Introduction
Major depression (MD), forecast to become the second leading cause of disability worldwide by 2020 (Lopez & Murray, Reference Lopez and Murray1998), is characterized by diverse clinical symptoms (Lewis, Reference Lewis1934; APA, 1994), a subset of which became symptomatic criteria in the Diagnostic and Statistical Manual of Mental Disorders, fourth edition (DSM-IV) based on clinical observation and expert consensus (Kendler et al. Reference Kendler, Munoz and Murphy2010).
Whether the symptoms of MD can be well captured with one psychopathological dimension or require multiple dimensions has been long debated (Lewis, Reference Lewis1934; Grinker et al. Reference Grinker, Miller, Sabshin, Nunn and Nunnally1961; MacFadyen, Reference MacFadyen1975). Recent analyses suggest that multiple factors are required to explain the co-occurrence of current depressive symptoms (e.g. Shafer, Reference Shafer2006; Romera et al. Reference Romera, Delgado-Cohen, Perez, Caballero and Gilaberte2008; Bech et al. Reference Bech, Fava, Trivedi, Wisniewski and Rush2011; Van Loo et al. Reference Van Loo, de Jonge, Romeijn, Kessler and Schoevers2012). A twin study found three genetic factors underlying the DSM-IV A criteria for MD (Kendler et al. Reference Kendler, Aggen and Neale2012).
The DSM-IV nine MD A diagnostic criteria evolved from the Feighner and Research Diagnostic Criteria (Feighner et al. Reference Feighner, Robins, Guze, Woodruff, Winokur and Munoz1972; Kendler et al. Reference Kendler, Munoz and Murphy2010), whose unidimensionality was later supported by empirical evidence from factor analysis using community samples (Muthén, Reference Muthén1989; Aggen et al. Reference Aggen, Neale and Kendler2005). A meta-analysis of the factor structure for four commonly used depression questionnaires has reported two common factors including the general depression severity factor and a somatic symptom factor (Shafer, Reference Shafer2006). A recent review paper examined the results of both exploratory factor analysis (EFA) and confirmatory factor analysis (CFA) studies of nine DSM-IV criteria for MD (Van Loo et al. Reference Van Loo, de Jonge, Romeijn, Kessler and Schoevers2012). Results were diverse and did not provide conclusive evidence for any single typology of depressive symptoms. The authors noted that this literature was difficult to interpret because of differences in sample characteristics and specific items included in the factor analyses.
This study seeks to determine the factor structure of the symptoms of MD as reported for the lifetime worst episode in a very large sample of Han Chinese women with recurrent depression. Our sample size is sufficient to utilize EFA in a random split-half of the sample. The results are then verified using CFA in the second split-half.
We performed factor analyses on three sets of items: (i) the nine DSM-IV A criteria for MD (APA, 1994); (ii) 14 items representing the disaggregated DSM-IV criteria (i.e. increased and decreased appetite and weight, insomnia or hypersomnia, and psychomotor agitation or retardation); and (iii) 27 items, consisting of the 14 above mentioned plus 13 more detailed assessments of DSM criteria and symptoms of melancholia, anxiety and Beck's cognitive trio (Beck et al. Reference Beck, Rush, Shaw and Emery1980).
Method
Subjects for this report came from the China, Oxford and VCU (Virginia Commonwealth University) Experimental Research on Genetic Epidemiology (CONVERGE) study (Flint et al. Reference Flint, Chen, Shi and Kendler2012). The analysis was based on the final phenotypic sample of 6008 cases recruited from 57 mental health centers and psychiatric departments of general hospitals in 45 cities in 23 provinces in China.
Subjects were females aged 30–60 years who reported two or more lifetime episodes of MD meeting DSM-IV criteria (APA, 1994). Their age at onset was between 14 and 55 years and each had four Han Chinese grandparents. Cases were excluded if they had a history of mania, psychosis outside of mood episodes or mental retardation, or had abused drugs or alcohol before their first depressive episode. The samples were primarily collected for a large genome-wide association study. Twin studies have suggested that the heritability of MD is higher in females and the genetic risk factors are not identical across sexes (Kendler et al. Reference Kendler, Gardner, Neale and Prescott2001, Reference Kendler, Gatz, Gardner and Pedersen2006). We therefore studied women only to reduce genetic heterogeneity.
