The term schizotypy (Reference MeehlMeehl, 1962) describes eccentric behaviour similar to that in patients with schizophrenia but less florid and debilitating. The Structured Interview for Schizotypy (SIS; Reference Kendler and Lister-SharpKendler & Lister-Sharp, 1989) is an interview assessment based partly on self-report symptoms and partly on interviewer judgements. Its factor structure has been determined in first-degree relatives of patients (Reference Kendler, McGuire and GruenbergKendler et al, 1995), with seven factors emerging. There have been other factor studies (Reference GruzelierGruzelier, 1996), but exact comparisons are difficult. Gruzelier (Reference Gruzelier1996) suggests that schizotypy consists mainly of impulsive non-conformity, social anxiety, positive features such as unusual perceptions and negative features such as introversion. The present study uses the Edinburgh study of subjects at high risk of developing schizophrenia to examine three issues. What is the factor structure of the SIS in these subjects? Do subjects showing psychotic symptoms manifest higher levels of schizotypal symptoms and signs? Are there aspects of schizotypy that predict future schizophrenia?
METHOD
The Edinburgh High-Risk Study has been described in greater detail in previous papers (Reference Byrne, Hodges and GrantByrne et al, 1999; Reference Hodges, Byrne and GrantHodges et al, 1999; Reference Lawrie, Whalley and KestelmanLawrie et al, 1999; Reference Johnstone, Abukmeil and ByrneJohnstone et al, 2000). Briefly, the main concern here is with three groups, all of which have been recruited since the start of the project in 1994. The 155 high-risk subjects were aged 16-25 years, had never themselves received a diagnosis of serious psychiatric disorder and were not clinically ill at recruitment but had at least two first— or second-degree relatives who suffered from schizophrenia. This group was recruited throughout Scotland by a painstaking process involving scrutiny of psychiatric case notes followed by approaches to adolescent relatives of patients. A control group of 36 subjects with no known family history of psychotic illness, comparable to the high-risk group in age, gender and social class, was obtained partly from Edinburgh youth groups and partly from the social network of the high-risk group. Finally, a group of 37 first-episode patients from the Edinburgh area who met DSM—IV (American Psychiatric Association, 1994) criteria for schizophrenia and were aged 16-25 years was recruited. This last group had no known relatives with schizophrenia. After complete description of the study to the subjects, written informed consent was obtained. The first two groups have been followed up at approximately 18-month intervals and, at the time of writing, it is intended that this procedure will continue until the year 2004. The latter two groups are deliberately smaller than the high-risk group in order to be comparable to the predicted number of high-risk subjects who ultimately suffer full-blown psychotic illness. This ultimately should facilitate comparison of well subjects and ill subjects with and without relatives with schizophrenia.
It will be 10 years from the commencement of the study before we can make these comparisons, and in the meantime many data have been acquired. Interim analyses have been conducted because the plan for the second 5 years (and indeed the funding) depended on the progress and findings of the first 5 years. The analysis is complicated further by the fact that, because the recruitment was conducted during the study, the length of time for which subjects have been involved is variable. The plan is to consider the findings at four time points: after approximately 3 years, when 100 cases had been ascertained; after 4.5 years, at closure of the first phase; after a further 3.5 years, when the situation of each person in the study after 5 years will be considered, and at closure of the study, for the final comparison as described above. The data in this paper are from the second collection point.
On entry to the study all groups received, as part of a larger battery, the SIS administered by one interviewer and the Present State Examination (PSE; Reference Wing, Cooper and SartoriusWing et al, 1974) administered by another. The SIS contains two main sections, the first of which consists of a structured interview with probes in which the interviewer elicits self-reported information on schizotypal symptoms and social relationships. This results in 19 global ratings on seven-point scales of items such as childhood social isolation, ideas of reference, magical thinking and impulsivity. The second section, on schizotypal signs, consists of the interviewer's observations of behaviour during the interview. There are 16 scales covering, for example, rapport, attention-seeking, grooming and enjoyment of the interview. Average intraclass correlations in the original studies were of the order of 0.8 for symptoms and 0.7 for signs. In our own study they were 0.85 for symptoms and signs together.
