Introduction
Frailty is a multi-dimensional, clinical condition characterised as a state of increased vulnerability to adverse health outcomes when exposed to a stressor, for example, a chronic disease diagnosis, an acute infection or a fall (Clegg et al. Reference Clegg, Young, Iliffe, Rikkert and Rockwood2013; Lang et al. Reference Lang, Hubbard, Andrew, Llewellyn, Melzer and Rockwood2009; Topinková Reference Topinková2008). Evidence suggests that frailty is a dynamic process, transitioning from robustness through a sometimes clinically silent, pre-frail condition to a frail outcome (Ferrucci et al. Reference Ferrucci, Guralnik, Studenski, Fried, Cutler and Walston2004). During this process, total physiologic reserves dissipate and individuals become less able to remain active and cope with daily stressors or acute illnesses. Consequently, frailty is associated with disease, dependency and ultimately death, as well as entailing a high demand for, and utilisation of formal and informal health-care services (Young Reference Young2003), social and community services and other resources (Auyeung et al. Reference Auyeung, Lee, Kwok and Woo2011; Fried et al. Reference Fried, Tangen, Walston, Newman, Hirsch, Gottdiener, Seeman, Tracy, Kop, Burke and McBurnie2001; Rockwood et al. Reference Rockwood, Mitnitski, Song, Steen and Skoog2006).
Given that frailty is dynamic, research suggests it can be considered a malleable and manageable condition and, therefore, there may be opportunities along its pathway to halt, reverse, manage and/or prevent its adverse consequences and worsening (Andreasen et al. Reference Andreasen, Lund, Aadahl and Sørensen2015; Cameron et al. Reference Cameron, Fairhall, Langron, Lockwood, Monaghan, Aggar, Sherrington, Lord and Kurrle2013; Cesari et al. Reference Cesari, Marzetti, Thiem, Pérez-Zepeda, Abellan Van Kan, Landi, Petrovic, Cherubini and Bernabei2016; Gill et al. Reference Gill, Baker, Gottschalk, Peduzzi, Allore and Byers2002; Kapan et al. Reference Kapan, Luger, Haider, Titze, Schindler, Lackinger and Dorner2016; Ng et al. Reference Ng, Feng, Nyunt, Feng, Niti, Tan, Chan, Khoo, Chan, Yap and Yap2015; Theou et al. Reference Theou, Stathokostas, Roland, Jakobi, Patterson, Vandervoort and Jones2011). Positive prevention strategies include being pro-active about one's own life and engaging in healthy lifestyle choices, particularly in terms of maintaining a healthy weight, adequate nutrition, exercise and not smoking (Zuliani et al. Reference Zuliani, Soavi, Maggio, De Vita, Cherubini and Volpato2015). Physical exercise, particularly resistance exercise, has been well studied and has been found to be beneficial in terms of preventing and treating frailty and improving functional performance (Alexander et al. Reference Alexander, Galecki, Grenier, Nyquist, Hofmeyer, Grunawalt, Medell and Fry-Welch2001; De Vreede et al. Reference De Vreede, Samson, Van Meeteren, Duursma and Verhaar2005; Manini et al. Reference Manini, Marko, VanArnam, Cook, Fernhall, Burke and Ploutz-Snyder2007). Changes to diet alone are less successful in preventing or reversing frailty without an associated exercise component (Zuliani et al. Reference Zuliani, Soavi, Maggio, De Vita, Cherubini and Volpato2015), although an adequate intake of protein, calories and vitamin D are critical (Zuliani et al. Reference Zuliani, Soavi, Maggio, De Vita, Cherubini and Volpato2015).
Screening programmes provide the potential to identify frailty at a population level and ensure that preventative therapeutic measures and intervention strategies can be properly targeted at both societal and individual levels, in order to help to manage health-care costs and resources while improving individual health and wellbeing (Cherniack, Flores and Troen Reference Cherniack, Flores and Troen2007; Galvin and Todres Reference Galvin and Todres2011). This study aims to explore and better understand how frailty prevention and screening for frailty would be accepted and adopted by frail and non-frail older adults, by family care-givers, and health and social care professionals.
Although there is no benchmark definition of frailty, the two most widely accepted and cited assessment tools are based on Fried's phenotype (Fried et al. Reference Fried, Tangen, Walston, Newman, Hirsch, Gottdiener, Seeman, Tracy, Kop, Burke and McBurnie2001, Reference Fried, Ferrucci, Darer, Williamson and Anderson2004) and an accumulation of deficits frailty index (Rockwood and Mitnitski Reference Rockwood and Mitnitski2011, Reference Rockwood and Mitnitski2007). These are documented here for clarity and completeness. Fried's phenotype conceptualises frailty as a biological syndrome resulting from deficits in five physiological domains: global weakness, overall slowness, exhaustion, low physical activity and unintentional weight loss. A ‘pre-frail’ state is indicated by two of these symptoms, three or more indicating a ‘frail’ state. Alternatively, a frailty index (Rockwood and Mitnitski Reference Rockwood and Mitnitski2007) operationalises frailty as a risk state by calculating the proportion of a set of health ‘deficits’ manifest in the individual. This model incorporates physical impairments and disability, as well as polypharmacy, cognitive impairments, psycho-social risk factors and geriatric syndromes (e.g. falls, delirium and urinary incontinence). Both identify an overlapping population at high risk of poor prognosis. Depending on the definition, estimates of frailty in older adults (over 65 years) vary from 4 to 17 per cent, with the prevalence of pre-frailty ranging between 19 and 59 per cent (Collard et al. Reference Collard, Boter, Schoevers and Voshaar2012). Irrespective, these perspectives and statistics underline that frailty is a threatening condition for older adults that is placing a burden on health and social care budgets.