Subjects were interviewed for an average of 2 h using a computerized assessment system that included assessment of psychopathology, demographic and personal characteristics, and psychosocial functioning. All interviewers, junior psychiatrists, postgraduate medical students, or senior nurses, were trained by the CONVERGE team for a minimum of 1 week. Interviews were recorded and a proportion of them edited for quality control. The study protocol was approved by the Ethical Review Board of Oxford University and the ethics committees in participating Chinese hospitals.
Measures
The diagnosis of MD was established with the Composite International Diagnostic Interview (CIDI; World Health Organization lifetime version 2.1; Chinese version), which classifies diagnoses according to DSM-IV criteria (APA, 1994). The interview was originally translated into Mandarin by a team of psychiatrists in Shanghai Mental Health Center, with the translation reviewed and modified by members of the CONVERGE team. The interview was supplemented by sections from interviews used in the Virginia Adult Twin Study of Psychiatric and Substance Use Disorders (VATSPSUD) (Kendler & Prescott, Reference Kendler and Prescott2006), and other items of interest to the investigators.
All interview sections, with built-in skip patterns, were computerized into a bilingual system of Mandarin and English that was installed on laptops. Once an interview was completed, a backup file containing the interview data was generated and, together with the audio record of the interview, uploaded to a server in Beijing and then transferred to Oxford. As operationalized in the CIDI, the symptoms analysed were based on those reported by the subject for the self-identified worst lifetime episode of MD.
Statistical methods
The total sample was randomly divided into two halves. The first sample was used to perform an EFA and the second was used to perform a CFA for validating the EFA symptom structure. Factor analyses were performed using the Mplus program (Muthén & Muthén, Reference Muthén and Muthén1998), with a weighted least squared means and variance adjusted (WLSMV) estimator that is designed for ordinal data (Flora & Curran, Reference Flora and Curran2004). EFA was performed using a geomin oblique rotation. CFA model fit was evaluated using the Tucker–Lewis index (TLI; Tucker & Lewis, Reference Tucker and Lewis1973), the comparative fit index (CFI; Bentler, Reference Bentler1990) and the root mean square error of approximation (RMSEA; Steiger, Reference Steiger1990). For the TLI and CFI, values between 0.90 and 0.95 are considered acceptable, and ⩾0.95 as good. For the RMSEA, good models have values ⩽0.05. To confirm that the split-sample procedure produced two random subsamples, we formally tested in Mplus for measurement invariance in our CFA data on the nine DSM-IV criteria. When we constrained factor loadings to be identical in the two subsamples, the robust χ 2 difference, as expected, was not significant.
Results
EFA and CFA on nine MD DSM-IV A criteria
Endorsement frequencies for the nine MD DSM-IV A criteria for MD were uniformly high and similar in our two subsamples (Table 1). An EFA in sample 1 produced two eigenvalues exceeding unity. The first factor displayed higher loadings primarily on the somatic symptoms of depression and less prominently on mood symptoms, and reflected a ‘general depressive symptom’ factor. The second factor had highest loadings on suicidal ideation and worthlessness/guilt, and reflected a ‘cognitive symptoms’ factor (Table 1). The inter-factor correlation coefficient was + 0.53. The best-fit CFA solution, two factors with all variable loadings ⩾0.30 from the EFA, had an excellent fit (RMSEA = 0.015, CFI = 0.98, TLI = 0.97), which was substantially better than those obtained with one factor (RMSEA = 0.031, CFI = 0.89, TLI = 0.86). The inter-factor correlation was + 0.78. The loadings for the mood criteria A1 was stronger on the first factor and much weaker on the second factor in the CFA compared with the EFA. This factor, which still represented ‘general depressive symptoms’, had high loadings on seven of the nine A criteria. Factor 2, the ‘cognitive symptoms’ factor, had high loadings on the two criteria of worthlessness/guilt and suicidal ideation.
