Background:
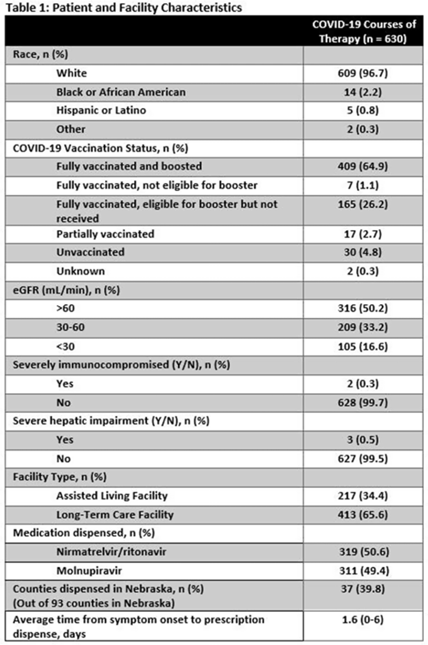
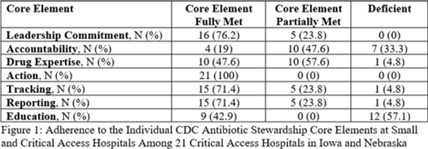
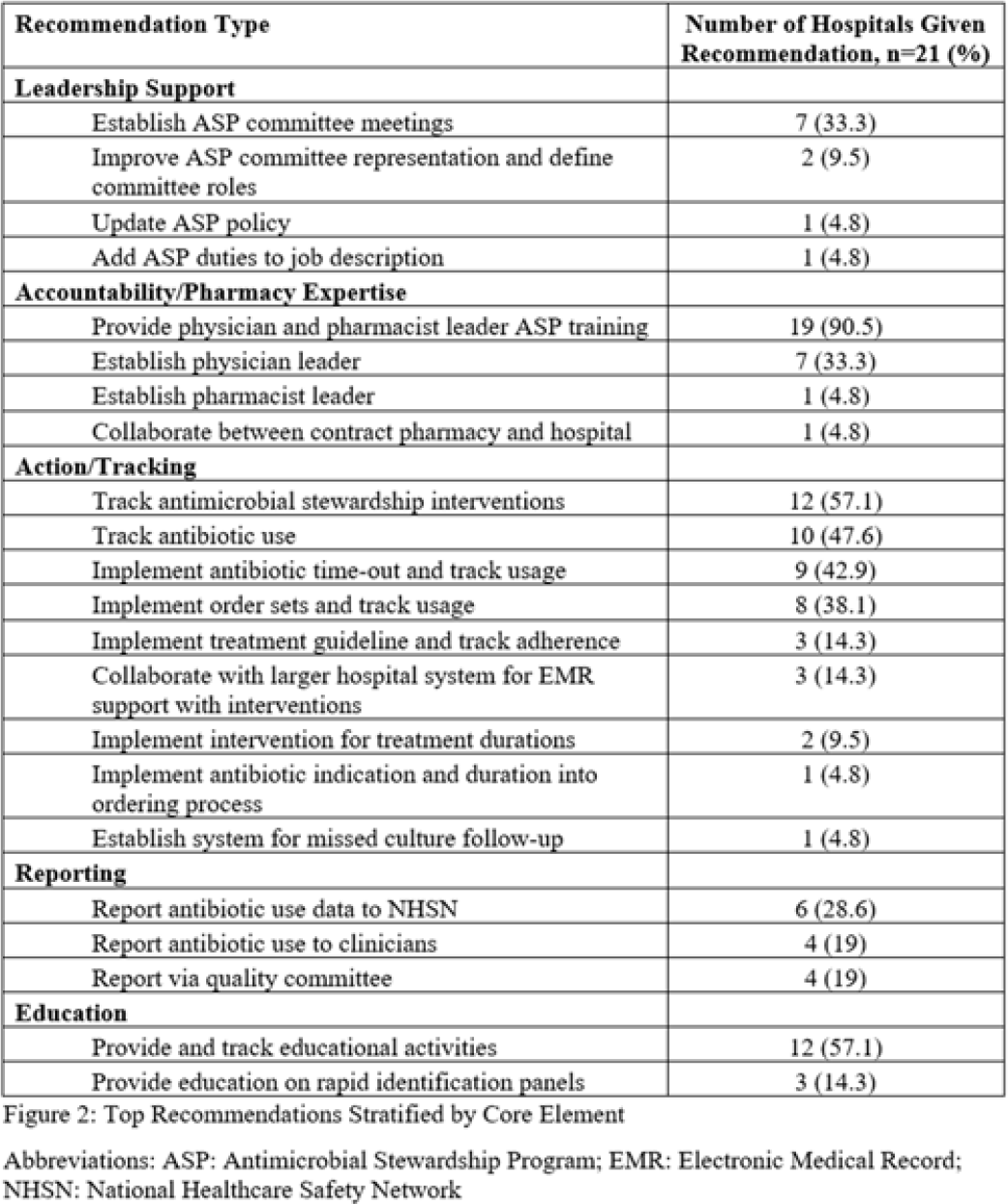
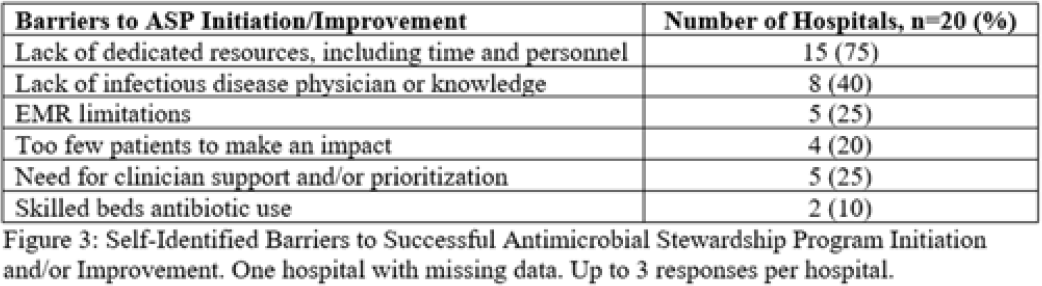
The CDC recommends that consultant pharmacists support antimicrobial stewardship programs (ASPs) in long-term care facilities (LTCFs). We studied CDC-recommended ASP core elements implementation and antibiotic use in LTCFs before and after training consultant pharmacists. Methods: Between August 2017 and October 2017, consultant pharmacists from a regional long-term care pharmacy attended 5 didactic sessions preparing them to assist LTCFs in implementation of CDC-recommended ASP core elements. Training also included creating a process for evaluating appropriateness of all systemic antibiotics and providing prescriber feedback during their monthly mandatory drug-regimen reviews. Once monthly “meet-the-expert” sessions were held with consultant pharmacists throughout the project (November 2017 to December 2018). LTCF enrollment began in November 2017 and >90% of facilities joined by January 2018. After enrollment, consultant pharmacists initiated ASP interventions including antibiotic reviews and feedback using standard templates. They also held regular meetings with infection preventionists to discuss Core Elements implementation and provided various ASP resources to LTCFs (eg, antibiotic policy template, guidance documents and standard assessment and communication tools). Data collection included ASP Core Elements, antibiotic starts, days of therapy (DOT), and resident days (RD). The McNemar test, the Wilcoxon signed-rank test, generalized estimating equation model, and the classic repeated measures approach were used