Hypertension is a major risk factor for the development and progression of microvascular and macrovascular chronic diabetic complications(1). Clinical trials have also demonstrated that lowering blood pressure (BP) reduced ischaemic cardiac events, stroke and nephropathy in patients with diabetes(2). In a multifactorial interventional study, patients with type 2 diabetes and a tight BP control – target systolic BP < 130 mmHg – had reduced cardiovascular deaths and events(Reference Gaede, Lund-Andersen and Parving3). Furthermore, guidelines recommend that the BP target for hypertensive patients with diabetes should be < 130 mmHg for systolic BP and < 80 mmHg for diastolic BP(Reference Chobanian, Bakris and Black4–6).
Dietary intervention reduces BP, prevents or delays the development of hypertension, enhances antihypertensive drug efficacy and decreases cardiovascular risk(Reference Chobanian, Bakris and Black4, Reference Buse, Ginsberg and Bakris5). Most of the dietary recommendations for hypertension include reduction of Na intake, moderation of alcohol consumption and the adoption of the Dietary Approaches to Stop Hypertension (DASH) diet eating plan(Reference Chobanian, Bakris and Black4, Reference Appel, Moore and Obarzanek7, Reference Sacks, Svetkey and Vollmer8). The DASH diet emphasises the consumption of fruits, vegetables and low-fat dairy foods; includes whole grains, poultry, fish, and small amounts of red meat, sweets and sugar-containing beverages. There are few data concerning the role of the DASH diet in BP, in patients with type 2 diabetes(Reference Gunther, Liese and Bell9). Therefore, the aim of the present study was to evaluate possible associations of the recommended food groups of the DASH diet eating plan with BP values in patients with type 2 diabetes.
Materials and methods
Patients
The present cross-sectional study was conducted in patients with type 2 diabetes, defined as subjects over 30 years of age at onset of diabetes, no previous episode of ketoacidosis or documented ketonuria and, if insulin users, the treatment with insulin began only 5 years after the diagnosis. The study recruited outpatients who consecutively attended the Endocrine Division of the Hospital de Clínicas de Porto Alegre, Brazil, and had not received any dietary counselling by a registered dietitian during the previous 6 months. Patient selection was as follows: BMI ≤ 40 kg/m2; serum creatinine < 176 mmol/l; urinary albumin excretion (UAE) < 300 mg/24 h. Patients with macroalbuminuria (UAE ≥ 300 mg/24 h) were not studied since they usually receive specific dietary recommendations. All medications in use were maintained during the study. Among 234 eligible patients, four patients refused to participate and five were excluded due to compliance issues. Thus, 225 patients were included.
The study was conducted according to the guidelines laid down in the Declaration of Helsinki and all procedures involving patients were approved by the Hospital Ethics Committee. Written informed consent was obtained from all patients.
Clinical evaluation
The frequency of exercise, according to activities during a typical day(Reference Tuomilehto, Lindstrom and Eriksson10), was classified into four levels based on an adapted questionnaire. Consumption of any kind of alcoholic beverage was considered as a positive alcohol intake. Patients were classified as current smokers or not and were self-identified as white or non-white.
Sitting BP was measured twice to the nearest 2 mmHg, after a 10 min rest, using an Omron HEM-705CP digital sphygmomanometer (Omron Healthcare, Inc., Bamockburn, IL, USA). Mean BP (MBP) was calculated by the following equation: systolic BP+(2 × diastolic BP)/3. Hypertension was defined as BP ≥ 140/90 mmHg, measured on two separate occasions or use of antihypertensive drugs(Reference Chobanian, Bakris and Black4). Abnormal waist circumference was considered as values >94 cm for men and >80 cm for women(Reference Alberti, Eckel and Grundy11).
Patients were classified as normoalbuminuric (UAE < 30 mg/24 h) or microalbuminuric (UAE 30–300 mg/24 h). Microalbuminuria was always confirmed(Reference Gross, Azevedo and Silveiro12).
Nutritional evaluation
The body weight and height of patients were obtained and BMI was calculated. Waist circumference was measured midway between the lowest rib margin and the iliac crest with a flexible fibreglass tape.
The usual diet was assessed by 3 d weighed-diet records as standardised previously(Reference Moulin, Tiskievicz and Zelmanovitz13). Briefly, patients were issued commercial scales and measuring cups. Compliance with this technique was confirmed by comparing estimated protein intake from diet records (0·96 (sd 0·19) g/kg weight) with protein intake from 24 h urinary N output (0·96 (sd 0·18) g/kg weight; P = 0·902). Completeness of urine collection was confirmed by 24 h urinary creatinine measurements.