Table 1. Item percentage endorsement frequency on sample 1 and sample 2 for the nine DSM-IV criteria for major depression and loadings estimated from an EFA on sample 1 and a CFA on sample 2 a
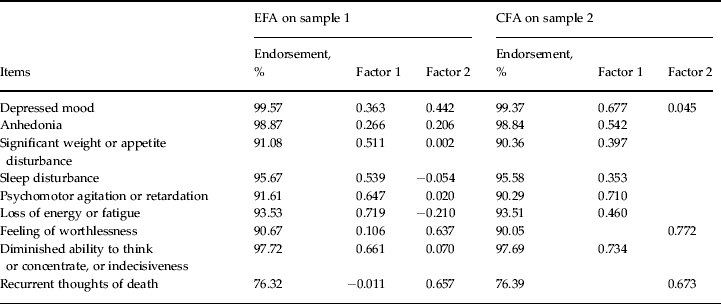
DSM-IV, Diagnostic and Statistical Manual of Mental Disorders, fourth edition; EFA, exploratory factor analysis; CFA, confirmatory factor analysis.
a Two-factor solution with loading cut-off at 0.3.
EFA and CFA on the 14 disaggregated DSM-IV A criteria
The frequencies of item endorsement in the 14 disaggregated DSM-IV A criteria were similar in the two subsamples and more variable than with the nine criteria (Table 2). Atypical vegetative symptoms were endorsed by 7–13% of patients. The scree plot for the EFA analyses showed four factors with eigenvalues exceeding 1 and a clear ‘elbow’ at three factors. Furthermore, a solution with three factors was considerably more interpretable than one with four and resulted in factors reflecting ‘weight/appetite symptoms’, ‘general depressive symptoms’ and ‘sleep disturbance’ (Table 2) with modest inter-factor correlations (Table 3). In our CFA analyses (which produced the most interpretable results when including all EFA loadings ⩾0.30), the three-factor solution had better-fit indices (RMSEA = 0.032, CFI = 0.94, TLI = 0.93) than the four-factor solution (RMSEA = 0.035, CFI = 0.93, TLI = 0.91), validating our interpretation of the EFA. Loadings from the CFA were comparable with those found in the EFA, identifying three broadly similar factors. Inter-factor correlations were modest except between factors 1 and 3, which equaled −0.44 (Table 3).
Table 2. Item percentage endorsement frequency on sample 1 and sample 2 for the 14 disaggregated DSM-IV criteria for major depression and loadings estimated from an EFA on sample 1 and a CFA on sample 2 a

DSM-IV, Diagnostic and Statistical Manual of Mental Disorders, fourth edition; EFA, exploratory factor analysis; CFA, confirmatory factor analysis.
a Items selected to load on CFA factors are based on EFA loading with a cut-off of 0.3.
Table 3. Inter-factor correlations for the EFA and CFA for the two-factor nine-item, three-factor 14-item and the five-factor 27-item factor analyses of the symptoms of major depression
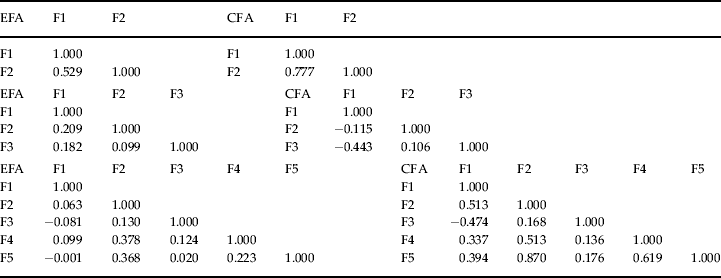
EFA, Exploratory factor analysis; CFA, confirmatory factor analysis; F1, factor 1; F2, factor 2; F3, factor 3; F4, factor 4; F5, factor 5.
EFA and CFA on all 27 individual symptoms assessed during worst depressive episode
Endorsement rates were variable for the 27 depression-related symptoms individually assessed during the worst lifetime episode and similar in our two subsamples (Table 4). More than 80% of our sample endorsed both key melancholic symptoms (e.g. lack of mood reactivity and distinct mood quality) and items assessing Beck's cognitive triad (e.g. hopelessness and worthlessness) indicating the clinical severity of the reported depressive episodes.
