A key objective of early intervention services for psychosis is to reduce the period between the onset of frank psychosis and the initiation of its treatment, the duration of untreated psychosis (DUP). 1 Early intervention services include teams that engage people who are at high risk of developing psychosis, and have an at risk mental state (ARMS). A substantial proportion (20–35%) of those engaged at this stage will develop a first episode of psychosis within 3 years of presentation, Reference Fusar-Poli, Bonoldi, Yung, Borgwardt, Kempton and Valmaggia2 mostly schizophrenia spectrum psychoses. Reference Fusar-Poli, Bechdolf, Taylor, Bonoldi, Carpenter and Yung3 Clinical services for ARMS closely monitor their clients for early signs of psychosis and may therefore be able to detect the onset of psychosis at a relatively early stage, This might be expected to minimise the interval between the onset of illness and the initiation of treatment, Reference Valmaggia, McCrone, Knapp, Woolley, Broome and Tabraham4 although the putative benefit of high risk services has yet be demonstrated. One aim of the present study was to address this issue by comparing the DUP in such patients with that in patients who did not present to services until the first episode of psychosis.
There is a robust relationship between the DUP and clinical outcomes in psychosis, with a shorter DUP associated with better clinical and functional outcomes. Reference Hegelstad, Larsen, Auestad, Evensen, Haahr and Joa5 A related objective of the present study was to compare short-term clinical outcomes in these two groups, using frequency of hospital admission and frequency of compulsory treatment in the first year after the onset of psychosis as outcome measures.
Because people who present to clinical services for people with an ARMS are ‘help-seeking’, it is sometimes assumed that psychotic patients who were seen before the onset of illness may be unrepresentative of the overall patient population, and may have a relatively good prognosis. However, to our knowledge, the sociodemographic features of this group have never been compared to those of a general first-episode sample. The final aim of our study was to address this issue.
Our first hypothesis was that patients who had been engaged by services before the onset of psychosis would have a shorter DUP and better clinical outcomes than patients who had not been seen before the first episode. We then tested the hypothesis that the groups would differ on sociodemographic features that are thought to influence prognosis following the first episode.
Method
Study design
We compared the DUP, admissions rate and length of admission in people attending the Outreach and Support in South London Service (OASIS), a specialised community mental health service for people with an ARMS for psychosis Reference Fusar-Poli, Byrne, Badger, Valmaggia and McGuire6 with a first-episode sample that did not access help before becoming psychotic referred to the Lambeth Early Onset Crisis and Assessment Team (LEO-CAT). Reference Power, McGuire, Iacoponi, Garety, Morris and Valmaggia7 The LEO-CAT patients in the present study were assessed over a similar time period (2003–2005) to those whose first episode developed subsequent to management by OASIS (2002–2007).
Patients who developed psychosis after presenting in the prodromal phase
This group was drawn from 228 participants who had been recruited to OASIS and met the PACE criteria Reference Yung, Phillips, McGorry, McFarlane, Francey and Harrigan8 for an ARMS for psychosis. OASIS accepts self-referrals, and referrals from relatives and non-health agencies, as well as from health professionals, with most referrals coming from primary care. Reference Fusar-Poli, Byrne, Badger, Valmaggia and McGuire6 Most presented with attenuated psychotic symptoms alone (n = 159, 70%). A smaller proportion had both attenuated symptoms and a trait risk factor (n = 27, 12%), or attenuated symptoms plus a brief limited intermittent psychotic (BLIP) episode (n = 18, 8%), or a BLIP alone (n = 21, 9%). One participant (0.4%) had a BLIP and a trait risk factor and one (0.4%) reported attenuated symptoms, a trait risk factor and a BLIP; one was a missing value (0.4%). Of this sample, 43 subsequently developed a first episode of psychosis, most of whom (33/43) did so within 2 years. The mean time between presentation to OASIS and the onset of psychosis was 563 days (s.d. = 721), while the median was 345 days (25th and 75th percentiles = 135, 714).
