1424 results
VaTEST III: Validation of 8 Potential Super-Earths from TESS Data
-
- Journal:
- Publications of the Astronomical Society of Australia / Accepted manuscript
- Published online by Cambridge University Press:
- 11 April 2024, pp. 1-22
-
- Article
- Export citation
Rise and diversification of chondrichthyans in the Paleozoic
-
- Journal:
- Paleobiology , First View
- Published online by Cambridge University Press:
- 14 March 2024, pp. 1-14
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Predictors of primary care psychological therapy outcomes for depression and anxiety in people living with dementia: evidence from national healthcare records in England
-
- Journal:
- The British Journal of Psychiatry , FirstView
- Published online by Cambridge University Press:
- 08 February 2024, pp. 1-8
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Variation of subclinical psychosis across 16 sites in Europe and Brazil: findings from the multi-national EU-GEI study
-
- Journal:
- Psychological Medicine , First View
- Published online by Cambridge University Press:
- 30 January 2024, pp. 1-14
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Early technology review: towards an expedited pathway
-
- Journal:
- International Journal of Technology Assessment in Health Care / Volume 40 / Issue 1 / 2024
- Published online by Cambridge University Press:
- 29 January 2024, e13
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Castor Toxin Adsorption to Clay Minerals
-
- Journal:
- Clays and Clay Minerals / Volume 53 / Issue 3 / June 2005
- Published online by Cambridge University Press:
- 01 January 2024, pp. 268-277
-
- Article
- Export citation
4 The Role of Cognition and Self-Awareness on Driving Patterns After Moderate-to-Severe Traumatic Brain Injury
-
- Journal:
- Journal of the International Neuropsychological Society / Volume 29 / Issue s1 / November 2023
- Published online by Cambridge University Press:
- 21 December 2023, pp. 116-117
-
- Article
-
- You have access
- Export citation
3 Mobile Toolbox: Enrollment of a Large Normative Sample Using the UCSF Brain Health Registry
-
- Journal:
- Journal of the International Neuropsychological Society / Volume 29 / Issue s1 / November 2023
- Published online by Cambridge University Press:
- 21 December 2023, pp. 781-782
-
- Article
-
- You have access
- Export citation
98 Cognitive Outcomes Following Bilateral Focused Ultrasound Thalamotomy for Tremor
-
- Journal:
- Journal of the International Neuropsychological Society / Volume 29 / Issue s1 / November 2023
- Published online by Cambridge University Press:
- 21 December 2023, pp. 197-198
-
- Article
-
- You have access
- Export citation
Distortions in focusing laser pulses due to spatio-temporal couplings–An analytic description
-
- Journal:
- High Power Laser Science and Engineering / Accepted manuscript
- Published online by Cambridge University Press:
- 18 December 2023, pp. 1-34
-
- Article
-
- You have access
- Open access
- Export citation
Changing human-cattle relationships in Ireland: a 6000-year isotopic perspective
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Anoplocephalid tapeworms in mountain gorillas (Gorilla beringei beringei) inhabiting the Volcanoes National Park, Rwanda
