Major depression is an important public health problem, associated with high levels of functional impairment and impairment in quality of life. Reference Spitzer, Kroenke, Linzer, Hahn, Williams and deGruy1,Reference Üstun, Ayuso-Mateos, Chatterji, Mathers and Murray2 Moreover, depression is related to high health service utilisation, work absenteeism and decreased performance at work with elevated direct and indirect social costs. Reference Fernández, Bellón, Pinto-Meza, Luciano, Autonell and Palao3,Reference Lerner, Adler, Chang, Lapitsky, Hood and Perissinotto4 The most authoritative guidelines basically agree on first-line treatments for individuals with moderate to severe depression; however, they differ on recommendations for ‘mild major’ depression, because few data exist on this condition. Reference Davidson5 The American Psychiatric Association practice guidelines for the treatment of major depression recommend either psychotherapy or antidepressant monotherapy for mild depression. 6 Only two criteria for the choice were proposed: patient preference and previous treatment response. The National Institute for Health and Care Excellence (NICE) guidelines recommend that for mild major depression a range of low-intensity psychosocial interventions and a stepped-care approach should be used. 7 Antidepressants should not be used routinely because the risk-benefit ratio is poor and limited to specific situations, for example mild persistent depressive symptoms or a history of severe depression.
Mild depression is the most prevalent form of depression in the community Reference Kessler, Berglund, Demler, Jin, Koretz and Merikangas8 and its management involves mainly primary healthcare services. It is therefore important to improve the selection of first-line treatments available to primary care settings. However, to date, there is a lack of evidence from studies comparing the efficacy and effectiveness of pharmacotherapy v. psychotherapy that may serve as a guide for primary care practitioners when choosing between treatments for patients with mild depression. Given that antidepressant medication and psychotherapies have comparable response rates and that different antidepressants have similar efficacy, the treatment choice should be based ideally on patient characteristics and treatment preference. Reference Simon and Perlis9 This personalised approach takes advantage of the identification of patient characteristics that predict a differential response to alternative treatments (the so-called moderators of treatment response, or effect modifiers). Reference Papakostas and Fava10 We therefore carried out a large multicentre randomised controlled trial (RCT) comparing a brief structured psychological intervention, interpersonal counselling, with selective serotonin reuptake inhibitor (SSRI) use for patients with mild to moderate major depression. The primary and secondary objectives of the study were: (a) to compare the efficacy of interpersonal counselling with SSRIs in primary care attenders; and (b) to identify moderators of treatment outcome at 2 months. We examined both demographic and baseline clinical characteristics as potential moderators of treatment outcome. Based on evidence from previous studies conducted in the mental health setting Reference Frank, Cassano, Rucci, Thompson, Kraemer and Fagiolini11-Reference Kocsis, Leon, Markowitz, Manber, Arnow and Klein14 and on NICE guidelines, 7 we hypothesised that patients with more severe depression, previous depressive episodes and comorbid anxiety disorder would have a better response to drug treatment than to the psychological intervention. We also hypothesised, as suggested by Fournier et al, Reference Fournier, DeRubeis, Shelton, Hollon, Amsterdam and Gallop15 that married and unemployed patients would exhibit a better response to the psychological intervention than to the drug treatment.
Method
The full protocol for the DEPICS study is described elsewhere. Reference Menchetti, Bortolotti, Rucci, Scocco, Bombi and Berardi16 Briefly, this multicentre RCT comparing interpersonal counselling and SSRI pharmacotherapy took place between May 2006 and May 2008 at nine academic centres located in Northern, Central and Southern Italy (the final follow-up was completed in July 2009). In each centre the research project was conducted by specific psychiatric consultation-liaison services collaborating with primary care physicians working in the catchment area to improve the quality of treatment for patients with depression and to promote enrolment in the trial. Patients identified by primary care physicians as depressed were referred to the consultation-liaison service and seen by a psychiatrist and a research assistant to determine their eligibility for the study. Eligible patients signed a written informed consent after an explanation of the study procedures and an opportunity to ask questions. The study was approved by the ethics committee of the Bologna University Hospital Authority Sant’Orsola-Malpighi and registered with the Australian New Zealand Clinical Trials Registry (ACTRN12608000479303).