The participants were regularly monitored for signs of frank psychosis for at least 2 years. They also received social and vocational support, psychological therapy and medication. Approximately 12% of patients disengage from the service. Reference Fusar-Poli, Byrne, Badger, Valmaggia and McGuire6 We recently carried out a follow-up study (median length of follow-up 4 years) and we were able to find information regarding current diagnosis and current use of services for all service users, including those who made a transition after disengaging with OASIS or after moving outside of the catchment area of the service. Among the OASIS service users who made a transition to psychosis, 10 individuals did so after the 2-year treatment window offered by OASIS.
If a participant developed frank psychosis, they were immediately referred to the local first-episode team (Lambeth Early Onset Service or Southwark Early Intervention Team Reference Power, McGuire, Iacoponi, Garety, Morris and Valmaggia7,Reference Reynolds, Wuyts, Badger, Fusar-Poli, McGuire and Valmaggia9 ), which then assumed clinical responsibility for the patient. Both teams offer similar comprehensive care packages to first-episode patients. All clinical decisions about the management of the patient, thereafter, including whether treatment with antipsychotic medication was indicated, the timing of treatment initiation, and the type of medication used, were made by the early intervention team (independent of OASIS). The same applied to decisions about whether the patients should be managed in the community or required hospital admission, and whether compulsory treatment was necessary.
Patients who did not present until the first episode of psychosis
These patients (n = 147) were referred to a crisis and assessment team for patients with first-episode psychosis (the LEO-CAT), serving in the same geographical catchment area in South London as OASIS. Reference Power, McGuire, Iacoponi, Garety, Morris and Valmaggia7 The team was designed to detect and engage patients (16–35 years old) as soon after the onset of first-episode psychosis as possible. Patients who had previously contacted mental health services with prodromal symptoms were excluded. Like OASIS, LEO-CAT accepted self-referrals, and referrals made by health and non-health agencies. Referrals were usually seen within a few days of referral. The majority of these patients had been referred by secondary care services.
Role of the funding source
The OASIS service and the LEO-CAT team were supported by the Guy's and St Thomas' Charitable Foundation, by the Mental Health Foundation and by the South London and Maudsley NHS Trust. The funding sources had no role in the design, conduct or analysis of this study.
Ethical approval
The study received ethical approval by the ethical committee of the South London and Maudsley Trust (study approval number 195/02).
Measures
The ARMS was defined according to PACE criteria Reference Yung, Phillips, McGorry, McFarlane, Francey and Harrigan8 as assessed using the comprehensive assessment of the ARMS (CAARMS), Reference Phillips, Yung and McGorry10 which has excellent validity and reliability. Reference Yung, Yuen, McGorry, Phillips, Kelly and Dell'Olio11 The onset of psychosis in the OASIS group was defined prospectively, using the criteria for transition to psychosis in the CAARMS. Reference Yung, Yuen, McGorry, Phillips, Kelly and Dell'Olio11 A first-episode diagnosis of psychosis was made by a member of the clinical team and confirmed by the team psychiatrist. The diagnosis of first-episode psychosis was confirmed by accessing the electronic clinical records of each patient after their transfer from OASIS to a local first-episode team. The electronic records were also used to define the date when antipsychotic treatment was initiated. All patients in the study (in both groups) were managed by the local health trust (South London And Maudsley NHS Trust) after the onset of psychosis, and all clinical information on the subjects was systematically recorded and stored on a single electronic database (Electronic Patient Journey System). The onset of psychosis in the LEO-CAT group was determined retrospectively, by a trained member of the clinical research team. In both groups, the DUP was defined as the time in days from the onset of psychosis to the start of treatment with antipsychotic medication.
Clinical outcomes in the 12 months following the first episode of psychosis were assessed by contacting each patients' responsible medical officer and by examining each patient's electronic patient record. These records also specified whether patients had been admitted to hospital, whether this involved use of the Mental Health Act, and the dates of admission and discharge for any stays in hospital.