Nutrients from the dietary records were analysed using Nutribase 2007 Clinical Nutritional Manager software version 7.14 (Cybersoft, Phoenix, AZ, USA) and updated(14). Most data (61 %) were collected in winter and autumn.
The 24 h glycaemic index (GI) was estimated by the weighted GI value of each consumed food at 24 h and expressed as percentage(15). The values of the GI and available carbohydrates of each food were obtained(Reference Atkinson, Foster-Powell and Brand-Miller16) and glucose was used as the reference food. Dietary glycaemic load was calculated as the product of dietary GI and total carbohydrate intake divided by 100(Reference Brand-Miller, Thomas and Swan17).
A DASH diet score was created to evaluate compliance with the DASH diet recommendations(Reference Appel, Moore and Obarzanek7, Reference Sacks, Svetkey and Vollmer8). The following eight food groups based on the original DASH diet eating plan(Reference Appel, Moore and Obarzanek7) were included in this score: fruits; vegetables; low-fat dairy foods; whole grains; red meat, poultry and fish; nuts, seeds and beans; oils and fats; sweets. Each food group, expressed as daily portions, contributed equally to the total score (eight points = full compliance). Serving size specifications for the score were matched and adapted to the original plan of the DASH diet and the document of the US Department of Health and Human Services(Reference Appel, Moore and Obarzanek7, 18). In the present study, the number of portions for each food group, based on DASH diet recommendations(Reference Appel, Moore and Obarzanek7), was adjusted for 4184 kJ (1000 kcal) of total energy intake. Therefore, in the created score, the established daily portions per 4184 kJ (1000 kcal) were: 80 g for fruits; 50 g for vegetables; 120 ml for milk or 40 g for cheese; 30 g for nuts or 80 g for beans; 5 g for sweets; < 170 g for meats; 20 g for whole grains; 5 ml for oils or margarines.
In the description of the selected foods, fruits included juices and raw fruits, dairy products included milk, yogurt and cheese, and vegetables included raw/cooked vegetables. The category of legumes and nuts included beans, lentils, peanuts and all kinds of nuts. Whole grains included whole-wheat or rye bread, and oat bran, and other whole grains. Sweets included sweet foods and beverages. The term ‘lean meats’ indicated red and white lean meat and their by-products. White meat included fish, shellfish and their products, and poultry and their processed products. Oil intake represented the amount of daily table oil intake by the participants at each shared mealtime. Total margarine intake included soft and margarine-like spread.
Laboratory measurements
Blood samples were obtained after a 12 h fast. Plasma glucose was determined by a glucose oxidase method, creatinine values by Jaffe's reaction, HbA1c by an ion-exchange HPLC procedure (reference range 4·7–6·0 %), total cholesterol and TAG by enzymatic colorimetric methods and HDL by the homogeneous direct method. LDL-cholesterol was calculated using Friedewald's formula: LDL = total cholesterol − HDL-cholesterol − (TAG/2·2)(Reference Friedewald, Levy and Fredrickson19). UAE was measured by immunoturbidimetry (Ames-Bayer, Tarrytown, NY, USA).
Statistical methods
The estimated number of included patients (n 210) was based on a 5·5 mmHg reduction in systolic BP(Reference Appel, Moore and Obarzanek7), with a power of 80 % and an α of 0·05. Student's t test, the Mann–Whitney U test and Pearson's χ2 were used as appropriate. Multivariate logistic regression analyses were used to calculate the OR for HIGH BP values (second plus third tertiles) using the lowest tertile of BP as the reference, adjusted for potential confounders. Results are expressed as means and standard deviations, or medians (P25–P75). P values < 0·05 (two-sided) were considered as statistically significant. Statistical analysis was performed using SPSS 17.0 software (SPSS, Chicago, IL, USA).
Results
A total of 225 patients aged 61·1 (sd 10·4) years, with 13·1 (sd 9·1) years of diabetes duration, 48·4 % of males, HbA1c of 7·1 (sd 1·3) %, systolic BP of 136·7 (sd 20·0) mmHg and diastolic BP of 78·4 (sd 11·8) mmHg, were studied. The majority of the patients were sedentary (86·3 %), 23 % had microalbuminuria and 82·2 % were hypertensive.