Table 4. Item percentage endorsement frequency on sample 1 and sample 2 for the 27 depressive symptoms and loadings estimated from an EFA on sample 1 and a CFA on sample 2 a
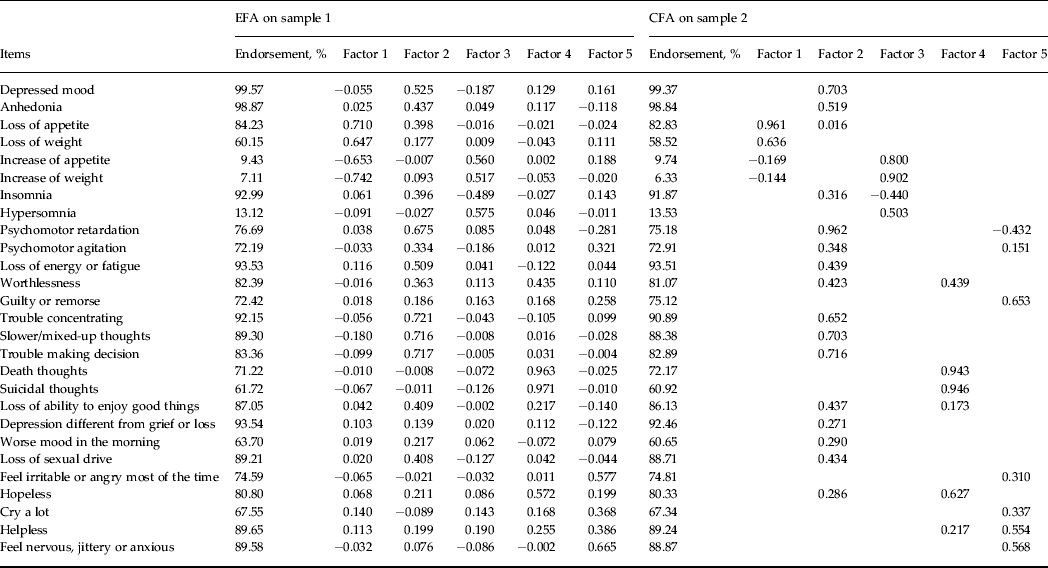
EFA, Exploratory factor analysis; CFA, confirmatory factor analysis.
a Items selected to load on CFA factors are based on EFA loading with a cut-off of 0.2.
The factor structure of these 27 items was initially examined by EFA (Table 3), resulting in eight eigenvalues exceeding 1 without a clear ‘elbow’ in the scree plot. With seven- and eight-factor solutions, estimated residual variances of some items became negative, indicating over-extraction. The five-factor EFA model was clinically more sensible than the six-factor solution. Similar to the results from the 14-item analysis, the first factor reflected ‘weight/appetite symptoms’ (Table 4). The second factor was also similar to that seen with the 14-item solution with a more prominent loading on psychomotor retardation. We called this the ‘general retarded depressive symptom’ factor. The third factor had highest loadings on the ‘atypical vegetative symptoms’ of increased appetite and weight, and hypersomnia. The fourth factor had prominent loadings on suicidal symptoms and Beck's triad of helplessness, hopelessness and worthlessness, and was called a ‘suicidal/hopeless’ factor. The fifth factor had prominent loadings on ‘agitated depressive symptoms’ including agitation, nervousness, guilt, irritability and crying. Inter-factor correlations were generally modest (Table 3), with the highest observed between the general depressive and suicidal/hopeless factors (+0.38).
In the CFA, when the number of factors equalled six or greater, standard errors of model parameter estimates as well as the factor scores could not be computed, which is also an indication of factor over-extraction. Both four-factor and five-factor solutions (with items of EFA loading cut-off of ⩾0.2) described the data well, with the five-factor solution resulting in slightly superior fits (RMSEA = 0.030, CFI = 0.953, TLI = 0.946 v. RMSEA = 0.030, CFI = 0.950, TLI = 0.943), again congruent with our clinical interpretation. The loadings closely resembled those found in the EFA. The general retarded depressive symptom factor had notable loadings (with absolute value ⩾0.2) on by far the most items (n = 15) with higher loadings for typical severe retarded depressive symptoms including several of the melancholic symptoms. The agitated depressive and suicidal/hopeless factors were next, with prominent loadings on six and five symptoms, respectively. The atypical vegetative and weight/appetite symptom factors were the smallest, with prominent loadings on four and two symptoms, respectively.
