CLINICAL SCENARIO
A 12-year-old male injured his ankle while playing hockey (Figure 1). His dad reports that he was checked into the boards. His ankle is swollen, but does not appear deformed. His distal neurovascular exam is normal. There is bony tenderness over the lateral malleolus in accordance with the Ottawa Ankle Rules.
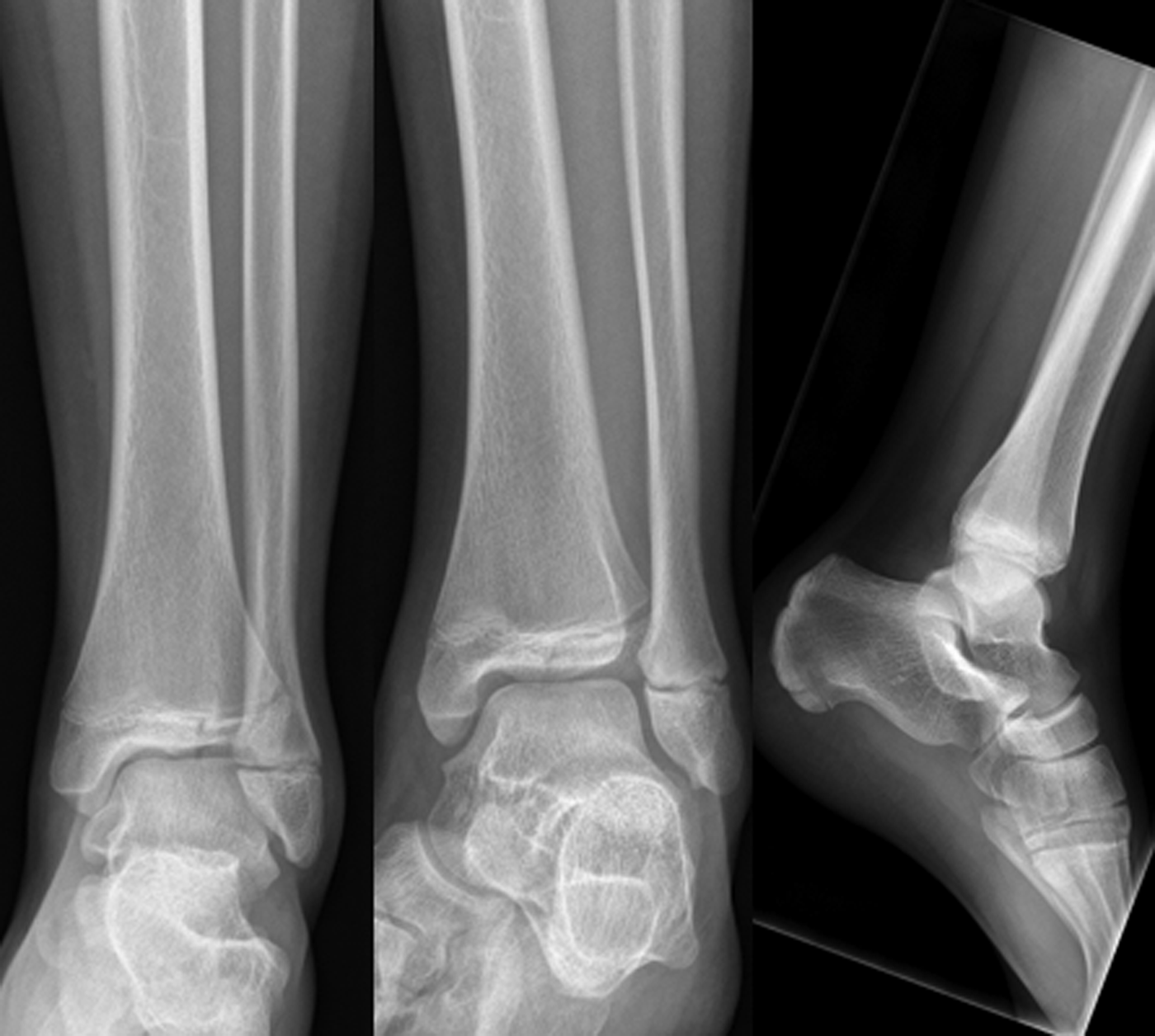
Figure 1. Radiographs of 12-year-old male with ankle injury.
- 1.
Why is it important not to miss growth plate fractures?