The PSE consists of 140 items covering psychiatric symptoms, both psychotic and non-psychotic. Patients were classified as having psychotic symptoms if, according to specified PSE items (listed in Reference Johnstone, Abukmeil and ByrneJohnstone et al, 2000), they showed evidence of delusions, hallucinations or other behaviour commonly present in schizophrenia. In no case were these symptoms sufficiently severe to meet any of the common criteria for a clinical diagnosis of psychotic illness. These subjects did not regard themselves as ill and their general practitioners confirmed that they were not known to be suffering from a psychiatric illness, had never been regarded as psychotic or possibly psychotic and had not received treatment with antipsychotic drugs.
In addition, the later clinical status of all the control and high-risk subjects was ascertained up to July 1999. This was done partly at follow-up interviews and partly by contacting their general practitioners. All subjects who gave rise to concern over their clinical status were interviewed using the PSE and, where appropriate, a diagnosis of schizophrenia in terms of ICD-10 (World Health Organization, 1992) was assigned.
RESULTS
Subjects
Of 228 subjects recruited into the study and providing at least some data, 16 either were not tested on the SIS or failed to complete it in full. The analyses below concern mainly the global assessment items of the SIS, excluding the item ‘adult anti-social traits’, which was missing in a large number of cases. The remaining 212 subjects were grouped initially as follows:
-
(a) 36 control subjects;
-
(b) 113 non-symptomatic high-risk subjects who displayed no psychotic symptoms on the PSE at the time of entry to the study;
-
(c) 38 symptomatic high-risk subjects who did display psychotic symptoms on their entry assessment but who, by definition, were not clinically ill.
-
(d) 25 first-episode patients with schizophrenia.
These groups were similar in age, with mean ages ranging from 21.2 to 21.6 years (F=0.2, d.f.=3,224, NS). There was no significant difference in gender composition (% female: controls, 52.8; high-risk non-symptomatic, 48.1; high-risk symptomatic, 55.3; and patients, 32.4; χ2=4.93; d.f.=3; P=0.18). However, the controls and the patients had more fathers in non-manual social classes (% non-manual: controls, 60.0; high-risk non-symptomatic, 33.7; high-risk symptomatic, 27.9; patients, 58.3; χ 2=12.65; d.f.=3; P=0.005). On entry, four of the controls were found to have psychotic symptoms, mainly isolated hallucinations (Reference Johnstone, Abukmeil and ByrneJohnstone et al, 2000). These subjects were included in the overall factor analysis described below but were dropped from the other analyses.
Factor structure of schizotypy
Principal component analysis with varimax rotation was performed on the SIS items using data on all 212 subjects. Before factoring, the scoring direction of each item was reversed (i.e. the item was scored with the most severe ratings scored highest) and the resulting score was log-transformed. Principal components analysis yielded nine components with eigenvalues greater than unity, but the scree test clearly indicated that only four should be extracted. Table 1 shows the rotated component loadings. These four components account for 47.8% of the variance and will be labelled social withdrawal, psychotic symptoms, socio-emotional dysfunction and odd behaviour. This structure was compared with that obtained when the same extraction was performed on the high-risk group only. On correlating the factor loadings obtained for each component in the two analyses, the lowest of the four possible correlations was 0.82.
