INTRODUCTION
Scombroid poisoning or histamine fish poisoning is a foodborne chemical disease associated with fish consumption. Most cases have been observed with fish belonging to the Scombridae family (e.g. tuna, mackerel), although non-scombroid fish species may also be implicated (e.g. sardines, herring) [Reference Hungerford1]. These fishes share high levels of free histidine in their muscle tissues. Histamine is generated from free histidine by a bacterial enzyme histamine-decarboxylase, usually following time-temperature abuse [Reference Hungerford1]. Bacteria such as Pseudomonas, Klebsiella, Enterobacter, Escherichia or Clostridium may be responsible for this transformation; they either constitute normal flora in the fish or come from contamination during handling. Although histamine formation is best controlled by preventing time-temperature abuse, it is known that some bacteria have the ability to form elevated concentrations of histamine at temperatures as low as 0–5°C [Reference Duflos2]. Scombroid fish poisoning is probably underestimated since symptoms can easily be misclassified as allergic reactions. However, it ranks among the most prominent seafood intoxications and is reported worldwide [Reference Dalgaard and Borresen3].
On 26 November 2010, a large number of French Armed Forces soldiers in Dakar (Senegal) became ill with symptoms resembling an allergic reaction within 2 h after eating lunch at the military catering facility. Most cases experienced clinical manifestations like flushing (on the face, neck and trunk) pruritus or headache. Due to the large number of patients and the rapid onset of symptoms after lunch, a foodborne disease was quickly suspected. On the basis of clinical manifestations and fish consumption during lunch, scombroid fish poisoning was considered. A case-control study was undertaken in order to describe this outbreak, identify its source and quickly implement prevention measures. In this report, the authors summarize the steps and the main results of the investigation.
SUBJECTS AND METHODS
Attendees of the incriminated lunch were eligible for this study. Those who reported at least one of the following clinical manifestations (flushing, headache, diarrhoea) within 72 h after lunch were classified as cases. A similar number of controls were randomly selected from the attendees at the lunch that did not report any clinical manifestations. For all cases and controls, food items eaten during that lunch were recorded as well as past history of allergy and current treatments. Data were collected using a semi-structured questionnaire. For cases, clinical manifestations (including their onset, duration and recovery) as well as treatment prescribed were also recorded. In addition, stools samples were taken from six case-patients who experienced diarrhoea and were analysed at the Institut Pasteur de Dakar (Senegal).
Chemical and bacteriological analyses were performed on a single 100-g sample of each food item on the lunch menu that had been stored as recommended. The quantification of sulphate-reducing anaerobic bacteria, coagulase-positive staphylococci and salmonellae was assessed at the Institut Pasteur de Dakar. Histamine, cadaverine and putrescine concentrations in the tuna were assessed twice on the same sample by high performance liquid chromatography (Hitachi, LaChrom Elite®, Japan) in the ANSES laboratory [Reference Malle, Valle and Bouquelet4].
Data were analysed using Stata software (StataCorp., USA). Qualitative data were compared using Pearson's χ2 test, or Fisher's exact test when required, while quantitative data were compared using Student's t test or non-parametric tests. A multivariate analysis (logistic regression) was performed to identify factors related to illness. A P value of ⩽0·05 was considered as significant.
RESULTS
In total, 71 of the 237 lunch attendees met the case definition (66 presenting at the medical facility and a further five identified in the randomly selected controls). This corresponded to an attack rate of 30·0%. Seventy-eight controls were selected randomly from those that attended the suspected lunch. This group mainly comprised young and healthy adults (age range 19–56, median 32 years); the majority were male (136/149). Cases were significantly younger than controls (30·2 vs. 34·8 years, P=0·001), but were similar in all other respects (gender, allergy history, chronic medications).
The most frequently reported symptoms were a sensation of warmth, flushing, headache, weakness, rapid/weak pulse and diarrhoea (Table 1). In all patients, symptoms began during or shortly after lunch (median 1 h, range 0–180 min) (Fig. 1). Of the 71 cases, 66 patients were managed at the medical facility of the French Armed Forces in Dakar; 60 of whom received treatment. Four of the five remaining cases self-medicated. Most patients were prescribed anti-allergic treatment: antihistamine 52/71 (73·2%) and/or corticoids (9·9%). According to the symptoms they experienced, patients were also prescribed paracetamol (29/71, 40·8%), racecadotril (12/71, 16·9%), diosmectite (14/71, 19·7%) or phloroglucinol (3/71, 4·2%). Clinical manifestations were sufficiently severe in some cases to require hospitalization (16/71 patients, 22·5%) and/or perfusion (with Ringer's lactate and/or HEA Voluven® (Lab. Fresenius Kabi, France) in 14 (19·7%) patients. Most patients recovered within a few hours after onset of clinical manifestations, with the most seriously affected recovering the following morning.
