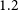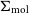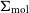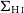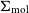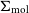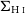463 results
280 Enhancing Nephrology Care Access: Development and Implementation of a Telenephrology Dashboard Through Human-Centered Design
- Part of
-
- Journal:
- Journal of Clinical and Translational Science / Volume 8 / Issue s1 / April 2024
- Published online by Cambridge University Press:
- 03 April 2024, p. 85
-
- Article
-
- You have access
- Open access
- Export citation
Separating the rash from the chaff: novel clinical decision support deployed during the mpox outbreak
-
- Journal:
- Infection Control & Hospital Epidemiology , First View
- Published online by Cambridge University Press:
- 02 April 2024, pp. 1-3
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Cost-effectiveness of severe acute respiratory coronavirus virus 2 (SARS-CoV-2) testing and isolation strategies in nursing homes
-
- Journal:
- Infection Control & Hospital Epidemiology , First View
- Published online by Cambridge University Press:
- 15 February 2024, pp. 1-8
-
- Article
- Export citation
Incidence and transmission associated with respiratory viruses in an acute care facility: An observational study
-
- Journal:
- Infection Control & Hospital Epidemiology , First View
- Published online by Cambridge University Press:
- 14 February 2024, pp. 1-3
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
FC18: Can rehabilitation improve functional independence of older people with dementia? A pragmatic randomized controlled trial (RCT) of the Interdisciplinary Home-bAsed Reablement Program (I-HARP)
-
- Journal:
- International Psychogeriatrics / Volume 35 / Issue S1 / December 2023
- Published online by Cambridge University Press:
- 02 February 2024, pp. 80-81
-
- Article
-
- You have access
- Export citation
GNOMES II: Analysis of the Galactic diffuse molecular ISM in all four ground state hydroxyl transitions using Amoeba – CORRIGENDUM
-
- Journal:
- Publications of the Astronomical Society of Australia / Volume 41 / 2024
- Published online by Cambridge University Press:
- 15 January 2024, e006
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
60 The Impact of Retirement Status on Cognitive Dysfunction in Alzheimer’s Disease
-
- Journal:
- Journal of the International Neuropsychological Society / Volume 29 / Issue s1 / November 2023
- Published online by Cambridge University Press:
- 21 December 2023, pp. 366-367
-
- Article
-
- You have access
- Export citation
32 Prediction of Seizure Outcome with Presurgical IAT, MRI, and PET in Patients with Temporal Lobe Epilepsy Undergoing Surgery
-
- Journal:
- Journal of the International Neuropsychological Society / Volume 29 / Issue s1 / November 2023
- Published online by Cambridge University Press:
- 21 December 2023, pp. 31-32
-
- Article
-
- You have access
- Export citation
63 Comparison of Measures for Identification of Social Difficulties in Early Childhood for Children with Neurofibromatosis Type 1
-
- Journal:
- Journal of the International Neuropsychological Society / Volume 29 / Issue s1 / November 2023
- Published online by Cambridge University Press:
- 21 December 2023, pp. 739-740
-
- Article
-
- You have access
- Export citation
Advocacy at the Eighth World Congress of Pediatric Cardiology and Cardiac Surgery
-
- Journal:
- Cardiology in the Young / Volume 33 / Issue 8 / August 2023
- Published online by Cambridge University Press:
- 24 August 2023, pp. 1277-1287
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Excessive fear of clusters of holes, its interaction with stressful life events and the association with anxiety and depressive symptoms: large epidemiological study of young people in Hong Kong
-
- Journal:
- BJPsych Open / Volume 9 / Issue 5 / September 2023
- Published online by Cambridge University Press:
- 14 August 2023, e151
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Antibiotic Selection and Duration for Catheter-Associated Urinary Tract Infection in Non-Hospitalized Older Adults: A Population-Based Cohort Study
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 3 / Issue 1 / 2023
- Published online by Cambridge University Press:
- 01 August 2023, e132
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Cognitive flexibility moderates the relationship between exposure to COVID stressors and obsessive-compulsive (OCS) symptoms
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S230
-
- Article
-
- You have access
- Open access
- Export citation
Assessing the effectiveness and observing fidelity of a psychosocial support program for Rohingya refugee mothers and their children in Cox’s Bazar, Bangladesh
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S356-S357
-
- Article
-
- You have access
- Open access
- Export citation
Systematic Review on the Mechanisms of Action of Psilocybin in the Treatment of Depression
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S416-S417
-
- Article
-
- You have access
- Open access
- Export citation
Implementing strategies to prevent infections in acute-care settings
- Part of
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 44 / Issue 8 / August 2023
- Published online by Cambridge University Press:
- 11 July 2023, pp. 1232-1246
- Print publication:
- August 2023
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
WALLABY pilot survey: The diversity of HI structural parameters in nearby galaxies
-
- Journal:
- Publications of the Astronomical Society of Australia / Volume 40 / 2023
- Published online by Cambridge University Press:
- 08 June 2023, e032
-
- Article
- Export citation
P.005 A virtual interdisciplinary diagnostic memory clinic: rural patient and caregiver satisfaction
-
- Journal:
- Canadian Journal of Neurological Sciences / Volume 50 / Issue s2 / June 2023
- Published online by Cambridge University Press:
- 05 June 2023, p. S58
-
- Article
-
- You have access
- Export citation
VERTICO V: The environmentally driven evolution of the inner cold gas discs of Virgo cluster galaxies
-
- Journal:
- Publications of the Astronomical Society of Australia / Volume 40 / 2023
- Published online by Cambridge University Press:
- 27 April 2023, e017
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
39 Prenatal antibiotic exposure and risk of childhood asthma among children with Down syndrome
- Part of
-
- Journal:
- Journal of Clinical and Translational Science / Volume 7 / Issue s1 / April 2023
- Published online by Cambridge University Press:
- 24 April 2023, p. 10
-
- Article
-
- You have access
- Open access
- Export citation