The prevalence of obesity has increased dramatically in the recent past in the USA and remains a significant public health concern with nearly 35 % of the adult population meeting the clinical criteria for obesity(Reference Cohen, Cziraky and Cai1, Reference Flegal, Carroll and Ogden2). At present, it is unclear whether the macronutrient composition of the diet contributes to body weight. However, it has been hypothesised that greater dietary fat consumption is related to energy imbalance because it is the most energy-dense macronutrient(Reference Willett3). Additionally, some types of dietary fats have been implicated in the inflammatory processes that contribute to chronic disease burden(Reference Calder4). Despite the known adverse consequences of excess dietary fat intake, it is unclear whether recommendations to reduce the intake of dietary fats influence their consumption. In response to consistent recommendations to reduce dietary fat intake and accompanying consumer demand, more than 3400 low-fat and fat-free products were introduced in the market in the 1990s(Reference Kuchler, Golan and Variyam5). Consequently, health claims and low-fat labelling(Reference Chandon and Wansink6) may increase energy intake perhaps by encouraging consumers to select larger portions of foods that they perceive to be less energy dense(Reference Wansink and Chandon7). This may adversely or favourably influence fat intake.
Few longitudinal studies carried out in the USA have evaluated long-term dietary fat intakes in adults or among lean, overweight and obese individuals(Reference Willett3). Longitudinal observations may provide insights into how changes in the dietary composition of a population parallel shifts in national dietary recommendations and concomitant changes in the food environment, such as the introduction of low-fat products into the market(Reference Worsley8). The objective of the present study was to examine trends in the intakes of dietary fats and foods rich in fat among members of the Framingham Heart Study (FHS) Offspring Cohort from 1991 to 2008, representing a 17-year period. The availability of serially collected dietary and anthropometric data for the Offspring cohort provides a unique opportunity to investigate changes in dietary patterns during middle through older adulthood, which represents a critical window of exposure to risk factors that influence chronic disease pathophysiology. The present study encompasses a period in the USA during which dietary recommendations consistently emphasised reductions in dietary fat intake(Reference Austin, Ogden and Hill9).
Methods
Study population
The Framingham Heart Study Offspring Cohort
The FHS is an ongoing study carried out in Framingham, Massachusetts, consisting of approximately 14 000 adults recruited from three familial generations spanning the period 1948–53(Reference Dawber, Meadors and Moore10). The first generation of participants, referred to as the Original cohort, comprises a primarily Caucasian sample of men and women aged 30–62 years (n 5209)(Reference Splansky, Corey and Yang11). The second generation of participants (the Offspring cohort) comprises children of the Original cohort and their spouses (n 5124 adults), and it was established in the period 1971–75. Clinical examinations were conducted, on average, every 4 years for the Offspring cohort, and the latest examination was conducted in 2008(Reference Larson, Atwood and Benjamin12). The details of the FHS have been published elsewhere(Reference Dawber, Meadors and Moore10, Reference Splansky, Corey and Yang11, Reference Feinleib, Kannel and Garrison13). All research activities adhered to the ethical standards of New York University's Institutional Review Board for the analysis of secondary data (IRB no. 10-0555). The Framingham Study is conducted according to the guidelines laid down in the Declaration of Helsinki, and all procedures involving human subjects were approved by the Institutional Review Board of Boston University Medical Center. Written informed consent was obtained from all the Framingham Study participants.
Analysis dataset
In the present study, analyses included members of the Offspring cohort who were at least 25 years of age by exam 5 and who had undergone at least three of the four dietary assessments from 1991 to 2008. The collection of dietary data using the FFQ was first initiated in 1991 corresponding to exam 5, at which point, 981 participants had been lost to follow-up. An additional 810 participants were excluded because they did not complete at least three dietary questionnaires or had thirteen or more blanks on the FFQ. Participants who reported energy intakes < 2510 or >16 736 kJ/d ( < 600 or >4000 kcal/d) were considered as having invalid dietary data and were excluded (n 446). The final analytical dataset consisted of valid dietary data for 2887 men and women (70 % of those who attended exam 5).
Data collection
Assessment of dietary intake
Dietary intake was assessed a total of four times (exams 5 to 8) since 1991 (Fig. 1) using the validated 131-item Harvard semi-quantitative FFQ that queries participants about their intake of foods with standard serving sizes(Reference Rimm, Giovannucci and Stampfer14). The FFQ were mailed to the participants and reviewed with them for accuracy by trained personnel at the study site. The participants reported their food intake and frequency of consumption, ranging from never or < 1 serving/month to ≥ 6 servings/d, for the past year. The FHS derived weekly servings by using these categorical responses. The United States Department of Agriculture Nutrient database(Reference Anderson, Ahuja and Raper15) was used in conjunction with the FFQ and was updated continuously to reflect changes in the food supply over time(Reference Wolongevicz, Brown and Millen16).
