37 results
Multi-Level Factors Associated with Relationship-Centred and Task-Focused Mealtime Practices in Long-Term Care: A Secondary Data Analysis of the Making the Most of Mealtimes Study
-
- Journal:
- Canadian Journal on Aging / La Revue canadienne du vieillissement / Volume 42 / Issue 4 / December 2023
- Published online by Cambridge University Press:
- 06 June 2023, pp. 696-709
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Thermals from finite sources in stable and unstable environments
-
- Journal:
- Journal of Fluid Mechanics / Volume 960 / 10 April 2023
- Published online by Cambridge University Press:
- 11 April 2023, A41
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
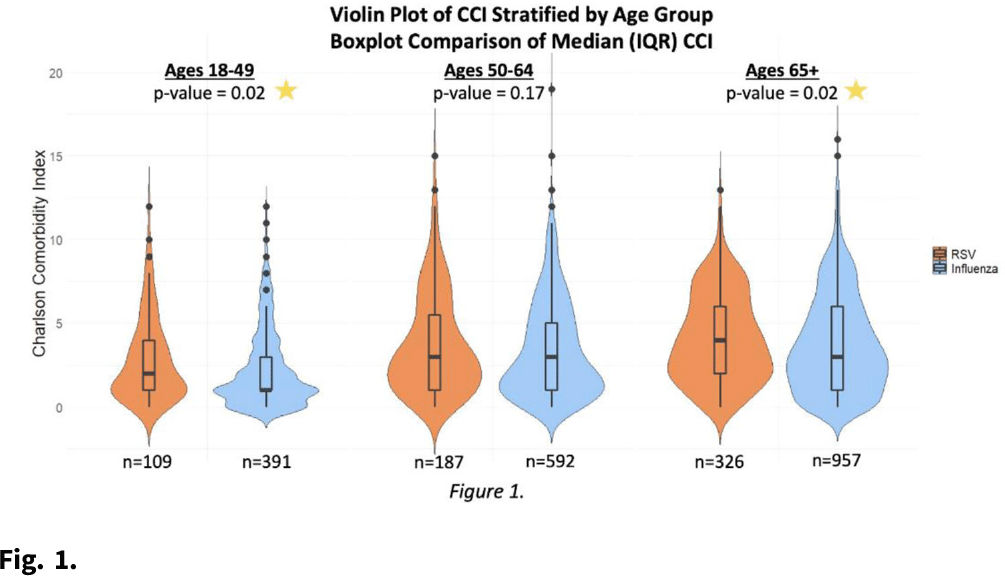
Relevance of RSV in hospitalized adults and the need for continued testing
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 2 / Issue S1 / July 2022
- Published online by Cambridge University Press:
- 16 May 2022, p. s62
-
- Article
-
- You have access
- Open access
- Export citation
Neutron Star Extreme Matter Observatory: A kilohertz-band gravitational-wave detector in the global network
- Part of
-
- Journal:
- Publications of the Astronomical Society of Australia / Volume 37 / 2020
- Published online by Cambridge University Press:
- 05 November 2020, e047
-
- Article
-
- You have access
- HTML
- Export citation
P02-08 - Mental Health Crisis Resolution and Home Treatment Teams: a Qualitative Evaluation
-
- Journal:
- European Psychiatry / Volume 25 / Issue S1 / 2010
- Published online by Cambridge University Press:
- 17 April 2020, 25-E621
-
- Article
-
- You have access
- Export citation
P-659 - the use of Coercive Measures Within Forensic Psychiatry
-
- Journal:
- European Psychiatry / Volume 27 / Issue S1 / 2012
- Published online by Cambridge University Press:
- 15 April 2020, p. 1
-
- Article
-
- You have access
- Export citation
Subfossil lemur discoveries from the Beanka Protected Area in western Madagascar
-
- Journal:
- Quaternary Research / Volume 93 / January 2020
- Published online by Cambridge University Press:
- 02 October 2019, pp. 187-203
-
- Article
- Export citation
LO68: Does point-of-care ultrasonography change actual care delivered by shock subcategory in emergency department patients with undifferentiated hypotension? An international randomized controlled trial from the SHoC-ED investigators
-
- Journal:
- Canadian Journal of Emergency Medicine / Volume 21 / Issue S1 / May 2019
- Published online by Cambridge University Press:
- 02 May 2019, p. S32
- Print publication:
- May 2019
-
- Article
-
- You have access
- Export citation
LO22: Does point-of-care ultrasonography improve diagnostic accuracy in emergency department patients with undifferentiated hypotension? An international randomized controlled trial from the SHoC-ED investigators
-
- Journal:
- Canadian Journal of Emergency Medicine / Volume 21 / Issue S1 / May 2019
- Published online by Cambridge University Press:
- 02 May 2019, p. S15
- Print publication:
- May 2019
-
- Article
-
- You have access
- Export citation
TYPIFICATION OF SRI LANKAN GESNERIACEAE
-
- Journal:
- Edinburgh Journal of Botany / Volume 76 / Issue 2 / July 2019
- Published online by Cambridge University Press:
- 20 February 2019, pp. 221-229
- Print publication:
- July 2019
-
- Article
- Export citation
A NEW SPECIES OF AESCHYNANTHUS (GESNERIACEAE) FROM VIETNAM
-
- Journal:
- Edinburgh Journal of Botany / Volume 76 / Issue 1 / March 2019
- Published online by Cambridge University Press:
- 22 October 2018, pp. 29-32