The recommended food groups of the DASH diet were initially evaluated according to MBP tertiles. In general, no differences in the intake of these components were observed among the BP tertiles (ANOVA; P>0·05 for all). The absolute values of intake in the highest tertiles were very similar. For instance, the daily consumption of fruits in tertiles of MBP was 1·9 (sd 1·3), 1·7 (sd 1·1) and 1·7 (sd 1·4) portions per 4184 kJ (1000 kcal), in the first, second and third tertiles, respectively (P = 0·415). Therefore, in all analyses, we decided to divide the patients into two groups: HIGH BP group, which included patients from the second and third tertiles of BP and LOW BP group, with patients from the first BP tertile.
Characteristics of patients according to blood pressure groups
Characteristics of patients according to HIGH MBP (MBP ≥ 92 mmHg) and LOW MBP (MBP < 92 mmHg) are described in Table 1. The HIGH MBP group had a significantly shorter duration of diabetes, lower urinary K excretion, and higher BMI, HbA1c and UAE values than patients in the LOW MBP group. Patients with HIGH MBP more frequently had abnormal waist circumference and microalbuminuria. Angiotensin-converting enzyme inhibitors and diuretics were the most often used antihypertensive drugs and their use was significantly more frequent in the LOW MBP group. Regarding the current alcohol consumption, in the sixty patients who reported consuming any alcoholic beverages (26·6 % of the studied sample), the median weekly intake was 175·0 ml (87·5–350·0 ml). The proportion of patients who drank more than 175·0 ml/week in the group with HIGH MBP was 58·1 % and in the group with LOW MBP, 41·9 % (P = 0·752).
Table 1 Clinical and laboratory characteristics of patients with type 2 diabetes according to mean blood pressure (MBP)
(Mean values and standard deviations, median values and percentiles, or percentages)

UAE, urinary albumin excretion; ACE, angiotensin-converting enzyme.
* Student's t test.
† Pearson's χ2.
‡ >94 cm for men and >80 cm for women.
§ Mann–Whitney U test.
The daily intake of nutrients is shown in Table 2. The intake of carbohydrates and soluble fibres was lower in patients with HIGH MBP compared with patients with LOW MBP, without any difference between the groups in the consumption of other nutrients. The 24 h glycaemic load was higher in patients from the HIGH MBP group compared with the LOW MBP group (108·6 (sd 33·3) g v. 99·0 (sd 30·2) g; P = 0·037). The daily intakes of each food group of the DASH diet eating plan are described in Table 3. Patients with HIGH MBP consumed (g/kg weight) less fruits, vegetables and oils than patients with LOW MBP; also, their intake (portions per 4184 kJ (1000 kcal)) of dairy foods was lower. Considering the number of recommended food portions in the original DASH diet(Reference Appel, Moore and Obarzanek7), patients with HIGH MBP had a lower consumption of vegetables and sweets than the LOW MBP group.
Table 2 Daily intake of nutrients in patients with type 2 diabetes according to mean blood pressure (MBP)
(Mean values and standard deviations)
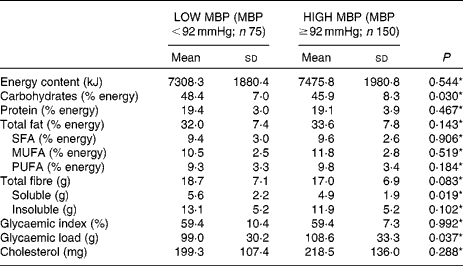
* Student's t test.
Table 3 Daily intake of Dietary Approaches to Stop Hypertension (DASH) diet food groups in patients with type 2 diabetes according to mean blood pressure (MBP)
(Mean values and standard deviations, median values and percentiles, or percentages)

* Student's t test.
† Mann–Whitney U test.
‡ Recommended food portions in the original DASH diet eating plan(7).
§ Pearson's χ2.
Intake of the recommended foods in the DASH diet was also evaluated in patients with HIGH and LOW systolic and diastolic BP. The intake of fruits (3·8 (sd 2·5) v. 3·1 (sd 2·4) g/kg; P = 0·032) and oils (0·4 (sd 0·2) v. 0·3 (sd 0·2) g/kg; P = 0·029) was lower in patients with HIGH systolic BP ( ≥ 125 mmHg) than with LOW systolic BP ( < 125 mmHg). Additionally, the intake of fruits (3·8 (sd 2·4) v. 3·1 (sd 2·4) g/kg; P = 0·040) and dairy foods (3·6 (sd 2·9) v. 2·7 (sd 2·6) g/kg; P = 0·017) was lower in patients with HIGH diastolic BP ( ≥ 73 mmHg) than with LOW diastolic BP ( < 73 mmHg). The intake of other DASH diet food groups was not different.
