Alternative medical therapies are functionally defined as interventions neither taught widely in medical schools nor generally available in mainstream hospitals. National surveys suggest that alternative medicine is popular throughout the industrialised world. In a UK-wide postal survey of 1200 people with agoraphobia (Reference Marks and HerstMarks & Herst, 1970), 15% had seen a religious or spiritual healer for their phobia, and they had taken two to three times longer (mean of 57 months) to seek that help than to seek help from general practitioners (GPs) or psychiatrists, respectively. The rate of 15% is like the one in seven proportion of members of the UK Consumers' Association in 1985 who had visited a non-conventional practitioner in the preceding 12 months; this rate rose to almost one in four in 1991 (Consumers' Association, 1992).
In 1993 the National Association of Health Authorities and Trusts showed that £1 million of public money was spent on purchasing complementary treatments (Reference Goldbeck-Wood, Dorozynski and Gunnar LieGoldbeck-Wood et al, 1996). This use of alternative therapies is set to rise. Estimated expenditures in the USA for alternative therapy services by the general population increased 45% between 1990 and 1997 and were conservatively estimated at $21 billion in 1997 (Reference Eisenberg, Davis and EttnerEisenberg et al, 1998). The same authors found that in the USA the therapies increasing the most included self-help groups, herbal medicine, massage, megavitamins, folk remedies, energy healing and homeopathy.
The study
A small article was placed on the BBC teletext community pages on ‘Self treatment for anxiety’ to advertise the Maudsley Hospital's computer-aided self-help services for obsessive—compulsive disorder and agoraphobia. Information on the service and a survey questionnaire was sent to 326 enquirers who disclosed their address. Respondents were asked to rate the severity and duration of their problem and the therapies and services they had previously used, both conventional and alternative.
A simple tick box questionnaire was devised asking respondents whether they had been treated for their anxiety disorder by: (a) their GP; (b) a psychiatrist; (c) a psychologist; (d) a nurse therapist; (e) a community psychiatric nurse; (f) a hypotherapist; (g) self-help therapy; and/or other therapies, and they were asked to specify which ones. Respondents were also asked to rate the severity of their problem on a 0-8-point scale (0, problem absent; 8, problem very severe, disturbing/disabling). Respondents were also asked to rate how long they had had their phobias or obsessive—compulsive problems on a six-point scale (less than 1 year, 1-2 years, 2-5 years, 5-10 years, 10-20 years or over 20 years).
Findings
One hundred and thirteen (35%) completed questionnaires were returned. Fifteen per cent of respondents had received no treatment (conventional or alternative) for their anxiety problem. Seventy-six (67%) had been treated by their GP, 62 (55%) by a psychiatrist or psychologist and 30 (27%) by a nurse therapist or community psychiatric nurse, while 48 (42%) had received alternative therapies for their anxiety. Thirty-four (55%) of the respondents who had been treated by a psychiatrist or psychologist had also used alternative therapies. The most popular alternative therapy was hypnotherapy, with 32 (28%) respondents having used it. Other alternative therapies used were: self-help therapy, n=18 (16%); autogenic training, n=4 (4%); cranial osteopathy, n=1 (1%); reflexology, n=1 (1%); acupuncture, n=1 (1%); and meditation, n=1 (1%). The self-reported severity and duration of problem were compared between respondents who had received no treatment, those who had been treated by their GP, those who had been treated by a psychiatrist or psychologist and those who had used alternative therapies (see Table 1).
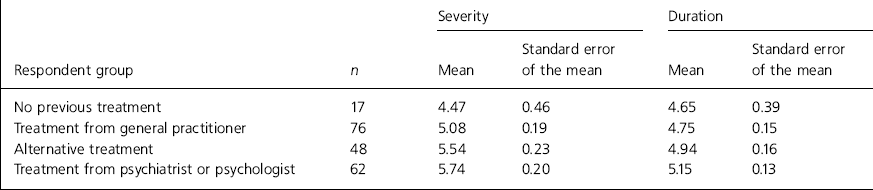
Table 1. Self-rated severity and duration of anxiety problem
| Severity | Duration | ||||
|---|---|---|---|---|---|
| Respondent group | n | Mean | Standard error of the mean | Mean | Standard error of the mean |
| No previous treatment | 17 | 4.47 | 0.46 | 4.65 | 0.39 |
| Treatment from general practitioner | 76 | 5.08 | 0.19 | 4.75 | 0.15 |
| Alternative treatment | 48 | 5.54 | 0.23 | 4.94 | 0.16 |
| Treatment from psychiatrist or psychologist | 62 | 5.74 | 0.20 | 5.15 | 0.13 |
Severity of problem
There was no significant difference in the self-rated severity of problem between the group who had received no therapy and those who had been treated by their GP (unpaired t-test, t=1.31, d.f.=91, P=0.51). The self-rated severity of problem in those who had received no therapy was less than in those who had been treated by a psychiatrist or psychologist (unpaired t-test, t=2.77, d.f.=77, P=0.01) and those who had used alternative therapy (unpaired t-test, t=2.29, d.f.=63, P=0.03). The self-rated severity of problem did not differ significantly between those treated by a psychologist or psychiatrist and those who had used alternative therapy (unpaired t-test, t=0.66, d.f.=108, P=0.51).
Duration of problem
There was no significant difference in the self-reported duration of problem between any of the four groups: no therapy compared with those treated by their GP (unpaired t-test, t=0.27, d.f.=91, P=0.79), with those who had been treated by a psychiatrist or psychologist (unpaired t-test, t=1.59, d.f.=77, P=0.12) and with those who had used alternative therapies (unpaired t-test, t=0.80, d.f.=63, P=0.42).
Discussion
The response rate of the study (35%), while low, is average for postal surveys (Reference PartenParten, 1950; Reference KerlingerKerlinger, 1973), but does mean conclusions can only be tentative. Our population is also likely to be skewed towards those who use alternative therapies because they were responding to an article on self-help therapy. A large minority of our group used hypnotherapy (28%), which is not widely used in other European countries (Reference Fisher and WardFisher & Ward, 1994). None admitted to using homeopathy, probably because we did not specifically ask about homeopathy.
Within our sample, self-reported duration of problem was not associated with treatment-seeking behaviour, but self-rated severity of problem did. The more severe anxiety sufferers had been treated by a psychiatrist or psychologist and had used alternative therapies. Our findings agree with those of Astin (Reference Astin1998), who found poorer health predicted more alternative therapy use in 1035 randomly selected individuals who had agreed to participate in mail surveys. Our findings also agree in two respects with those of Marks & Herst (Reference Marks and Herst1970). First, of the 1200 people with agoraphobia surveyed the 5% with no past medical treatment for their phobia were no more severe than those treated by a GP for their phobia. These untreated 5% were, however, more shy about confiding in anyone (not only doctors) and took longer to seek help from anyone not only for their phobia, but also for their physical illnesses — the present study did not examine the latter issue. The second similarity was that the people with agoraphobia in Marks & Herst's study who had been treated by a GP for their phobia were less severe than those who had had psychiatric out-patient treatment for it.
Our findings in a selected sample suggest that more severe anxiety sufferers use both mental health services and alternative therapies more. In our sample over half of respondents (55%) who had been treated by a psychiatrist or psychologist had also used alternative therapies. In view of these findings, as clinicians, we need to educate ourselves as to the alternative therapies available, their efficacy and side-effects and we need to actively ask patients about their use.




eLetters
No eLetters have been published for this article.