Whereas the earlier conceptualisations of frailty were dominated by a medical paradigm focusing on a biological syndrome, a broader multi-dimensional approach (Rodríguez-Mañas et al. Reference Rodríguez-Mañas, Féart, Mann, Viña, Chatterji, Chodzko-Zajko, Gonzalez-Colaço Harmand, Bergman, Carcaillon, Nicholson, Scuteri, Sinclair, Pelaez, Van der Cammen, Beland, Bickenbach, Delamarche, Ferrucci, Fried, Gutiérrez-Robledo, Rockwood, Rodríguez Artalejo, Serviddio and Vega2013; Walston et al. Reference Walston, Hadley, Ferrucci, Guralnik, Newman, Studenski, Ershler, Harris and Fried2006) has been adopted more recently to acknowledge psychological elements like quality of life, as well as social elements such as lack of social contacts, situational factors and wellbeing (Langlois et al. Reference Langlois, Vu, Kergoat, Chassé, Dupuis and Bherer2012; Rodríguez-Mañas et al. Reference Rodríguez-Mañas, Féart, Mann, Viña, Chatterji, Chodzko-Zajko, Gonzalez-Colaço Harmand, Bergman, Carcaillon, Nicholson, Scuteri, Sinclair, Pelaez, Van der Cammen, Beland, Bickenbach, Delamarche, Ferrucci, Fried, Gutiérrez-Robledo, Rockwood, Rodríguez Artalejo, Serviddio and Vega2013; Todres, Galvin and Dahlberg Reference Todres, Galvin and Dahlberg2006). In addition, (Grenier Reference Grenier2005, Reference Grenier2006) highlighted the negative emotions felt, such as fear, in response to functional limitations and growing incapacities. Hence, the subjective meanings one attributes to becoming frail can be experienced deeply; Shaw et al. (Reference Shaw, West, Hagger and Holland2016b) developed Fillit and Butler's (Reference Fillit and Butler2009) notion that becoming frail could be experienced as ontologically challenging. This threat to self was explored in depth by Warmoth et al. (Reference Warmoth, Lang, Phoenix, Abraham, Andrew, Hubbard and Tarrant2016) who found that self-identifying as frail could signal ‘giving up’ and withdrawal from the social world. The meaning of becoming frail therefore needs to be encompassed in future interventions. A recent study tested a domiciliary intervention including physical training, nutrition advice and social support (Luger et al. Reference Luger, Dorner, Haider, Kapan, Lackinger and Schindler2016). Multi-component interventions of this nature may prevent future health risk and isolation.
However, older adults’ and other stakeholders’ views on frailty screening have not been sought. Although previous public health campaigns have demonstrated the benefits of screening and interventions to identify and treat high-risk individuals (e.g. Cochrane et al. Reference Cochrane, Davey, Iqbal, Gidlow, Kumar, Chambers and Mawby2012; Holland et al. Reference Holland, Cooper, Shaw, Pattison and Cooke2013; NHS Health Check 2012; Nnoaham et al. Reference Nnoaham, Frater, Roderick, Moon and Halloran2010), frailty screening may not be universally popular or even acceptable to the general population of older adults, their care-givers or other stakeholders, including the health and social care staff who may have to conduct assessments or deliver interventions. Studies have shown that older adults are more likely to refuse health-care services than younger groups (Littlechild and Glasby Reference Littlechild and Glasby2000). They are also more likely to cite barriers to screening in terms of the costs in accessing screening including transport services and the screening location (Waller et al. Reference Waller, Jackowska, Marlow and Wardle2012). Other systematic reviews on barriers to screening have noted that female gender, ethnicity, low educational attainment and fear of having the screening test all contribute to lower uptake of population screening programmes by older adults (Guessous et al. Reference Guessous, Dash, Lapin, Doroshenk, Smith and Klabunde2010).
Similarly, other stakeholders, including health and social care professionals involved in screening and intervention programmes, cite barriers to screening in terms of their belief in the efficacy (UK CRC 2003) of the screening or intervention, as well as expectations about its implementation, structure or deliverability (e.g. Holland et al. Reference Holland, Cooper, Shaw, Pattison and Cooke2013; Shaw et al. Reference Shaw, Holland, Pattison and Cooke2016a). Understanding and clarifying the issues faced by these professionals is essential in determining whether frailty screening would be acceptable to key stakeholders and, if so, how that might feasibly be implemented.
Further, it is essential to take into account older adults’ views, attitudes and perceptions about the prevention and the malleability of frailty. If people do not believe that frailty is malleable, they may be reluctant to participate in screening programmes or interventions. Ensuring that screening and interventions are viewed positively will assist with uptake and a healthy ageing process.
Study aims
The purpose of this study was (a) to explore stakeholders’ experiences of frailty and the meanings of frailty to individuals; (b) to determine their understanding, beliefs and views on the malleability of frailty through screening and prevention programmes; and (c) to inform the development and evaluation of interventions that will be feasible in clinical practice.
Method
This qualitative study forms part of a larger programme of research within the European Innovation Partnership for Active and Healthy Ageing (EIP-AHA; see Bousquet et al. Reference Bousquet, Bewick, Cano, Eklund and Fico2017; and the EIP-AHA action plan, http://ec.europa.eu/research/innovation-union/pdf/active-healthy-ageing/a3_renovated_ap.pdf). That programme of work is entitled: ‘Frailty Management Optimisation Through EIP-AHA Commitments and Utilisation of Stakeholders Input’ (FOCUS), and is funded by the European Union (for further information, see http://focus-aha.eu/en/home). The FOCUS Project (Apóstolo et al. Reference Apóstolo, Cooke, Bobrowicz-Campos, Santana, Marcucci, Cano, Vollenbroek-Hutten, Germini and Holland2017; Cano et al. Reference Cano, Kurpas, Bujnowska-Fedak, Santana, Holland, Marcucci, Gonzalez-Segura, Vollenbroek-Hutten, D'Avanzo, Nobili, Apostolo, Bobrowicz-Campos and Martinez-Arroyo2016; Gwyther et al. Reference Gwyther, Cooke, Shaw, Marcucci, Cano and Holland2017) aims to consolidate evidence-based information about frailty and pre-frailty through a series of systematic reviews of the evidence, rigorous analysis of stakeholders’ perspectives, and through the development and testing of evidence-based interventions designed to prevent or reverse the effects of frailty. The study reported here, led by the Aston Research Centre for Healthy Ageing, has the discrete purpose of accessing stakeholders’ perspectives.