It is crucial not to miss growth plate fractures because traumatic epiphyseal blood supply disruption can result in osteonecrosis, slowed bone growth, growth plate closure, and abnormal secondary ossification.Reference Podeszwa and Mubarak1 Fortunately, most growth plate fractures are nondisplaced low-grade Salter-Harris (SH) fractures (~75% SH-II), and these fractures rarely lead to clinically important complications. However, if displaced SH-II, SH-III, SH-IV, or SH-V go unrecognized, they can result in growth arrest and functional impairment. This is especially true if the growth plate fracture occurs in a bone that is high risk for this outcome (e.g., femur, tibia). If these diagnoses are caught by a radiologist and communicated to the treating physician within 2–3 days, the long-term functional outcome is not likely to be different. There are, however, other important reasons not to miss growth plate fractures at the first encounter. While true long-term harm is extremely rare, these errors can result in broken trust of families, repeat unnecessary visits, unnecessary prolonged pain, and medico-legal complaints.Reference Boutis2
With tibial fractures specifically, the risk of growth arrest ranges from 2% to 50%, depending on the type of SH fracture and the degree of displacement. The risk of complication is best predicted from the degree of displacement of the physis, with > 2–3 mm indicating a high likelihood of entrapped periosteum. Reduction of these injuries whether closed or open should be done gently by experienced providers. It should also be accomplished in as few attempts as possible to minimize further trauma to the growth plate tissue. Satisfactory reduction is important to prevent joint incongruity and subsequent early degenerative arthritis.Reference Podeszwa and Mubarak1
- 2.
How often are pediatric musculoskeletal radiographs misinterpreted?
Misinterpretation of pediatric musculoskeletal (MSK) radiographs in pediatric EDs has been estimated to occur in 3% to 15% of cases. Risks of missing a fracture are greatest in children who present with joint injuries, where growth plate injuries are most common.Reference Boutis2
- 3.
Why are these injuries missed?
Growth plate areas on radiographs are anatomically complex and add to the diagnostic interpretation challenges. Cognitive biases can also play a role in radiograph interpretation error. The most common cognitive biases that can impact radiograph diagnostic accuracy are nonavailability bias (i.e., no previous experience with fracture type), search satisficing bias (i.e., find part of a fracture or the first fracture of multiple and stop looking), and ascertainment bias (i.e., low pretest probability and miss a fracture).Reference Croskerry3
There are examples of these types of errors with growth plate fractures. Nondisplaced SH-II fractures of the distal radius are commonly misinterpreted as buckle fractures. Because an injury is seen, the extension or second injury is not looked for or appreciated (search satisficing bias). SH-IV or lateral condyle fractures of the distal humerus are another source of missed injuries. Because the elbow has a large amount of cartilaginous and radio-lucent structure to it, it is hard to visualize what you are looking at when you look at an x-ray. Additionally, multiple ossification centers appear at different ages, and it can be difficult to tell what is a fracture due to inexperience (nonavailability bias).
