CLINICIAN'S CAPSULE
What is known about the topic?
Emergency department (ED) wait-times before triage are not well captured and can represent a significant period of time.
What did this study ask?
Can a self-check-in kiosk be used by ambulatory patients to check into triage and decrease identification time?
What did this study find?
Self-check-in kiosks can be implemented effectively in the ED to improve patient identification time and queue patients for triage.
Why does this study matter to clinicians?
Local implementation of similar self-check-in kiosks could improve staff and patient satisfaction while improving departmental flow and patient experience.
INTRODUCTION
Prolonged wait-times in the emergency department (ED) increase mortality and hospital admission,Reference Guttman, Schull, Vermeulen and Stukel1 decrease productivity,Reference Rondeau, Francescutti and Zanardelli2 and increase patient complaints.Reference Derlet and Richards3 Although the triage process is largely standardized,Reference Iverson and Moskop4 the method in which patients are identified on arrival and queued for triage is variable and ED arrival time is often captured.Reference Betz, Stempien, Trivedi and Bryce5 The typical first-come-first-serve triage approach does not account for patient acuity when determining triage order. Interestingly, delays to triage are rarely reported or included in wait-times and often exceed the Canadian Triage and Acuity Scale (CTAS) recommended time to physician initial assessment.Reference Iverson and Moskop4
We identified three concerns with our triage identification system. Firstly, it does not capture the number of patients waiting for triage, placing patients at risk of being unidentified for prolonged periods. Secondly, not queuing patients based on acuity may create delays in the management of time-sensitive conditions. Finally, it may cause confusion and anxiety for patients and result in unnecessary interruptions for triage staff.
Self-service kiosks are one strategy to improve ED operationsReference Wiler, Gentle and Halfpenny6 and have been used effectively to distribute discharge instructions,Reference Porter, Cai and Gribbons7 screen patients,Reference Houry, Kaslow and Kemball8 and enter basic medical history.Reference Sinha, Khor, Amresh and Drachman9 We believe that introducing kiosks in ED waiting rooms can provide a solution to the triage identification gap. The goal of this study was to provide proof-of-concept that ED patients can use a self-check-in kiosk upon arrival and to compare time-to-first-identification with our current triage system.
METHODS
Study design, setting, and population
The prospective randomized trial took place at the ED of a tertiary care academic hospital in Toronto, Canada, that treats an average of 63,000 patients yearly. Ethics approval was obtained from the hospital. The kiosk was available on weekdays during random weeks with intervening control periods where triage nurses identified arriving patients. Data were collected during a 10-week period.
Patients arriving during study hours (1030 to 1830) were eligible for enrolment. Research assistants approached random patients on arrival, obtained consent to access their health records, and documented their arrival times on a tablet. Research assistants did not direct patients following consent. Patients who arrived via ambulance, directed to an admitting service, or were a CTAS Level 110 were excluded prior to analysis.
Intervention
During intervention weeks, patients were directed by signs, floor maps, and security staff, to one of two kiosks. Kiosks were custom designed by an inter-professional group of ED staff. At the kiosk, patients swiped their Ontario Health Insurance Plan card or typed their demographic information before selecting their chief complaint from a pre-populated list or entered a free-text response. Patients then received an instruction sheet about their ED visit with an alphanumeric identifier. The information entered and arrival time were immediately available to triage nurses on screens at triage. Nurses selected patients for triage based on arrival time or complaint, and called them using their alphanumeric identifier.
During control weeks, patients were identified by triage nurses using standard processes or pre-triage processes. Pre-triage occurred when multiple patients were queuing at triage and required a nurse to create a pre-triage list limited to name, chief complaint, and time, which was then used to prioritize triage order. During peak hours, there were three triage nurses who share these duties.
Outcomes
Time-to-first-identification
In the intervention group, time-to-first-identification was the interval from ED arrival to kiosk completion. In the control group, time-to-first-identification was the interval from ED arrival to pre-triage or triage, as captured in the Emergency Database Information System (EDIS). This measure is an estimate of time required for new arrivals to be identified by the system rather than the time to direct contact with a healthcare provider.
Time-to-triage
Time-to-triage is defined as the interval from ED arrival to the completion of triage.
Time-to-MD
Time-to-MD is defined as the interval from ED arrival to physician assessment as captured in EDIS.
Kiosk usability
Kiosk usability is defined as the percentage of ambulatory patients that used the kiosk during the intervention periods.
Data collection
Pre-triage time, triage time, demographics, and CTAS scores were collected from EDIS.