-
- Journal:
- Parasitology / Volume 151 / Issue 2 / February 2024
- Published online by Cambridge University Press:
- 29 November 2023, pp. 135-150
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
How old is the Ordovician–Silurian boundary at Dob’s Linn, Scotland? Integrating LA-ICP-MS and CA-ID-TIMS U-Pb zircon dates
-
- Journal:
- Geological Magazine / Volume 160 / Issue 9 / September 2023
- Published online by Cambridge University Press:
- 22 November 2023, pp. 1775-1789
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
They’re Still There, He’s All Gone: American Fatalities in Foreign Wars and Right-Wing Radicalization at Home
-
- Journal:
- American Political Science Review , First View
- Published online by Cambridge University Press:
- 19 October 2023, pp. 1-7
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
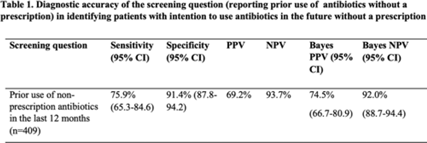
Identifying nonprescription antibiotic users with screening questions in a primary care setting
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 3 / Issue S2 / June 2023
- Published online by Cambridge University Press:
- 29 September 2023, pp. s20-s21
-
- Article
-
- You have access
- Open access
- Export citation
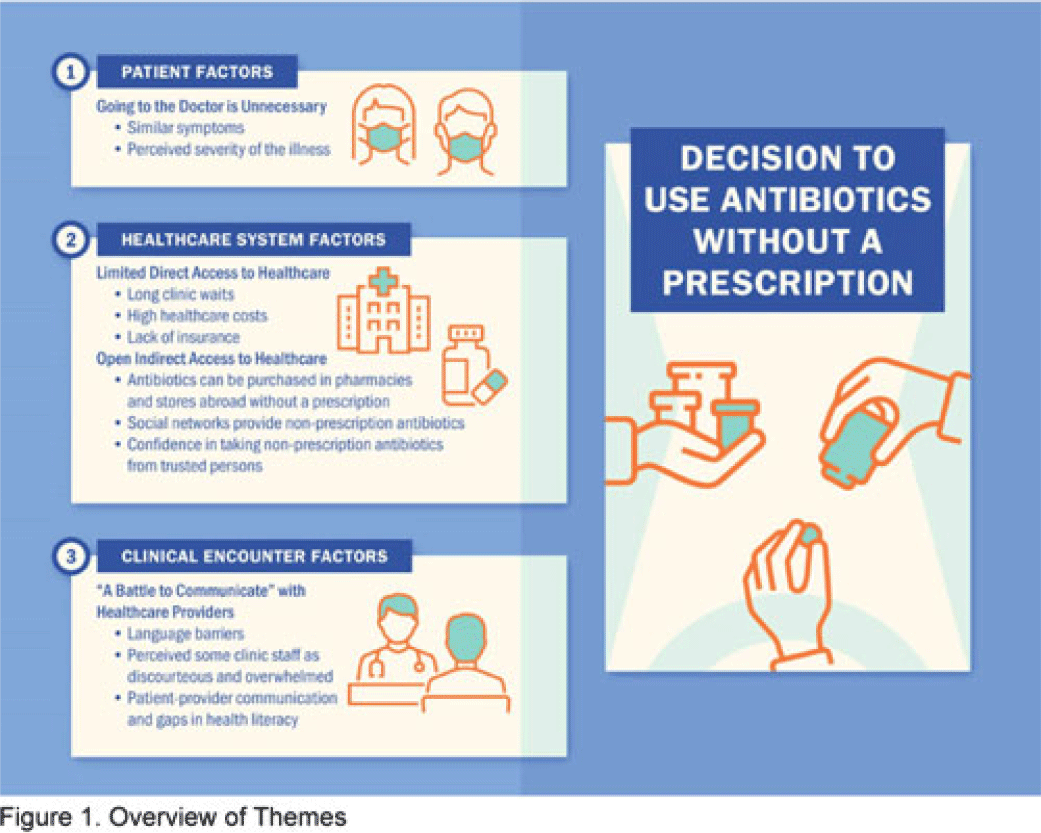
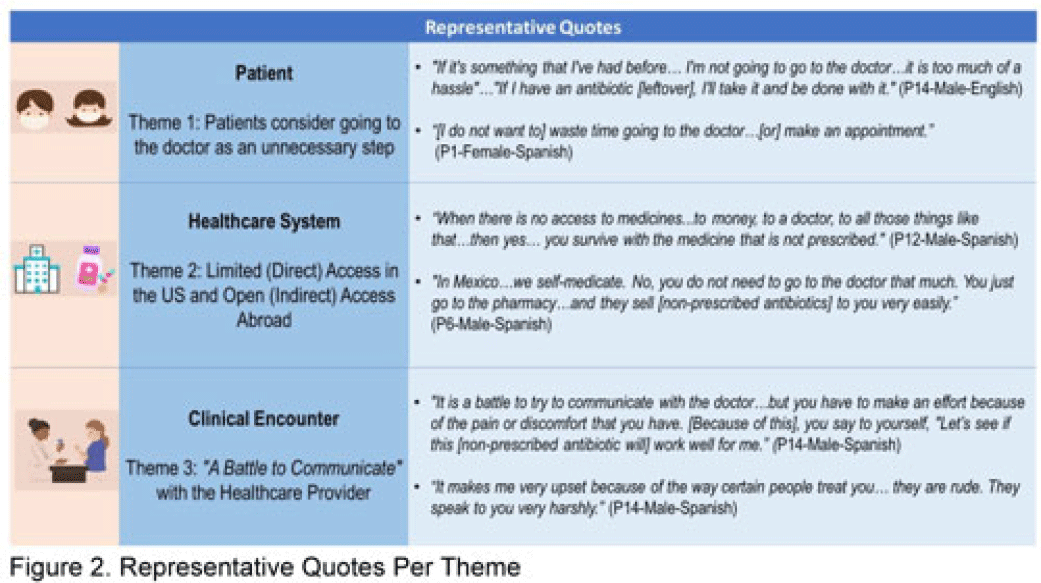
Perspectives on nonprescription antibiotic use among Hispanic patients in the Houston metroplex: A qualitative study
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 3 / Issue S2 / June 2023
- Published online by Cambridge University Press:
- 29 September 2023, p. s20
-
- Article
-
- You have access
- Open access
- Export citation
National validation of the Centers for Medicare & Medicaid Services strategy for identifying potential surgical-site infections following colon surgery and abdominal hysterectomy
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 45 / Issue 2 / February 2024
- Published online by Cambridge University Press:
- 07 September 2023, pp. 167-173
- Print publication:
- February 2024
-
- Article
- Export citation
A multi-country comparison of jurisdictions with and without mandatory nutrition labelling policies in restaurants: analysis of behaviours associated with menu labelling in the 2019 International Food Policy Study
-
- Journal:
- Public Health Nutrition / Volume 26 / Issue 11 / November 2023
- Published online by Cambridge University Press:
- 04 September 2023, pp. 2595-2606
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Barriers and facilitators to recruitment of underrepresented research participants: Perspectives of clinical research coordinators
-
- Journal:
- Journal of Clinical and Translational Science / Volume 7 / Issue 1 / 2023
- Published online by Cambridge University Press:
- 18 August 2023, e193
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Pathways to care for psychosis in Malawi
-
- Journal:
- BJPsych International / Volume 20 / Issue 4 / November 2023
- Published online by Cambridge University Press:
- 31 July 2023, pp. 84-89
- Print publication:
- November 2023
-
- Article
-
- You have access
- Open access
- HTML
- Export citation



 R
R R
R R
R R
R R
R R
R R
R R
R