Participants
Five stakeholder groups were to be targeted to gather evidence from across the sector in three European countries, Italy, Poland and the United Kingdom (UK): frail and non-frail older adults, family care-givers, health-care professionals and social care professionals. Ethical approval from each participating country was received. Volunteers were given participant information sheets in plain language describing the study and what they were asked to do. Informed consent was received. Non-frail older adults (aged over 65 years) were sourced through invitations to a research centre volunteer panel, through advertisements in social centres including recreational centres, churches, schools, older adult education and learning facilities, retirement villages, and in general practitioners (GP) clinics. Frail older adults were contacted through inpatient and outpatient health and social care services and were identified by health-care professionals as frail. In the UK, participants were identified as frail, pre-frail or robust using a measure based on an accumulation of deficits model (Rockwood and Mitnitski Reference Rockwood and Mitnitski2007, Reference Rockwood and Mitnitski2011). In Italy and Poland, no formal measures were used to identify frailty status other than the physician's clinical judgement. Participant Information Sheets given to frail and non-frail groups of older adults stated: ‘we are interested in hearing from people who consider themselves frail or infirm as well as people who regard themselves as healthy and active’. This enabled older adults to self-identify as frail or not frail. Individuals with severe dementia and/or terminal illness were not included because of concerns regarding capacity to consent and fitness for participation. Health-care professionals were recruited through professional networking and were required to have an active role in either geriatric inpatient or outpatient services with at least two years’ experience. Social care providers were recruited through social care services, volunteer associations and, in the UK, in retirement villages, and were also required to have two years’ experience in the field. Finally, care-givers were contacted through patients’ associations as well as health and social care services. They were required to have responsibility for a frail older adult on a regular basis but were not required to be co-residents or have daily responsibilities. UK participants were reimbursed for their travel expenses. In Italy, transportation was provided to frail older adults. In Poland, meetings were organised near the residence of the older participants and each participant received a small gift in the form of a vitamin set or a blood pressure manometer.
Data collection
Focus groups were chosen as the most appropriate method of data collection in order to explore stakeholders’ accounts of frailty (Krueger Reference Krueger1988; Morgan and Krueger Reference Morgan and Krueger1998). Given the sensitive nature of the subject matter and the mobility restrictions of some older adults, participants were offered a choice of focus group at a research centre (university premises, medical centre) or their venue of choice (workplace, church hall). Some UK older adults requested an individual interview, expressing a desire to discuss this alone, either at home or at a research centre.
All discussions were digitally audio-recorded and transcribed verbatim in their language of origin. We were careful to ensure comprehension of the concept of frailty across languages, following previous work which identified challenges translating it into Dutch (Puts et al. Reference Puts, Toubasi, Andrew, Ashe, Ploeg, Atkinson, Ayala, Roy, Rodríguez Monforte, Bergman and McGilton2009). Researchers were careful to check participants understood the breadth of the term frailty to enable them to discuss their perceptions and experiences of it within their own lives or the lives of those close to them. The Italian and Polish researchers were not aware of any difficulties with direct translation. Sessions in the UK lasted between 11 (where the participant became distressed) and 65 minutes; in Italy between 60 and 130; in Poland between 18 and 90 minutes. A semi-structured format was used covering frailty themes compiled and defined in advance through discussions with the research team and based on the literature reviews conducted as part of the larger FOCUS project (http://focus-aha.eu/en/home). The topics were designed to guide a participant-led discussion, to reduce interviewer bias, and improve consistency and comparability between the three countries. The same set of questions was used in all three countries but slightly different questions were asked of each stakeholder group (see Table 1). In Italy, the focus groups were facilitated by a psychologist and a non-medical researcher; in Poland, by two GPs; and in the UK, by a psychologist experienced in applied health research with older adults.
Table 1. Interview schedule

Data analysis
Transcriptions were analysed using thematic analysis (Braun and Clarke Reference Braun and Clarke2006). Initial analyses were conducted in languages of origin. At this stage, notes were made on transcripts to highlight key topics and concerns raised by stakeholders. These were then enriched through a search for patterns within and across stakeholder groups to develop a set of initial themes per stakeholder group per country. Key extracts from Italy and Poland were translated into English to allow a comparison across countries. We were over-inclusive at this stage to ensure all potentially relevant data were translated and grouped into possible thematic areas. At this stage, analysts from each country met to develop the analysis and to identify recurring themes within and between stakeholder groups across all countries. At this meeting, cross-comparisons were made within the whole data-set and a coding frame was generated to allow a systematic and rigorous analysis of data from each country. Analysts then met again to refine themes and agree the final set presented here. Reliability was ensured by the use of transparent procedures within each country, and through constant exchange between the analysts involved. Analysts and those collecting data also engaged in reflexivity by explicitly thinking through their own preconceptions about frailty throughout the process to ensure data generation and analysis were participant-led, and they considered the impact of their individual relationships to participants, e.g. as a co-professional or professional to patient or family care-giver.
Results
Characteristics of the sample
Participants’ characteristics are reported in Tables 2–6. Five focus groups were held in Italy and Poland, one per stakeholder group, six in the UK (two with older adults of mixed frailty status: two with health-care professionals, one with social care professionals and one with family carers) and four individual interviews (three older adults and one family carer) were held in the UK.
Table 2. Frail older adults

Notes: 1. The number for individual interviews is given in parentheses. 2. Day hospital admissions are not included. NR: no response.
Table 3. Non-frail older adults

Notes: 1. One person was 60. 2. Day hospital admissions are not included. NR: no response.
Table 4. Family care-givers
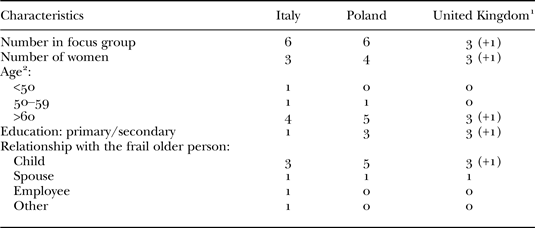
Notes: 1. The number for individual interviews is given in parentheses. 2. Age of older adult. 3. One participant cared for her mother and her mother-in-law.
