‘Clinicians who assess and try to treat or help people who have harmed themselves are … doing so in a context that makes evaluation of their strategies and interventions complicated. Furthermore, these assessments are done by different people, from different professions, working in different clinical and local service contexts.’
(Royal College of Psychiatrists, 2004: p. 7)
‘It is like a scream without a sound.’
I recently asked a patient who repeatedly cut her forearms what provoked her to do this. ‘I do it because it’s the only way I feel I can regain control’, she replied.
Patients who injure themselves repeatedly do so for many reasons. As a non-suicidal gesture self-injury can express anger, a need to punish oneself, generate normal feelings or distraction (Reference Brown, Comtois and LinehanBrown et al, 2002), but it is helpful to understand the behaviour as an attempt at regaining mastery over intolerably distressing feelings. It can emerge in a fit of anger, or to relieve tension or unbearable urges (Reference Favazza, DeRosear and ConterioFavazza et al, 1989). Rarely, it is influenced by religious preoccupations (commands from God, purification of sins, identification with martyrs) or sexual difficulties (gender identity problems, control of hypersexuality). Regardless, the issue of emotional control is a central theme that reverberates across the patient/mental health services divide and, as I will discuss later, often determines the nature of interventions. Reference ShearerShearer (1994) portrayed self-injury as an attempt ‘to feel concrete pain when the other pain I am feeling is so overwhelming and confusing that I can’t grasp it’. Quite apart from the personal and emotional costs of self-injurious behaviour, this clinical problem has considerable financial consequences (Reference Swinton and SmithSwinton & Smith, 1997).
Self-injury and self-poisoning: do they differ?
In this article I address the issue of repeated self-injury (intentional cutting, burning or other physical damage) in individuals presenting or admitted to general psychiatric services. In line with others (Reference Taylor and CameronTaylor & Cameron, 1998; Reference Stanley, Gameroff and MichalsenStanley et al, 2001), I see self-injury as different from self-poisoning, where substances (usually drugs) are ingested, usually in order to die, cry for help or obtain temporary respite from unhappiness or unbearable distress, and I believe that people who poison themselves have different characteristics from those who injure themselves.
It has been proposed that separate syndromes of non-accidental self-poisoning and self-injury should be incorporated into the next revision of the DSM classification, on the basis of phenomenological and empirical data (Reference Kahan and PattisonKahan & Pattison, 1984; Reference MuehlenkampMuehlenkamp, 2005). Countering this argument, however, Reference Horrocks, Price and HouseHorrocks et al(2003) point out that there is a significant degree of overlap and many people both poison and injure themselves, blurring the distinction.
The majority of individuals who present with self-injurious behaviour to the accident and emergency (A&E) department are known to psychiatric services and have a diagnosis of mental disorder. Unfortunately, many are not comprehensively assessed in A&E, indicating negative staff attitudes towards them. When they are properly assessed they are more likely to be referred to psychiatric services (Reference Horrocks, Price and HouseHorrocks et al, 2003).
Self-injury cannot be ignored as a trivial event. A follow-up study of attempted suicide showed that, in more than half of those who finally died by suicide, laceration was used in the index episode of self-harm (Reference Cullberg, Wasserman and StefanssonCullberg et al, 1988).
Characteristics of individuals who repeatedly injure themselves
The UK has one of the highest incidences of self-injury in Europe, especially in schoolchildren and younger adults (Reference Hawton, Rodham and EvansHawton et al, 2002). The Office for National Statistics’ household survey of psychiatric morbidity among adults in Great Britain in 2000 found that 2% of men and 3% of women interviewed admitted to self-harm without suicidal intent; by age-group, the reported incidence decreased from 5% in young people to 0.2% of those aged 65–74 (Reference Meltzer, Lader and CorbinMeltzer et al, 2002).