Analysis
A statistical analysis was performed with SAS Version 9.4 (SAS Institute, Cary, NC, USA). Descriptive statistics were calculated for all variables of interest. Comparisons between groups were run using two-sample, two-sided t-tests for continuous variables and chi-square tests for categorical variables. Only patients who used the kiosk were labeled as the intervention group.
Multiple linear regressions were performed to examine differences in our outcome measures, controlling for age, CTAS, patient disposition, and triage burden. To adjust for the effect of variable inflow during the intervention and control periods, we created a volume burden on triage measure. Patients were assigned a triage burden value, defined as the number of patients triaged during the period from their arrival to their triage, with higher values reflecting a higher inflow demand.
RESULTS
Of 3,561 eligible arriving patients, research assistants enrolled 2,181 (61.2%). After data matching and exclusion, a final sample of 1,732 patients was analysed. Kiosk usability was found to be 97%. Baseline characteristics were similar for control and intervention groups, except for the triage burden (Table 1), which was significantly higher in the intervention group.
Table 1. Comparison of baseline characteristics across groups
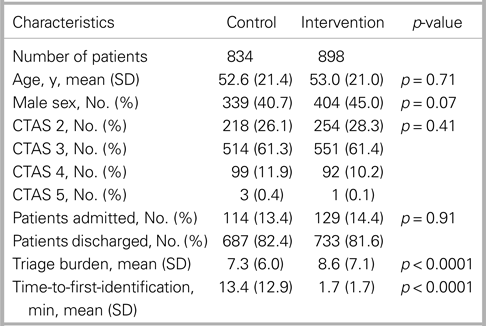
CTAS = Canadian Triage and Acuity Scale; SD = standard deviation.
The analysis showed that the median (interquartile range) time-to-first-identification was 4 (1.0–2.08) for intervention patients and 9 (5–18) for control patients. The regression analysis revealed that the time-to-first-identification was 13.6 minutes (95% confidence interval [CI]: 12.8–14.5) faster in the intervention group (Table 2). The median time-to-triage was 27.5 (14–51) and 22 (11–44) in the intervention and control groups, whereas the median time-to-MD was 145 (98–207) and 144 (86–210) in the intervention and control groups. The regression analysis found no statistically significant difference for both variables after correcting for triage burden.
Table 2. Results of linear regression analysis on time-to-first-identification (n = 1663)
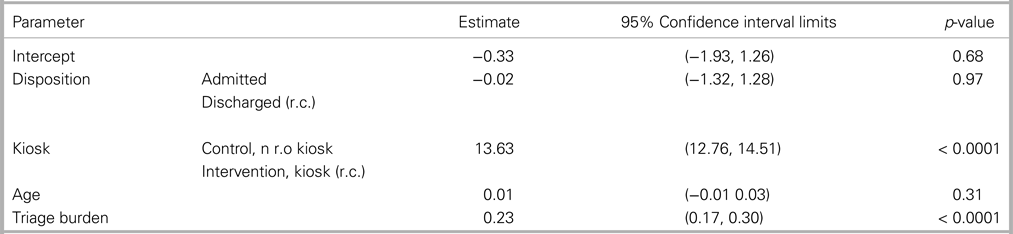
r.c. = reference category.
DISCUSSION
In this study, we examined whether a self-check-in kiosk could be used to identify patients arriving in our ED, and its effectiveness. We found that 97% of patients arriving in our ED during peak hours were able to use the kiosk and that the kiosk significantly improved the time required to identify new arrivals. Two limitations of our study were that we tested the kiosk only during peak hours, and we had only one research assistant for data collection. We believe that testing during peak times meant that ED stressors would be felt most during these times, and the kiosk's success or failure would be highlighted. Our limited research assistant coverage and challenges matching names to our administrative database resulted in some missing data; however, we believe that this was random and did not skew the data in one particular direction.
Although we found no improvement in time-to-triage or time-to-MD, we are confident that this study provided an important first step in evaluating and improving ED triage processes. The kiosk provides an objective measure of the pre-triage interval, which traditionally is not included in wait-time data or collected. The automated measurement of the pre-triage interval is an important gain because it allows for measuring and improving time-to-triage. Before this study, we were unaware of the time before triage, which is significant at over 30 minutes during peak hours. The ability to track triage delays in real time provides a mechanism to activate triage surge strategies and allocate resources in an efficient manner. It is also thought that chief complaint information allows nurses to prioritize triage based on perceived acuity, and this could be an area of future study.
CONCLUSION
This study shows that a self-check-in kiosk can be used by patients arriving in the ED to self-identify and capture the arrival times of patients. We believe that these results provide a strong proof-of-concept for the use of kiosks in EDs.
Competing interests
None declared.




