To the Editor—We read with interest the recent article by Scheuerman et al,Reference Scheuerman, Schechner and Carmeli 1 in which they found that patients with extended-spectrum-β-lactamase (ESBL) producing Klebsiella pneumoniae infections had higher 30-day mortality than patients with ESBL producing Escherichia coli infections. We have recently published on mortality, readmissions, recurrences, and the benefit of infectious diseases consultation for patients with various multidrug resistant organism infections.Reference Burnham, Kwon, Olsen, Babcock and Kollef 2 , Reference Burnham, Olsen, Stwalley, Kwon, Babcock and Kollef 3 We included in our study patients with various ESBL producing Enterobacteriaceae infections, among them K. pneumoniae and E. coli. Given the recent findings of Scheuerman et al, we conducted a retrospective evaluation to determine the association between ESBL producing organism (K. pneumoniae or E. coli) and 30-day all-cause mortality at our institution.
This study was conducted at Barnes-Jewish Hospital, a 1,250-bed academic medical center in St Louis, Missouri. The study period was January 1, 2006, to October 1, 2015. We included patients with positive sterile site and bronchial wash/bronchoalveolar lavage cultures for ESBL-producing E. coli and K. pneumoniae. Sterile sites were defined as bloodstream; pleural, intra-abdominal, pericardial, cerebrospinal, and synovial fluids; bone marrow; and surgical specimens collected from lymph nodes, central nervous system, liver, spleen, kidney, pancreas, ovary, or vascular tissue. The presence of ESBL production was assumed based on ceftriaxone, aztreonam, cefotaxime, or ceftazidime nonsusceptibility. 4 The Washington University School of Medicine Institutional Review Board approved this study with a waiver of informed consent.
The primary endpoint was 30-day all-cause mortality. Kaplan-Meier curves for 30-day all-cause mortality were generated to compare organism type and significance determined using the log-rank test. Escherichia coli was used as the reference group for determining the association between organism and mortality. Log-log survival plots were used to graphically test the proportional hazards assumption. Factors associated with mortality in bivariate analysis (P<.20) were entered into a multivariate Cox proportional hazards model to determine hazard ratios (HR) for 30-day all-cause mortality. All analyses were conducted with SPSS version 25 software (IBM, Armonk, NY).
In total, 605 patients met the eligibility criteria: 543 with ESBL E. coli and 62 with ESBL K. pneumoniae. Among patients with ESBL E. coli, 96 (17.7%) died within 30 days compared to 16 (25.8%) with ESBL K. pneumoniae. In Kaplan-Meier analysis, mortality was not significantly different between patients infected with K. pneumoniae and E. coli ESBL organisms (P=0.12). Variables retained in the final Cox proportional hazards model are shown in Table 1. Infection with ESBL-producing K. pneumoniae was marginally associated with mortality in the final Cox proportional hazards model (hazard ratio [HR], 1.69; 95% confidence interval [CI], 0.97–2.92; P=.062). Because the number of patients in the ESBL K. pneumoniae group was small, we performed a post-hoc power analysis and found that we had only 35.8% power to detect a significant difference in mortality.
Table 1 Factors Associated with 30-Day All-Cause Mortality in a Cox Proportional Hazards ModelFootnote a
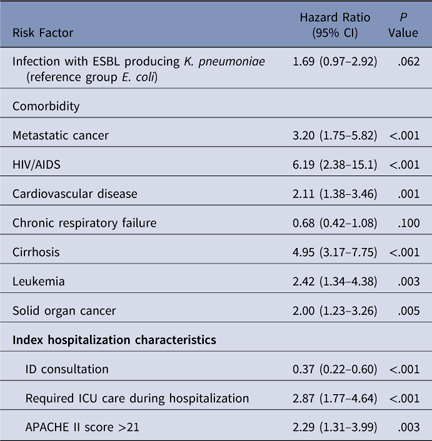
NOTE. HIV/AIDS, human immunodeficiency virus/acquired immunodeficiency syndrome; APACHE, Acute Physiology and Chronic Health Evaluation; CI, confidence interval; HR, hazard ratio; ICU, intensive care unit; ID, infectious diseases.
a Variables not retained in final model included admitting service, sex, lymphoma, congestive heart failure, diabetes, solid organ transplant, bone marrow transplant, chronic kidney disease, and end-stage renal disease.
Our results add to the body of literature on differences in mortality between ESBL-producing K. pneumoniae and E. coli. Despite the low power of our study, ESBL-producing K. pneumoniae was associated with marginally increased risk of 30-day mortality. Our data are important to add to the literature on this subject and could be combined with the data of Scheuerman et al and future studies in a meta-analysis to more definitively determine the association between ESBL-producing organism type and mortality. In addition, as demonstrated in our previous study, infectious disease consultation was associated with reduced mortality for drug-resistant Enterobacteriaceae infections.
Acknowledgments
The content is solely the responsibility of the authors and does not necessarily represent the official view of the National Institutes of Health (NIH).
Financial support
This work was supported by a grant from the Washington University Institute of Clinical and Translational Sciences (grant no. UL1TR000448) and by a subaward (no. KL2TR000450) from the National Center for Advancing Translational Sciences (NCATS) of the NIH.
Potential conflicts of interest
Dr Kollef was supported by the Barnes-Jewish Hospital Foundation. All other authors report no conflicts of interest relevant to this article.