Table 5. Social care professionals

Note: NR: no response.
Table 6. Health-care professionals
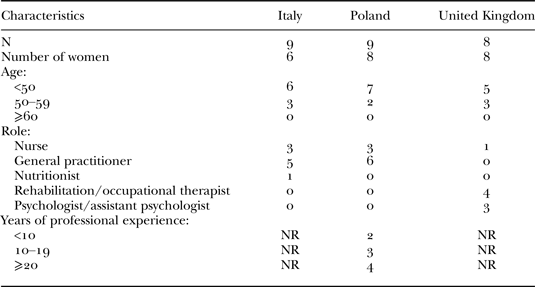
Note: NR: no response.
Four themes were identified: (a) The synchronicity between the physical and the psychological in frailty; (b) Living with frailty in the social world; (c) The need for a new kind of care; and (d) Screening for and preventing frailty. Each theme will be presented in turn with example verbatim quotations to illustrate their significance and how they meet the study aims. Quotations are attributed by country (Italy, Poland or UK), by participant group (F = frail older adults, NF = non-frail older adults; HP = health-care professionals; SP = social care professionals; FC = family carers); and finally by a unique participant number.
The synchronicity between the physical and the psychological in frailty
This theme emphasises the synchronicity between the body and mind in participants’ conceptualisations of frailty and how these work together, either synergistically to build resilience and prevent frailty or antagonistically to threaten independence and confidence through increasing isolation.
People's perceptions of frailty drew on dominant imagery of the ‘elderly’ as infirm, illustrated by this UK health-care professional:
I think frailty [is] almost like paper thin, susceptible, blow over with the wind, that sort of thing, and very susceptible to things and the environment affecting them. (UK HP19)
The initial sense is of physical weakness and vulnerability. However, it soon became clear from health professional groups across the countries that, despite a common initial focus on the physical, the psychological aspects of frailty were perhaps more powerful. One UK psychologist said:
It's actually quite an interesting concept when you think about frailty because I think in some ways our role is about building resilience which is actually moving away from the label of frailty because although we've described it in physical health terms I think there is a mental health aspect to it and I think the frailty is a shock to the family and to the person themselves. (UK HP30)
There was a realisation in this discussion of practitioner psychologists that frailty also encompassed cognitive health issues and that becoming frail was experienced as a shock by older adults and their families. Initially, the conversations with health professionals focused on physical indicators but for older adults, the cognitive or psychological aspects of frailty were prominent and more concerning. In fact, there was a deep fear attached to psychological frailty.
What scares me the most is probably the fear of not being able to use my brain anymore, have diminished mental abilities. I don't think physical abilities will be a problem looking at the future because in a short time there will be machines, devices, gym methods available. (ITA NF3)
Indeed, for this older adult in Italy, losing mental capacity was not something that could be ‘solved’ by the use of equipment or technology like physical frailty. Another Italian woman said that physical deficits could be managed effectively, as in the case of her sister who had lived with impeded mobility throughout her life. However, to achieve that her sister had been required to retain a certain level of psychological resilience and involvement in the things she loved:
Mobility and mental ability are the most important things … What I admired in my sister was the will to live in spite of her deficit, her interest for music, art. (ITA NF3)
In this instance, the management of physical frailty was possible because of psychological resilience. Within the focus group discussions with older adults across countries there was a sense that they needed to be proactive and try ‘to do everything’ (POL NF6) to maintain one's psychological and physical strength. This was clear in the recommendations older adults in Poland made about what was needed to maintain their resilience in the face of ageing:
[We need] something like a place where elderly people would meet at chess, play bridge, come and read. (POL NF8)
The activities listed above and by other older adults, e.g. managing an older adults’ lunch club (UK NF10); committee membership for the University of the Third Age (UK F11) and Women's Institute (UK NF13), volunteering at tourism venues (UK F11 and UK F9), choir membership (UK F3), involve cognitive activity, as well as social contact. These psychological factors of keeping the brain active and engaging socially appeared more important to older adults than their physical ailments – or that their physical ailments were manageable if those other needs were fulfilled. A number of older adult participants began to explore the nature of the connection between the physical and the psychological in frailty. Older adults in the UK noted the link:
But the trick is, I think the trick is, you have this medical condition, ailment, disability or whatever, if you have friends or societies that you're keenly interested in you will think, shall I? Yes I will go to that meeting. I will get out to that meeting. If you haven't got that, you will tend to stay in the house and get you know… (UK F12)
I think it's [frailty] also a mental thing. If you become physically less able to do things possibly your mental resilience drops as well and I think there may be a connection between the two, but it's increasingly losing your independence. (UK NF1)
For the latter individual, frailty was almost linear, with the suggestion that when a person becomes physically frail, psychological frailty may follow. This implies that physical frailty may be a contributory factor in psychological frailty. Indeed, losing physical mobility may reduce one's opportunities for social and psychological engagement, which may deplete mood and affect feelings of wellbeing. But for others, there was a suggestion that there was a compensatory and dynamic relationship, or synergy between the physical and the psychological, i.e. that they were bound up together and their co-existence created an enhanced combined effect. A synergistic relationship of this kind would mean that the physical and the psychological are intimately connected within the ageing process without one discretely being responsible for the other. This was evident in this UK health professional's clinical experience:
It's about attitude of mind because you can have some people who might be physically very immobile, having lots of difficulties with sensory impairment but you wouldn't describe them as frail because of their kind of attitude of mind and they can be quite feisty. (UK HP30)
This notion of psychological resilience or positive mental outlook was significant in assuaging the potential threat of defeat by the effects of physical immobility. However, it could also mean that an individual who lacks self-confidence might not seek help when it is needed. The presence of psychological resilience may therefore have a protective effect for people who need support or care due to physical immobility because it gives them the motivation to seek help which then prevents further decline.