Statistical analyses
Data were analysed using SPSS version 21. The Kruskal–Wallis non-parametric one-way analysis of variance and the Mann–Whitney U-test were used to examine the quantitative variables because the data were either not normally distributed or the sample size was small. Both one and two sample chi-square tests were used for categorical data.
Results
Demographic differences between OASIS and LEO-CAT patients
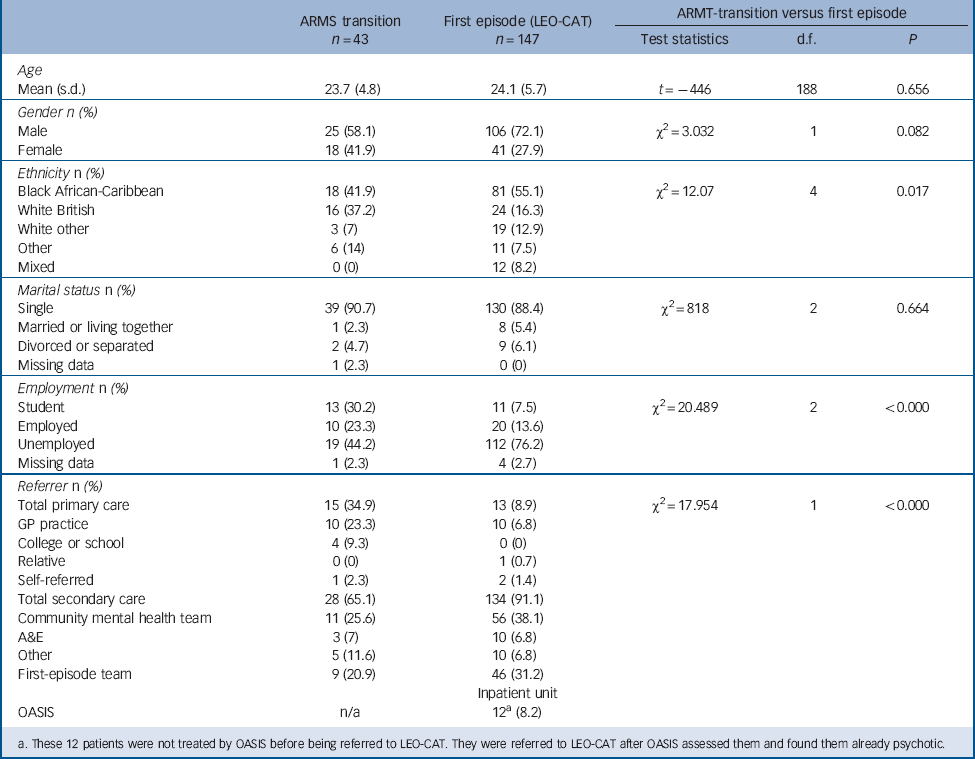
The two groups were similar in terms of age, gender and marital status, but patients who had not presented until their first episode were more likely to be unemployed and to belong to an ethnic minority group (Table 1). As expected patients who had presented in the prodromal phase were more likely to have been referred from primary care.