- 4.
How can radiograph detection skills be improved?
The techniques for improving skills in growth plate injury radiograph interpretation are not different from improving skills in general radiograph interpretation. Simply being aware of the types of cognitive biases that lead to misinterpretation of radiographs are insufficient to protect physicians from making errors. Developing experience with feedback and coaching is a physician's best defence against diagnostic error.Reference Norman, Monteiro, Sherbino, Ilgen, Schmidt and Mamede4 There are several ways to get better at MSK radiograph interpretation. When there doubts or discomfort about radiograph interpretation, or when attempting to interpret a radiograph not often encountered, it is useful to double check interpretations with colleagues (Emergency Medicine, Orthopedics, or Radiology) in real-time. As a quality assurance initiative, EDs can develop film libraries of imaging that were misinterpreted (including pediatric MSK) and discuss these cases at monthly meetings. Independent engagement in education is also important to increase case exposure and solutions. On-line learning platforms have been shown to improve competence through a large sample of radiographs using the learning theory of cognitive simulation, deliberate practice, and performance based-competency on interpretation skills.Reference Lee, Pusic, Carrière, Dixon, Stimec and Boutis5
CASE RESOLUTION
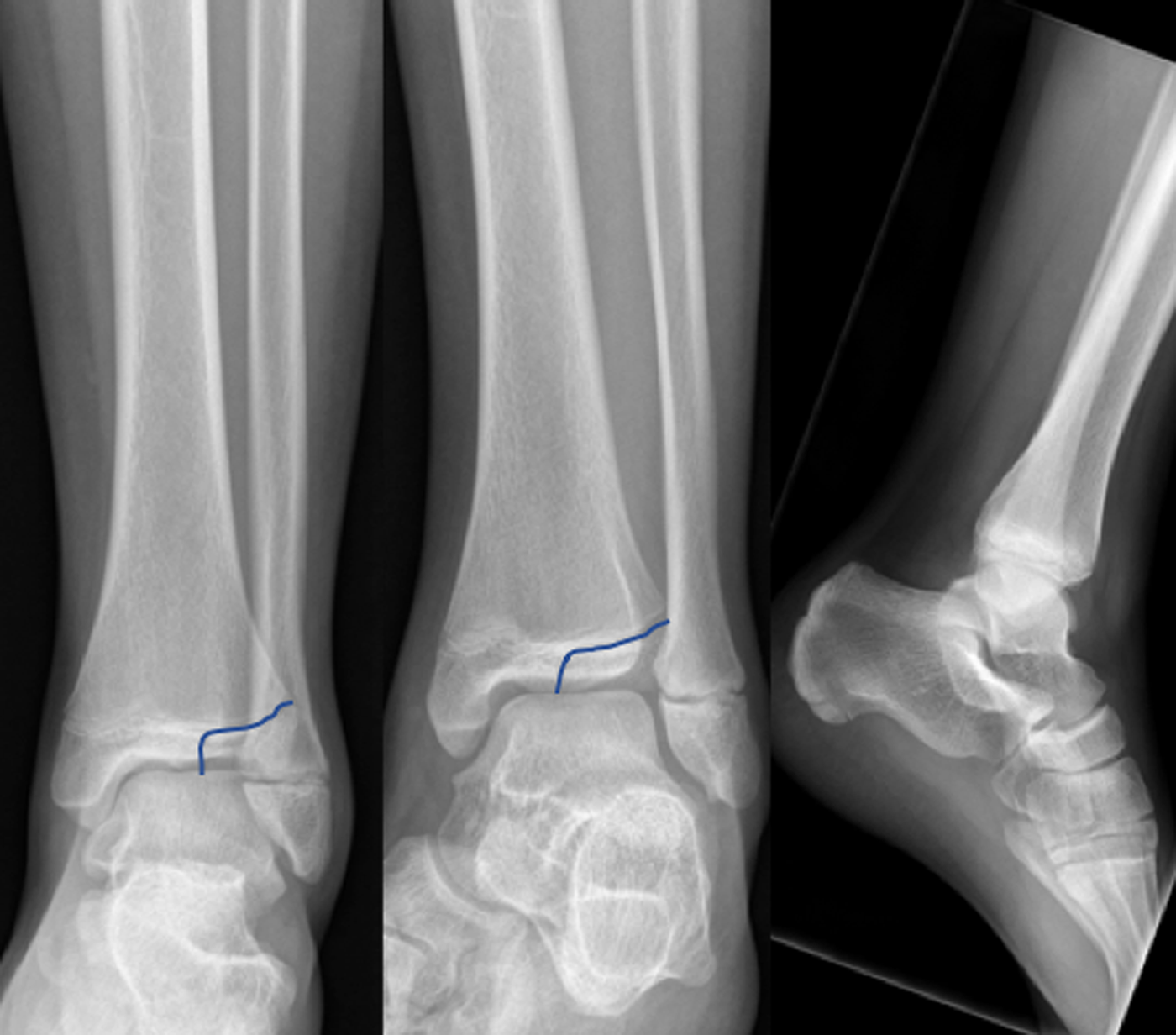
Given the child's age and presentation, the ED physician was suspicious of an ankle sprain, but the Ottawa Ankle Rules were positive so the ED physician ordered a radiograph. The ED physician did not see any fracture and placed the child in a removable splint for comfort and advised rest, ice, compression, and elevation. The radiology interpretation the next day identified a minimally displaced SH-III fracture of the distal tibia, also known as a Tillaux fracture (Figure 2). On review of this case with the initial ED physician, it was identified that they only examined the tenderness points specific to the Ottawa Ankle Rules and did not examine the anterior joint line. In the absence of this finding, their suspicion for a fracture was low (prevalence bias), which led to them missing the fracture located in the anterior joint line area of the radiograph. At the second ED visit, orthopedics was consulted, who recommended open reduction and internal fixation of the fracture to reduce the risk of growth arrest and early arthritis.

Figure 2. Growth plate fracture line showing a nondisplaced SH-III fracture of the distal tibia (aka Tillaux fracture).
Financial support
There are no funders to report for this submission.
Competing interests
Dr. Kathy Boutis runs ImageSIM, which we reference as one possible tool to help improve pediatric MSK radiograph interpretation skills. Dr. Boutis does not receive any personal monetary profit from the program.