Inclusion criteria were: age ⩾18 years, meeting DSM-IV criteria 17 for major depression, confirmed with the Mini-International Neuropsychiatric Interview (MINI), Reference Sheehan, Lecrubier, Sheehan, Amorim, Janavs and Weiller18 treatment for either a first or second depressive episode and a score ⩾13 on the Hamilton Rating Scale for Depression (HRSD, 21-item version). Reference Hamilton19 Exclusion criteria were: ongoing effective treatment with antidepressants or psychotherapy, moderate to high suicide risk, more than two treated episodes of major depression, current/past episodes of mania or hypomania, current/past psychotic symptoms, borderline or antisocial personality disorder, substance use disorder, cognitive impairment, pregnancy or breastfeeding, poor knowledge of the Italian language. Those patients who met all inclusion/exclusion criteria but had an HRSD score <13 at baseline were reassessed after 1 month to establish their eligibility for the study; if their HRSD score was ⩾13 after 1 month they were enrolled and randomised to interpersonal counselling or SSRIs.
Randomisation sequences, derived from a computer random number generator, were delivered to each centre by the coordinating centre. In each centre, allocation to treatment group was made by dedicated research personnel outside the consultation-liaison service where the patients were recruited, assessed and treated. After baseline assessment and consent to participate in the study was obtained, the researcher was contacted via telephone by clinicians and disclosed the assignment.
Interventions
Interpersonal counselling is a brief structured psychological intervention derived from interpersonal psychotherapy, a time-limited evidence-based psychotherapy for major depression. Reference Klerman, Weissman, Rounsaville and Chevron20 As with interpersonal psychotherapy, interpersonal counselling focuses on patients’ current interpersonal problems and social functioning in four problem areas: complicated grief, interpersonal disputes, role transitions and interpersonal deficits. It consisted of six 30 min sessions, with the initial session lasting 1 h. The therapist could evaluate if one or two additional sessions were needed. Originally designed for distressed patients with symptoms relating to current life stressors in primary care, Reference Klerman, Budman, Berwick, Weissman, Damico-White and Demby21 interpersonal counselling has subsequently been tested as a stand-alone intervention in patients with mild or subthreshold depression. Reference Mossey, Knott, Higgins and Talerico22,Reference Neugebauer, Kline, Bleiberg, Baxi, Markowitz and Rosing23 More details about the intervention are given in the online supplement.
Regarding drug treatment, the protocol allowed the use of two SSRIs (sertraline or citalopram) on the basis of the study psychiatrists’ clinical judgement. At the first treatment visit, the psychiatrists provided education about antidepressants and their side-effects. Two or three subsequent visits with the psychiatrist were planned at 2- to 3-week intervals in order to evaluate patients’ adherence to treatment, clinical response and initial side-effects.
Baseline assessment and outcome measure
Demographic characteristics and medical history, including both significant current and past physical illnesses and depressive episodes were collected. Severity of depression was evaluated with the 21-item HRSD. An HRSD score from 8 to 17 indicates mild depression, from 18 to 24 moderate depression and a score ⩾25 indicates severe depression. Daily functioning was assessed using the Work and Social Adjustment Scale (WSAS). Reference Mundt, Marks, Shear and Greist24 This self-report scale consists of five items exploring work functioning, home management, social leisure, private leisure and relationships on an eight-point ordinal scale. A score from 11 to 20 denotes mild functional impairment, whereas a score higher than 20 denotes severe functional impairment. Reference Thase, Entsuah and Rudolph25 Raters who administered the assessment instruments were different from the clinicians who provided psychiatric consultation to the primary care physicians and delivered the pharmacological or psychological interventions. Efforts were made to keep raters masked to randomisation assignment. The primary end-point was remission of depressive symptoms, defined as an HRSD ⩽7 at the 2-month follow-up visit.