TABLE 1 Demographic characteristics of ARMS patient who made a transition to psychosis and first-episode patients
| ARMS transition n = 43 |
First episode (LEO-CAT) n = 147 |
ARMT-transition versus first episode | |||
|---|---|---|---|---|---|
| Test statistics | d.f. | P | |||
| Age | |||||
| Mean (s.d.) | 23.7 (4.8) | 24.1 (5.7) | t = −446 | 188 | 0.656 |
| Gender n (%) | |||||
| Male | 25 (58.1) | 106 (72.1) | χ2 = 3.032 | 1 | 0.082 |
| Female | 18 (41.9) | 41 (27.9) | |||
| Ethnicity n (%) | |||||
| Black African-Caribbean | 18 (41.9) | 81 (55.1) | χ2 = 12.07 | 4 | 0.017 |
| White British | 16 (37.2) | 24 (16.3) | |||
| White other | 3 (7) | 19 (12.9) | |||
| Other | 6 (14) | 11 (7.5) | |||
| Mixed | 0(0) | 12 (8.2) | |||
| Marital status n (%) | |||||
| Single | 39 (90.7) | 130 (88.4) | χ2 = 818 | 2 | 0.664 |
| Married or living together | 1 (2.3) | 8 (5.4) | |||
| Divorced or separated | 2 (4.7) | 9 (6.1) | |||
| Missing data | 1 (2.3) | 0 (0) | |||
| Employment n (%) | |||||
| Student | 13 (30.2) | 11 (7.5) | χ2 = 20.489 | 2 | <0.000 |
| Employed | 10 (23.3) | 20 (13.6) | |||
| Unemployed | 19 (44.2) | 112 (76.2) | |||
| Missing data | 1 (2.3) | 4 (2.7) | |||
| Referrer n (%) | |||||
| Total primary care | 15 (34.9) | 13 (8.9) | χ2 = 17.954 | 1 | <0.000 |
| GP practice | 10 (23.3) | 10 (6.8) | |||
| College or school | 4 (9.3) | 0 (0) | |||
| Relative | 0 (0) | 1 (0.7) | |||
| Self-referred | 1 (2.3) | 2 (1.4) | |||
| Total secondary care | 28 (65.1) | 134 (91.1) | |||
| Community mental health team | 11 (25.6) | 56 (38.1) | |||
| A&E | 3 (7) | 10 (6.8) | |||
| Other | 5 (11.6) | 10 (6.8) | |||
| First-episode team | 9 (20.9) | 46 (31.2) | |||
| Inpatient unit | |||||
| OASIS | n/a | 12Footnote a (8.2) | |||
a. These 12 patients were not treated by OASIS before being referred to LEO-CAT. They were referred to LEO-CAT after OASIS assessed them and found them already psychotic.
Duration of untreated psychosis
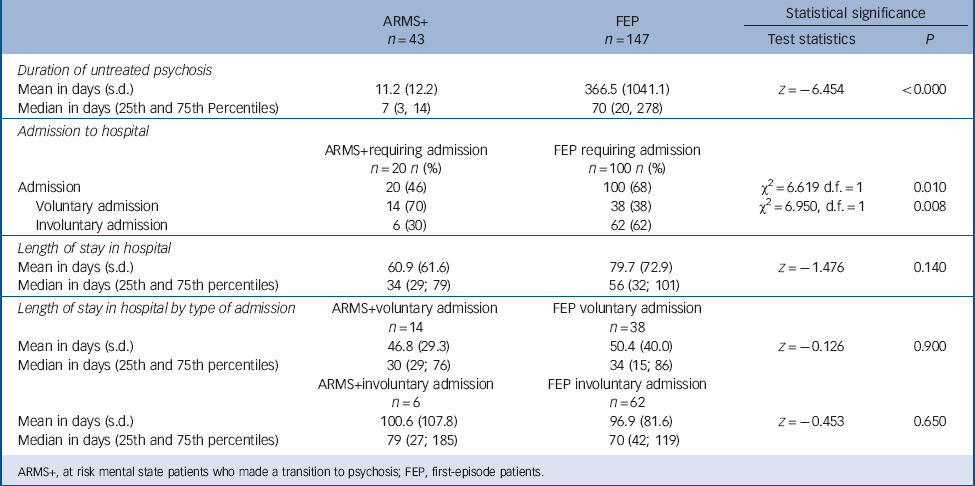
The mean DUP in patients who developed psychosis after being managed by OASIS was 11.2 days (s.d. = 12.2), while the median was 7 (25th and 75th Percentiles = 3, 14). The mean DUP for patients who presented with psychosis to LEO-CAT was 366.5 days (s.d. = 1041.1; median = 70; 25th and 75th percentiles = 20, 278) (Z = −6.454, P≤0.000; Table 2).
