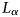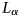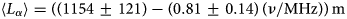109 results
Can a five-minute meeting improve the wellbeing of students? The Indian school experience
-
- Journal:
- Journal of Psychologists and Counsellors in Schools / Volume 33 / Issue 2 / December 2023
- Published online by Cambridge University Press:
- 31 August 2023, pp. 252-262
- Print publication:
- December 2023
-
- Article
- Export citation
Chapter 103 - Anesthetic Considerations of Cancer Chemotherapy
- from Section 14 - Other Situations
-
-
- Book:
- Anesthesia Oral Board Review
- Published online:
- 03 August 2023
- Print publication:
- 24 August 2023, pp 436-439
-
- Chapter
- Export citation
Metastatic breast cancer to oesophagus: a case report and review of the literature
-
- Journal:
- Journal of Radiotherapy in Practice / Volume 22 / 2023
- Published online by Cambridge University Press:
- 28 July 2023, e73
-
- Article
- Export citation
Assessing the Preparedness for a Cyanide Poisoning Mass Casualty Incident in Brooklyn
-
- Journal:
- Prehospital and Disaster Medicine / Volume 38 / Issue S1 / May 2023
- Published online by Cambridge University Press:
- 13 July 2023, p. s110
- Print publication:
- May 2023
-
- Article
-
- You have access
- Export citation
Improving Hospital Preparedness for Pediatric Abductions
-
- Journal:
- Prehospital and Disaster Medicine / Volume 38 / Issue S1 / May 2023
- Published online by Cambridge University Press:
- 13 July 2023, pp. s216-s217
- Print publication:
- May 2023
-
- Article
-
- You have access
- Export citation
Interface models for three-dimensional Rayleigh–Taylor instability
-
- Journal:
- Journal of Fluid Mechanics / Volume 959 / 25 March 2023
- Published online by Cambridge University Press:
- 16 March 2023, A10
-
- Article
- Export citation
A critical appraisal of clinical practice guidelines for the diagnosis and management of benign paroxysmal positional vertigo
-
- Journal:
- The Journal of Laryngology & Otology / Volume 137 / Issue 2 / February 2023
- Published online by Cambridge University Press:
- 17 June 2022, pp. 121-126
- Print publication:
- February 2023
-
- Article
- Export citation
In situ, broadband measurement of the radio frequency attenuation length at Summit Station, Greenland
-
- Journal:
- Journal of Glaciology / Volume 68 / Issue 272 / December 2022
- Published online by Cambridge University Press:
- 30 May 2022, pp. 1234-1242
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
ENNOBLE-ATE trial: an open-label, randomised, multi-centre, observational study of edoxaban for children with cardiac diseases at risk of thromboembolism
- Part of
-
- Journal:
- Cardiology in the Young / Volume 31 / Issue 8 / August 2021
- Published online by Cambridge University Press:
- 04 August 2021, pp. 1213-1219
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
PP143 TeCHO+ Program In Gujarat, India: A Protocol For Health Technology Assessment
-
- Journal:
- International Journal of Technology Assessment in Health Care / Volume 36 / Issue S1 / December 2020
- Published online by Cambridge University Press:
- 28 December 2020, p. 17
-
- Article
-
- You have access
- Export citation
OP145 Review Of eHealth Interventions For Improving Primary Healthcare In Low-Middle Income Countries
-
- Journal:
- International Journal of Technology Assessment in Health Care / Volume 36 / Issue S1 / December 2020
- Published online by Cambridge University Press:
- 28 December 2020, p. 2
-
- Article
-
- You have access
- Export citation
Chapter 1 - American Football: Cognitive Impairment
-
-
- Book:
- Case Studies in Sports Psychiatry
- Published online:
- 29 July 2020
- Print publication:
- 06 August 2020, pp 1-14
-
- Chapter
- Export citation
Just the facts: Risk stratifying nontraumatic back pain for Cauda Equina Syndrome in the emergency department
-
- Journal:
- Canadian Journal of Emergency Medicine / Volume 22 / Issue 5 / September 2020
- Published online by Cambridge University Press:
- 10 June 2020, pp. 652-654
- Print publication:
- September 2020
-
- Article
-
- You have access
- HTML
- Export citation
Left ventricular dysfunction in Duchenne muscular dystrophy
-
- Journal:
- Cardiology in the Young / Volume 30 / Issue 2 / February 2020
- Published online by Cambridge University Press:
- 22 January 2020, pp. 171-176
-
- Article
- Export citation
Scan Strategies for Electron Energy Loss Spectroscopy at Optical and Vibrational Energies in Perylene Diimide Nanobelts
-
- Journal:
- Microscopy and Microanalysis / Volume 25 / Issue S2 / August 2019
- Published online by Cambridge University Press:
- 05 August 2019, pp. 1738-1739
- Print publication:
- August 2019
-
- Article
-
- You have access
- Export citation
77 - Service User and Lay involvement in Health Care
- from Theme 1: - Health Care Environment and Behaviour
-
-
- Book:
- Cambridge Handbook of Psychology, Health and Medicine
- Published online:
- 05 June 2019
- Print publication:
- 16 May 2019, pp 347-352
-
- Chapter
- Export citation
Effect of concentration of etchant on the shape of etch pits on cleavage faces of calcite
-
- Journal:
- Mineralogical Magazine / Volume 37 / Issue 288 / December 1969
- Published online by Cambridge University Press:
- 05 July 2018, pp. 525-527
-
- Article
- Export citation
P120: Rapid hepatitis C virus screening and diagnostic testing for high-risk patients in an urban emergency department: a pilot project
-
- Journal:
- Canadian Journal of Emergency Medicine / Volume 20 / Issue S1 / May 2018
- Published online by Cambridge University Press:
- 11 May 2018, p. S99
- Print publication:
- May 2018
-
- Article
-
- You have access
- Export citation
23 - Surgical Procedures for Urinary Incontinence and Urethral Diverticula
- from Section 4 - Urogynecology and Pelvic Floor Dysfunction
-
-
- Book:
- Gynecologic Care
- Published online:
- 01 February 2018
- Print publication:
- 15 February 2018, pp 224-230
-
- Chapter
- Export citation
23 - Surgical Procedures for Urinary Incontinence and Urethral Diverticula
- from Section 4 - Urogynecology and Pelvic Floor Dysfunction
-
-
- Book:
- Gynecologic Care
- Published online:
- 01 February 2018
- Print publication:
- 15 February 2018, pp 224-230
-
- Chapter
- Export citation