Compared with individuals who present to general hospitals with self-poisoning, those who present with self-cutting are more likely to be single, unemployed males with a previous history of self-harm, living alone, misusing alcohol and to have low suicidal intent (Reference Hawton, Harriss and SimkinHawton et al, 2004). Among young adults, significantly more males than females use self-injury to kill themselves (Reference Van Heeringen and De VolderVan Heeringen & De Volder, 2002).
Individuals with personality disorders with or without an Axis I diagnosis are overrepresented among people who harm themselves (Box 1). Personality disorders have been highly correlated with self-injurious behaviour in a number of studies (Reference Horrocks, Price and HouseHorrocks et al, 2003) and repeated self-injury is one of the operational criteria for borderline personality disorder in DSM–IV(American Psychiatric Association, 1994). It is said of these patients that their stories are ‘written on their bodies’ (Reference Barker and Buchanan-BarkerBarker & Buchanan-Barker, 2004).
Box 1 Psychopathological associations in individuals who injure themselves
-
• Borderline personality disorders
-
• History of sexual abuse
-
• Disorders with somatic preoccupation
-
• Dissociative disorders
-
• Manic or depressive tendencies
-
• Alcohol use disorders
-
• Eating disorders
-
• Command auditory hallucinations
-
• Poor perceived academic performance
There is a large body of evidence associating all modes of self-harm, including repeated self-injury, with histories of sexual abuse in women and men (Reference Crowe and BunclarkCrowe & Bunclark, 2000; Reference Sansone, Gaither and SongerSansone et al, 2002; Reference Weaver, Chard and MechanicWeaver et al, 2004; Reference Gladstone, Parker and MitchellGladstone et al, 2004). Other associations are with somatic preoccupation (Reference Sansone, Wiederman and SansoneSansone et al, 2000), dissociative disorders (Reference Saxe, Chawla and Van der VolkSaxe et al, 2002), violent command hallucinations (Reference Rogers, Watt and GrayRogers et al, 2002), bipolar affective conditions (Reference D'Alessandro and LesterD’Alessandro & Lester 2000), alcohol use disorders (Reference Haw, Houston and TownsendHaw et al, 2001) eating disorders (Reference Claes, Vandereycken and VertommenClaes et al, 2001; Reference Favaro and SantonastasoFavaro & Santonastaso, 2002) and with poor perceived academic performance (Reference Richardson, Bergen and MartinRichardson et al, 2005).
It is worth noting here that self-harm, including self-poisoning and self-injury, is a strong predictor of suicide in schizophrenia, in particular for people with past or recent suicidal ideation, previous self-harm, a high number of psychiatric admissions and a history of depression or substance misuse (Reference Haw, Hawton and SuttonHaw et al, 2005).
Child and adolescent studies suggest that there are gender differences in self-cutting behaviour: females are more likely than males to say that they wished to punish themselves (51% v. 25%) and had tried to get relief from a ‘terrible state of mind’ (77.2% v. 60.9%). Individuals who cut themselves tend to be more impulsive than those who poison themselves (Reference Rodham, Hawton and EvansRodham et al, 2004). In females, body shame is also positively correlated with self-harming behaviours (Reference Milligan and AndrewsMilligan & Andrews, 2005; Reference Muehlenkamp, Swanson and BrauschMuehlenkamp et al, 2005).
Self-cutting is the most common form of self-injury (over 61%; Reference Horrocks, Price and HouseHorrocks et al, 2003). In comparison with matched healthy controls, individuals who engaged in self-injury have reported feeling less pain when carrying out the act, which could be associated with the level of distress or dissociation (Reference Bohus, Limberger and EbnerBohus et al, 2000b ).
More rarely, bizarre forms of self-mutilation occur in the acute phases of psychosis, in particular as a result of psychotic religious delusions or command hallucinations. There have been cases of attacks on genitalia, amputation of fingers or limbs and injuries to the eyes and ear lobes (Reference Simeon and HollanderSimeon & Hollander, 2001). Self-injurious behaviour is also observed in Tourette syndrome (Reference Robertson, Trimble and LeesRobertson et al, 1989), as well as in the rarer forms of trichotillomania (recurrent pulling out of one’s hair, resulting in noticeable hair loss).
