The first 2–3 years following a first episode of psychosis may represent a critical period during which crucial biological and psycho-social changes are imprinted in the mind of the patient, thus forming the predictors of the long-term outcome (Reference Birchwood, Todd and JacksonBirchwood et al, 1998). According to this theory, psycho-social interventions counteracting the damaging effects of the negative predictors at this stage may have a disproportionate positive impact compared with interventions later in the course of the illness. The basis for a lasting result is, however, that the intervention is sustained for a period of years (Reference Linszen, Dingemans and LeniorLinszen et al, 2001). The Danish National Schizophrenia Project investigates precisely the effects of early, rapid and year-long sustained intervention after the first signs of psychosis.
Background of the study
The Danish National Mental Health Service has a long tradition of equal access to and free treatment for all inhabitants regardless of their location, income, ethnicity or religion. Psychiatric treatment is organised according to sector, and there is no private psychiatric hospital in Denmark. The National Mental Health Service has 4100 beds, approximately 105 community mental health centres and 125 private specialists in psychiatry in the adult psychiatry section. General practitioners and private specialists treat only a small percentage of patients with schizophrenia and related disorders. All specialists in psychiatry complete the same theoretical courses as part of their specialist training. The pathways to treatment for patients with psychosis and the quality of their psychiatric care can be considered to be equal in all psychiatric units throughout the country.
Our study was designed to test whether supportive psychodynamic psychotherapy in addition to treatment as usual or an integrated, assertive psychosocial and educational treatment programme could improve the course of illness compared with treatment as usual. We wanted to explore whether the treatment methods in our investigation, including treatment as usual, would help patients to improve their psychic and social functioning, and whether the interventions would lead to greater improvement than usual treatment alone, with respect to symptoms and social functioning.
METHOD
Study design
The study was a prospective, comparative longitudinal study with a minimum intervention period of 2 years and assessments of participants at baseline and 1, 2 and 5 years after inclusion. Participants were allocated to three different treatments (Table 1).
-
(a) Treatment 1 (n=119): patients were offered scheduled, manualised, supportive individual psychotherapy (one 45-min session per week, for a period of 1–3 years) and/or group psychotherapy (one 60-min session per week for a period of 1–3 years), in addition to treatment as usual. Antipsychotic medication was given in doses based on individual needs.
-
(b) Treatment 2 (n=139): patients were offered an integrated treatment package — a scheduled, 2-year programme consisting of assertive community treatment, psycho-educational multifamily treatment (according to McFarlane et al (Reference McFarlane, Lukens and Link1995)), in which four to six families, including the patients, meet for 1½ h every second week for 18 months), social skills training (concerning medication, self-management, coping with symptoms, and conversational, problem-solving and conflict-solving skills) and anti-psychotic medication (low-dose strategy). This project has been described in detail elsewhere (Reference Jorgensen, Nordentoft and AbelJorgensen et al, 2000; Reference Nordentoft, Jeppesen and AbelNordentoft et al, 2002).
-
(c) Treatment 3 (n=304): patients were offered treatment as usual, consisting of many different therapies — psychological methods, medication, medical advice and treatment by the in-patient and day hospital treatment service — administered according to patients’ needs and the available resources of the clinic at the time of treatment, not delivered in any pre-scheduled manner.