Sample size calculation
A meta-analysis of RCTs on major depression estimated a 35% remission rate with SSRI treatment. Reference Thase, Entsuah and Rudolph25 Studies conducted in primary care reported higher remission rates with SSRIs, ranging from 52 to 67%. Reference McPartlin, Reynolds and Anderson26,Reference Mynors-Wallis, Gath, Day and Baker27 No data are available for interpersonal counselling for depression in primary care as a stand-alone therapy. We based the sample size calculation on a critical difference in remission rates between the two treatments of 15%. We calculated that a sample size of 274 (137 per arm, 15.2 per site per arm) would result in a power of 80% at a 0.05 alpha level. To protect against a drop-out rate of about 10% at the first 2-month follow-up, we planned to enrol 300 patients (150 per arm, 16.6 per site per arm).
Statistical analysis
All analyses were carried out using an intention-to-treat approach. Patients who dropped out from the study were considered to be ‘non-remitters’. Moderators analyses were carried out using the approach of Kraemer et al Reference Kraemer, Wilson, Fairburn and Agras28 and the methodological criteria set by Pincus et al Reference Pincus, Miles, Froud, Underwood, Carnes and Taylor29 and Sun et al Reference Sun, Briel, Busse, You, Akl and Mejza30 (see online supplement).
We computed three equivalent measures of treatment effect size: the success rate difference (SRD), that is the difference between the proportions of patients remitting with interpersonal counselling and with SSRIs, the number needed to treat (NNT), where NNT = 1/SRD, and the area under the curve (AUC), defined as the probability that a patient randomly assigned to interpersonal counselling will have a better outcome than a patient randomly assigned to SSRIs. The AUC ranges from 0 to 1, with a value of 0.5 if there is no difference between interpersonal counselling and SSRIs (the probability of the toss of a coin). The higher the AUC, the greater the advantage of interpersonal counselling over SSRIs, and the lower the AUC, the greater the advantage of SSRIs over interpersonal counselling. As a rule of thumb, small, medium and large effect sizes correspond to AUCs of 0.556, 0.638 and 0.714, to a NNT of about 9, 4 and 2 and SRDs of 0.1, 0.3 and 0.5. Reference Kraemer and Kupfer31
The moderator effect size is computed as the difference between the SRD in patients with and without the characteristics of interest.
Results
Primary analyses
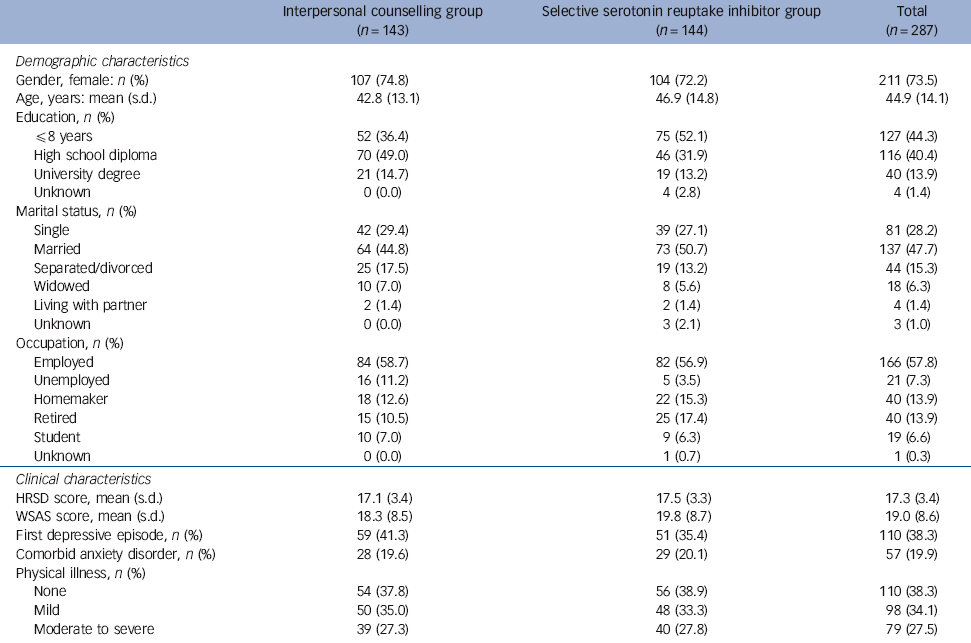
The study sample included 287 patients (Fig. 1) with a mean age of 44.9 years; 73.5% were female and 49.1% were married or living with a partner (Table 1). The proportion of patients who achieved remission at 2 months was significantly higher in the interpersonal counselling group compared with the SSRI group (intention-to-treat sample: 58.7% v. 45.1%, χ2 = 5.3, d.f. = 1, P = 0.021). This corresponds to an SRD = 0.136 (95% CI 0.021-0.251), an NNT = 7.3 (95% CI 4-46.5) and an AUC = 0.568 (95% 0.502-0.634). Of the patients who received the allocated intervention, 6/136 (4.4%) assigned to interpersonal counselling and 13/139 (9.3%) assigned to SSRIs discontinued treatment. Reasons for treatment discontinuation are shown in Fig. 1. In the course of the trial no severe side-effects were recorded.