Discussion
The goal of this study was to clarify the structure of the symptoms of MD experienced during the lifetime worst depressive episodes reported by Han Chinese women with recurrent DSM-IV MD (APA, 1994) ascertained in clinical settings throughout China. We conducted an EFA in a random split-half of the sample and then verified those results by CFA in the second random half. We conducted these analyses with: (i) the nine DSM-IV A criteria for MD; (ii) 14 items representing the disaggregated DSM-IV A criteria; and (iii) all 27 symptoms independently assessed in our interview for the worst lifetime depressive episode. Our preliminary EFA results on one half of our sample were consistently verified by the findings from CFA in the second random half.
Our study produced three major findings. First, we detected two factors underlying the nine DSM criteria for MD. The two ‘cognitive’ DSM criteria – worthlessness/guilt and suicidal ideation formed their own factor. Our results are convergent with prior analyses from the VATSPSUD (Lux & Kendler, Reference Lux and Kendler2010) that detected evidence for covert heterogeneity within the DSM-IV A criteria for MD, particularly between somatic and cognitive criteria (Lux & Kendler, Reference Lux and Kendler2010), as well as results from the Beck depression rating scale that cognitive symptoms form a factor independent of the somatic and affective features of depression (Beck et al. Reference Beck, Ward, Mendelson, Mock and Erbaugh1961). These findings suggest that in clinically depressed individuals, the DSM-IV A criteria for MD – which have changed very little since the days of the Research Diagnostic Criteria (Spitzer et al. Reference Spitzer, Endicott and Robins1975) and DSM-III (APA, 1980) – in fact reflect two inter-correlated but meaningfully distinct rather than one underlying psychopathological dimension.
It is particularly useful to compare our findings with those reported by Van Loo et al. (Reference Van Loo, de Jonge, Romeijn, Kessler and Schoevers2012) who reviewed the results for nine studies of EFA and principal component analysis of DSM MD criteria. Of note, the sample size in our study is substantially greater than that of all nine of these prior studies. Contrary to the report of Aggen et al. (Reference Aggen, Neale and Kendler2005), all the studies reviewed detected at least two factors. Most commonly, as seen in our CFA, the core items of sad mood and loss of interest loaded on the first factor. However, the other features of the results of the individual studies were quite varied, further illustrating how dependent the results of factor analysis can be on the nature of the items examined and the sample studied.
Second, consistent with several prior multivariate analyses of MD criteria (Kendler et al. Reference Kendler, Eaves, Walters, Neale, Heath and Kessler1996; Sullivan et al. Reference Sullivan, Kessler and Kendler1998; Matza et al. Reference Matza, Revicki, Davidson and Stewart2003) and depressive symptom scales (Bech et al. Reference Bech, Fava, Trivedi, Wisniewski and Rush2011), when atypical vegetative symptoms are well represented among the items, they form a distinct dimension of depressive symptomatology (Stewart et al. Reference Stewart, McGrath, Rabkin and Quitkin1993). However, contrary to most prior studies of clinical criteria, perhaps because of our statistical power, we found that items reflecting sleep difficulty were moderately independent from the other vegetative symptoms reflecting changes in weight/appetite and formed their own factor. However, our results are consistent with a meta-analysis of the Hamilton Rating Scale for Depression that demonstrated separate factors in clinically depressed subjects for sleep problems and weight loss (Shafer, Reference Shafer2006). Sleep disturbances in severe MD may form an important psychopathological dimension at least partially independent of other neurovegetative changes (Kupfer, Reference Kupfer1995).