Table 1 Comparison of the intervention strategies

| Treatment 1 Supportive psychodynamic psychotherapy | Treatment 2 Integrated treatment programme | Treatment as usual | |
|---|---|---|---|
| Medication | Yes, but no pre-scheduled strategy | Yes, non-specified low-dose strategy | Yes, but no pre-scheduled strategy |
| Assertive outreach | No | Yes | No |
| Multifamily group therapy | No | Yes (McFarlane therapy) | No |
| Social skills training | No | Yes (concerning medication, self-management, coping strategies, conversational skills, problem- and conflict-solving skills) | No |
| Individual psychotherapy | Yes1 | No | ? |
| Group psychotherapy | Yes1 | No | ? |
| Social support | Yes | Yes, assertive | Yes |
Study participants
The principal inclusion period started on 1 October 1997 and lasted 2 years. Participants were consecutively referred patients, aged 16–35 years, with a first psychotic episode of a schizophrenic spectrum disorder diagnosed by ICD–10 criteria (F20–29; World Health Organization, 1992). Written informed consent had to be obtained from all patients, although not necessarily in the initial phase of the treatment. Patients were excluded if they had a diagnosis of mental retardation or organic brain damage, or were not sufficiently proficient Danish speakers.
Patients with a first episode of psychosis, admitted to either an in-patient unit or a community mental health centre, were systematically assessed within 2 weeks and included if they fulfilled the above criteria. The assessment was conducted by members of a trained, independent research team connected to the centre. Inclusion or exclusion was decided by the team.
Treatment allocation
Two centres (52% of the sample) randomised the patients individually to either treatment 2 or treatment as usual. In three centres (13% of the sample), patients from the first part of the intake were allocated to treatment 1 and those from the second part of the intake to treatment as usual (Fig. 1). This was necessitated by the requirement to complete the treatments being studied in a relatively short period with sufficient numbers of patients. In five centres (14% of the sample), patients were only offered treatment treatment 1 (in addition to usual treatment), and six centres (21% of the sample) offered only usual treatment to their patients.

Fig. 1 Study profile.
Assessments
At baseline the following data were collected:
-
(a) demographic and socio-economic data;
-
(b) diagnosis according to ICD—10 research criteria, determined by clinical observation and judgement and confirmed by the Operational Criteria Checklist for Psychotic Illness (OPCRIT; Reference McGuffin, Farmer and HarveyMcGuffin et al, 1991);
-
(c) clinical status, determined by Global Assessment of Functioning (GAF; American Psychiatric Association, 1994), the Strauss—Carpenter Outcome Scale (Strauss & Carpenter, Reference Strauss and Carpenter1974, Reference Strauss and Carpenter1977) and the Positive and Negative Syndrome Scale (PANSS; Reference Kay, Fiszbein and OplerKay et al, 1987).
The test battery was repeated in years 1 and 2, and is currently being repeated in year 5. All assessments were conducted by trained, independent interviewers.
The assessment of treatment as usual encompassed a detailed registration of the elements of treatment for each patient during the intervention period and 3 years after, covering seven domains of the psychiatric treatment: continuity in doctor–patient relationship; treatment frames (in-patient or out-patient); medication; psychotherapy; milieu therapy; short-term family groups for the relatives; and training in daily activities.
Intervention treatments
The two intervention treatments were conducted according to manuals. Regular supervision was provided for both kinds of intervention to enhance adherence to the manualised procedures. The manualised psychodynamic psychotherapies for group treatment (Lajer & Valbak, unpublished, available from the authors on request in Danish) and for individual treatment (Rosenbaum & Thorgaard, unpublished, available from the authors on request) aimed at a realistic cognition of psychosocial events (attitudes towards illness, realistic social goals, and emotional reactions in interpersonal relationships) and were focused on emotions, intrapsychically as well as interpersonally. The psycho-educational family treatment was manualised according to Reference McFarlane, Lukens and LinkMcFarlane et al, 1995. The focus of each session was problem-solving and the development of skills to cope with aspects of the illness. The social skills training was based on selected modules from Liberman et al (Reference Liberman, Wallace and Jacobs1986) and Bellack et al (Reference Bellack, Mueser and Gingerich1997).