Ethnic differences often play an important role in episodes of self-injury. For example, among young Asian women a high incidence of self-injury by burning, either with or without suicidal intent, has been reported both within Asia and in other countries where Asians settle (Reference Sheth, Dziewulski and SettleSheth et al, 1994). Adapting to life in a country that is not their parents’ birthplace and has very different social mores can lead them to seek a dramatic way out of their dilemmas, by suicide or serious self-injury that draws attention to their plight.
The in-patient ward
Self-injury raises considerable anxiety in referrers to psychiatric in-patient services and is often highlighted above other symptoms (Reference Way and BanksWay & Banks, 2001). The prevalence of self-injury in in-patient environments varies considerably across studies, from 5.8% to 77% (Reference Langbehn and PfohlLangbehn & Pfohl, 1993; Reference Zlotnick, Shea and PearlsteinZlotnick et al, 1996, Reference Zlotnick, Mattia and Zimmerman1999). The way in which threatened or actual self-injury is communicated to the clinician influences the clinical response. Some individuals are very open about their intentions, whereas others are discreet or even devious in their attempts to conceal them. Often the request for help comes from a distressed family member, friend or fellow patient.
There is no evidence to suggest that acts of auto-aggression are precipated by external events (although acts of aggression directed at staff or objects are). Predictably, self-injurious behaviour is more likely to occur in the evenings when the ward is quiet, and in patients’ bedrooms or areas where they can be alone (Reference Nijman and CampoNijman & Campo, 2002).
Searching in-patients
Patients who burn their skin require just a lighted cigarette, but those who repeatedly cut themselves can be very clever at importing and hiding all manner of implements. This places staff in the difficult situation of having to decide whether to search patients regularly for sharp objects. Generally speaking, such searches can be the beginning of a spiral of reactions detrimental to the therapeutic relationship. Unless patients are clearly responding to command hallucinations or delusional ideas that can lead to self-harm, it is best to let them know that regular preventive searches will not to be carried out, but that staff will respond if they are asked for help by a patient who feels the impulse to harm themselves. It is also as well to warn patients that staff would obviously take measures to prevent an incident, should they see it unfolding. In this way, the staff will be acknowledging the patient’s need to gain a measure of ascendancy over their overwhelming feelings.
Assessment of repeated self-injury
A thorough assessment is required, for which staff need dedicated training and support, with refresher training courses every 3 years (Department of Health, 1999a ). During assessment, particular attention should be paid to identifying motives and associated social problems amenable to intervention, such as psychological or social difficulties, mental disorder and alcohol or drug misuse. Good contacts with local substance misuse services can be important. Staff should assess the patient’s mental capacity and ability to give valid and informed consent. They must know when the Mental Health Act 1983 needs to be used to treat the physical consequences of self-harming behaviour. A thorough psychosocial assessment incorporating needs and risk, helped by an adequate risk assessment tool (e.g. the Manchester Self-Harm Project’s self-harm assessment form; Royal College of Psychiatrists, 2004: p. 19), can be an invaluable aid to decision-making, as long as it is accompanied by a good clinical history and an attempt to involve the patient in understanding their behaviour.
Although there is still not enough evidence to indicate treatment standards and strategies for repeated self-injury, there is consensus on how it should be assessed and the skills required to do so (Royal College of Psychiatrists, 2004). The standards contained in the College’s guidance cover assessment by both non-specialist (Box 2) and specialist staff (Box 3). It also contains recommendations on how training should take place. In essence, all trainees, regardless of their professional background, should carry out joint assessments under supervision until deemed competent. The supervisor should see at least three of the trainee’s patients during assessment. After achieving competency, the trainee should receive supervision on their next six cases.
