14 results
Trends of antibiotic use at the end-of-life of cancer and non-cancer decedents: a nationwide population-based longitudinal study (2006–2018)
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 4 / Issue 1 / 2024
- Published online by Cambridge University Press:
- 13 May 2024, e83
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Antibiotic prescribing behavior among physicians in Asia: a multinational survey
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 3 / Issue 1 / 2023
- Published online by Cambridge University Press:
- 29 June 2023, e112
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
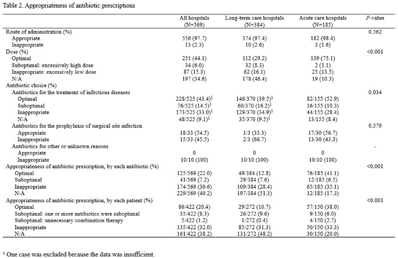
Prescriptions patterns and appropriateness of usage of antibiotics in small and medium- sized hospitals in Korea
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 2 / Issue S1 / July 2022
- Published online by Cambridge University Press:
- 16 May 2022, p. s19
-
- Article
-
- You have access
- Open access
- Export citation
Rapid diagnostic testing for antimicrobial stewardship: Utility in Asia Pacific
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 42 / Issue 7 / July 2021
- Published online by Cambridge University Press:
- 15 June 2021, pp. 864-868
- Print publication:
- July 2021
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Human resources required for antimicrobial stewardship activities for hospitalized patients in Korea
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue 12 / December 2020
- Published online by Cambridge University Press:
- 26 October 2020, pp. 1429-1435
- Print publication:
- December 2020
-
- Article
- Export citation
Evaluation of Patients’ Adverse Events Associated With Contact Isolation: Matched Cohort Study With Propensity Score
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 02 November 2020, pp. s476-s478
- Print publication:
- October 2020
-
- Article
-
- You have access
- Export citation
Impact on National Policy on the Hand Hygiene Promotion Activities in Hospitals in Korea
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 02 November 2020, p. s267
- Print publication:
- October 2020
-
- Article
-
- You have access
- Export citation
Decreased hemoglobin levels, cerebral small-vessel disease, and cortical atrophy: among cognitively normal elderly women and men
-
- Journal:
- International Psychogeriatrics / Volume 28 / Issue 1 / January 2016
- Published online by Cambridge University Press:
- 20 May 2015, pp. 147-156
-
- Article
- Export citation
Differences in the Risk Factors for Surgical Site Infection between Total Hip Arthroplasty and Total Knee Arthroplasty in the Korean Nosocomial Infections Surveillance System (KONIS)
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 33 / Issue 11 / November 2012
- Published online by Cambridge University Press:
- 02 January 2015, pp. 1086-1093
- Print publication:
- November 2012
-
- Article
- Export citation
Prospective Nationwide Surveillance of Surgical Site Infections after Gastric Surgery and Risk Factor Analysis in the Korean Nosocomial Infections Surveillance System (KONIS)
- Part of
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 33 / Issue 6 / June 2012
- Published online by Cambridge University Press:
- 02 January 2015, pp. 572-580
- Print publication:
- June 2012
-
- Article
-
- You have access
- Export citation
Clinical Epidemiology of Ciprofloxacin Resistance and Its Relationship to Broad-Spectrum Cephalosporin Resistance in Bloodstream Infections Caused by Enterobacter Species
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 26 / Issue 1 / January 2005
- Published online by Cambridge University Press:
- 21 June 2016, pp. 88-92
- Print publication:
- January 2005
-
- Article
- Export citation
Risk Factors for and Clinical Outcomes of Bloodstream Infections Caused by Extended-Spectrum Beta-Lactamase-Producing Klebsiella pneumoniae
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 25 / Issue 10 / October 2004
- Published online by Cambridge University Press:
- 02 January 2015, pp. 860-867
- Print publication:
- October 2004
-
- Article
- Export citation
Characterization of Carbon Nanotubes/Cu Nanocomposites Processed by Using Nano-sized Cu Powders
-
- Journal:
- MRS Online Proceedings Library Archive / Volume 821 / 2004
- Published online by Cambridge University Press:
- 15 March 2011, P3.25
- Print publication:
- 2004
-
- Article
- Export citation
Outcomes of Hickman Catheter Salvage in Febrile Neutropenic Cancer Patients With Staphylococcus aureus Bacteremia
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 24 / Issue 12 / December 2003
- Published online by Cambridge University Press:
- 02 January 2015, pp. 897-904
- Print publication:
- December 2003
-
- Article
- Export citation