Table 1 Rotated principal component loadings from the Structured Interview for Schizotypy1 for all subjects

| Component | ||||
|---|---|---|---|---|
| I Social withdrawal | II Psychotic symptoms | III Socio-emotional dysfunction | IV Odd behaviour | |
| Introversion | 0.72 | |||
| Sensitivity | 0.72 | |||
| Social anxiety | 0.69 | 0.39 | ||
| Social isolation | 0.64 | 0.31 | ||
| Childhood social isolation | 0.60 | |||
| Observed anxiety (during interview) | 0.53 | |||
| Observed blunting of affect | 0.39 | |||
| Ideas of reference | 0.39 | 0.66 | ||
| Derealisation/depersonalisation | 0.66 | |||
| Magical thinking | 0.65 | |||
| Illusions | 0.64 | |||
| Impulsiveness | 0.63 | 0.32 | ||
| Irritability | 0.62 | |||
| Suspiciousness | 0.40 | 0.57 | ||
| Psychotic-like phenomena | 0.56 | |||
| Childhood antisocial traits | 0.47 | 0.39 | ||
| Affective instability | 0.32 | 0.44 | ||
| Suicidal threats | 0.43 | 0.40 | ||
| Emptiness | 0.38 | 0.40 | ||
| Observed rapport | 0.36 | 0.68 | ||
| Observed enjoyment of the interview | 0.65 | |||
| Observed interpersonal functioning | 0.43 | 0.65 | ||
| Occupational functioning | 0.62 | |||
| Restricted emotion | 0.56 | |||
| Observed affect | 0.40 | 0.54 | 0.43 | |
| Observed psychiatric functioning | 0.49 | 0.50 | ||
| Observed narcissism | 0.75 | |||
| Observed attention-seeking | 0.75 | |||
| Observed odd behaviour | 0.67 | |||
| Observed flirtatiousness | 0.58 | |||
| Observed irritability | 0.53 | |||
| Observed suspiciousness | 0.52 | |||
| Observed speech organisation | 0.49 | |||
| Observed grooming | 0.33 | 0.37 | ||
Univariate distributions of schizotypal symptoms and signs
On performing a one-way analysis of variance (ANOVA) on the four groups of subjects, significant overall differences beyond the 0.05 level are apparent on 31 out of 35 of the SIS items (18 differences are beyond the 0.001 level). On the majority of items, the symptomatic high-risk group score was worse than that of the non-symptomatic high-risk group. The exceptions mostly concern symptoms reflecting problems with social interaction. Mean values for the control group are generally similar to those for the non-symptomatic high-risk group.
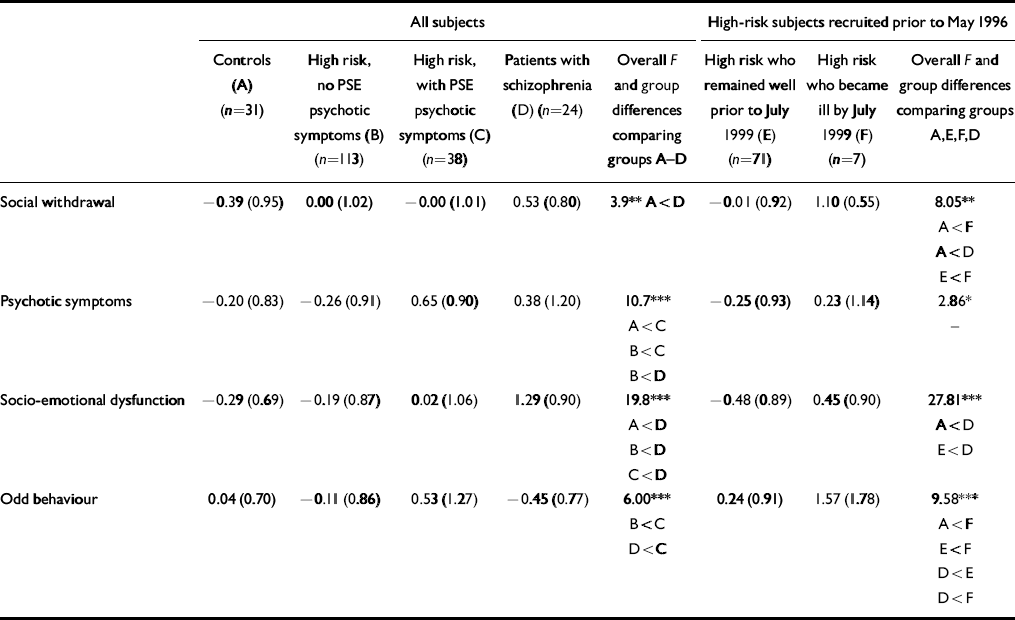
Table 2 sets out the means and standard deviations on the four principal components extracted and also the results of a one-way ANOVA followed by the Scheffé test. On social withdrawal, the patients with schizophrenia score highest and differ significantly from the control group. For psychotic symptoms the patients and the symptomatic high-risk group are similar and score higher than the other groups. The patients are clearly worse than the other groups on socio-emotional dysfunction but the symptomatic high-risk group score highest on odd behaviour.