Box 2 General clinical competencies at standard level (for staff in A&E departments)
-
• Prompt assessment of physical condition and level of consciousness
-
• Effective treatment of physical condition to minimise risk to life or risk of disability
-
• Simple psychosocial assessment to detect mental illness, alcohol or drug problems and social difficulties
-
• Detection of immediate suicide risk
-
• Judgement of when to refer for specialist assessment
-
• Making a culturally relevant assessment
-
• Understanding of capacity and consent to treatment in emergencies
(after Royal College of Psychiatrists, 2004: p. 13)
Box 3 Clinical competencies at specialist level (for psychiatrists)
-
• Making a diagnostic formulation
-
• Assessment of further risk of self-harm
-
• Drawing up an agreed management plan
-
• Linking up with appropriate services to carry out the management plan
-
• Assessing hostile or guarded patients
-
• Implementing a treatment plan, including psychological and social interventions
(after Royal College of Psychiatrists, 2004: p. 13)
Staff response to self-injury
The response of staff dealing with self-harm will depend as much on their experience as anything else. A junior psychiatrist answering a desperate call on a Friday evening about a young man threatening to cut his wrists may give different advice than a seasoned clinician who knows this patient well, and who might be able to talk him through the crisis. As mentioned earlier, at the heart of intervention is the issue of gaining and losing control, not only for patients but also for staff.
It is not always clinically advisable to put patients newly admitted because of threatened self-harm under continuous observation. Their threats may, consciously or unconsciously, be a way of obtaining personal gratification (secondary gain) from continuous attention, extra medication or special treatment (for example benefits or a community placement).
The admission experience for patients who are suicidal or have harmed themselves varies greatly in overstretched and sometimes stressful in-patient environments. It is not unusual for repeated self-injury to continue even after hospital admission. National guidelines advise that in-patient teams respond consistently to each new attempt at self-injury (National Collaborating Centre for Mental Health, 2004), dealing with the physical consequences in a way that is neither punitive nor revealing of their disappointment at yet another incident. This is a lot to ask. Reference DrewDrew (2000) suggests that consistency of nursing assignment for patients considered to be at risk of suicide is associated with better patient outcome, but others are doubtful about the benefits of special observations for patients deemed to be at risk of repeated self-harm (Reference Bowers, Gournay and DuffyBowers et al, 2000; Reference Gournay and BowersGournay & Bowers, 2000).
There is evidence that training or experience in psychotherapy allows staff to contain their anxiety more effectively when dealing with people who mutilate themselves (Reference Huband and TantamHuband & Tantam, 2000).
Relationships with other patients and family members
Occasionally in-patients who injure themselves can induce others to use copy-cat behaviour in order to achieve secondary gain. But if properly handled, and if appropriate therapeutic options are available, there is a good chance that individuals will use the time with staff and other patients to reflect and gain perspective on their motivations to injure themselves. In particular, opportunities to discuss their difficulties in individual counselling sessions with trained staff or to participate in group therapy can be of great value.
The in-patient facility can also be a temporary safe haven from stressors and circumstances that triggered self-harm. However, the psychosocial pressures that prompted self-injuring behaviour often remain on discharge, and staff should use the admission to address factors that played a part in the self-injuring behaviour, such as symptoms of mental illness or dependency on alcohol or drugs. Work can be done with the patient alone or with members of the patient’s family or friends to discuss difficulties and come up with different strategies.
The discharge CPA meeting
If the patient is to be discharged under the care programme approach (CPA), issues of control and the potential for suicide are likely to overshadow the CPA planning meeting, which is attended by the patient, staff and sometimes family members or carers. If there is any hint of a surrender of control to others, the patient may see the meeting as a means to assuage other people’s fears, rather than as a venue in which their own feelings can be addressed. However, sensitively conducted the discharge CPA meeting can offer a constructive way forward for everybody concerned.
One of the most valuable things that staff can do during the meeting is to explore with the patient and family alternative, non-destructive ways in which the patient can regain control of unpleasant feelings. It is important to acknowledge the risk of repetition but to stress that help is at hand from named people and outreach services such as crisis intervention teams and emergency telephone contacts. Also stress that follow-up and support will be available for both the patient and their carers.