Statistical analysis
The multicentre structure of this study had to be taken into account in the analyses since two patients treated at the same centre might not give independent observations. Logistic regression with generalised estimating equations (Reference Hardin and HilbeHardin & Hilbe, 2003; Reference Donner and KlarDonner & Klar, 2004) was used for dichotomous variables and linear mixed models were used for continuous variables. These methods were used to compare the three study groups at baseline, at 1 year and for differences between base-line and 1 year. In the calculation of changes from baseline to year 1, the analysis was adjusted for baseline values. Members of the independent research teams met twice a year and rated videotape of patient assessments. The results of 12 rating sessions were used for the calculation of reliability. It was measured for PANSS and GAF by calculating the intraclass correlation coefficient (ICC; Reference Bartko and CarpenterBartko & Carpenter, 1976). All tests were two-sided, and all analyses were executed by using SAS software version 8.2. Owing to multiple comparisons, the Bonferroni correction was used in the interpretation of the results at baseline and for the pairwise comparisons at 1 year of treatment.
RESULTS
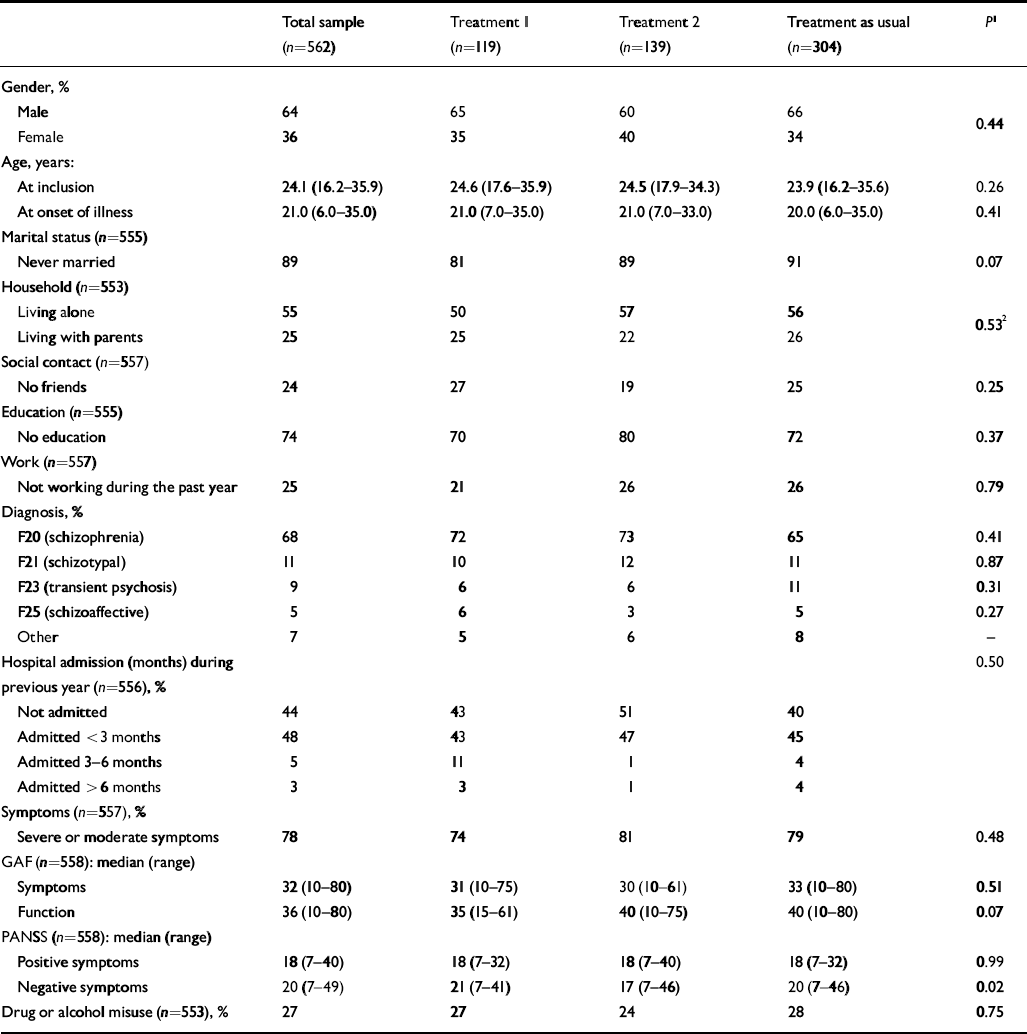
A total of 562 patients (361 men and 201 women) met the inclusion criteria and gave informed consent to participation in the study. Most were of Nordic origin (92%). The socio-demographic and clinical data of the sample at inclusion are shown in Table 2. (Patients who had been admitted to the hospital system in the year preceding the outbreak of psychosis had all been given diagnoses of non-psychotic conditions.)
