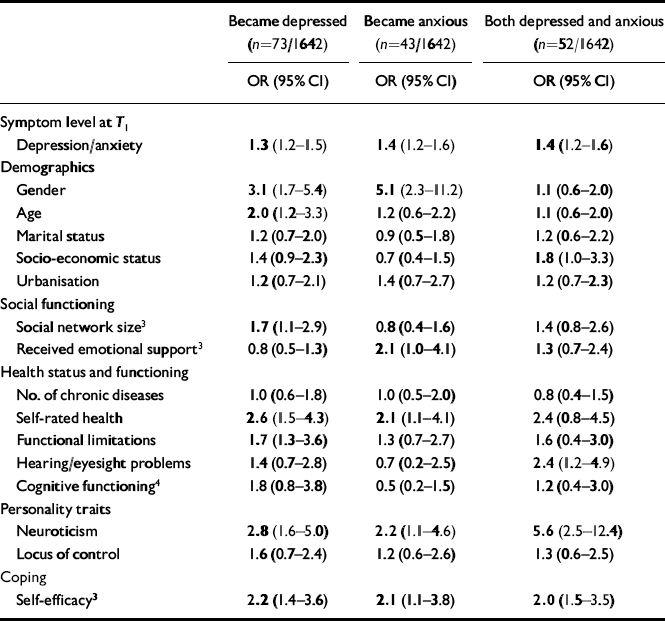
Table 2 presents the results of multiple logistic regression analyses of variables representing vulnerability. The results indicate that for all three symptom groups the initial symptom level (averaged score on the CES-D and HADS-A atT 1) was predictive of destabilisation. For demographic variables the findings show that gender, age and socio-economic status were associated with scoring beyond threshold: females were overrepresented among the purely depressed and the purely anxious; the older old were more likely to be purely depressed; and low socio-economic status increased the chance for depression with anxiety. Results for social functioning were mixed: a smaller social network was predictive of becoming depressed, but not anxious, whereas less emotional support was predictive of anxiety but not depression. Social functioning was not a predictive factor for getting symptoms of both depression and anxiety. Regarding health status and functioning, we found that worse self-rated health predicted pure depression and pure anxiety, but not both anxiety and depression. Furthermore, functional limitations predicted the onset of depression and hearing/eyesight problems predicted the onset of both depression and anxiety. Of the personality variables, neuroticism was predictive of symptoms, especially for the group scoring beyond threshold on both depression and anxiety. Self-efficacy was predictive in all groups that scored beyond threshold at T 2.
Table 2 Association of vulnerability factors1 measured atT 1 with exceeding thresholds2 for symptoms of depression, anxiety and both depression and anxiety according to multiple logistic regression analyses
| Became depressed (n=73/1642) | Became anxious (n=43/1642) | Both depressed and anxious (n=52/1642) | |
|---|---|---|---|
| OR (95%CI) | OR (95%CI) | OR (95%CI) | |
| Symptom level at T 1 | |||
| Depression/anxiety | 1.3(1.2-1.5) | 1.4(1.2-1.6) | 1.4(1.2-1.6) |
| Demographics | |||
| Gender | 3.1(1.7-5.4) | 5.1(2.3-11.2) | 1.1(0.6-2.0) |
| Age | 2.0(1.2-3.3) | 1.2 (0.6-2.2) | 1.1 (0.6-2.0) |
| Marital status | 1.2 (0.7-2.0) | 0.9 (0.5-1.8) | 1.2 (0.6-2.2) |
| Socio-economic status | 1.4 (0.9-2.3) | 0.7 (0.4-1.5) | 1.8(1.0-3.3) |
| Urbanisation | 1.2 (0.7-2.1) | 1.4 (0.7-2.7) | 1.2 (0.7-2.3) |
| Social functioning | |||
| Social network size3 | 1.7(1.1-2.9) | 0.8 (0.4-1.6) | 1.4 (0.8-2.6) |
| Received emotional support3 | 0.8 (0.5-1.3) | 2.1(1.0-4.1) | 1.3 (0.7-2.4) |
| Health status and functioning | |||
| No. of chronic diseases | 1.0 (0.6-1.8) | 1.0 (0.5-2.0) | 0.8 (0.4-1.5) |
| Self-rated health | 2.6(1.5-4.3) | 2.1(1.1-4.1) | 2.4 (0.8-4.5) |
| Functional limitations | 1.7(1.3-3.6) | 1.3 (0.7-2.7) | 1.6 (0.4-3.0) |
| Hearing/eyesight problems | 1.4 (0.7-2.8) | 0.7 (0.2-2.5) | 2.4(1.2-4.9) |
| Cognitive functioning4 | 1.8 (0.8-3.8) | 0.5 (0.2-1.5) | 1.2 (0.4-3.0) |
| Personality traits | |||
| Neuroticism | 2.8(1.6-5.0) | 2.2(1.1-4.6) | 5.6(2.5-12.4) |
| Locus of control | 1.6 (0.7-2.4) | 1.2 (0.6-2.6) | 1.3 (0.6-2.5) |
| Coping | |||
| Self-efficacy3 | 2.2(1.4-3.6) | 2.1(1.1-3.8) | 2.0(1.5-3.5) |
Stepwise multivariate analyses