TABLE 2 DUP and admissions of ARMS patients who made a transition to psychosis and first-episode patients
| ARMS+ n = 43 |
FEP n = 147 |
Statistical significance | ||
|---|---|---|---|---|
| Test statistics | P | |||
| Duration of untreated psychosis | ||||
| Mean in days (s.d.) | 11.2 (12.2) | 366.5 (1041.1) | Z = −6.454 | <0.000 |
| Median in days (25th and 75th Percentiles) | 7 (3, 14) | 70 (20, 278) | ||
| Admission to hospital | ||||
| ARMS+requiring admission n = 20 n (%) |
FEP requiring admission n = 100 n (%) |
|||
| Admission | 20 (46) | 100 (68) | χ2 = 6.619 d.f. = 1 | 0.010 |
| Voluntary admission | 14 (70) | 38 (38) | χ2 = 6.950, d.f. = 1 | 0.008 |
| Involuntary admission | 6 (30) | 62 (62) | ||
| Length of stay in hospital | ||||
| Mean in days (s.d.) | 60.9 (61.6) | 79.7 (72.9) | Z = −1.476 | 0.140 |
| Median in days (25th and 75th percentiles) | 34 (29; 79) | 56 (32; 101) | ||
| Length of stay in hospital by type of admission | ARMS+voluntary admission n = 14 |
FEP voluntary admission n = 38 |
||
| Mean in days (s.d.) | 46.8 (29.3) | 50.4 (40.0) | Z = −0.126 | 0.900 |
| Median in days (25th and 75th percentiles) | 30 (29; 76) | 34 (15; 86) | ||
| ARMS+involuntary admission n=6 |
FEP involuntary admission n=62 |
|||
| Mean in days (s.d.) | 100.6 (107.8) | 96.9 (81.6) | Z = −0.453 | 0.650 |
| Median in days (25th and 75th percentiles) | 79 (27; 185) | 70 (42; 119) | ||
ARMS+, at risk mental state patients who made a transition to psychosis; FEP, first-episode patients.
Admission to hospital within 1 year from transition
Less than half (46%) of the 43 patients who developed psychosis after management by OASIS were admitted to hospital by the first-episode team that they were referred to. Most (14; 70%) were admitted voluntarily, with a minority (6; 30%) admitted on a compulsory basis under the Mental Health Act. The mean duration of admission was 60.9 days (s.d. = 61.6; median = 34; 25th and 75th percentiles = 29, 79).
By contrast, 100 (68%) of the 147 patients seen by LEO-CAT were admitted to hospital, and in most cases (74, 74%) this was compulsory admission under the Mental Health Act. The mean length of stay in hospital was 79.7 days (s.d. = 72.9; median 56; 25th and 75th percentiles = 32, 101).
Compared to those treated by LEO-CAT, the patients who originally presented to OASIS were less likely to require hospital admission (χ2 = 6.619; d.f. = 1; P = 0.010) and less likely to be admitted under the Mental Health Act (χ2 = 6.950; d.f. = 1; P≤0.008). The group differences in the duration of hospital admissions were not significant (z = −1.476; P = 0.140).
With regard to the effect of employment status at baseline and length of admission, the results showed no effect of employment status on length of admission in both groups (OASIS: χ2 = 1.899, d.f. = 2, P<0.387; LEO: χ2 = 6.607, d.f. = 3, P<0.086).
Discussion
This study explored whether there was a difference in DUP and admission rates between patients who engaged in treatment during the prodromal stage and subsequently developed psychosis and patients whose initial contact with mental health services was at the time of the first episode of psychosis. In line with our first hypothesis, the DUP in the prodromal group was much shorter than in those who presented with a first episode: on average 11 days, as opposed to approximately 1 year. Patients who presented in the prodromal stage were less likely to require admission following the onset of psychosis and less likely to require a compulsory admission.