Next we examined whether the sites differed in the overall proportion of individuals who remitted and treatment effect. Preliminary analyses were carried out including site and the interaction treatment site. Although one site proved to perform better than the others, no interaction effect was found (i.e. site was not a moderator of treatment effect). After these preliminary analyses, one of the nine research sites was excluded because the proportion of individuals who remitted was extremely low compared with the other sites and none of the patients recruited had remitted with interpersonal counselling, leading to problems in the estimation of the coefficients in the logistic regression models. This site had recruited a larger proportion of patients with moderate to severe physical illness (56%) compared with the others (⩽34%). Therefore, we carried out the subsequent secondary analyses on eight sites and 264 patients.

Fig. 1 Study flow chart.
Secondary analyses
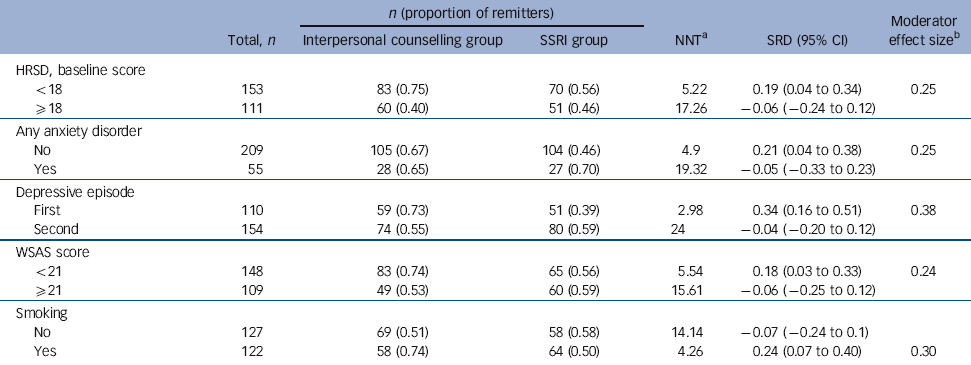
Potential moderators of remission were then examined in 13 separate logistic regression models. Five significant moderators of treatment outcome were found (Table 2). The strongest moderator was being in a first episode of depression, with an effect size of 0.38, which corresponds to a medium effect size according to Cohen’s standards.
Patients in their first episode were more likely to remit with interpersonal counselling, whereas those in a second episode were more likely to remit with SSRIs. The other four moderators were: baseline HRSD score, baseline WSAS score, comorbidity with anxiety disorder and smoking status. Patients with a baseline HRSD score <18, a WSAS score <21, without an anxiety disorder and those who smoked were more likely to remit with interpersonal counselling than with SSRIs. On the contrary those with a baseline HRSD score ⩾18, a WSAS score ⩾21, anxiety comorbidity and who did not smoke experienced a better outcome when treated with SSRIs compared with interpersonal counselling.