Next we evaluated all variables that significantly predicted scoring beyond threshold in three stepwise logistic regression analyses. For pure depression, the number of significantly predictive variables was reduced from eight to five (female gender, higher age, worse self-rated health, more functional limitations, and neuroticism). The likelihood ratio of the final model was χ 2 (6)=75.0, pseudo R 2=0.16. Four variables remained to predict anxiety (higher initial symptom level, female gender, less received emotional support and lower self-efficacy). The likelihood ratio of this model was χ2 (4)=34.2, pseudo R 2=0.11. Getting symptoms of both anxiety and depression was predicted by four variables (higher initial symptom level, lower socio-economic status, having hearing or eyesight problems and neuroticism); the likelihood ratio was χ 2 (5)=40.2, pseudo R 2=0.12. All of the stepwise logistic regression analyses were repeated while omitting neuroticism (the variable was 25% missing values owing to non-response). The pattern of associations of the remaining variables on this larger sample did not differ meaningfully from the results described above. By and large, the findings of the stepwise analyses concur with the findings when vulnerability factors were analysed in sets. Apparently, most of the significant predictors of Table 2 have independent predictive value for destabilisation.
Life events associated with depression and anxiety
Stressful life events
Next, the predictive value of stressful life events that occurred in the time interval between both assessments was evaluated. Odds ratios were calculated representing the risk of crossing the threshold when an event had occurred. Table 3 presents the frequency of occurrence of events in the full sample and their odds ratios (with 95% CIs) for each of the three symptoms groups. Statistically significant odds ratios are printed in bold typeface.
Table 3 Results of logistic regression analyses for the effect of stressful life events on destabilisation (bivariate analyses)

| Life events | % | Depression (n=73/1638) | Anxiety (n=43/1638) | Depression and anxiety (n=52/1638) |
|---|---|---|---|---|
| OR (95%CI) | OR (95%CI) | OR (95%CI) | ||
| Illness of partner | 13.3 | 1.5 (0.8-2.8) | 2.0(1.0-4.3) | 1.4 (0.7-3.0) |
| Death of partner | 5.8 | 2.5(1.2-5.2) | 1.3 (0.4-4.4) | 2.3 (1.0-5.6) |
| Illness of other relative | 43.6 | 1.0 (0.6-1.6) | 1.7 (0.9-3.1) | 1.2 (0.7-2.1) |
| Death of other close relative | 31.4 | 1.6 (1.0-2.6) | 1.4 (0.7-2.5) | 2.0(1.1-3.4) |
| Conflict with others | 7.5 | 1.8 (0.9-3.7) | — 1 | 1.2 (0.5-2.9) |
| Victim of crime | 3.6 | — 1 | — 1 | 2.9(1.1-7.4) |
| Income loss | 19.9 | 1.0 (0.6-1.8) | 0.8 (0.4-1.5) | 1.2 (0.7-2.2) |
| Relocation | 12.7 | 1.7 (0.9-3.0) | 0.7 (0.3-2.0) | 0.9 (0.4-2.2) |
| Any of the above | 73.9 | 1.7 (0.9-3.1) | 1.4 (0.7-2.9) | 1.8 (0.9-3.6) |
To investigate which events had an association with destabilisation while controlling for the effects of other events, we also performed a multiple logistic regression with stepwise selection of events. For pure depression, death of the partner, death of another family member and a major conflict were associated with destabilisation. The main events associated with an increase in anxiety symptoms were illness of the partner or a family member and having had a major conflict. Finally, events associated with crossing the threshold for both depression and anxiety were the death of a family member and having been victimised by crime.