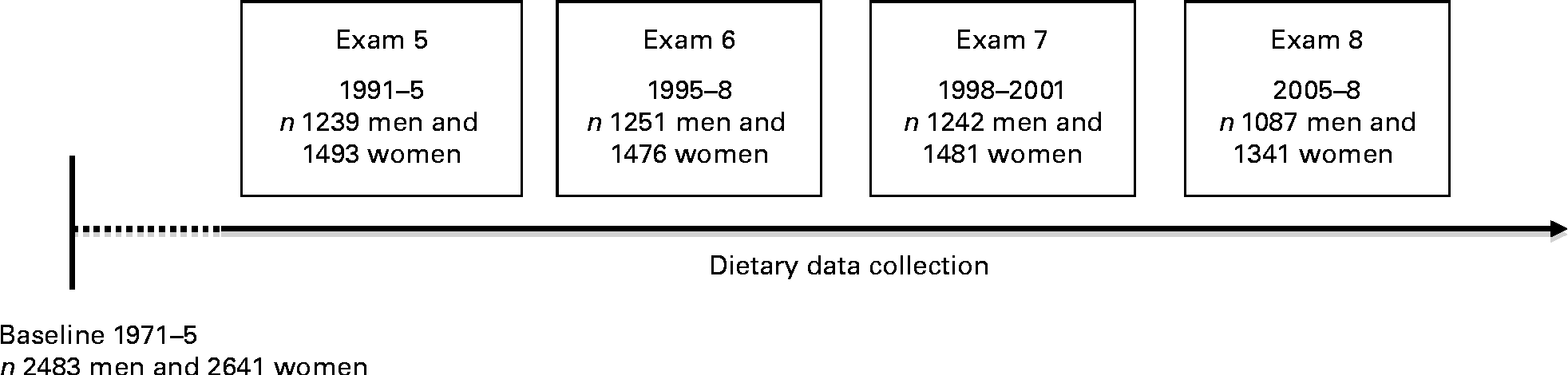
Fig. 1 Design of the Framingham Offspring Study and participation rates through 2008. The study began in 1971–5 and recruited 5124 participants. Beginning in 1991 (exam 5), comprehensive dietary data were collected using the FFQ every 4 years through 2008. Data collection is ongoing in the Offspring cohort.
Other covariates
Fasting blood glucose concentrations were assessed during clinical examinations. Impaired fasting blood glucose concentrations were defined as concentrations ≥ 1100 mg/l (110 mg/dl)(17) in the present analyses. Height and weight were measured by trained personnel at each visit and were used to calculate BMI. Other variables including age, education and smoking status were self-reported during each examination, with the exception of education, which was self-reported once during exam 2.
Statistical analyses
First, baseline (exam 5) descriptive characteristics including means and standard deviations were computed using SAS version 9.3 (SAS Institute, Inc.)(18). Next, trends in the intakes of dietary fats and high-fat foods over time among men and women were evaluated using the longitudinal nature of the data. These analyses were carried out using the statistical package R (R Foundation for Statistical Computing)(Reference Pinheiro, Bates and DebRoy19). The dietary trends were evaluated using a repeated-measures model with subject-specific random intercepts to account for serial correlation. All P values for trends and interactions were derived from such models. We made an a priori decision to stratify the analyses by sex and BMI because of its potential clinical significance. Therefore, we re-examined trends stratified by the following BMI categories: normal, ≥ 18·5–24·9 kg/m2; overweight, ≥ 25–29·9 kg/m2; obese, ≥ 30 kg/m2(20). Bonferroni corrections were applied to subgroup analyses in order to correct for multiple comparisons.
Results
Participant characteristics during exam 5
The characteristics of the Offspring cohort during exam 5 are expressed as either percentages for categorical variables or means with their corresponding standard deviations for continuous variables (Table 1). The mean age of men was 54·4 years and that of women was 53·9 years during exam 5. During exam 8, the mean age of both men and women was 66·8 years. On average, the population was educated beyond high school. During exam 5, mean BMI was 28·2 kg/m2 for men and 26·5 kg/m2 for women; 23 % of the participants were obese and 13 % had impaired fasting glucose concentrations. During exam 5, fewer than 20 % of the participants reported of having smoked over the past year.