Table 2 Demographic, clinical and social baseline data
| Total sample (n=562) | Treatment 1 (n=119) | Treatment 2 (n=139) | Treatment as usual (n=304) | P 1 | |
|---|---|---|---|---|---|
| Gender, % | |||||
| Male | 64 | 65 | 60 | 66 | 0.44 |
| Female | 36 | 35 | 40 | 34 | |
| Age, years: | |||||
| At inclusion | 24.1 (16.2-35.9) | 24.6 (17.6-35.9) | 24.5 (17.9-34.3) | 23.9 (16.2-35.6) | 0.26 |
| At onset of illness | 21.0 (6.0-35.0) | 21.0 (7.0-35.0) | 21.0 (7.0-33.0) | 20.0 (6.0-35.0) | 0.41 |
| Marital status (n=555) | |||||
| Never married | 89 | 81 | 89 | 91 | 0.07 |
| Household (n=553) | |||||
| Living alone | 55 | 50 | 57 | 56 | 0.532 |
| Living with parents | 25 | 25 | 22 | 26 | |
| Social contact (n=557) | |||||
| No friends | 24 | 27 | 19 | 25 | 0.25 |
| Education (n=555) | |||||
| No education | 74 | 70 | 80 | 72 | 0.37 |
| Work (n=557) | |||||
| Not working during the past year | 25 | 21 | 26 | 26 | 0.79 |
| Diagnosis, % | |||||
| F20 (schizophrenia) | 68 | 72 | 73 | 65 | 0.41 |
| F21 (schizotypal) | 11 | 10 | 12 | 11 | 0.87 |
| F23 (transient psychosis) | 9 | 6 | 6 | 11 | 0.31 |
| F25 (schizoaffective) | 5 | 6 | 3 | 5 | 0.27 |
| Other | 7 | 5 | 6 | 8 | - |
| Hospital admission (months) during | 0.50 | ||||
| previous year (n=556), % | |||||
| Not admitted | 44 | 43 | 51 | 40 | |
| Admitted <3 months | 48 | 43 | 47 | 45 | |
| Admitted 3-6 months | 5 | 11 | 1 | 4 | |
| Admitted >6 months | 3 | 3 | 1 | 4 | |
| Symptoms (n=557), % | |||||
| Severe or moderate symptoms | 78 | 74 | 81 | 79 | 0.48 |
| GAF (n=558): median (range) | |||||
| Symptoms | 32 (10-80) | 31 (10-75) | 30 (10-61) | 33 (10-80) | 0.51 |
| Function | 36 (10-80) | 35 (15-61) | 40 (10-75) | 40 (10-80) | 0.07 |
| PANSS (n=558): median (range) | |||||
| Positive symptoms | 18 (7-40) | 18 (7-32) | 18 (7-40) | 18 (7-32) | 0.99 |
| Negative symptoms | 20 (7-49) | 21 (7-41) | 17 (7-46) | 20 (7-46) | 0.02 |
| Drug or alcohol misuse (n=553), % | 27 | 27 | 24 | 28 | 0.75 |
Reliability of study measures
The ICC for PANSS positive symptoms was 0.70, for PANSS negative symptoms it was 0.74, for GAF symptoms it was 0.56 and for GAF function it was 0.74. The ICC agreement is thus good for PANSS and GAF function, and moderate but acceptable for GAF symptoms.