Interaction of vulnerability factors and stressful life events
Finally, interactions between significant vulnerability factors (neuroticism, mastery, social network size and coping style) and a selected set of stressful life events were studied. Low mastery was expected to amplify the effect of stress due to loss, and high neuroticism was expected to amplify the adverse effects of stress related to threat on mental health. Regarding social functioning, a protective effect of a large social network was hypothesised, moderating the adverse influence of stressful life events in general. Likewise, higher self-efficacy was hypothesised to protect for the effect of general stress. Hypotheses regarding effect modification were investigated by testing the main effect for each pair of predictors, as well as their interaction. Results showed that in analyses involving neuroticism and mastery none of the interaction terms were significant. Thus, no augmenting effect of neuroticism or low mastery on negative life events for developing depression and/or anxiety symptoms was found. This finding indicates that vulnerability factors and stressful life events, rather than interacting, add to each other in increasing the odds for destabilisation. Regarding the buffering effect of social functioning, only the interaction between received emotional support and stress for developing pure anxiety was marginally significant: respondents who reported more social support were less likely to develop anxiety when faced with stressful events (standardised β =1.21, OR=3.3 (0.9-12.6), P=0.07). No significant interaction of self-efficacy and general stress was found.
DISCUSSION
Limitations
Analyses were performed on a substantially smaller subsample compared with the initial random sample because of attrition from T 1 toT 2. However, attrition for reasons other than mortality was limited. Additional analyses were performed to check for selective attrition. The T 2 sample did differ from theT 1 sample on many of the predictor variables but not in depression or anxiety level. The respondents who were lost had belonged to the older, less healthy, poorest functioning part of the T 1 sample. Furthermore, we selected a subgroup of nondepressed and non-anxious subjects at T 1. Analyses involving neuroticism further diminished the sample size because of non-response on the self-report questionnaires. Loss of subjects through attrition and limiting the sample to emotionally healthy subjects at T 1 limits the range in the risk factors, making it less probable to find significant associations. Furthermore, this reduction in size of the sample diminished the statistical power to find significant results, which is especially relevant for variables with low rates of occurrence, such as being a victim of crime.
Another cautionary remark regarding methodological aspects of the study concerns the status of life events as predictors. Most life events were assessed retrospectively at T 2 and therefore are not predictors in the true sense of the word. Our hypothesis was that negative life events would increase the odds for getting symptoms. However, respondents who destabilised into depression might have had a better recollection for negative events (mood congruent recall; Reference BowerBower, 1981), thus biasing the results in favour of the hypothesis. On the other hand the most significant events, such as the death of one's spouse, are unlikely to be influenced by recall bias. Nevertheless, a cautionary presentation of the present findings regarding life events describes them as associations rather than as directional relations. With these limitations in mind we will briefly review the most interesting findings.
Variables predictive of getting depression and/or anxiety symptoms
Important vulnerability factors for getting symptoms were female gender, high neuroticism and worse self-rated health. Generally, epidemiological studies report a higher prevalence of depression and anxiety among women. High neuroticism was predictive for all symptom groups. Of course, neuroticism was associated with depression or anxiety level at baseline (cf. Reference Clark and MinekaClark et al, 1994). The present findings reveal the prognostic value of neuroticism for developing emotional problems in a prospective design. Similar findings have been reported for younger age groups. Duncan-Jones (Reference Duncan-Jones and Cooper1987) reported the findings of a longitudinal study in an Australian sample of mixed-age adults where fluctuations in symptoms of psychopathology were well predicted by neuroticism scores. Ormel & Schaufeli (Reference Ormel and Schaufeli1991) replicated these findings in a sample of college students. The present findings complement this literature, by demonstrating the importance of premorbid personality characteristics to emotional problems in late life.
Analysis of the vulnerability factors regarding health and functioning in late life revealed self-perceived poor health as a better predictor for mental health decline than chronic diseases. Apparently, how respondents experience their own health predicts subsequent emotional functioning more strongly than their objective health status. Similar findings were reported by Bath & Morgan (Reference Bath and Morgan1998). In contrast, with mixed-age groups many studies report a strong effect of somatic illness on emotional functioning (Reference Viney and WestbrookViney & Westbrook, 1981). The adverse effect of a physical illness on emotional functioning may diminish with rising age, because in late life chronic diseases are much more common and accepted as a fact of life.