Table 1 Characteristics of the male and female members of the Framingham Heart Study Offspring population in 1995 (exam 5)* (Mean values and standard deviations or percentages)
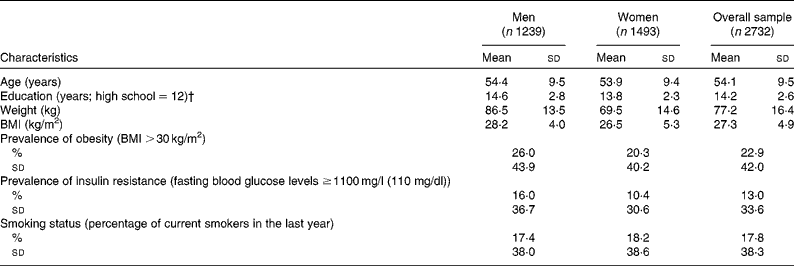
* Baseline (exam 5) descriptive characteristics including means and standard deviations are cross-sectional in nature and were computed using the SAS version 9.3.
† Recorded during exam 2; for a very small portion ( < 2 %) of this cohort, education may have been recorded at a pre-college age, so this value understates completed education.
Trends in dietary fat and macronutrient intakes in men and women
The percentage of energy derived from total fat increased in the overall population (27·3–29·8 %) and in men (27·5–29·7 %) and women (27·2–29·9 %) (Table 2). The percentage of energy derived from animal fat (16·1–17·2 %), vegetable fat (14·9–15·8 %), saturated fat (10·4–11·1 %), polyunsaturated fat (5·7–6·3 %), monounsaturated fat (11·1–12·4 %) and n-3 fat (0·1–0·2 %) also increased in both the sexes and in the population from exam 5 to exam 8 (P-trend < 0·01). The only exception was that derived from trans-fats, which decreased in both men (1·6–1·2 %) and women (1·5–1·2 %) (P-trend < 0·01). The percentage of energy derived from carbohydrate decreased among both men (50·1–46·0 % of energy) and women (51·7–47·4 % of energy), while that derived from protein (16·1–17·3 % of energy and 17·5–18·5 % of energy, respectively) increased (P-trend < 0·01). We also observed significant interactions by sex for saturated fat with women reporting a greater increase in saturated fat intake (percentage of energy) over time compared with men (β = 0·32 v. 0·22, P< 0·01) and for trans-fat with men reporting a greater decrease in trans-fat intake (percentage of energy) over time compared with women (β = − 0·13 v. − 0·09, P< 0·01) (Table 2). There was no statistical evidence of differences between men and women for trends in the intakes of any other fats.
Table 2 Trends in macronutrient and dietary fat intakes in men and women from 1991 to 2008* (Mean values and standard deviations)
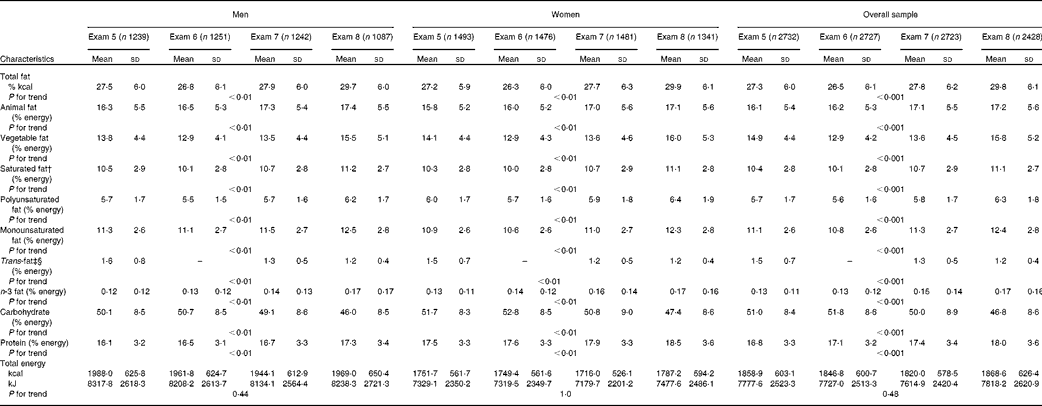
* The P values that are listed are for the overall trend and then for males and females, which were calculated using the statistical package R. The dietary trends were evaluated using a repeated-measures model with subject-specific random intercepts to account for serial correlation. Bonferroni corrections were applied to subgroup analyses in order to correct for multiple comparisons.
† P values for interaction by sex were calculated. There was a significant interaction by sex for saturated fat with women reporting a greater increase in saturated fat intake (% energy) over time compared with men (β = 0·32 v. 0·22, P< 0·01).
‡ Trans-fats data were not available for exam 6.