Comparison between the three groups at baseline
The groups were similar at baseline in terms of age, diagnosis, PANSS positive score, GAF symptom score, GAF function score, GAF total score, and admission/non-admission to hospital during the year before inclusion in the study (i.e. admitted with a diagnosis of a psychiatric illness other than F20 psychosis). A significant lower PANSS negative symptom score for the treatment 2 group disappeared when the Bonferroni correction was used.
At year 1, data were obtained from 450 patients (80%). These participants did not differ from the group for whom data were not obtained, in terms of age, gender, diagnosis, GAF and PANSS scores. Furthermore, there was no statistical difference between the three investigated groups. In the F20 group of patients with schizophrenia, 80% participated in the rating at year 1.
Improvement in symptoms and social function after 1 year of treatment
At year 1, a significant improvement was found for GAF symptom score, GAF function score, GAF total score, PANSS positive score (P<0.0001) and PANSS negative score (P<0.04) when the three treatment groups were sampled together. More than half of the sample (54%) had more contact with friends in year 1 compared with the year prior to baseline, 18% had more work and 58% had fewer symptoms.
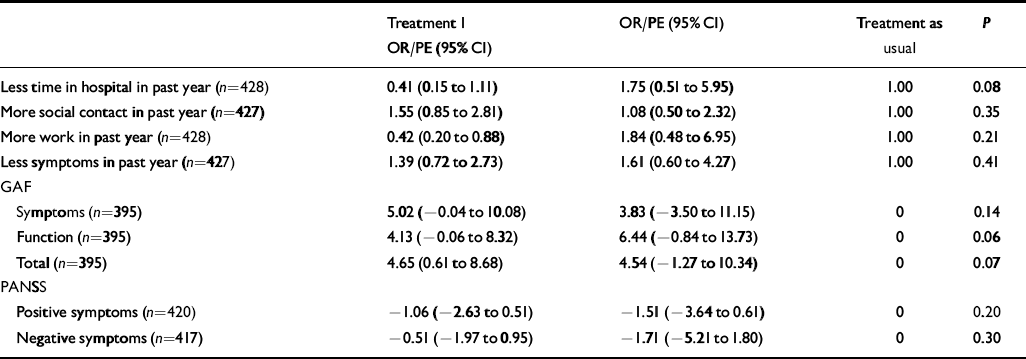
Comparing the improvements in the three groups at year 1 did not reveal any significant difference between each of the two intervention groups and the usual treatment group (Table 3). Non-significant tendencies were found for hospital admission and GAF function. The reduction in time spent in hospital (ν. the year before inclusion) was greater in patients receiving treatment 2 or treatment as usual than in patients receiving treatment 1 (P=0.08), whereas treatments 1 and 2 both improved the patients’ GAF function scores more than treatment as usual (P = 0.06). Comparisons between treatment 1 and treatment as usual were in favour of the intervention: GAF total (P=0.03). With the Bonferroni correction, however, this difference disappeared. When we controlled for drug and alcohol misuse as a confounding factor, we found that both intervention treatments produced significant improvements in GAF function score (P=0.02) and PANSS negative score (P=0.02).