Dietary Approaches to Stop Hypertension score
The mean DASH score of all patients was 4·36 (sd 1·34). Patients with a DASH score of >4 (n 98) had lower UAE (24·5 (2·9–253·4) v. 33·9 (3·0–563·8) mg/24 h; P = 0·038) and higher HDL-cholesterol (1·3 (sd 0·4) v. 1·2 (sd 0·3) mmol/l; P = 0·018) than patients with a DASH score of ≤ 4. MBP values were not different between patients with scores >4 and ≤ 4 (100·2 (sd 14·7) v. 97·1 (sd 12·2) mmHg; P = 0·120).
Multivariate logistic regression models
Associations of the daily intake of selected DASH diet foods with MBP were evaluated in multivariate logistic regression analyses (Table 4). All models were adjusted for abnormal waist circumference, UAE, duration of diabetes and HbA1c. Abnormal waist circumference was included as a covariate because the proportion of abnormal waist circumference was significantly different (P < 0·0001) in men (73·4 %) and in women (94·8 %), besides being different in the MBP groups. The intake of fruits or vegetables reduced the chance of the presence of HIGH MBP ( ≥ 92 mmHg).
Table 4 Multiple logistic regression analyses: daily intake of Dietary Approaches to Stop Hypertension (DASH) diet food groups and their OR for HIGH mean blood pressure (MBP) values (dependent variable)
(Odd ratios and 95 % confidence intervals)

* Regression models adjusted for abnormal waist circumference, urinary albumin excretion, diabetes duration and HbA1c.
† Recommended portions in the DASH diet eating plan.
In practical terms, consumption of 80 g of fruits (1 portion of fruits per 4184 kJ (1000 kcal)) or 50 g of vegetables (1 portion of vegetables per 4184 kJ (1000 kcal)) reduced the chance of HIGH MBP by 22 % each. In addition, patients who consumed >105 g of vegetables (or >2·1 portions per 4184 kJ (1000 kcal)) had a 50 % reduction in the chance of presenting HIGH MBP values.
Discussion
The present study demonstrated that in patients with type 2 diabetes, the consumption of foods recommended in the DASH diet, especially fruits and vegetables, was associated with reduced MBP values. Each daily portion per 4184 kJ (1000 kcal) of fruits (80 g) or vegetables (50 g) reduced the chance of the presence of an MBP ≥ 92 mmHg by 22 %, adjusted for abnormal waist circumference, UAE, diabetes duration and HbA1c.
The association of a high intake of fruits and vegetables with reduced BP was fully demonstrated in the SU.VI.MAX (Supplémentation en Vitamines et Minéraux Antioxydants)(Reference Dauchet, Kesse-Guyot and Czernichow20) cohort. In that study, the intake of more than five daily portions of fruits and vegetables during 5 years promoted a smaller increase in BP than lower intakes. The present study confirmed previous associations observed in subjects without diabetes and from different ethnic groups(Reference Miura, Greenland and Stamler21, Reference Alonso, Fuente and Martı'n-Arnau22).
Only one study examined the relationship between the DASH diet and BP in diabetes(Reference Gunther, Liese and Bell9). In that study, both patients with type 1 (n 2440) and type 2 diabetes (n 390) were included. The compliance with DASH diet recommendations was associated with low BP only in type 1 diabetes. The negative results in patients with type 2 diabetes, contrary to the results from the present study, could have been related to the use of the FFQ, a less accurate dietary tool than the weighed-diet records that we used. This limitation was probably overcome in type 1 patients by the large number of studied patients. Furthermore, their patients were younger (less than 20 years old) and had lower BP levels ( < 120/80 mmHg) than our patients.
The mechanisms and the role of each nutrient and/or food linked to the beneficial effect of the DASH diet on BP are not fully established. An important point to consider when reduction of BP values is evaluated, besides the reduction of Na intake(Reference Appel, Moore and Obarzanek7, Reference Sacks, Svetkey and Vollmer8), is the increased K intake. A possible explanation is the intake of fruits and vegetables due to their high K content(23, Reference Mierlo, Greyling and Zock24). In fact, in the present study, patients with LOW MBP consumed more fruits and vegetables and had 24 h urinary K higher than patients with HIGH MBP. Another reason for low BP values associated with fruit and vegetable intakes could be related to their intake of high fibre content. The effect of fibre intake on BP could be explained by its effects on improving insulin sensitivity(Reference Ard, Grambow and Liu25) along with a reduction of BMI(Reference Steffen, Kroenke and Yu26). In the present study, it was observed that patients in the LOW MBP group consumed more fibre. We have also previously demonstrated in patients with type 2 diabetes that the intake of soluble fibres can be protective for the presence of the metabolic syndrome(Reference Steemburgo, Dall'Alba and Almeida27), a condition in which high BP is particularly common.