Table 1 Baseline characteristics of randomised patients
| Interpersonal
counselling group (n = 143) |
Selective serotonin
reuptake inhibitor group (n = 144) |
Total (n = 287) |
|
|---|---|---|---|
| Demographic characteristics | |||
| Gender, female: n (%) | 107 (74.8) | 104 (72.2) | 211 (73.5) |
| Age, years: mean (s.d.) | 42.8 (13.1) | 46.9 (14.8) | 44.9 (14.1) |
| Education, n (%) | |||
| ⩽8 years | 52 (36.4) | 75 (52.1) | 127 (44.3) |
| High school diploma | 70 (49.0) | 46 (31.9) | 116 (40.4) |
| University degree | 21 (14.7) | 19 (13.2) | 40 (13.9) |
| Unknown | 0 (0.0) | 4 (2.8) | 4 (1.4) |
| Marital status, n (%) | |||
| Single | 42 (29.4) | 39 (27.1) | 81 (28.2) |
| Married | 64 (44.8) | 73 (50.7) | 137 (47.7) |
| Separated/divorced | 25 (17.5) | 19 (13.2) | 44 (15.3) |
| Widowed | 10 (7.0) | 8 (5.6) | 18 (6.3) |
| Living with partner | 2 (1.4) | 2 (1.4) | 4 (1.4) |
| Unknown | 0 (0.0) | 3 (2.1) | 3 (1.0) |
| Occupation, n (%) | |||
| Employed | 84 (58.7) | 82 (56.9) | 166 (57.8) |
| Unemployed | 16 (11.2) | 5 (3.5) | 21 (7.3) |
| Homemaker | 18 (12.6) | 22 (15.3) | 40 (13.9) |
| Retired | 15 (10.5) | 25 (17.4) | 40 (13.9) |
| Student | 10 (7.0) | 9 (6.3) | 19 (6.6) |
| Unknown | 0 (0.0) | 1 (0.7) | 1 (0.3) |
| Clinical characteristics | |||
| HRSD score, mean (s.d.) | 17.1 (3.4) | 17.5 (3.3) | 17.3 (3.4) |
| WSAS score, mean (s.d.) | 18.3 (8.5) | 19.8 (8.7) | 19.0 (8.6) |
| First depressive episode, n (%) | 59 (41.3) | 51 (35.4) | 110 (38.3) |
| Comorbid anxiety disorder, n (%) | 28 (19.6) | 29 (20.1) | 57 (19.9) |
| Physical illness, n (%) | |||
| None | 54 (37.8) | 56 (38.9) | 110 (38.3) |
| Mild | 50 (35.0) | 48 (33.3) | 98 (34.1) |
| Moderate to severe | 39 (27.3) | 40 (27.8) | 79 (27.5) |
HRSD, Hamilton Rating Scale for Depression; WSAS, Work and Social Adjustment Scale.
Table 2 Moderators of remission by 2 months of treatment
| n (proportion of remitters) | Moderator effect sizeFootnote b |
|||||
|---|---|---|---|---|---|---|
| Total, n | Interpersonal counselling group | SSRI group | NNTFootnote a | SRD (95% CI) | ||
| HRSD, baseline score | ||||||
| <18 | 153 | 83 (0.75) | 70 (0.56) | 5.22 | 0.19 (0.04 to 0.34) | 0.25 |
| ⩾18 | 111 | 60 (0.40) | 51 (0.46) | 17.26 | −0.06 (−0.24 to 0.12) | |
| Any anxiety disorder | ||||||
| No | 209 | 105 (0.67) | 104 (0.46) | 4.9 | 0.21 (0.04 to 0.38) | 0.25 |
| Yes | 55 | 28 (0.65) | 27 (0.70) | 19.32 | −0.05 (−0.33 to 0.23) | |
| Depressive episode | ||||||
| First | 110 | 59 (0.73) | 51 (0.39) | 2.98 | 0.34 (0.16 to 0.51) | 0.38 |
| Second | 154 | 74 (0.55) | 80 (0.59) | 24 | −0.04 (−0.20 to 0.12) | |
| WSAS score | ||||||
| <21 | 148 | 83 (0.74) | 65 (0.56) | 5.54 | 0.18 (0.03 to 0.33) | 0.24 |
| ⩾21 | 109 | 49 (0.53) | 60 (0.59) | 15.61 | −0.06 (−0.25 to 0.12) | |
| Smoking | ||||||
| No | 127 | 69 (0.51) | 58 (0.58) | 14.14 | −0.07 (−0.24 to 0.1) | |
| Yes | 122 | 58 (0.74) | 64 (0.50) | 4.26 | 0.24 (0.07 to 0.40) | 0.30 |
SSRI, selective serotonin reuptake inhibitor; SRD, standardised rate difference; HRSD, Hamilton Rating Scale for Depression; WSAS, Work and Social Adjustment Scale.