§ P values for interaction by sex were calculated. There was a significant interaction by sex for trans-fat with men reporting a greater decrease in trans-fat intake (percentage of energy) over time compared with women (β = − 0·13 v. − 0·09, P< 0·01).
Trends in dietary fat and macronutrient intakes in normal-weight, overweight and obese participants
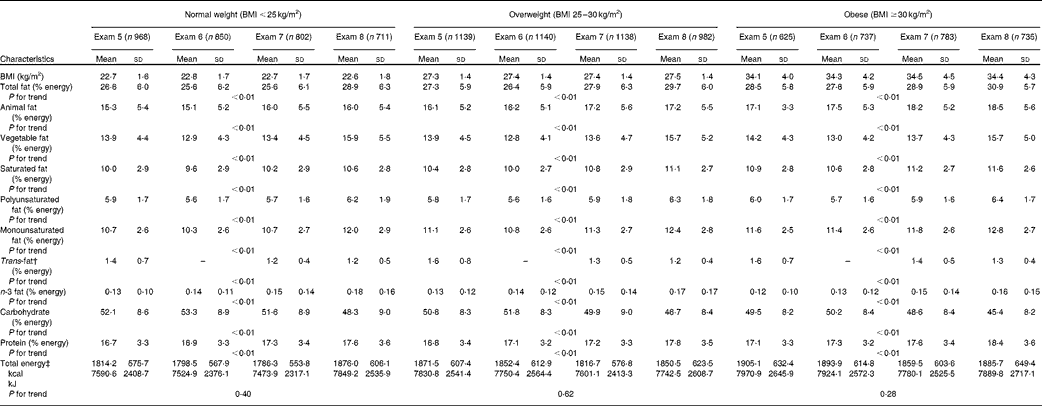
Trends in dietary fat intake were also stratified by BMI category (Table 3). As in the main analysis (Table 2), the percentage of energy consumed as fat and protein increased over time in all the BMI categories (P-trend < 0·01), while the percentage of energy derived from carbohydrate decreased (P-trend < 0·01). The percentage of energy derived from all types of fats, with the exception of that derived from trans-fat, increased (P-trend < 0·01), and there was no effect modification by BMI category. Trans-fat intake decreased over time across all the BMI categories (P-trend < 0·01). There was no significant difference by BMI category for trends in the intake of any of the dietary fats, but we observed a significant interaction by BMI category for total energy intake with energy intake increasing over time in normal-weight individuals (β = 13·2) and decreasing in overweight and obese individuals (β = − 10·7 and − 15·5, respectively). However, the trends in energy intake over time were not statistically significant within any of the BMI categories.
Table 3 Trends in macronutrient and dietary fat intakes in normal-weight and overweight participants from 1991 to 2008*(Mean values and standard deviations)

* The P values that are listed are for the overall trend for normal-weight, overweight and obese individuals, disaggregated, which were calculated using the statistical package R. The dietary trends were evaluated using a repeated-measures model with subject-specific random intercepts to account for serial correlation. Bonferroni corrections were applied to subgroup analyses in order to correct for multiple comparisons.
† Trans-fats data were not available for exam 6.
‡ P values for interaction by BMI category were calculated. There was a significant interaction by BMI category for total energy intake with energy intake increasing over time in normal-weight individuals (β = 13·2) and decreasing in overweight and obese individuals (β = − 10·7 and − 15·5, respectively). It is important to note that the FFQ is not sufficiently accurate to be able to detect changes in energy, so rather than discussing energy trends, all the analyses were adjusted for energy as a means of removing errors.
Trends in high-fat food intake among men and women
Food groups determined to be key contributors to dietary fat intake by the nationally representative Continuing Survey of Food Intakes by Individuals were selected a priori for the present analyses (Table 4) (Reference Cotton, Subar and Friday21). The food sources that contributed at least 1 % of dietary fat intake in the Continuing Survey of Food Intakes by Individuals, with the exception of total oils, were examined in the Framingham Offspring cohort; in descending order, these foods were beef, salad dressing/mayonnaise, oils, cheese, cakes, cookies, quick breads, doughnuts, and candy (confectioneries), margarine, other fats (shortening and animal fats), milk, poultry, pizza, chips and popcorn (snack foods), yeast bread, sausages/processed meats, ice cream, sherbet, and frozen yogurt, eggs, butter, and nuts and seeds(Reference Cotton, Subar and Friday21). Between 1991 and 2008 in the Framingham Offspring, the number of weekly servings of cheese, eggs, ice cream, sherbet and frozen yogurt, and nuts/seeds increased significantly in men, women and the overall population (P-trend < 0·01). The number of weekly servings of cakes, cookies, quick breads, doughnuts, and candy, margarine, milk, and pizza, chips and popcorn decreased over time in men, women and the overall population. Poultry intake decreased in the population (P-trend < 0·05), but not in men or women when the sexes were evaluated separately. The number of weekly servings of sausages/processed meats increased in the population (P-trend = 0·006), but no change in women or men was observed separately. The number of servings of butter increased in the population and among women (P-trend < 0·01), but not in men.