It is known that high-GI foods increase plasma glucose(Reference Jenkins, Wolever and Taylor28) and low-GI diets improve glucose control in patients with diabetes(Reference Thomas and Elliott29). In this sense, one point of concern could be a deleterious effect on glycaemic control of the intake of fruits and certain types of vegetables due to their carbohydrate content. The present results demonstrated that glycaemic load was actually lower in patients with LOW MBP who consumed more fruits and vegetables. The high fibre intake in these patients compared with the HIGH MBP group can explain this low glycaemic load value.
A potential limitation of the present study would be that the results could not be generalised. For instance, in our state, located in the south of Brazil, people eat cottage cheese and sausages, foods that are not common in the northern part of the country. The inclusion of other typical regional foods with complex and different nutrients could blunt the beneficial effects of fruits and vegetables on BP. Another shortcoming could involve dietary records. The food-frequency techniques, used in most observational studies, are limited due to the lack of accuracy for quantitative data. However, in the present study, diet was assessed by a standardised 3 d weighed-diet record technique, which includes a 24 h urinary urea measurement to validate dietary intake estimated from records(Reference Moulin, Tiskievicz and Zelmanovitz13). In fact, this dietary tool has been used to confirm dietary compliance in studies with diabetic patients(Reference Moulin, Tiskievicz and Zelmanovitz13, Reference Gross, Zelmanovitz and Moulin30–Reference Mello, Zelmanovitz and Azevedo32). The use of MBP instead of a conventional BP measurement might also be a limitation. However, we think the strength of the present study is that it describes an original association of dietary factors with BP in diabetic patients. Actually, these results should be confirmed in a large sample of patients with diabetes. Finally, another limitation of the present study could be attributed to its cross-sectional design that precludes a causal relationship between food intake and BP.
The mean DASH diet score of patients in the present study was 4·36 (sd 1·34). None of the patients reached the maximum of eight points in the created DASH diet score. This means that patients with type 2 diabetes complied with only about 50 % of the DASH diet recommendations. An even lower compliance with the DASH dietary pattern (about 20 %) occurred in hypertensive patients without diabetes, as demonstrated recently(Reference Mellen, Gao and Vitolins33). The reason for the lack of compliance observed in different clinical settings should be investigated in order to improve the role of this dietary intervention in hypertensive patients. The importance of the DASH diet recommendations is reinforced by the demonstration in the present study that minor dietary changes, such as the daily intake of >105 g of vegetables, can significantly reduce the chance of having HIGH MBP by more than 50 %. Also, the intake of fruits can protect patients from HIGH MBP. Therefore, fruits and vegetables should always be emphasised as part of the dietary recommendations for hypertensive patients with type 2 diabetes. These results should be confirmed in patients with diabetes in prospective cohort studies and randomised clinical trials.
In conclusion, fruit and vegetables were the food groups of the DASH diet associated with reduced BP values in patients with type 2 diabetes and their consumption might play a protective role for increased BP values.
Acknowledgements
The authors declare that there is no conflict of interest. This study was partially supported by grants from Projeto de Núcleos de Excelência do Ministério de Ciência e Tecnologia, Ministério de Ciência e Tecnologia, Conselho Nacional de Desenvolvimento Científico e Tecnológico (MCT/CNPq no. 502050/2005-5) and FIPE-Hospital de Clínicas de Porto Alegre. T. P. d. P., T. S. and V. D. A. were recipients of scholarships from Fundação Coordenação de Aperfeiçoamento de Pessoal de Nível Superior and CNPq, respectively. The contributions of the authors were as follows: T. P. d. P. was involved in study design data collection and management, statistical analyses and interpretation, and manuscript writing; J. C. d. A. and V. D. A. were involved in the study design, data collection and management; T. S. was involved in the statistical analyses and interpretation, and manuscript writing; J. L. G. was involved in the study design, statistical interpretation and manuscript writing. M. J. d. A. is the head of the project and carried out all parts of the research and is central in the writing of the manuscript.