a. The number needed to treat (NNT) is computed as 1/SRD. For instance, the NNT for patients with an HRSD <18 indicates that one would expect to treat 5 individuals with interpersonal counselling to have one more success (or one less failure) than if the same number were treated with SSRIs. Similarly, the NNT for patients with an HRSD ⩾18 indicates that one would expect to treat 17 individuals with SSRIs to have one more success (or one less failure) than if the same number were treated with interpersonal counselling.
b. The moderator effect size is computed as the difference between the SRD in patients with and without the characteristics of interest. For instance, the moderator effect size for the HRSD score is 0.19 - (−0.06) = 0.25. An effect size of 0.1, 0.3, 0.5 correspond to a d of 0.2, 0.5, 0.8 respectively, i.e. small, medium and large effect sizes by Cohen’s standards (see Kraemer & Kupfer).31
Two characteristics were identified as non-specific predictors of outcome: unmarried patients and those with no or mild comorbid physical illness were more likely to remit regardless of treatment assignment. Specifically, the percentage of remitters among unmarried v. married patients was 73% v. 57% with interpersonal counselling and 65% v. 42% with SSRIs, and the percentage of remitters among patients without v. with comorbid physical illness was 70% v. 40% with interpersonal counselling and 56% v. 48% with SSRIs.
To examine the extent to which the clinical moderators identified represent alternative indicators of severity, we analysed their bivariate correlations. Spearman’s correlation coefficients were close to zero (ρ = –0.085 to 0.107), except for baseline HRSD and baseline functional impairment (ρ = 0.327). This indicates that the variables are unrelated to each other and should not be combined because they provide independent information about severity.
Discussion
Interpersonal counselling proved to be more efficacious than SSRIs in primary care patients with mild to moderate depression in their first or second depressive episode. About 59% of participants achieved symptom remission in 2 months with interpersonal counselling compared with 45% with SSRIs. The NNT with interpersonal counselling to have one more remission than with SSRIs was seven, which corresponds to a moderate effect size.
We identified five clinical moderators of treatment outcome, including depression severity, functional impairment, anxiety comorbidity, previous depressive episodes and smoking habit. Specifically, mild depression, low functional impairment, being in a first depressive episode, having no comorbid anxiety disorder and being a smoker predicted a better outcome with interpersonal counselling. Whereas, moderate to severe depression, moderate to severe functional impairment, being in a second depressive episode, comorbid anxiety and not being a smoker predicted a better outcome with SSRIs. In addition, being unmarried and having no or mild comorbid physical illness proved to be two predictors of better outcome regardless of treatment assignment. The role of pharmacological and psychological interventions for mild depression is uncertain. There are very few trials in the literature that have compared brief psychological interventions with antidepressant treatment for depression in primary care. Reference Mynors-Wallis, Gath, Day and Baker27,Reference Mynors-Wallis, Gath, Lloyd-Thomas and Tomlinson32-Reference Chilvers, Dewey, Fielding, Gretton, Miller and Palmer34 In three out of four of these studies tricyclic antidepressants were prescribed and nowadays these are used infrequently in clinical practice. They all found no difference between the two approaches, in part because of low statistical power. Reference Bortolotti, Menchetti, Bellini, Montaguti and Berardi35 In contrast, our adequately powered study found a higher efficacy of interpersonal counselling compared with SSRIs, thus suggesting that many patients with depression in primary care would benefit from structured and focused psychological interventions.