- Print publication:
- March 2019
-
- Article
- Export citation
Arsenic hazard in shallow Cambodian groundwaters
-
- Journal:
- Mineralogical Magazine / Volume 69 / Issue 5 / October 2005
- Published online by Cambridge University Press:
- 05 July 2018, pp. 807-823
-
- Article
- Export citation
TWO NEW SPECIES OF OREOCHARIS (GESNERIACEAE) FROM NORTHERN VIETNAM
-
- Journal:
- Edinburgh Journal of Botany / Volume 75 / Issue 3 / November 2018
- Published online by Cambridge University Press:
- 14 June 2018, pp. 309-319
- Print publication:
- November 2018
-
- Article
- Export citation
LO44: Initial validation of the core components in the SHoC-Hypotension Protocol. What rates of ultrasound findings are reported in emergency department patients with undifferentiated hypotension? Results from the first Sonography in Hypotension and Cardiac Arrest in the Emergency Department (SHOC-ED1) Study; an international randomized controlled trial
-
- Journal:
- Canadian Journal of Emergency Medicine / Volume 19 / Issue S1 / May 2017
- Published online by Cambridge University Press:
- 15 May 2017, pp. S42-S43
- Print publication:
- May 2017
-
- Article
-
- You have access
- Export citation
LO45: Does the use of point of care ultrasonography improve survival in emergency department patients with undifferentiated hypotension? The first Sonography in Hypotension and Cardiac Arrest in the Emergency Department (SHOC-ED1) Study; an international randomized controlled trial
-
- Journal:
- Canadian Journal of Emergency Medicine / Volume 19 / Issue S1 / May 2017
- Published online by Cambridge University Press:
- 15 May 2017, p. S43
- Print publication:
- May 2017
-
- Article
-
- You have access
- Export citation
LO43: Does point of care ultrasound improve resuscitation markers in emergency department patients with undifferentiated hypotension? The first Sonography in Hypotension and Cardiac Arrest in the Emergency Department (SHOC-ED 1) Study; an international randomized controlled trial
-
- Journal:
- Canadian Journal of Emergency Medicine / Volume 19 / Issue S1 / May 2017
- Published online by Cambridge University Press:
- 15 May 2017, p. S42
- Print publication:
- May 2017
-
- Article
-
- You have access
- Export citation
LO07: Does point of care ultrasonography improve diagnostic accuracy in emergency department patients with undifferentiated hypotension? The first Sonography in Hypotension and Cardiac Arrest in the Emergency Department (SHOC-ED1) Study; an international randomized controlled trial
-
- Journal:
- Canadian Journal of Emergency Medicine / Volume 19 / Issue S1 / May 2017
- Published online by Cambridge University Press:
- 15 May 2017, p. S29
- Print publication:
- May 2017
-
- Article
-
- You have access
- Export citation
Sleep and circadian rhythm disturbance in bipolar disorder
-
- Journal:
- Psychological Medicine / Volume 47 / Issue 9 / July 2017
- Published online by Cambridge University Press:
- 08 February 2017, pp. 1678-1689
-
- Article
- Export citation
‘The first fifty years of composite materials in aircraft construction’
-
- Journal:
- The Aeronautical Journal / Volume 96 / Issue 953 / March 1992
- Published online by Cambridge University Press:
- 04 July 2016, pp. 96-104
-
- Article
- Export citation
A qualitative evaluation of a regional obesity prevention programme
-
- Journal:
- Proceedings of the Nutrition Society / Volume 70 / Issue OCE4 / 2011
- Published online by Cambridge University Press:
- 14 October 2011, E206
-
- Article
-
- You have access
- HTML
- Export citation