Third, when we added to the DSM-IV disaggregated A criteria a range of other common depressive symptoms, a richer and potentially more informative picture emerged of the clinical complexity of severe depressive illness. We found replicated evidence for five depressive symptom factors. The largest factor contained prominent loadings on traditional mood changes, psychomotor retardation and several melancholic criteria, with modest loadings on certain cognitive symptoms. Items in this general retarded depressive symptom factor reflected six of the nine DSM IV A criteria: sad mood, anhedonia, psychomotor changes, worthlessness, fatigue, and concentration problems.
The next largest factor reflected agitated and anxious depressive symptoms, with additional high loadings on guilt, crying and feelings of helplessness. These symptoms resemble those describing the agitated depression (Koukopoulos & Koukopoulos, Reference Koukopoulos and Koukopoulos1999) that was recognized as a subtype in the Research Diagnostic Criteria (Spitzer et al. Reference Spitzer, Endicott and Robins1975). These findings provide further evidence that anxiety symptoms can be a prominent part of the presentation of some forms of severe MD and may form a potentially important independent symptom factor as has been proposed for DSM-5 (First, Reference First2011).
Perhaps the most interesting factor to emerge had prominent loadings on suicidal symptoms and Beck's triad of hopelessness, worthlessness and (somewhat more weakly) helplessness (Beck & Alford, Reference Beck and Alford2008). Consistent with a large body of influential work (Beck et al. Reference Beck, Rush, Shaw and Emery1980; Beck & Alford, Reference Beck and Alford2008), our results suggest that cognitive symptoms reflecting distorted views of the self, the world and the future form an important and largely independent dimension of depressive symptomatology which in this ascertained population is very closely related to suicidal ideation. These results also suggest that criterion A7 for MD does not reflect a unitary psychopathological construct, as its two major subcomponents – worthlessness and guilt – loaded on different depressive symptom factors.
Finally, similar to the analyses of the 14 items, the factor analyses of our 27 items identified two factors reflecting typical and atypical vegetative symptoms with weight/appetite and sleep items loading on separate factors.
Both our EFA and CFA utilized oblique rotations so that the depressive symptoms factors could inter-correlate. This approach produces a picture that, while more complex, is probably more realistic. For technical reasons (because CFA sets to zero low item loadings which partly capture inter-factor associations in an EFA), inter-factor correlations are typically higher in CFA than EFA. Because psychiatric symptoms are likely to be ‘messy’ and truly reflect more than one underlying dimension, the inter-factor correlations estimated with the more complex EFA factor loading patterns are probably more accurate than those produced by the stronger simple structure imposed in the CFAs. We would therefore emphasize only three of these correlations, all positive, as being especially noteworthy: between the general depressive and cognitive symptom factors in our nine-item analyses and, in our 27-item analyses between our general retarded depressive symptom factor and both the suicidal/hopeless and agitated depressive symptom factors.
Our results differ from two prior factor analyses of the nine DSM A criteria for MD in community samples (Muthén, Reference Muthén1989; Aggen et al. Reference Aggen, Neale and Kendler2005), both of which detected only a single factor with substantially higher loadings on all criteria. Perhaps our ability to detect a second cognitive factor is related to our larger sample size and the greater clinical severity of our subjects. We are not aware of prior studies using similar methods and symptom content for our 14- and 27-item analyses. However, it is helpful to contextualize our findings by reviewing selectively earlier and more recent attempts to derive symptomatic factors from clinically depressed individuals. A classic factor analytic study of Grinker et al. (Reference Grinker, Miller, Sabshin, Nunn and Nunnally1961) of a wide variety of symptoms in 96 hospitalized depressed patients produced two factors similar to those we detected dominated by loadings on: (i) tension, anxiety and feeling jittery; and (ii) feeling hopeless, helpless, unworthy, and a failure (Grinker et al. Reference Grinker, Miller, Sabshin, Nunn and Nunnally1961). The initial description of the Hamilton Rating Scale for Depression reported on 49 depressed patients four symptom factors, three of which resemble those we recovered including factors dominated by high loadings on: (i) suicide and guilt; (ii) agitation and anxiety; and (iii) insomnia and weight loss (Hamilton, Reference Hamilton1960). Friedman, in another early study of 170 cases of psychotic depression using Grinker's 60-item depression rating scale, reported four symptom-dominated factors, three of which resembled factors that we isolated with high loadings on: (i) guilt and low self-esteem; (ii) appetite and sleep disturbance; and (iii) irritability, physical complaints and agitation (Friedman et al. Reference Friedman, Cowitz, Cohen and Granick1963). An early analysis of the Beck Depression Scale on 254 hospitalized depressed patients yielded three interpretable factors of which two resembled those we had found with prominent loadings on: (i) guilt, self-accusation, sense of failure, self-punitive wishes and self-hate; and (ii) weight loss, loss of appetite, and sleep disturbance (Weckowicz et al. Reference Weckowicz, Muir and Cropley1967).