Table 4 Trends in the intakes of food sources of fats in men and women from 1991 to 2008 (Mean values and standard deviations)*†
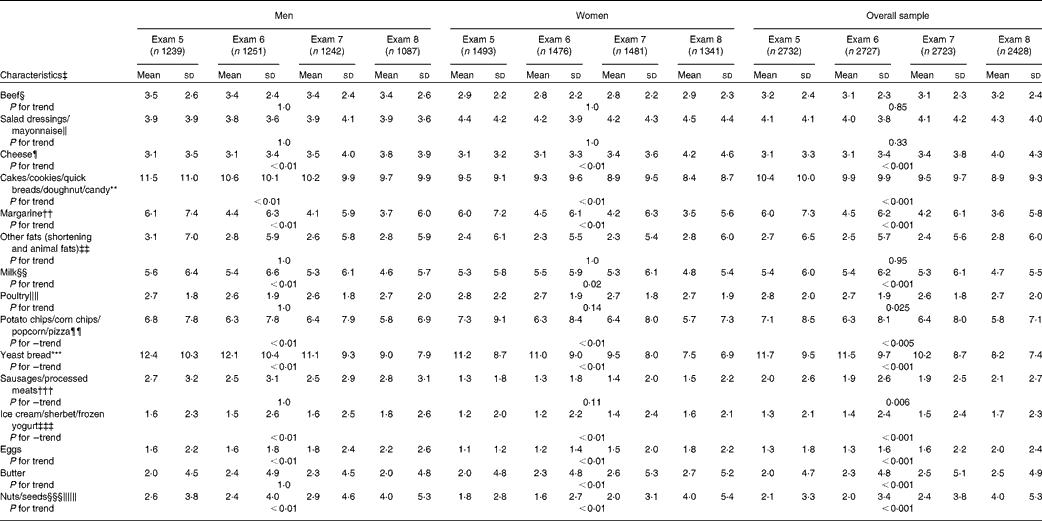
* The P values that are listed are for the overall trend and then for males and females, which were calculated using the statistical package R. The dietary trends were evaluated using a repeated-measures model with subject-specific random intercepts to account for serial correlation. Bonferroni corrections were applied to subgroup analyses in order to correct for multiple comparisons.
† The Framingham Heart Study researchers derived the number of continuous weekly servings of each food from categorical responses provided by participants in the FFQ.
‡ Based on food sources of total fat among US adults from the 1989–91 Continuing Survey of Food Intake by Individuals. Oils were also a primary source of total fat among US adults, but this information was not available for the Offspring cohort.
§ Includes hamburger, beef, pork and lamb as sandwich or mixed dish, and beef, pork and lamb as main dish.
∥ Includes oil and vinegar dressing and mayonnaise/creamy dressing.
¶ Includes cottage/ricotta cheese, cream cheese and other cheeses.
** Includes muffins/biscuits, pancakes/waffles, home-made cookies, ready-made cookies, brownies, doughnuts, home-made cake, ready-made cake, home-made sweet rolls, ready-made sweet rolls, home-made pie, ready-made pie, chocolate, candy bars and candy without chocolate.
†† Includes margarine added to food.
‡‡ Includes cream and sour cream.
§§ Includes skimmed or low-fat milk and whole milk.
∥∥ Includes chicken/turkey with skin and chicken/turkey without skin.
¶¶ Includes potato/corn chips, crackers, triskets, wheat thins, popcorn, pizza and French-fried potatoes.
*** Includes dark bread, white bread and English muffin/bagels.
††† Includes hot dogs, processed meats and bacon.
‡‡‡ Includes sherbet/ice milk and ice cream.
§§§ Includes nuts and peanut butter.
∥∥∥ P values for interaction by sex were calculated. There was a significant interaction by sex for nut intake with women reporting a greater increase in nut/seed intake over time compared with men (β = 0·69 v. 0·46, P< 0·01).