The marked difference in DUP is particularly notable because LEO-CAT was a specialised team designed to detect first-episode psychosis as early as possible. Reference Power, McGuire, Iacoponi, Garety, Morris and Valmaggia7 This suggests that the difference is not attributable to a lack of awareness of the need for the early initiation of treatment in the comparison service. Indeed the DUP in the LEO-CAT group is comparable to that reported in other studies from the same geographical area (10.5 months; Reference Craig, Garety, Power, Rahaman, Colbert and Fornells-Ambrojo12 12 months Reference Morgan, Fearon, Hutchinson, McKenzie, Lappin and Abdul-Al13 ), from other parts of the UK (9 months Reference Drake, Haley, Akhtar and Lewis14 ), and internationally (12–24 months Reference Norman, Townsend and Malla15 ). We predicted that the DUP in people who were initially managed by a high risk service would be relative short because one of the main aims of clinical management at this stage is to closely monitor the first signs of psychosis. Moreover, people with an ARMS are relatively insightful and help-seeking, and show high levels of engagement with high risk services. Reference Green, McGuire, Ashworth and Valmaggia16,Reference Lappin, Morgan, Valmaggia, Broome, Woolley and Johns17 As a result they are generally likely to report changes in their mental state to the clinicians who are working with them. Once the onset of psychosis has been detected, the typically close working relationship between high risk services and local teams for patients with first-episode psychosis facilitates the rapid transfer of patients to the most appropriate service for the initiation of antipsychotic treatment.
Reducing the DUP is a central objective of early intervention in psychosis Reference Craig, Garety, Power, Rahaman, Colbert and Fornells-Ambrojo12 as there is a robust association between its length and subsequent clinical outcome with a shorter DUP being linked to a better prognosis. Reference Marshall, Lewis, Lockwood, Drake, Jones and Croudace18 However, whether a shorter DUP leads to a better clinical outcome or a short DUP is a feature of a subgroup of patients who are more likely to have a good outcome (or both) remains unclear. One way of resolving this issue is to examine the effect of clinical interventions that reduce the DUP on clinical outcomes. In the present study, we found that the outcome in the first year after engagement with a first-episode team was better in the patients who had first been engaged in the prodromal phase: they were less likely to be admitted to hospital and less likely to require a compulsory admission. This better outcome may have resulted from engagement with services in the prodromal phase and a shorter DUP. A recent study in Norway found in first-episode patients receiving early intervention that a shorter DUP was associated with fewer inpatient admissions at 2-year follow-up Reference Melle, Larsen, Haahr, Friis, Johannesen and Opjordsmoen19 and higher recovery rates at 10 years. Reference Hegelstad, Larsen, Auestad, Evensen, Haahr and Joa5
However, it is also possible that people who present to high risk services before the onset of psychosis represent a subgroup of the first-episode population with a relatively good prognosis. In the present study, the two groups were similar in age, gender and marital status. The patients who had first presented to a high risk service were more likely to have been referred from primary care. However, in this case it probably reflects the fact that primary care is the main source of referrals of people with an ARMS. Reference Fusar-Poli, Byrne, Badger, Valmaggia and McGuire6 Similarly, being employed is a good prognostic factor in first-episode patients, but the higher levels of employment in the group who first presented in the prodrome might simply be related to them presenting to services at an earlier stage of the disorder: the prodromal phase is when many patients with psychosis first become unemployed. Reference Valmaggia, McCrone, Knapp, Woolley, Broome and Tabraham4
Although the OASIS group reported better functioning, it is theoretically possible that having a psychosis prodrome is associated with a worse prognosis. Previous findings have shown that longer length of stay in hospital at admission in individuals who presents with an ‘acute onset’ are associated with a poorer outcome. Reference Queirazza, Semple and Lawrie20 However, while we found that individuals who engaged in the prodromal stage were less likely to be admitted to hospital and less likely to require the use of compulsory admission, no difference was found between the two groups in length of admission. Furthermore, in both groups, voluntary admission was associated with a shorter length of stay in hospital.