Turning to more recent studies, in a meta-analysis of four popular self-report depression questionnaires, Shafer (Reference Shafer2006) noted the consistency with which neurovegetative symptoms of depression loaded on an independent factor from other clinical symptoms. Bech et al. (Reference Bech, Fava, Trivedi, Wisniewski and Rush2011), using principal component analysis applied to the 17-item Hamilton Rating Scale for Depression (HAMD17) scores from 4041 patients from the STAR*D (Sequenced Treatment Alternatives to Relieve Depression) study, found two factors, one reflecting general depressive severity and the second vegetative symptoms of weight, appetite and sleep disturbance. They also analysed the Inventory of Depressive Symptomatology (IDS-C30) in the same sample also reporting two factors. The first factor again included a broad array of depressive symptoms, while the second factor had notable loadings on panic, arousal, agitation, but also sleep difficulties (Parker, Reference Parker2007). Finally, in 1049 primary care patients with MD, Romero et al. (Reference Romera, Delgado-Cohen, Perez, Caballero and Gilaberte2008) found four factors in the Zung Depression Scale, three of which were quite similar to factors we extracted with notable loadings on: (i) emptiness, hopelessness and suicidal rumination; (ii) agitation, irritability and crying spells; and (iii) decreased appetite and weight loss.
Our subjects were Han Chinese women with recurrent and severe MD recruited through clinical settings. We cannot be sure of the degree to which these results would extrapolate to men, to other ethnic groups, or to the milder forms of illness or symptom dimensions studied in community samples. However, the World Health Organization examined patients seeking care for depression in five international sites including East Asia and concluded that the clinical similarities of individuals far outweighed the modest cross-cultural differences (Sartorius et al. Reference Sartorius, Jablensky, Gulbinat and Ernberg1980). The factor structure of the Beck Depression Scale in Japan is very similar to that seen in Western populations (Kojima et al. Reference Kojima, Furukawa, Takahashi, Kawai, Nagaya and Tokudome2002). Prior studies in this sample have shown that MD is associated, in a similar manner, with a range of risk factors previously demonstrated in Western samples including childhood sexual abuse (Cong et al. Reference Cong, Li, Shao, Chen, Wu, Shang, Wang, Liu, Liu, Gao, Li, Wu, Deng, Liu, Sang, Liu, Rong, Gan, Li, Li, Pan, Li, Cui, Sun, Liu, Liu, Zhao, Zhang, Zhang, Chen, Wang, Li, Chen, Lin, Kendler, Flint and Shi2011), neuroticism (Xia et al. Reference Xia, He, Li, Xie, Zhu, Chen, Shen, Zhang, Wei, Chen, Shen, Zhang, Gao, Li, Ding, Shen, Wang, Cao, Liu, Zhang, Duan, Bao, Ma, Zhou, Luo, Zhang, Liu, Li, Jin, Zhang, Liang, Chen, Zhao, Li, Chen, Shi, Kendler, Flint and Wang2011), stressful life events (Tao et al. Reference Tao, Li, Xie, Wang, Qiu, Wu, Sun, Wang, Tao, Zhao, Tian, Zhang, Gao, Niu, Li, Liu, Liu, Zhang, He, Rong, Gan, Li, Chen, Pan, Li, Cui, Han, Ma, Xie, Jin, Li, Zhang, Tan, Zhang, Guan, Shi, Chen, Kendler, Flint and Gao2011) and low parental warmth (Gao et al. Reference Gao, Li, Cai, Chen, Shen, Ni, Wei, Qiu, Zhu, Liu, Lu, Chen, Niu, Tang, Yang, Wang, Cui, Xia, Liu, Zhang, Zhao, Guo, Pan, Chen, Luo, Sun, Xiao, Chen, Zhao, He, Lv, Guo, Liu, Li, Shi, Flint, Kendler and Tao2012), and has similar patterns of co-morbidity with anxiety disorders (Li et al. Reference Li, Shi, Yang, Gao, Li, Tao, Wang, Zhang, Gao, Liu, Li, Li, Liu, Wang, Zhang, Lv, Wang, Chen, Hu, Sun, Shi, Chen, Xie, Flint, Kendler and Zhang2012) and dysthymia (Sang et al. Reference Sang, Li, Su, Yang, Wu, Shang, Zhang, Shen, Sun, Guo, Li, Yan, Zhang, Wang, Liu, Liu, Zhang, Wang, Yu, Pan, Li, Hu, Yang, Huang, Xie, Wang, Liu, Lv, Chen, Zhang, Dang, Shi, Chen, Kendler, Flint and Li2011).