Trends in high-fat food intake among normal-weight, overweight and obese participants
The intakes of food groups determined to be key contributors of dietary fat intake in the Continuing Survey of Food Intakes by Individuals study population were examined by BMI category (normal weight, overweight and obese) (Table 5)(Reference Cotton, Subar and Friday21). Between 1991 and 2008, the number of weekly servings of cheese, eggs, ice cream, sherbet, and frozen yogurt, and nuts/seeds increased among the normal-weight, overweight and obese participants (P-trend < 0·05). The number of weekly servings of butter increased significantly in the overweight and obese groups (P-trend < 0·05), but not in the normal-weight participants. The number of servings of margarine and yeast breads decreased significantly among all the weight subgroups (P-trend < 0·01). The number of servings of cakes, cookies, quick breads, doughnuts and candy decreased in the overweight and obese groups (P-trend < 0·01), but not among the normal-weight participants. Similarly, the number of servings of pizza, chips and popcorn (snack foods) decreased among the obese individuals (P-trend < 0·01), but not in the normal-weight or overweight participants. No significant changes in the intake of the other food groups were observed.
Table 5 Trends in the intakes of food sources of fats in normal-weight and overweight participants from 1991 to 2008 (Mean values and standard deviations)*†
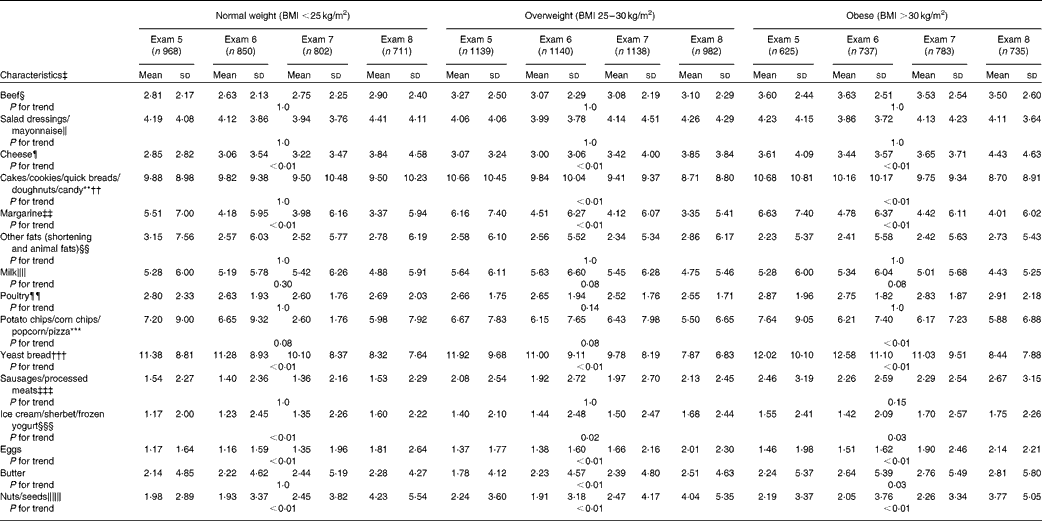
* The P values that are listed are for the overall trend for normal-weight, overweight and obese individuals, disaggregated, which were calculated using the statistical package R. The dietary trends were evaluated using a repeated-measures model with subject-specific random intercepts to account for serial correlation. Bonferroni corrections were applied to subgroup analyses in order to correct for multiple comparisons.
† The Framingham Heart study researchers derived the number of continuous weekly servings of each food from categorical responses provided by the participants in the FFQ.
‡ Based on food sources of total fat among US adults from the 1989–91 Continuing Survey of Food Intake by Individuals. Oils were also a primary source of total fat among US adults, but this information was not available for the Offspring cohort.
§ Includes hamburger, beef, pork, lamb as sandwich or mixed dish, and beef, pork, lamb as main dish.
∥ Includes oil and vinegar dressing and mayonnaise/creamy dressing.
¶ Includes cottage/ricotta cheese, cream cheese and other cheeses.
** Includes muffins/biscuits, pancakes/waffles, home-made cookies, ready-made cookies, brownies, doughnuts, home-made cake, ready-made cake, home-made sweet rolls, ready-made sweet rolls, home-made pie, ready-made pie, chocolate, candy bars, and candy without chocolate.
†† P values for interaction by BMI category were calculated. There was a significant interaction by BMI category for the intake of confectioneries (i.e. cakes/cookies/quick breads/doughnuts/candy) with normal-weight individuals reporting less of a decrease in confectionery intake over time compared with overweight and obese individuals (β = − 0·13 v. − 0·62, P< 0·01).
‡‡ Includes margarine added to food.
§§ Includes cream and sour cream.
∥∥ Includes skimmed or low-fat milk and whole milk.
¶¶ Includes chicken/turkey with skin and chicken/turkey without skin.
*** Includes potato/corn chips, crackers, triskets, wheat thins, popcorn, pizza and French-fried potatoes.
††† Includes dark bread, white bread and English muffin/bagels.
‡‡‡ Includes hot dogs, processed meats and bacon.