Although it is crucial to identify the characteristics of patients who respond favourably to psychological interventions, available data on moderators of outcome on this topic are still lacking. There are few studies in the literature that have examined potential moderators of treatment effects in patient populations recruited from psychiatric settings and with moderate to severe and/or recurrent depression. These studies identified moderators of differential response to antidepressants v. psychotherapy, by testing the interaction (moderator treatment) effect in mixed-effect models Reference Kocsis, Leon, Markowitz, Manber, Arnow and Klein14,Reference Fournier, DeRubeis, Shelton, Hollon, Amsterdam and Gallop15 or in survival models. Reference Frank, Cassano, Rucci, Thompson, Kraemer and Fagiolini11 To our knowledge, only one primary care study has been conducted that examines which patient characteristics predict a differential response to psychological and pharmacological treatments, Reference Brown, Schulberg and Prigerson36 but the use of stratified analyses did not allow the identification of moderators of outcome. Our study is the first to investigate this issue in primary care using a large sample and an adequate methodological approach. Comparison of previous studies with our findings should be made keeping in mind differences in the clinical population examined.
Our data may suggest that patients experiencing mild and non-chronic depression could be initially treated with a psychological intervention. This approach is consistent with the NICE clinical guidance, which recommends a stepped-care model for the management of depression 7 and differentiate treatment options according to the severity and course of depressive symptoms. A previous study comparing paroxetine with cognitive therapy Reference Fournier, DeRubeis, Shelton, Hollon, Amsterdam and Gallop15 found that the presence of a life event associated with depression predicted a better response to the psychological intervention compared with antidepressants. We did not assess life events but they are often detectable in the first episode of depression, especially in women. Reference You and Conner37 We could hypothesise that psychological interventions actively work on the ability to manage stressful circumstances and may confer an advantage compared with drugs in new and mild cases associated with recent life events.
The role of comorbid anxiety as a moderator of remission was evaluated in two studies. Brown et al Reference Brown, Schulberg and Prigerson36 in a sample of primary care patients with depression found that patients without a history of comorbid anxiety were significantly more likely to recover with interpersonal psychotherapy compared with those on nortriptyline. On the other hand, Frank et al, Reference Frank, Cassano, Rucci, Thompson, Kraemer and Fagiolini11 in an out-patient psychiatric setting, found that the absence of comorbid anxiety disorder was a non-specific predictor of better outcome with SSRIs and interpersonal psychotherapy, but not a moderator. In that study, 69.3% of the patients had recurrent depression and 48.5% had lifetime comorbid anxiety disorder. It is possible that anxiety is a moderator only in patients with mild to moderate depression, where recurrence and comorbidity are less frequent. Thus, moderators of outcome should be confirmed in studies conducted in primary and secondary care settings.
Strengths and limitations of the study
The strengths of the present study are the relatively large sample size and the inclusion of patients with mild and non-chronic depression who are representative of the primary care setting, a group that are usually excluded from RCTs. Primary care is the health service entry point for the majority of people experiencing depressive disorders and therefore it is essential to collect data in this area. In addition, our attrition rate was very low (13.7%). The discontinuation rates of antidepressant or psychological treatments in primary care trials carried out in Germany and Finland were higher, ranging from 22 to 33%. Reference Salminen, Karlsson, Hietala, Kajander, Aalto and Markkula38,Reference Hegerl, Hautzinger, Mergl, Kohnen, Schütze and Scheunemann39 In these trials the mean HRSD score at baseline was equal or lower than in our sample, suggesting that patients with milder symptomatology might be less motivated to complete treatment. Moreover, evidence from a multicentre study comparing SSRIs with interpersonal psychotherapy in patients with moderate to severe depression, indicates a higher retention rate in Italy compared with the USA at 3 months (81.2% v. 73.9%). Reference Frank, Cassano, Rucci, Thompson, Kraemer and Fagiolini11
Several potential limitations of our study need to be acknowledged. First, interpersonal counselling might have been delivered in a different way at the study sites. In order to minimise site differences, we employed trained clinicians similar in background and years of experience and who attended a specific training programme. In addition, we addressed this point in the analytical strategy, by including site and site treatment effects in the models. This procedure makes it possible to estimate the treatment effect adjusted for differences in the case mix among sites and for possible site-specific factors, including beliefs about the effectiveness of the treatment strategies and clinical expertise. However, this strategy forced us to exclude one site.
Our results should be interpreted keeping in mind that patients with more than two treated depressive episodes in their personal history were excluded. Our findings are not generalisable to patients with chronic or more recurrent mood disorders. However, because response to treatment may vary across episodes, Reference Simon and Perlis9 our inclusion of homogeneous patients in their first or second episode allowed us to exclude a possible source of variability related to their previous treatment experience.