to compare the presence of all 7 core elements and antibiotic use during the baseline (2017) and intervention (2018) year.Results: In total, 9 trained consultant pharmacists assisted 32 LTCFs with ASP implementation. When evaluating 27 LTCFs that provided complete data, a significant increase in presence of all 7 Core Elements after the intervention was noted compared to baseline (67% vs 0; median Core Elements, 7 vs 2; range, 6–7 vs 1–6; P < .001). Median monthly antibiotic starts per 1,000 RD and DOT per 1,000 RD decreased in 2018 compared to 2017: 8.93 versus 9.91 (P < .01) and 106.47 versus 141.59 (P < .001), respectively. However, variations in antibiotic use were detected among facilities (Table 1). When comparing trends, antibiotic starts and DOT were already trending downward during 2017 (Fig. 1A and 1B). On average, antibiotic starts decreased by 0.27 per 1,000 RD (P < .001) and DOT by 1.92 per 1,000 RD (P < .001) each month during 2017. Although antibiotic starts remained mostly stable in 2018, DOT continued to decline further (average monthly decline, 2.60 per 1,000 RD; P < .001). When analyzing aggregated mean, antibiotic use across all sites per month by year, DOT were consistently lower throughout 2018 and antibiotic starts were lower for the first 9 months (Fig. 1C and 1D). Conclusions: Consultant pharmacists can play an important role in strengthening ASPs and in decreasing antibiotic use in LTCFs. Educational programs should be developed nationally to train long-term care consultant pharmacists in ASP implementation.
Funding: Merck & Co., Inc, provided funding for this study.
Disclosures: Muhammad Salman Ashraf and Scott Bergman report receipt of a research grant from Merck.