Table 3 Changes from baseline to year 1: results from generalised linear mixed model (odds ratio) or linear mixed model (parameter estimate), adjusted for baseline value
| Treatment 1 OR/PE (95% CI) | OR/PE (95% CI) | Treatment as usual | P | |
|---|---|---|---|---|
| Less time in hospital in past year (n=428) | 0.41 (0.15 to 1.11) | 1.75 (0.51 to 5.95) | 1.00 | 0.08 |
| More social contact in past year (n=427) | 1.55 (0.85 to 2.81) | 1.08 (0.50 to 2.32) | 1.00 | 0.35 |
| More work in past year (n=428) | 0.42 (0.20 to 0.88) | 1.84 (0.48 to 6.95) | 1.00 | 0.21 |
| Less symptoms in past year (n=427) | 1.39 (0.72 to 2.73) | 1.61 (0.60 to 4.27) | 1.00 | 0.41 |
| GAF | ||||
| Symptoms (n=395) | 5.02 (-0.04 to 10.08) | 3.83 (-3.50 to 11.15) | 0 | 0.14 |
| Function (n=395) | 4.13 (-0.06 to 8.32) | 6.44 (-0.84 to 13.73) | 0 | 0.06 |
| Total (n=395) | 4.65 (0.61 to 8.68) | 4.54 (-1.27 to 10.34) | 0 | 0.07 |
| PANSS | ||||
| Positive symptoms (n=420) | -1.06 (-2.63 to 0.51) | -1.51 (-3.64 to 0.61) | 0 | 0.20 |
| Negative symptoms (n=417) | -0.51 (-1.97 to 0.95) | -1.71 (-5.21 to 1.80) | 0 | 0.30 |
Five people died by suicide during year 1 (0.9% of the whole sample), including two unexplained deaths; no difference was found between suicide rates in the intervention groups and in the usual treatment group.
DISCUSSION
From clinical experience it might be assumed that the psychopharmacological treatment accounted for much of the improvement during the first year of treatment. That contributes in part to the understanding of the lack of statistical difference between the specific interventions and treatment as usual. Moreover, in the initial phase of the treatment of patients with a first episode of psychosis, in which the creation of an alliance with the patient is of major importance, the active ingredients of the specific interventions used in this study were not expected to have worked for a sufficient amount of time to make a significant difference. For instance, at the time of the year 1 assessment, some of the intended-to-treat patients might have only received less than 6 months of individual psychodynamic psychotherapy or of social skills training, and major changes were not expected within that time span.
Even though our study participants had only been exposed for a limited time to the specific intervention, it is an interesting (although from clinical experience not unexpected) finding that patients who do not misuse alcohol or drugs are receptive to the specific interventions to such an extent that for some variables it results in a statistically significant difference between the improvements in the intervention groups compared with treatment as usual. This may serve as a guideline to the selection of the patients who might benefit from psychotherapy in the initial phase of treatment.
The multisite study
Conducting a prospective, long-term study involving 16 centres is a laborious process with many pitfalls (Reference KraemerKraemer, 2000). The strengths of the multisite model in our study are the quantity of consecutively referred patients; the inclusion of different types of treatment centres (small/big, urban/rural, university/non-university) in all three groups being compared; the percentage of the Danish population covered by the study (approximately 45%); the comparison of two different therapies with standard treatment of supposedly good quality; and that the treatment was conducted mainly by therapists with standard training rather than master clinicians. The study was thus both naturalistic and realistic, and mimicked the actual conditions of the Danish national health system at the time of the health system's development (1998–2000). This supports the generalisations of the results as well as the possibility of recommending in the future the use of both clinical measures and treatment methods in the day-to-day practice of psychiatry. Furthermore, it is in accordance with recent reports emphasising that pragmatically defined public health, integrated treatment programmes and effectiveness studies in many ways are more useful in the planning of schizophrenia prevention than narrowly defined regulatory models and efficacy studies (Reference Lebowitz and PearsonLebowitz & Pearson, 2001; Reference Gilbody, Wahlbeck and AdamsGilbody et al, 2002).
An additional positive element of the long-term multisite project is the establishment of a network of centres that can collaborate through adopting the same treatment methods, the same measurement scales and upholding the same treatment values. The collaboration requires an idealistic approach and has to overcome the potential lack of funding. The reward for each centre is the provision of training of interviewers in the use of psychometric scales and of therapists in the chosen methods of treatment. As a result of these collaborative efforts, the reliability of the ratings of PANSS and GAF was satisfactory.