Table 1. Scombroid fish poisoning in Dakar (Senegal): main clinical manifestations with frequencies observed in 71 cases, in the 72 h following the incriminated meal

During the lunch, three different fishes were offered as main course: tuna (130 portions), shark (90) and salmon (40), respectively. Tuna was the only food item found to be positively associated to illness [Pearson's χ2=43·1, P<10−6, odds ratio (OR) 36·3, 95% confidence interval (CI) 6·3–210·0]. On the contrary, shark was found to have a protective effect (P<0·001, OR 0·1, 95% CI 0·03–0·4). None of the other food items served was significantly related to illness (Table 2). In addition, of the 107 attendees who ate tuna, individuals who ate more than one piece of tuna were 3·6 times more likely to become ill than those who ate one piece or less (multivariate analysis, P=0·003). However, the time between consumption and the onset of symptoms was not related to the amount of tuna eaten (P=0·18). Stool samples of cases were negative for pathogenic bacteria or parasites.
Table 2. Scombroid fish poisoning in Dakar (Senegal): number and percentage of cases and controls reporting consumption of food items (n=149)
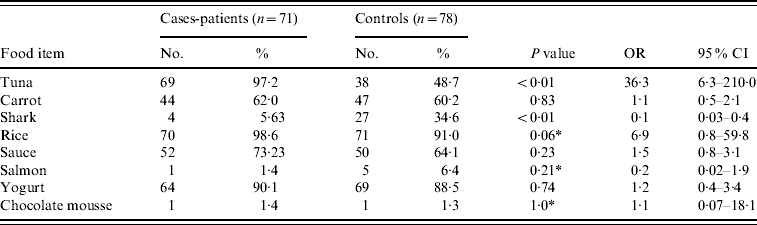
OR, Odds ratio; CI, confidence interval.
* Fisher's exact test.
Environmental investigation
The bacteriological analyses of the control meal food items, performed at the Institut Pasteur de Dakar were all negative. Conversely, mean histamine concentration measured was 4900±145 mg/kg, almost 50-fold higher than the concentration allowed by European regulations (100 mg/kg) [5]. Putrescine concentration was 282±1 mg/kg and cadaverine 300±7 mg/kg.
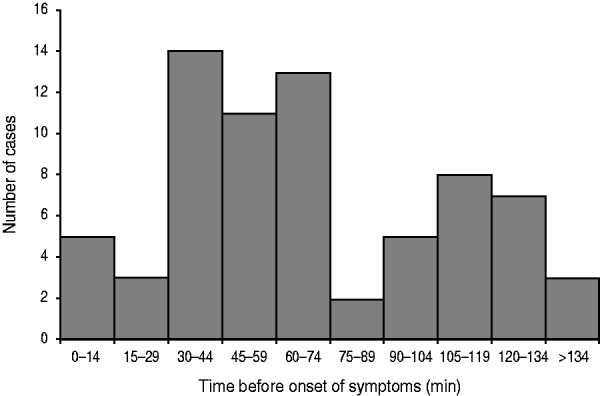
Fig. 1. Scombroid fish poisoning in Dakar (Senegal); time to onset of symptoms (n=71 cases).
Since no traceback information about the source and handling of the incriminated tuna was available prior to it being sold to the military unit, an investigation was planned including each person involved, from the initial fishing to the final sale. According to the seller at the local fish market, the tuna was fished on 25 November 2010 (the day before consumption). However the original fisherman could not be identified. It was reported to have been purchased by a wholesale sea-fish merchant in Dakar on Yoff beach and transported in a refrigerated van to a rented workshop. Tuna fillets were cut on 25 November 2010 between 11:30 and 13:30 hours in a relatively functional and air-conditioned room although somewhat dilapidated. Tuna fillets were delivered to the military restaurant on 25 November 2010 on melting ice at 14:30 hours. The control of goods received did not reveal any non-conformity. Fillets were stored in a walk-in cooler until the next morning. They were portioned in a room dedicated to cold preparation; fried, sauced and cooked in an oven at 150°C. Serving platters were steamed (70–75°C) before service. In the days following the outbreak, a clinical evaluation of the food handlers was performed according to European and French military regulations [6]. No pathology, suspected to be the origin of this foodborne disease, was identified for any of the food handlers.