§§§ Includes sherbet/ice milk and ice cream.
∥∥∥ Includes nuts and peanut butter.
Discussion
In the present study, we investigated trends in dietary fat intake between 1991 and 2008 in the Framingham Offspring cohort, which consists of older, predominantly White American adults. Data obtained from the FHS provided a unique opportunity to observe a population's dietary patterns during a period when the prevalence of obesity and insulin resistance increased dramatically in the population (7·4 and 12·7 %, respectively, from exam 5 to exam 8) and nationwide(Reference Flegal, Carroll and Ogden2, Reference Ioannou, Bryson and Boyko22).
Based on the present analyses, it appears that the intake of foods rich in animal fat increased over time; however, the percentage of energy derived from animal fat did not increase markedly in men and women (16·3–17·4 % in men and 15·8–17·1 % in women, P< 0·01), probably due to a reduction in the animal fat content of the food supply during this period. The percentage of energy derived from vegetable fat increased substantively (13·8–15·5 % in men and 14·1–16·0 % in women, P< 0·01) and appears to be driven by an increased intake of nuts and seeds in this population. However, we were unable to examine trends in total oil intake in this population, which may have also contributed to an increase in vegetable fat intake over time. The reduction in trans-fat intake seems to be driven by a decrease in margarine intake. The intake of sources of fat from grain products decreased over time and may partly reflect the low-carbohydrate dietary messages that were circulating during this period. Importantly, the observed increase in the percentage of energy derived from dietary fats may partly be due to a reduction in carbohydrate intake over time, which is consistent with the enthusiasm for the low-carbohydrate trend beginning in the early 2000s(Reference Kuchler, Golan and Variyam5). This is noteworthy because the greatest increase in the percentage of energy derived from dietary fats occurred during exams 7 and 8 (1998–2008), suggesting a shift in consumer focus towards reducing dietary carbohydrate intake in lieu of reducing dietary fat intake.
Changes in macronutrient intake observed in the present study differ from those observed in the cross-sectional National Health and Nutrition Examination Survey (NHANES) analyses that have historically been used to evaluate secular trends in dietary intake nationwide. In the NHANES study, the percentage of energy derived from carbohydrate (44·0–48·7 %) increased, while that derived from fat (36·6–33·7 %) and protein (16·5–15·7 %) decreased between 1971–5 and 2005–6(Reference Austin, Ogden and Hill9). However, absolute fat intake in grams remained unchanged, indicating that the observed decrease in the percentage of energy derived from fat could be attributed to an increase in energy consumption(Reference Austin, Ogden and Hill9).
Trends in macronutrient intake within the NHANES 1999–2008 coinciding with the last decade of the Offspring cohort follow-up period are more congruent with the current FHS observations. During this period, energy intake remained stable in the NHANES study, and the percentage of energy derived from carbohydrate decreased, while that derived from protein increased(Reference Wright and Wang23), as noted in the FHS. However, unlike in the FHS population, no significant trends in fat intake were observed among the Caucasian NHANES participants(Reference Wright and Wang23).
The first numerical recommendation for dietary fat intake was established in the 1990 Dietary Guidelines for Americans, suggesting that adults limit their intake of total fat to ≤ 30 % of energy and saturated fat to ≤ 10 % of energy(Reference Frazao24, 25). The 2005 Dietary Guidelines liberalised the range for total dietary fat intake to 20–35 % of energy(26). In the Offspring cohort, dietary fat intake increased over time, but it always remained less than 30 % of total energy. The Offspring cohort (1991–2008) exceeded the recommended saturated fat limits and consistently consumed more than 10 % of total energy as saturated fat over time.
Discrepancies between NHANES study and FHS findings may be related to inherent differences between the two study samples as well as methodological differences. The mean age of members of the Offspring cohort (66·6 years in 2005–2008) is notably higher than that of the NHANES study participants (40·5 years in 2005–2006)(Reference Austin, Ogden and Hill9). Ageing can be associated with reduced food and energy intakes, which may clarify some of the observed differences in dietary composition between the samples(Reference Morley27). The Offspring population is predominantly Caucasian and middle- to older-aged, and therefore findings are not generalisable to the larger American population. It is also possible that the FHS participants are healthier than the majority of the US population based on their voluntary participation in a longitudinal health study.