If a substantive diagnosis of borderline personality disorder has been made, referral to dedicated specialist services, if they are available locally, should be considered before discharge.
Dealing with countertransference
It is worrying that surveys have indicated training of staff to deal with countertransference to be ‘suboptimal’ in many parts of mental health services (Reference Slinn, King and EvansSlinn et al, 2001). Strong countertransference feelings may be expressed in the wish to discharge a patient or transfer them to an intensive care ward, to become overinvolved in the case, to be punitive or critical, to berate the consultant for admitting the patient in the first place or not doing something more effective to prevent a repeated self-injury. Staff often need support and the opportunity to disclose these uncomfortable and conflicting feelings in a confidential and trusting environment such as individual supervision or staff groups. Junior doctors can benefit from their individual sessions with their consultants, but only if their relationship with their senior trainer feels safe. It seems that nurses, because of their close relationship with patients, are especially vulnerable to being drawn into the emotional maelstrom created by patients in crisis, especially if they have no robust supervisory arrangements to support them (Reference ReeceReece, 2005).
Staff guidelines for intervention
Also of concern are reports that mental health workers in general (Reference Jeffery and WarmJeffery & Warm 2002), and nurses in particular, often have a poor understanding of self-harm (Reference ReeceReece, 2005). Having a well-written and easily accessible self-harm policy on the unit can be very helpful (Box 4 gives some guidelines), but is certainly not enough. Regular policy updates and staff training are essential. ‘Serious untoward incidents’ offer an important opportunity for reflection on practice.
Box 4 Guidelines for staff dealing with repeated self-injury (adapted from Reference GoughGough, 2005)
-
• Record details of all incidences of self-injury and describe possible environmental or personal factors in order to detect patterns
-
• Ensure that all physical injuries are examined and treated
-
• Ensure that all staff are adopting a consistent response to the behaviour
-
• Ensure that the individual is also given attention and support at times when they are not engaging in self-injury
-
• Adopt a non-judgemental attitude
-
• Encourage the person to engage in psychological treatment in order to understand the behaviour
-
• Try to instil a sense of hope
-
• Encourage problem-solving skills
-
• Avoid putting pressure on the individual not to self-harm, without condoning or being indifferent to it
-
• Plan what to do if a person approaches a member of staff saying that they have an urge to injure themselves
-
• Foster the notion that people who harm themselves need to be in control over their treatment and be responsible for their behaviour
-
• Ensure that staff are adequately supported
It is useful and clinically prudent to try to understand what the patient is communicating and to decide on a style of response to future gestures of this nature, with an eye to the long-term goal of making the distress something that the patient can recognise and deal with in more constructive ways. This understanding and conceptualisation needs to be agreed between all clinical workers likely to be in contact with the patient, as it is very important that everybody is working in the same manner and that messages are clear and unequivocal (Reference Shepperd and McAllisterShepperd & McAllister, 2003; National Collaborating Centre for Mental Health, 2004).
Equally important is that staff understand the very strong negative countertransference feelings mentioned in the previous section. Too much reliance on firm guidelines and expectations of ‘having the right attitude’ can have a counterproductive effect on both staff and patients.
Boxes 5 and 6 show some useful mnemonic guidelines, although I would suggest that they should not be interpreted too rigidly.