I think [the frail] they're generally at more frailty and at more risk because they're not necessarily the ones that will ask for help either so they will just suffer on in silence until there's a crisis point and then that's when everything goes all hands to deck really. (UK HP18)
These sentiments were echoed by older adults in Italy and Poland where participants stressed the need to be pro-active in building psychological resilience:
One must manage, must succeed. If you go on saying ‘I cannot manage it’ … you have to manage it. (ITA F3)
We have to be strong and not give up. First of all, I want to be healthy. This is the basic thing. (POL NF9)
In short, this theme has described the synergy between the physical and psychological in frailty. Building psychological resilience could be a protective strategy for preventing frailty. It was clear from participants’ accounts that cognitive function and social engagement were contributing factors to psychological resilience which could also help people manage physical immobility and experience a sense of wellbeing despite their physical frailty. The next theme turns towards the social to explore how stakeholders in each country conceptualised living with frailty within the contemporary social world.
Living with frailty in the social world
Frailty exists within a social world full of relationships and opportunities which could be taken up willingly or which became inaccessible due to an individual's situation within a particular environment and health and social care system. This theme examines the concepts of coping with frailty within the contemporary context. One Italian frail older adult identified the importance of maintaining social relationships but described how it had not always been easy:
I find it very important to keep the friendships I have acquired across the years, particularly with those who are facing difficulties. I would tend to close into myself, whereas I have to react to this. It is a struggle you have to do with yourself. (ITA F11)
Identifying that one must maintain relationships is one thing but this participant identified the importance of having strategies which make that possible. Some older people in the Italian sample struggled to maintain social connections because they were unable to leave their apartment buildings without external help. This created a tipping point between frailty prevention and becoming frail; being confined at home was a material factor which contributed to decline, as reported by this GP:
I work in an area of public residential buildings most of which have no elevator. Many of my patients are borderline for frail and could remain on this side of the line if they just could use the elevator. Someone had a problem with his knee, which could be cured, but if they do not have autonomy to go out, what happens? We as GPs have the possibility to initiate domiciliary care, but eventually the outcome is that this person will be confined at home, maybe with a paid care worker who will not be able to speak Italian so communication will be impoverished more and more. (ITA HP5)
This extract describes how much an older adult's environment or confinement within that environment with little opportunity for communication can affect their health and frailty status. This situation then erodes confidence and independence and results in the need for care. In this example, it was the lack of an elevator in an apartment block which prevented access to the community but it could equally be steps up to the house or a lack of local public transport. The desire for accessible groups and amenities in the community was also expressed by Polish older adults (‘[we need] a place where elderly people would meet at chess, play bridge, come and read’; POL NF8 above). This need to get out into the social world is significant because this, like psychological resilience, could have a protective effect in preventing frailty. Without that link to the social world, it is possible that an individual would lose their confidence, detach themselves from communication with others and become isolated. This Italian health professional implies that professionals may be complicit in the debilitating effects of isolation:
What I find more shocking is isolation. I have noticed that a patient is isolated, then I have noticed that he started losing weight, no desire, or positive attitude towards the world. This isolation comes from the patient but also from the professionals somehow. (ITA HP9)
The viewpoint that frailty is caused by withdrawal from the social world following confinement at home was supported by others:
because a lot of elderly people's frailties begin with one thing and it might be just loneliness and their frailty develops because their loneliness prevents them from doing things and they're not open to the outside world so they become… sitting at the television which makes their legs not work properly and the more you withdraw, the harder it is to get up and do it. So I think a lot of it can really be pinpointed in loneliness, just loneliness really. It starts off with that, with the death of a partner, or a divorce or whatever or that you've always been a single person but because you've got perhaps one single disability you can't do the things that you did so the loneliness sets in and then you become more frail in your mind and in your body. (UK FC17)
This was also described as ‘a tipping balance, a cumulative effect over a long length of time’ (UK HP18); if one protective feature is lost, it is possible that the others will also fall away, creating a vulnerable, isolated individual who then declines. This then becomes the frail older adult who could ‘blow over in the wind’ (UK HP19). The protective features identified in the analysis so far are psychological resilience and maintaining social connections to the world. These factors help older adults manage early signs of pre-frailty in order to adapt to their needs and to postpone the progressive and debilitating effects of frailty.
However, as the Italian GP stated above, the responsibility for this should not rest solely with the older adult as an individual or with the professionals. The help required to keep loneliness at bay can be difficult to deliver and professional care services alone cannot provide the answer. For example, the Italian GP described issues with language barriers while a UK family carer described the time pressures paid care workers face and the difficulties with care continuity:
This isolation thing and [paid] carers popping in for ten minutes in the morning and ten minutes in the evening, does not work. It just does not work and they're all different. The one that comes in the morning doesn't come at night. (UK FC17)
Therefore, a co-ordinated effort involving older adults, the professionals and the local community is required to avoid isolation. In some cases, stakeholders described local volunteers and how they helped older adults cope with physical and psychological symptoms of frailty. However, as this Italian social care provider described, such services were challenged by increased need caused by deprivation:
For several years, volunteers have been trying to develop bonds with frail older people, besides helping them with commitments, but also with being present, on Saturday and Sunday when often there is nobody … this can be very challenging in deprived residential areas [because] there is a serious problem of poverty. (ITA SP7)
We know that ill-health is related to poverty and so it is significant here. It was also mentioned in Poland – that there was a feeling of lack in the system and there was a need for support that was free. Furthermore, one health-care professional suggested that some individuals ‘do not know that frailty exists’ (POL HP6) which shifts the onus on to the health and social care system to provide support which otherwise older adults would not know was there.
Older people have no idea that this [frailty] is a disease, [it's] often described as old age. [They] are isolated from their closest environment, become less needed, get into such discouragement, do not engage, they feel rejected, they feel useless and this causes health problems. (POL HP1)
This extract summarises the key points highlighted in this theme: that isolation and loneliness are a condition, as well as a determinant of frailty, and that frailty can become worse if older adults lose their connections to the social world; the loss of those relationships can threaten an individual's sense of self-worth, and as a result they withdraw, become more vulnerable and begin to decline. Alternatively, if older adults live in an environment which facilitates those connections and provides opportunities for social engagement, some of those features of frailty can be delayed. What is required to do that though, is a supportive community and co-ordinated health and social care services. The next theme explores the notion of care in more depth.