Methodological differences between the FHS and NHANES study may also contribute to some of the observed dissimilarities. The FHS is a longitudinal study, while the NHANES study is cross-sectional. Additionally, most NHANES analyses rely on one or two 24 h recalls to assess dietary intake, while the FHS used a validated semi-quantitative FFQ(Reference Rimm, Giovannucci and Stampfer14). Each method has its own strengths and limitations. Data from one or two 24 h recalls may not capture usual long-term intakes(Reference Dodd, Guenther and Freedman28), while FFQ may be subject to recall bias, particularly in older populations(Reference Pope, Kritchevsky and Morris29). Moreover, FFQ are limited in their ability to precisely measure population mean intakes(Reference Schatzkin, Kipnis and Carroll30), thus attenuating any observed differences in consumption over time. Consequently, estimates obtained in the NHANES study and the FHS may not be directly comparable.
Some limitations of the present study should be noted. Ageing populations often consume less food over time(Reference Morley27), and since FFQ were unable to capture differences in portion size, over- or underestimation of macronutrient intake is possible. Importantly, while the nutrient database used to analyse the FFQ was updated over the study period to reflect changes in food composition and the market, FFQ do not capture absolute changes in macronutrient and high-fat food intakes, partly because they do not distinguish between low-fat and high-fat versions of foods. Furthermore, self-reported data in FFQ are especially prone to under-reporting(Reference Schatzkin, Kipnis and Carroll30). Despite the limitations of the FFQ, our estimates of fat intake are relatively consistent with those obtained in a previous analysis of the Offspring cohort that used 3 d food records to characterise dietary fat intake during exam 5(Reference Millen, Quatromoni and Franz31).
The present study makes an important contribution to the understanding of changes in dietary fat intake over the past two decades, among White American FHS participants. Our knowledge of trends in dietary fat intake in the USA has been drawn from the NHANES study population, in which secular rather than longitudinal trends were examined. The present prospective analyses uniquely provide insights into dietary fat intake over time among ageing individuals. Furthermore, we confirm earlier observations of the FHS(Reference Millen, Quatromoni and Gagnon32) with updated data to show that men and women embrace notably different eating patterns. Taken together, these observations suggest that tailoring dietary guidance by sex may be more effective for influencing positive dietary change than current population-based dietary guidelines.
In conclusion, despite national dietary guidance to reduce fat intake(Reference Austin, Ogden and Hill9), the proportion of energy derived from fat increased in the Framingham Offspring cohort during the 17-year study period. This observation paralleled a significant increase in the prevalence of obesity and insulin resistance in this population and nationwide(Reference Flegal, Carroll and Ogden2, Reference Ioannou, Bryson and Boyko22). Some favourable trends were observed in the present analyses, particularly an increase in vegetable intake when compared with animal fat intake and a decrease in trans-fat intake. Additionally, overall dietary fat intake remained below the recommended level of less than 35 % of total energy per the US Dietary Guidelines, although this may reflect the concomitant decrease in carbohydrate intake(25, 26). The increase in the percentage of energy derived from saturated fat in excess of the recommended limit of less than 10 % of total energy, particularly among women, warrants policy consideration given its associations with poor health outcomes(Reference Ortega, Varela and Bermudez33). FFQ are known to underestimate intake(Reference Schatzkin, Kipnis and Carroll30), suggesting that the present analyses may minimise the importance of these findings. Policies targeting the price and availability of foods in the marketplace have been shown to be more effective for influencing dietary changes than interventions that increase nutrition knowledge alone(Reference Brambila-Macias, Shankar and Capacci34). Our research supports the growing body of evidence that current strategies to improve dietary intake are insufficient at the population level.
Acknowledgements
Publicly available data from the FHS were utilised in the present study for secondary analyses. The FHS is conducted and supported by the National Heart, Lung, and Blood Institute in collaboration with Boston University (contract no. N01-HC-25 195). Funding support for the Framingham FFQ datasets was provided by ARS contract no. 53-3k06-5-10, ARS agreement no. 58-1950-9-001, 58-1950-4-401 and 58-1950-7-707. This manuscript was not prepared in collaboration with the investigators of the FHS and does not necessarily reflect the opinions or views of the FHS, Boston University or National Heart, Lung, and Blood Institute.
The present study was supported by the American Cancer Society Research Scholar Grant (no. RSG-12-005-01-CNE) and New York University's IDEA Research Challenge Grant awarded to N. P. The American Cancer Society had no role in the design and analysis of the study or in the writing of this article.
The authors' contributions are as follows: M. V. wrote the paper and assisted with the designing of the analyses; M. S. conducted the statistical analyses and reviewed the manuscript for statistical accuracy of results; P. Q. and P. J. provided insights into the review and revision of the manuscript for important intellectual content; N. P. developed the overall research plan, designed the analyses, reviewed the manuscript for important intellectual content, and had primary responsibility for the final content; N. P. was responsible for overseeing the entire study.
None of the authors has any conflicts of interests to declare.