Moreover, our moderator analyses should be considered as exploratory and aimed at contributing useful information for designing future clinical studies. The effect size measures provided for the moderators identified in the present paper may serve as a guidance to researchers for estimating the sample size needed in confirmation studies. The design of these confirmation studies implies the selection of a group with the characteristic of interest and the comparison of outcomes in patients receiving different treatments.
Finally, we emphasise that the sample size of the present study was determined anticipating a difference of 15% in the response to the two study treatments at 2 months, whereas the detection of moderator effects requires larger sample sizes. Reference Brookes, Whitely, Egger, Davey, Mulheran and Peters40 Therefore, if the moderator analyses had been planned as the primary aim of the study then a broader recruitment would have been carried out. However, a less conservative criterion for the moderator analysis, set by Pincus et al Reference Pincus, Miles, Froud, Underwood, Carnes and Taylor29 prescribes at least 20 people in the smallest subgroup of the moderator, and this criterion is met for each of the moderators identified in the present study.
Implications for research
The therapists delivering interpersonal counselling were recruited to work in the primary care psychiatric consultation-liaison services for the research study. At present, similar therapists do not exist in primary care services in Italy and further research evaluating both the feasibility and cost-effectiveness of interpersonal counselling in comparison with SSRIs is needed.
In contrast to findings in the literature, Reference Fournier, DeRubeis, Shelton, Hollon, Amsterdam and Gallop15,Reference Van, Schoevers and Dekker41 we found that being unmarried was a predictor of remission regardless of treatment assignment. Treatment preference was not a moderator of treatment outcome. Another study carried out on patients with chronic major depression found an interactive effect of preference and treatment outcome, this was particularly apparent for those who expressed a preference for one of the monotherapies. Reference Kocsis, Leon, Markowitz, Manber, Arnow and Klein14 Unexpectedly, we found that smoking was a moderator of treatment outcome; smokers had a better outcome with interpersonal counselling than with SSRIs. These results should be considered preliminary and warrant replication and further investigation in future studies.
In conclusion, the results of this trial suggest that interpersonal counselling is an efficacious treatment for primary care patients with depression. Some patient characteristics including mild depression, first episode of depression and absence of anxiety disorder predicted a better outcome with interpersonal counselling. Should our results be confirmed in future studies, the identified moderators will help clinicians to define criteria for first-line treatment with a psychological intervention in order to personalise treatment according to patient characteristics and prevent poor treatment response.
Acknowledgements
The DEPICS (DEpression in Primary care: Interpersonal Counseling vs. Selective serotonin reuptake inhibitors) Group: Claudia Luciano, Loredana Lia, Dario Manganaro, Michele Magnani, Claudia Nespeca, Massimo Succu (Institute of Psychiatry, University of Bologna); Silvio Bellino, Filippo Bogetto, Monica Zizza (Department of Neurosciences, University of Torino); Niccolò Colombini, Marco Rigatelli, Elena Simoni, Enrico Tedeschini (Department of Neuroscience - TCR, University of Modena and Reggio Emilia); Federico Baranzini, Paola Bortolaso, Camilla Callegari, Giovanni Croci Marcello Diurni, Simone Vender (Department of Medicine, University of Insubria); Valentina Martinelli, Pierluigi Politi, Paola Sciarini (Department of Health Sciences, University of Pavia); Massimiliano Piselli, Roberto Quartesan (Department of Clinical and Experimental Medicine, University of Perugia); Antonello Bellomo, Michela De Salvia, Madia Ferretti, Salvatore Iuso, Annamaria Petito (Department of Medical Sciences, University of Foggia); Valeria Affatati, Orlando Todarello (Department of Psychiatry, University of Bari); Bernardo Carpiniello, Cecilia Contu, Federica Pinna (Department of Mental Health, University of Cagliari).
We would like to thank David Goldberg for ideas and support; Fabrizio Asioli for advice with the protocol development; Paolo Carbonatto and Tiziano Scarponi, members of Italian Society of General Practice board; and finally all the primary care physicians who referred patients for the study.






eLetters
No eLetters have been published for this article.