Comparison with other studies
Previous studies of first-episode psychosis have found a positive outcome for various integrated treatments compared with standard treatment (Reference Martindale, Bateman and CroweMartindale et al, 2000: pp. 200–292). These integrated treatment programmes all differ in content, combination of treatment forms or length of treatment, and it is hard to compare them directly with our study. Furthermore, the active curative factors in these studies have been hard to distil. Possible curative factors in our integrated treatment programme (treatment 2) might be the rapid, consistent and long-term involvement of the treatment team; the specific targeting of the patient's return to work, school or other educational programme; and the specific targeting of the attempt to enable in-patients to progress to out-patient treatment.
Previous studies comparing psychodynamic psychotherapy and standard treatment are few and have diverse results, some in favour of the psychodynamic treatment (Reference Karon and VandenBosKaron & VandenBos, 1981), others against (Reference MayMay, 1968). Positive outcome has mainly been associated with treatment by experienced therapists or master clinicians (Reference Karon and VandenBosKaron & VandenBos, 1981) and/or with the formation of a therapeutic alliance (Reference Frank and GundersonFrank & Gunderson, 1990). However, none of the previous studies concerned patients with first-episode psychosis, and it is by no means given that we can extend the findings from these previous studies of psychotherapy of schizophrenia to our sample.
One limitation of our study is the lack of individual randomisation of all patients. It was, however, the price we had to pay in order to include many different types of centre. Another limitation to the interpretation of our results is the lack of 1-year data for 20% of the patients. This was not expected, but cannot be considered exceptionally high (Reference Gilbody, Wahlbeck and AdamsGilbody et al, 2002). No difference in adherence to the project was found between the treatment 1 group (0.86) and the treatment 2 group (0.81). However, a greater number of patients remaining in the study after 1 year might have increased the possibility of a significant effect of the interventions.
Finally, the study was constricted by the use of a limited battery of tests and by not including detailed analysis of possible factors confounding the effect of therapy, such as duration of untreated psychosis, premorbid social function, interpersonal attitude and behaviour in school. We did, however, include drug and alcohol misuse, and controlling the data for these confounding factors changed some measures in favour of the two treatment interventions.
Clinical Implications and Limitations
CLINICAL IMPLICATIONS
-
▪ An integrated assertive psychosocial and educational treatment programme and supportive psychodynamic psychotherapy may each improve outcome after 1 year of treatment for people with first-episode psychosis, compared with treatment as usual.
-
▪ Controlling the data for patients with drug and alcohol misuse gives rise to a statistically significant improvement of social functioning and negative symptoms in favour of the specific interventions compared with standard treatment.
-
▪ A large-scale, naturalistic, multisite study, with therapists with standard training, can be conducted with an acceptable withdrawal rate from the intervention groups and good reliability in the assessment of patients. This may have implications for the use of measures in the day-to-day practice in psychiatry.
LIMITATIONS
-
▪ The patient sample was not randomised individually.
-
▪ The extended test battery could not be used for the whole sample.
-
▪ There was no control of confounding factors except for alcohol and drug misuse.
Acknowledgements
The authors thank the following participatingcentres: Broenderslev. Psychiatric Hospital; Psychiatric Unit Herning; Psychiatric Hospital in. Aarhus; Psychiatric Hospital Middelfart; Psychiatric Hospital Nykoebing Sj.; Psychiatric Departments in Roskilde County; Slagelse Hospital Department of. Psychiatry; Holbaek Hospital Department of Child and Adolescent Psychiatry; Sct Hans Hospital Roskilde Department U7; Dianalund; Psychiatric Center. Glostrup; Bispebjerg Hospital Department of Psychiatry U and E; Frederiksborg. County Hospital Hilleroed.
A 6-year grant from the Danish Ministry of Health made it possible to carry. the project through to the treatment phase. Participating counties have also. contributed financially.







eLetters
No eLetters have been published for this article.