Box 5 REASSURE: mnemonic guidelines for staff dealing with repeated self-injury
-
• Respond sensitively and with empathy
-
• Explore the reasons that the person has injured him- or herself
-
• Accept that self-injury may continue for some time. The aim is to understand and support the individual in their distress, to help them gain more control over their feelings and increase their self-esteem
-
• Support the person (emotionally and practically) following self-injury
-
• Seek support for yourself
-
• Understand that self-injury is underpinned by distress or unhappiness of some kind
-
• Recognise that self-injury is a mechanism that is used to manage problems, feelings and experiences
-
• Examine associated problems such as bullying, bereavement or relationship difficulties
(Reference Paton and JenkinsPaton & Jenkins, 2002: disk 2, p. 7)
Box 6 ACCEPT: don’ts for staff dealing with repeated self-injury
Do not:
-
• Accuse the person of being manipulative or attention seeking. It is simplistic to think that self-injury is carried out as a way of manipulating the system or individuals in it. It is very unusual for people to injure themselves simply to gain ‘attention’
-
• Criticise the person for what they have done. This will make them feel worse and is likely to be counterproductive
-
• Conclude that the person is a ‘lost cause’ and nothing can be done to help them
-
• Expect too much of yourself. It is very unlikely that you will have all the answers. You are not expected to ‘get to the bottom’ of the individual’s problems or to be able to solve it
-
• Put pressure on the person to tell you about underlying factors if they don’t want to
-
• Threaten to take away your support if the person harms him- or herself again
(Reference Paton and JenkinsPaton & Jenkins, 2002: disk 2, pp. 7–8)
It is important to remember that people who repeatedly injure themselves may be doing it for different reasons on different occasions, and that it is easy to be complacent when assessing motivations, jumping to conclusions rather than looking at each new incident with fresh eyes:
‘there is no single explanation of self-harm, no single meaning or communication conveyed by self-harm and no single psychological disorder or personality profile associated with self-harm’ (Reference TurpTurp, 2002).
Treatment strategies
As mentioned above, repeated self-injury on in-patient units is likely to happen in the evening and when the individual can be alone. Staff caring for patients with a history of repeated self-harm should therefore be more vigilant when the ward is quiet and particulary if an individual seeks isolation or retreats to their bedroom. It is not unusual for patients in psychiatric units to have single bedrooms, and staff may have to decide whether it might be safer to assign shared bedrooms to patients known to harm themselves. Staff might also consider introducing communal activities as a matter of routine in the evening hours. There is no evidence to suggest that ‘safety agreements’ between staff and patients affect the incidence of self-harm (Reference Potter, Vitale and DawsonPotter et al, 2005).
Studies have shown that manual-assisted cognitive–behavioural therapy is a cost-effective method of reducing self-harming behaviour, but mostly in patients without borderline personality disorder (Reference Byford, Knapp and GreenshieldsByford et al, 2003; Reference Tyrer, Thompson and SchmidtTyrer et al, 2003, Reference Tyrer, Tom and Byford2004). In patients with borderline personality disorder, and in particular when the self-injurious behaviour is accompanied by dissociative states, dialectical behavioural therapy has been reported to be successful in secure hospitals (Reference Bohus, Haaf and StiglmayrBohus et al, 2000a ; Reference Low, Jones and DugganLow et al, 2001).
There are reports that naltrexone at doses of 50 mg/day can reduce repeated self-injurious behaviour when other treatments have failed (Reference Roth, Ostroff and HoffmanRoth et al, 1996; Reference Griengl, Sendera and DantendorferGriengl et al, 2001). Similar results have been published for clozapine (Reference Ferreri, Loze and RouillonFerreri et al, 2004). At present, neither of these treatments can be recommended, owing to the scarcity of data on their clinical use.
Community care
Community mental health centres are now likely to be a patient’s first point of contact with psychiatric services, and members of the multidisciplinary team are often asked to assess individuals who cause concern because of their self-harming behaviour. The establishment of alternatives to hospitalisation such as crisis resolution, home treatment and assertive outreach teams, has further complicated the management of care of people who repeatedly harm themselves. Levels of anxiety in staff and families are likely to determine whether home care is feasible or advisable. The difficult question facing the community team will always be: ‘Is it safe to manage this patient’s behaviour in the community?’
Indicators of community management
With patients known to services, previous experience of the type and seriousness of the injury may help staff to decide whether community care is appropriate. However, team members must be aware that complacency might lead themselves or colleagues to underestimate the seriousness of the behaviour, particularly if the patient presents with added emotional or psychosocial precipitants. Good training in risk assessment and management, as well as adequate supervision, helps to increase team members’ competence and confidence in the management of this anxiety-provoking disorder. The support and involvement of the patient’s family should also be taken into account, particularly if family members are coming to the end of their tether. Sometimes it is possible to help the patient by offering support to the family.