The need for a new kind of care
Here we investigated the phenomenon of care. Relationships between those in receipt of care and those providing it were identified as significant, suggesting a need for a kind of care which can be delivered in a person-centred way. This is particularly important when, as we saw above, there could be a reticence to seeking care among those who may end up becoming the most vulnerable.
It's a kind of dignity and privacy and autonomy thing … I wasn't very comfortable in hospital having my knee replaced. I didn't like it very much … I didn't like being in other people's hands. I don't like that dependency. (UK NF1)
There are several issues here: there was a threat to privacy because of lost autonomy to take control of one's body, which led to a sense of lost dignity; there was also a dislike of becoming a passive patient, dependent on others to survive. This suggests that a complex process of adaptation is necessary for an individual to work through the physical and psychological issues that have come together at this point – the ‘cumulative effect’ and ‘tipping balance’ (UK HP18) – to acknowledge the need for an external intervention of some kind.
The health and social care professionals in this sample were mindful of the need to be sensitive and to develop rapport with older adults when delivering personal care. There were examples of covering up exposed body parts with a towel or requesting that family members leave the room during personal care to maintain the older adults’ privacy. One of the simplest things they said was that getting to know their clients and talking to them would help retain a sense of dignity.
It's invasive … giving personal care and stuff. You need to create like a bond in a way, like you're going back to the talking and everything. That in itself creates a bond, you know with the person for them to feel comfortable enough for you to help them and then again, dignity comes into it. (UK SP5)
This significance of developing a relationship was also expressed in Italy where it was taken further towards developing a concept of care that was more than task-oriented activity and which became a practice of care that was holistic and valued the older adult's personhood.
Frailty starts when a person thinks that nobody can help her, but if I, as a nurse, when a patient arrives, say ‘my name is Isabella’, I communicate with her, I try to be close. This can seem trivial but it is essential. Nurses should do this, because patients don't ask but we should give anyway. To be hospitalised is to be abandoned … I speak with them a lot, I ask about their life [and help them see that hospital] is a place they are helped and cared for … We can give just a little, but this little bit can make a person great. (ITA HP8)
These extracts demonstrate ways in which health and social care professionals can alter the nature of their work by personalising their care and by relating with older adults in an individualised way. Furthermore, the Italian nurse above argued that simply speaking with older adults as another human being, an equal, could counteract the disempowering effects of frailty and the feeling of abandonment experienced by older adults in hospital. However, this does not solely rest with care professionals. Usually when an older adult is in receipt of care, family members have already taken on care-giver duties prior to or to supplement services provided by professionals. So there becomes a need to provide family-centred care rather than just person-centred care. In Poland, family care-givers described feeling abandoned by professional services because of the psychological burden they experienced:
This is a very big burden for me. And besides, I still have a family, children, responsibilities. And the lack of time. At the moment I am looking for help myself. I can honestly say that yesterday I went to a psychologist for a conversation, simply because I no longer have the strength. (POL FC2)
This extract reveals a need for support at the family level. It also highlights the stress of caring for older relatives in addition to existing commitments, including children and work. This is something which could be aided by transparent health and social care systems which clearly indicate eligibility for support and which offer support for family care-givers as well as older adults. Unfortunately, access to care, although different in participating countries, was similarly challenging. Across the sample there were instances of misunderstandings of overly complex systems which prevented stakeholders from accessing or indeed delivering the services they felt were needed. In Italy, one family care-giver observed that he had never received any communication about possible help for the very old frail people he cared for and wondered whether any authority knew about his care commitments:
I asked myself, ‘do social services know that I am taking care of two 90-year-old people?’ I've never received a letter explaining what they can do to help. I looked on the internet but there is so much, public and private, and so I have to decide by myself and do it by myself, and in the end I take the private ambulance and I pay others for it. (ITA FC6)
This extract indicates the need for self-advocacy; to access help and support one has to be pro-active in seeking it out rather than the state reaching out to individuals. The complexity experienced in Italy was echoed in Poland to the extent that one older adult suggested the need for a co-ordinating care manager, essentially an advocate, who could liaise with multiple departments and families to ensure the older adult received everything for which they were eligible:
It should be a person who will visit a patient and ask about wellbeing, then contact the doctor, or some sort of social worker. There is lack of communication right now … This is the biggest role … a doctor who knows all the elderly people in need of help, for example, always has time, and the same nurse. (POL NF5)
The need for a co-ordinator for adult health-care services was also raised in the UK. Although in this instance, the suggestion was for a health visitor-style role, as a monitor and source of information:
I think that we've got to deal with old age in the same way that we deal with childhood … the way that childhood is seen as an all-encompassing, up to the age of five we've got all sorts of things that can be accessed by adults on behalf of their children but we haven't got anything that can be accessed by children on behalf of their parents … and we've got people who monitor children's welfare, we've got people who monitor children's health, teeth and everything else but we don't have the same structure for the elderly. (UK FC17)
Health and social care professionals and family carers agreed with this need for more integrated care services. Indeed, in Poland, health-care professionals called for ‘a new model of social care [that does] not just focus on symptoms, [but is] complex’ (POL HP8). However, in the UK at least, where there have been significant cuts in social care provision, this was described as ‘pie in the sky’ (UK FC16) because of the unlikelihood of obtaining more professionals to provide the kind of care required: care that is consistent, one-to-one, focused on matters of ageing and available at the point of need. Delays in access to care and support were reported in all participating countries, which is reflective of the opaque information about care and support that is available, but also of the economic situation across Europe which has resulted in austerity measures.
Nevertheless, changing family carers’ outlook on care provision towards a holistic, family-centred approach could be conceived as a relatively cheap intervention and therefore realistic objective in the pursuit of preventing frailty and making cost savings otherwise caused by worsening complications of co-morbid conditions and increased hospitalisations. The final theme examines the potential screening services and the possibility of frailty prevention.