DISCUSSION
This study found that 71 members of the French military forces in Dakar had scombroid fish poisoning due to the high quantity of histamine present in the tuna they consumed. This is, as far as we know, the largest scale scombroid fish-poisoning outbreak ever reported. The diagnosis of histamine poisoning is usually based largely on a history of the food eaten by the patient immediately before onset of illness. Clinical differential diagnosis with allergy is easier if more than one person is affected in a group of people consuming the contaminated fish or if patients have not had a reaction to that fish before [Reference Attaran and Probst7]. If the symptoms are appropriate, the onset time is reasonably short, and the patient has eaten a type of food potentially implicated in cases of histamine poisoning, the diagnosis can be confirmed by detecting high levels of histamine in the implicated food, meal leftovers or a similar product obtained from the same source [Reference Taylor8].
In this outbreak, classic symptoms of scombroid poisoning, e.g. flushing, headache, dizziness and diarrhoea were observed. In scombroid poisoning, clinical manifestations usually occur within an hour after ingestion of the contaminated meal and last for several hours [Reference Hughes and Merson9]. In this outbreak, the epidemic curve, by time to onset of clinical manifestations, showed two consecutive peaks, probably because some attendees slept after lunch and only felt ill when they awoke. The intensity of symptoms was highly variable; from no notification until the patients were asked to complete the questionnaire, to so intense that they needed hospitalization or perfusion procedures. As previously reported [Reference Hungerford1], recovery occurred within 1 day. In the present outbreak, first-line treatment included symptomatic H1 receptor antagonists as recommended in the literature [Reference Hungerford1, Reference Hughes and Merson9]. Other authors propose the use of H2 antagonists in order to improve outcome. Here, corticoids were also prescribed even though their use is not recommended for treatment of scombroid fish poisoning.
Bacteriological investigations did not demonstrate any contamination, probably because they was performed on the cooked food items in the control meal. On the other hand, histamine is thermostable; once it is produced its concentration is not modified by cooking. European Union regulations stipulate that the critical level of histamine is 100 mg/kg for raw fish [5]; in the USA a more conservative level of 50 mg/kg is used [10]. In the present outbreak, chemical contamination was confirmed since histamine concentration was 4900 mg/kg, far above the concentration allowed by regulations (CE no. 1441/2007, 5th December 2007). As reported previously [Reference Lavon, Lurie and Bentur11], this study also found the amount of fish consumed to be related to the risk of development of clinical manifestations. This dose–response effect is another strong argument for a causal link between tuna consumption and illness. Although histamine has been recognized as a causative agent in scombroid fish poisoning [Reference Morrow12], many studies have failed to reproduce clinical manifestations after oral challenge with histamine. On the basis of animal experiment models, bioamines have been considered as potentiators since they are able to reduce histamine catabolism [Reference Taylor8] or increase the amount of histamine absorbed in the gastrointestinal tract [Reference Hungerford1, Reference Hughes and Merson9]. In the current study, the presence of cadaverine and putrescine reported in the incriminated tuna could have contributed to the pathology.
Since no traceback documents were available it is conceivable that the tuna had been fished some time before it was claimed to have been, or that it had not been properly stored after fishing. Fish production in Senegal includes two different sectors: the industrial sector, dedicated to export trade and the artisanal sector which supplies the local market. While the industrial sector is relatively well controlled concerning sanitary risks, the latter is more clearly deficient in terms of cold chain management, traceability, handling hygiene, etc. Since scombroid poisoning is strictly the result of fish product mishandling, it should be preventable. However, it is often encountered with recreational catches or in countries where international food hygiene standards are insufficiently applied. It is interesting to note that such an outbreak had already occurred several years previously in the French Armed Forces with fish bought in Dakar [Reference Boutin13]. For economic and diplomatic reasons, the traditional fishing sector has been chosen to supply the French Armed Forces in Senegal. Nonetheless, where national regulations and controls are deficient, food professionals must intensify sanitary risk management to protect the consumers. As a temporary disposition following the recent outbreak, the veterinary expert advised against scombroid fish consumption. In the future, although it is not specified in the Senegalese regulations, French Armed Forces should ensure improved sanitary security dispositions from their suppliers. The veterinary expert and logisticians in charge of food supplies need to have access to traceback documentation for each product. In particular the certified origin of the product (fishing date and location) and storage conditions (delay and temperature); moreover, handling conditions in respect of hygiene rules should be registered.
In conclusion, this scombroid fish-poisoning outbreak is, to the best of our knowledge, the largest ever reported. Histamine contamination in tuna was substantial and symptoms were extremely intense in some patients. Scombroid fish poisoning must be borne in mind by physicians and, at best, prevented by food professional and official controllers.
ACKNOWLEDGEMENTS
The authors are grateful to Dr S. Clarke for English correction of the manuscript and helpful comments.
DECLARATION OF INTEREST
None.