Community staff themselves need considerable support in caring for individuals who engage in repeated self-harm. Much of this can be shared with other team members, but often the senior psychiatrist will be carrying the anxiety of the entire team.
It is important that psychiatrists attached to community teams are aware of the medico-legal issues involved in caring for people who harm themselves, and have ensured that legal requirements are met and that team decisions and the reasons for making them are properly recorded.
Self-help strategies
A number of healthcare trusts and organisations have produced literature on repeated self-injury (Reference Arnold and MagillArnold & Magill, 1997, Reference Arnold and Magill1998; Selby and York Primary Care Trust, 2003. These guidelines and booklets, intended for service users and carers, give users’ accounts that can help people to understand the hidden causes of self-injury and to find alternative behaviours. They also debunk popular statements about self-injury which describe it, for example, as very rare, something that people grow out of, a failed suicide attempt and a habit that doesn’t hurt. User-led websites focusing on self-cutting are also used extensively in the UK (Reference Prasad and OwensPrasad & Owens, 2001): the home page of the American Self-Harm Clearing House (http://www.selfinjury.org) has a link to the Bodies Under Siege web ring, which currently includes 158 active sites.
Conclusions
Although public awareness of repeated self-injury, particularly in adolescents and young adults, appears to be increasing, mental health services are still lagging behind in defining and implementing strategies for prevention, assessment and management. This delay betrays a predominantly negative attitude towards people who injure themselves. Increased knowledge of the powerful underlying psychological forces that prompt this behaviour would increase the chances that these patients can be helped to gain mastery over their overwhelming emotions.
Declaration of interest
None
MCQs
-
1 Repeated self-injury:
-
a never leads to completed suicide
-
b is mostly carried out by girls and women
-
c is always a cry for help
-
d always starts in late adolescence
-
e is common in people with borderline personality disorder.
-
-
2 People who repeatedly injure themselves:
-
a are more likely to do so when they know that they will be discovered
-
b are more likely to have an underlying psychiatric disorder
-
c usually do so for the same reason every time
-
d do so impulsively
-
e feel intense pain during the injury.
-
-
3 Assessments of people who injure themselves:
-
a should not be carried out by A&E staff
-
b cannot be carried out if the patient is unable to give valid consent
-
c can be aided by risk-assessment tools
-
d aim to discover trigger factors amenable to intervention
-
e lead to evidence-based intervention strategies.
-
-
4 People who harm themselves and are admitted to a psychiatric unit:
-
a should be placed on very close observation
-
b often repeat the event in hospital
-
c are less likely to repeat the behaviour early in the morning
-
d should be searched regularly for items that they could use in self-injury
-
e are less likely to do so if they are invited to approach staff if they feel the urge to hurt themselves.
-
-
5 Treatment strategies for repeated self-injury can be helped by:
-
a cognitive–behavioural therapy
-
b making staff aware of strong countertransference feelings
-
c adopting prearranged responses
-
d the provision of CCTV cameras
-
e a CPA meeting involving family and other agencies.
-
MCQ answers
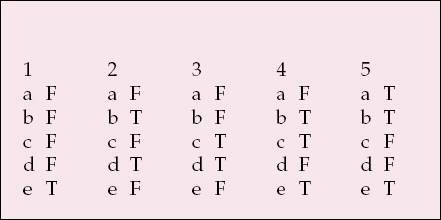
| 1 | 2 | 3 | 4 | 5 | |||||
|---|---|---|---|---|---|---|---|---|---|
| a | F | a | F | a | F | a | F | a | T |
| b | F | b | T | b | F | b | T | b | T |
| c | F | c | F | c | T | c | T | c | F |
| d | F | d | T | d | T | d | F | d | F |
| e | T | e | F | e | F | e | T | e | T |





eLetters
No eLetters have been published for this article.