The local population in the catchment area of both OASIS and LEO-CAT has a high proportion of people from ethnic minorities and a very high incidence of psychosis, especially in those from Black ethnic minorities. Reference Fearon, Kirkbride, Morgan, Dazzan, Morgan and Lloyd21 Among those managed by OASIS, although there was a higher rate of people from Black minority ethnic groups compared to the general population rates for the same area (22% according to the 2011 census), there were no significant differences between ethnic groups in the risk of transition to psychosis, hospital admission and use of the Mental Health Act. The patients who first presented to high risk services were less likely to belong to an ethnic minority than those who presented at the first episode. The relationship between ethnicity and outcomes in psychosis is controversial, with some studies suggesting that it was relatively good in minority groups, Reference Chorlton, McKenzie, Morgan and Doody22 but other found the opposite. Reference Morgan, Lappin, Heslin, Croudace, Doody and Donoghue23 The DUP in first-episode patients, which is usually related to clinical outcome, has not been found to differ between ethnic groups. Reference Morgan, Fearon, Hutchinson, McKenzie, Lappin and Abdul-Al13,Reference Chorlton, McKenzie, Morgan and Doody22,Reference Anderson, Flora, Archie, Morgan and McKenzie24 It is thus difficult to know whether the better clinical outcomes observed in the OASIS group in the present study were a result of the lower proportion of patients from minority groups.
Our results seem to indicate that early detection services like OASIS may have lower efficacy in socially deprived areas. Indeed, our recent work in an inner London prison identified a large number of individuals experiencing ARMS and early psychosis who in the community were not help-seeking and had not been detected by conventional health services. Reference Jarrett, Craig, Parrott, Forrester, Winton-Brown and Maguire25 Furthermore, a recent study analysing the 10-year outcome of first-episode patients found that social exclusion is present before the onset of the first episode and that it is still poor for the majority of cases at 10-year follow-up. Reference Morgan, Lappin, Heslin, Donoghue, Lomas and Reininghaus26
Limitations
Patients who presented in the prodrome were ascertained from a clinical service that is limited to people who are help-seeking, whereas there was no such restriction on the comparison group that it is possible that the group differences in DUP and clinical outcome were related to the sampling of a subgroup of first-episode patients with a relatively good prognosis. However, even if this were the case, the data suggest that high risk services provide a means of improving clinical outcomes in patients who present before the onset of psychosis. A further limitation is the lack of data regarding the use of illegal substances; however, in a recent study looking at the use of cannabis in ARMS, we found that lifetime cannabis use was common but not related to transition to psychosis. However, we did find that in the ARMS who used cannabis frequent use, early-onset use and continued use after clinical presentation were associated with transition to psychosis. Reference Valmaggia, Day, Jones, Bissoli, Pugh and Hall27 A final limitation to the study was that in the first-episode sample no data were available regarding the psychosis prodrome. Future studies should ascertain how many of the individuals presenting directly to the first episode psychosis service actually have a psychosis prodrome and compare those with people service users presenting during the ARMS stage.
Clinical implications
The benefits of clinical services for people at high risk for psychosis are usually conceptualised in terms of reducing the risk of psychosis, and ameliorating the presenting symptoms and social and vocational dysfunction. A further benefit may be that these services provide a very effective way of detecting the first signs of psychosis and minimising the interval between the onset of illness and the initiation of treatment.
Funding
The authors acknowledge financial support from the National Institute for Health Research (NIHR) Biomedical Research Centre for Mental Health at South London and Maudsley NHS Foundation Trust and King's College London. The views expressed are those of the authors and not necessarily those of the NHS, the NIHR or the Department of Health.
Acknowledgements
Our special thanks go to the staff and service users of OASIS and LEO-CAT.





eLetters
No eLetters have been published for this article.