Regarding the specificity of vulnerability factors for either depression or anxiety, the similarity of risk profiles for the groups outweighs dissimilarity. However, some discrepancies are worth noting. Higher age was predictive only of depression and remained so after controlling for other factors, such as poorer self-rated health. This finding is in line with the literature documenting that the likelihood of depression increases with older age (Reference Beekman, Copeland and PrinceBeekman et al, 1999). Functional limitations at baseline also were specifically associated with depression and not anxiety. Functional limitations have been implicated in depression among older persons previously. Regarding social functioning, network size and amount of emotional support traded places in predicting depression and anxiety. This finding underlines the multi-dimensional nature of social support (Reference Cohen and WillsCohen & Wills, 1985).
Recent stressful life events
Partial support for the hypothesised specificity of loss v. threat events for depression and anxiety was found: loss events (e.g. the death of a family member) were associated with becoming depressed, whereas threat (e.g. a family member getting a major illness) was predictive of becoming anxious. The significant association between death of the partner and depression may in part reflect bereavement rather than depression (Reference Prince, Harwood and BlizardPrince et al, 1997). However, in additional analyses, leaving out the respondents who lost their spouse in the previous 6 months, death of the partner was still a significant predictor of symptoms of depression. Unexpectedly, being a victim of crime (obviously a threat event) was associated with getting symptoms of both anxiety and depression. Apparently, this event, although seldom occurring in the life of Dutch citizens, has a quite pervasive influence.
The distinctness of risk profiles for depression and anxiety in older persons underlines the validity of distinguishing these clusters of symptoms. It has been argued that this distinction diminishes in late life, where depression and anxiety are often found as comorbid conditions. The present results show that depression and anxiety share common vulnerability factors, but also that distinct stressful events produce different outcomes.
Neuroticism, mastery, social support and self-efficacy as effect modifiers
The stress-vulnerability model hypothesises an augmenting effect of high neuroticism and low mastery (Reference Goldberg and HuxleyGoldberg & Huxley, 1992) and a buffering effect of social support for the effects of life events (Reference Brown and HarrisBrown & Harris, 1978). Although strong direct effects of neuroticism and distress on destabilisation were found, no evidence for significant interactions with stress were attained. The more specific hypotheses linking neuroticism with threat events and mastery with loss events were not supported either. Apparently, the adverse effects of neuroticism and life's stress add on to each other, rather than amplify their mutual effects. The results regarding social functioning were similar. Analyses revealed only a marginally significant interaction effect of emotional support and distress for developing anxiety symptoms, indicating that more emotional support buffers the effect of adverse life events. No other interaction terms were significant. The main effects of social support on the deterioration of mental health also were small, which is in line with recent findings (Reference Olstad, Sexton and SogaardOlstad et al, 1999). Overall, the present results do not lend support to the interaction hypothesis of the stress-vulnerability model.
Clinical Implications and Limitations
CLINICAL IMPLICATIONS
-
• Important risk factors for getting emotional problems in late life are female gender, bad health, high neuroticism and stressful events.
-
• Onset of depression is best predicted by the death of a partner or family member; anxiety is best predicted by having a partner who develops a major illness.
-
• Getting symptoms of both depression and anxiety is associated with low socio-economic status, hearing/eyesight problems and falling victim to crime.
LIMITATIONS
-
• This analysis was limited to emotionally healthy respondents; factors predictive of recovery were not studied.
-
• Although the initial study sample was sizable, the incidence of anxiety and depression symptoms is low, generating relatively small number of subjects in the groups that were compared, which limits the power to find significant associations.
-
• Because symptoms were assessed with a 3-year interval, short bouts of depression or anxiety may have been missed, thereby ignoring short-lived immediate responses to stressful life events.
Acknowledgements
The Longitudinal Aging Study Amsterdam (LASA) is largely funded by the Dutch Ministry of Health, Welfare and Sports. The present study was supported by a grant from the Dutch Organisation for Scientific Research (NWO).






eLetters
No eLetters have been published for this article.