Screening for and preventing frailty
A central aim of this study was to determine whether key stakeholders believed that frailty is preventable. This final theme examines the nature of screening and its utility in the prevention of frailty.
When asked if frailty was preventable, there was a sense among participants that it may be possible to delay the symptoms of frailty and maintain wellbeing for some length of time but that it was not possible to prevent the inevitable, ‘to stave off the evil day?!’ (UK F3), i.e. that older adults will become frail if they continue to live.
I don't think you can prevent it but you can aid them to be the best they can be. That's what I think. You can't prevent what is going to happen. (UK SP5)
There was also a question about whether prevention was ‘useful at 83?’ (ITA F9). However, within the previous quotation is a message that has shone out throughout this analysis, which is about ‘be[ing] the best they can be’ (UK SP5) and having ‘the will to live in spite of … deficit’ (ITA NF3). Yes, older adult life does involve increasing incapacities but those do not always have to mean a lower quality of life or loss of wellbeing. One Polish older adult's statement made this sentiment concrete: ‘I am getting depressive and my dog rescues me from depression’ (POL NF8). Another echoed that feeling and went on to discuss how screening could help older adults to maintain a positive outlook by showing them how to keep going with activities they enjoyed in a safe way that would not threaten their health.
I do exercises, or bike exercises at home, or walking more, then immediately my frame of mind is improved. It [screening] should be at least once a year, a few months, half a year, under the supervision of an expert. [And] at least a few days … where physiotherapists show how and what [older adults can do], explain, and then the patients themselves, if they want, they do this. (POL F3)
There was a concern in Poland that any physical activity should have endorsement from a health or social care professional; older adults wanted the reassurance that what they were doing was safe. Safety of keeping active was a concern expressed elsewhere and was something that made one UK health-care professional raise doubts about interventions to promote physical activity or resilience-building exercises in the home.
If they're very gentle exercises then it's probably okay but I think there's always risks if people are frail, particularly if we are talking about people who are at risk of falls and other injuries. (UK HP30)
Again, this emphasised the need for older adults to engage in exercises that are appropriate for their fitness level and, as stressed in Poland, to receive professional advice about this. But there was also doubt about whether individuals would take up exercises alone at home, which then revealed another benefit to incorporating a social element to services for older adults:
It's much better to get someone to go out, meet people, do an exercise, they would be more motivated … If you're doing a thing with a video … there's no guarantee that anyone's doing it. If you're going to a centre, then at least you can see if someone's adhering to the programme. (UK HP29)
There was a general consensus that screening for frailty – or raising awareness of measures to prevent frailty – would be beneficial. To be useful, screening had to be paired with access to services for older adults:
If you just have the person more aware that he is frail but have nothing to offer [it is no use]. (ITA HP5)
Screening works better if the pathway is clear. (ITA SP8)
It shouldn't be just tick boxes, it should be ‘have you considered such or what about…?’, it shouldn't be ‘must’, it's got to be an advisory and in consultation. And it does depend upon, it's what the environment is, where the practice is, what people will consider to be a norm. (UK F12)
It would be very expensive. Access to health care would be improved. (POL NF2)
The last two extracts present the challenges accompanied by introducing frailty screening: the form screening should take and its message to older adults would be significant in terms of its utility in the prevention of frailty; and it would be expensive for health and social care systems to implement the kind of screening required, i.e. screening that is consultative, sensitive and which leads to personalised care. Furthermore, frailty prevention services would need to be supported by local communities and would be dependent on fostering a changed attitude towards frailty; to engage in preventative strategies, older adults, their families and their professional care providers need to believe it is possible to reverse the effects of frailty and maintain a good quality of life.
Discussion
This study aimed to gather stakeholders’ perspectives about, and experiences of, frailty with a view to exploring the potential malleability of frailty in order to inform the development and evaluation of screening and prevention programmes in clinical practice. The data gathered have enabled us to consider what are the significant factors in frailty that might have protective effects, and thus which might be central to preventative programmes. Following previously expressed concerns about the potential negative impact of being labelled as ‘frail’ (e.g. Grenier Reference Grenier2005, Reference Grenier2006; Warmoth et al. Reference Warmoth, Lang, Phoenix, Abraham, Andrew, Hubbard and Tarrant2016), we identified a key concern across countries and stakeholder groups that screening for frailty must have an outcome or specific purpose and not stop at categorisation. Screening cannot therefore be implemented in isolation but must be accompanied by a transparent pathway to care, intervention and support services for older adults and their family care-givers; we also found that underpinning all of this is the significance of human relationships and connections to the social world, whether that is through personalised care or through facilitating the maintenance of existing friendships and hobbies that become difficult as incapacities develop. There was a clear awareness of the relationship between physical and psychological frailty and resilience in achievement of balance and maintenance of agency and identity, expressed by all groups. Having said that, the significance of the psychological was more prominent in accounts from older adults and social care professionals. Health professionals turned first to the physical and only began to contemplate the impact of the psychological during the discussions.
These findings corroborate recent evidence identifying the importance of psychological factors in frailty prevention and reversal such as quality of life, maintaining social contacts, situational factors and wellbeing. Converging evidence from epidemiological studies support this understanding of the link and a sense of trajectory from physical to cognitive frailty, with Boyle et al. (Reference Boyle, Buchman, Wilson, Leurgans and Bennett2010) demonstrating a 63 per cent increase in the risk of developing Mild Cognitive Impairment for every one point increase in physical frailty, even controlling for other contributing factors such as depression. In contrast, evidence also demonstrates the protective effects of social networks on the manifestation of cognitive difficulties, even in the context of significant neuropathology (Bennett et al. Reference Bennett, Schneider, Tang, Arnold and Wilson2006). Our participants’ understanding of the cumulative effect of deficits reflects what turns out to be a very useful way to define and assess frailty, for example, work by Rockwood et al. (Reference Rockwood, Mitnitski, Song, Steen and Skoog2006) which identified the cumulative effect of the impacts of different issues which may mount to produce increasing risk of a negative outcome – ‘the tipping balance’. This suggests that early intervention could prevent older adults from entering a cycle of decline and help to maintain those connections to the social world. All stakeholder groups emphasised the psychological and social elements of frailty which suggests interventions incorporating the opportunity for social interaction and cognitive stimulation as well as safe and appropriate physical activity would have a much greater possibility of success. This supports a recent scoping review of interventions to prevent or treat frailty which highlighted the effectiveness of safe physical activity interventions, either on their own or in combination with nutrition, cognitive training, geriatric assessment and management, and ‘prehabilitation’ (strength training) (Puts et al. Reference Puts, Toubasi, Andrew, Ashe, Ploeg, Atkinson, Ayala, Roy, Rodríguez Monforte, Bergman and McGilton2017). Of course, this would require an integrated set of services for older adults and their family care-givers.