Epidemiological studies have found that rates of MD are lower in East Asia than in most other countries (Parker et al. Reference Parker, Gladstone and Chee2001). There has been supporting evidence that the Chinese tend to deny depression or express it somatically (Kleinman, Reference Kleinman1982; Parker et al. Reference Parker, Gladstone and Chee2001). The leading theory is that this is a result of cultural stoicism and high levels of stigmatization. A recent epidemiological study in Taiwan supports this hypothesis. Individuals reporting MD were much more impaired than subjects reporting MD in parallel US studies and were only one-third as likely to seek professional help (Liao et al. Reference Liao, Chen, Lee, Lung, Lai, Liu, Lin, Yang and Chen2012). This might also explain the clinical severity of our sample that was ascertained entirely through psychiatric treatment centers.
While it is possible that the patterns of depressive illness described in our sample are unique to this subgroup, this seems unlikely given prior cross-cultural research and the many parallels between our findings and previous empirical studies of MD in Western populations.
To our knowledge, this is the first study to examine the underlying symptom pattern of depression in the Han Chinese population using a carefully screened clinical sample of this size. The fact that we have identified common factors from Western samples provides evidence that there is more similarity than dissimilarities in depression in China and in Western countries. Future studies are needed to compare samples recruited using the same criteria from diverse ethnic groups to address more definitively the role played by culture and ethnicity in shaping the symptom dimensions of depression.
Strengths and limitations
These results should be considered in the light of our potential methodological strengths and limitations. Four strengths are noteworthy. First, our phenotypic assessment was standardized and detailed with careful interview training and several quality-control features. Second, our sample was much larger than any previous similar effort and allowed us, with good power, to utilize EFA and CFA methods in split-half samples. Third, the goal of our sample collection strategy was to minimize heterogeneity that could add noise to our analysis. So, this sample was of a single sex with uniform ethnicity who suffered from severe recurrent depressive illness. Furthermore, drug and alcohol abuse were vanishingly rare in our sample of Han Chinese women, reducing a further major source of confound; also only 5% of them ever smoked. Fourth, the sample had a minimum age of 30 years and a mean age of 44.4 (s.d. = 8.9) years, reducing substantially the proportion that might eventually develop bipolar illness.
One major methodological limitation deserves comment. The results of factor analysis are critically dependent on the items analysed. We utilized a standardized interview for the DSM-IV criteria both in aggregated and disaggregated form. However, the other items added to form our final 27-item analysis reflected our own research interests. Furthermore, we could not include all the DSM-IV melancholic symptoms because some of them just assess the same symptoms as one of the A criteria at a more stringent level (e.g. melancholic criterion B4 is just a severe version of criterion A5). Including both items would cause estimation problems because the melancholic criterion would never be scored present in the absence of the relevant A criterion.
Acknowledgements
This work was funded by the Wellcome Trust. All authors are part of the CONVERGE consortium (China, Oxford and VCU Experimental Research on Genetic Epidemiology) and gratefully acknowledge the support of all partners in hospitals across China.
Declaration of Interest
None.