The concept of resilience was raised across stakeholder groups when thinking through possibilities for the prevention or reversal of frailty. Indeed, our findings provide examples for some of the conceptualisations of resilience in a recent piece by Wild, Wiles and Allen (Reference Wild, Wiles and Allen2013) in which the utility of resilience for critical gerontology is discussed. Several interpretations are offered which essentially call for a holistic approach to understanding resilience in older adulthood. They described the usefulness of the term ‘plasticity’ (Staudinger, Marsiske and Baltes Reference Staudinger, Marsiske and Baltes1993) – comparable to malleability – to reflect the flexibility and changeability of an older adult's life context over time and circumstance in relation to their ability to adapt and grow because of – rather than in spite of – adverse life events and their experiences of vulnerability. Furthermore, like us, Wild, Wiles and Allen (Reference Wild, Wiles and Allen2013) argued for research focusing on the notions of community and societal resilience alongside individual and family resilience.
In short, our findings recommend a holistic approach to care and services for older adults which incorporate ingredients that will be effective in stimulating cognitive activity, maintaining social relationships and engaging in a personalised exercise plan. They also recommend the need for an advocacy service to help older adults and their family care-givers to access services for which they are eligible; a care co-ordinator model was suggested which would link up interdisciplinary health and social care professionals to support uptake of appropriate services, enabling prevention before crisis points. Finally, for the screening and prevention of frailty to be possible, a shift in attitudes among social care professionals, frail and non-frail older adults may be necessary; there was doubt about the malleability of frailty which suggests the need to raise awareness that experiencing symptoms of frailty does not necessarily represent a point of no return, but early intervention is necessary to prevent those symptoms from worsening. In other words, awareness of the malleability of frailty needs to be raised among younger adults and across society more generally for that cultural shift in conceptualisations of frailty to be achieved, and attitudes towards prevention changed.
Limitations
Older adults were recruited through a combination of clinical judgement and self-identification in the absence of widespread usage of a standardised measure of frailty across participating countries. Self-perceptions of frailty do not always equate to clinical judgements, although self-ratings of health are shown to be reasonably accurate as predictors (e.g. Idler and Benyamini Reference Idler and Benyamini1997; Jylha Reference Jylha2009). Validated measures of frailty exist although they vary in their accuracy and are not universally used. The FOCUS team's overview of reviews of methods for assessing frailty (an umbrella review, Apóstolo et al. Reference Apóstolo, Cooke, Bobrowicz-Campos, Santana, Marcucci, Cano, Vollenbroek-Hutten, Germini and Holland2017) concludes that several measures could be used to good effect, with the most flexible to context being an accumulation of deficits model, or frailty index (Rockwood and Mitnitski Reference Rockwood and Mitnitski2007).
There were some differences in professional groups accessed in the participating countries, largely due to differences in the set-up of health and social care services in the different countries. Nevertheless, it was still possible to compare across countries, although a surprising level of similarity was seen in the issues raised in stakeholders’ accounts from the different contexts. There were some small differences between stakeholder groups; health professionals focused first on the physical aspects of frailty while it was psychological resilience which was prioritised by older adults; and conceptualising frailty as malleable may be more of a challenge among social care professionals, older adults and family carers. Nevertheless, on discussing the issues, stakeholders began to demonstrate agreement on what were the significant issues: maintaining social integration, making healthy lifestyle choices and the need for screening to be linked explicitly to a care pathway were consistent across stakeholders. This strengthens the data interrogated because the findings present a coherent message that is clearly attributable across the participating countries. What is needed now is further work with other European countries to determine whether differences could be found that would require a different approach.
Conclusions
Frailty is a complex phenomenon with multifaceted component parts. For it to be tackled in an effective way, health and social care services need to be integrated and need to offer prevention programmes that will help older adults stay connected to the social world so that they can continue to experience wellbeing despite physical incapacities and maintain a sense of self. Frailty screening could be implemented as a triage process, facilitating referral into appropriate care and treatment services for people with specific, identified health needs, ensuring that therapeutic measures are applied in a timely manner while preventing pre-frail individuals from deteriorating into a frail condition. From policy makers’ and health organisation planning perspectives, screening could also inform intervention policy and provide information on high-risk populations. Nevertheless, work to enable understanding of the malleability of frailty and the possibilities for prevention need to be accomplished for such endeavours to be successful more widely.
Acknowledgements
The team would like to thank Tomasz Kujawa in the Family Medicine Department, Wroclaw Medical University for undertaking recording and transcription services for the Polish focus groups. This work was supported by the Consumers, Health, Agriculture and Food Executive Agency (CHAFEA) of the European Commission, under the European Union Health Programme (2014–2020). The survey forms part of a larger study, ‘Frailty Management Optimisation Through EIP-AHA Commitments and Utilisation of Stakeholders Input’ (Grant Number 664367 FOCUS). Ethical approval was granted in each host institution to access the stakeholder groups (UK: Aston University, #844; Italy: EC of the Fondazione IRCCS Ca’ Granda Ospedale Maggiore Policlinico, 636_2015bis; Poland: Wroclaw Medical University, 502/2015). RLS and BDA led the study. All authors contributed to the conceptualisation of the study and its design. Analysis and interpretation of the data were led by RLS, BDA, HG, MB, DK and CH. All authors have contributed to the drafting or critical revision of the paper for important intellectual content. All authors have approved this version to be published. There is no conflict of interest to declare.