Table 2 The Structured Interview for Schizotypy factor scores for all subjects on entry to the study and for high-risk subjects recruited prior to May 1996 (mean (s.d.))
| All subjects | High-risk subjects recruited prior to May 1996 | |||||||
|---|---|---|---|---|---|---|---|---|
| Controls (A) (n=31) | High risk, no PSE psychotic symptoms (B) (n=113) | High risk, with PSE psychotic symptoms (C) (n=38) | Patients with schizophrenia (D) (n=24) | Overall Fand group differences comparing groups A—D | High risk who remained well prior to July 1999 (E) (n=71) | High risk who became ill by July 1999 (F) (n=7) | Overall Fand group differences comparing groups A, E, F, D | |
| Social withdrawal | -0.39 (0.95) | 0.00 (1.02) | -0.00 (1.01) | 0.53 (0.80) | 3.9**A < D | -0.01 (0.92) | 1.10 (0.55) | 8.05** |
| A < F | ||||||||
| A < D | ||||||||
| E < F | ||||||||
| Psychotic symptoms | -0.20 (0.83) | -0.26 (0.91) | 0.65 (0.90) | 0.38 (1.20) | 10.7*** | -0.25 (0.93) | 0.23 (1.14) | 2.86* |
| A < C | - | |||||||
| B < C | ||||||||
| B < D | ||||||||
| Socio-emotional dysfunction | -0.29 (0.69) | -0.19 (0.87) | 0.02 (1.06) | 1.29 (0.90) | 19.8*** | -0.48 (0.89) | 0.45 (0.90) | 27.81*** |
| A < D | A < D | |||||||
| B < D | E < D | |||||||
| C < D | ||||||||
| Odd behaviour | 0.04 (0.70) | -0.11 (0.86) | 0.53 (1.27) | -0.45 (0.77) | 6.00*** | 0.24 (0.91) | 1.57 (1.78) | 9.58*** |
| B < C | A < F | |||||||
| D < C | E < F | |||||||
| D < E | ||||||||
| D < F | ||||||||
The SIS as a predictor of the development of schizophrenia
To investigate this question an interim analysis of the first recruits to the high-risk group was attempted. Half of the current high-risk subjects had been recruited by the end of April 1996 and were included in this analysis. This left a minimum period of 39 months (to July 1999) in which a high-risk subject might become clinically ill. Seven subjects from this reduced high-risk group became ill within 39 months of recruitment. One other subject, recruited early in the study, developed psychotic illness more than 39 months after recruitment but for the purpose of the analysis was considered to be well. All the controls have remained well so far. In the analysis shown in Table 2 these early recruits to the high-risk group are divided into those who became clinically ill (group F) and all those who did not become ill (group E), irrespective of whether or not they had psychotic symptoms at the start of the study.
Comparisons again are made with the controls and the patients with schizophrenia using a one-way ANOVA followed by the Scheffé test. Ideally, groups E and F also would have been divided on psychotic symptom status at the start of the study, but numbers are unfortunately too small for this. However, it may be noted that three of the group F subjects demonstrated PSE psychotic symptoms on entry to the study but four did not, and in group E 16 subjects had symptoms at first interview but 55 did not. Despite the small numbers, several significant differences are evident. The seven high-risk subjects who became ill show high levels of social withdrawal and very high levels of odd behaviour (beyond the 0.01 level on the Scheffé test compared with all three of the other groups). On socio-emotional dysfunction they are intermediate between the patients and the other groups. For psychotic symptoms the discrimination between the groups is less clear. Following these analyses, receiver operating characteristic (ROC) analyses were run to determine the best cut-off points for each SIS component and for the total of all four components for predicting onset. Table 3 gives these cut-off points and sets out the sensitivity, specificity, positive predictive power and negative predictive power. Based on the positive predictive power, social withdrawal is the best single predictor of later illness, but the combination of all four components is best of all.
Table 3 Sensitivities, specificities, positive predictive power and negative predictive power of the four Structured Interview for Schizotypy (SIS) factors for the onset of psychosis

| Cut-off point1 | Sensitivity2 | Specificity3 | Positive predictive power4 | Negative predictive power5 | |
|---|---|---|---|---|---|
| Social withdrawal | 1.08 | 0.71 | 0.90 | 0.42 | 0.97 |
| Psychotic symptoms | 1.03 | 0.43 | 0.90 | 0.30 | 0.94 |
| Socio-emotional dysfunction | 0.23 | 0.71 | 0.85 | 0.31 | 0.96 |
| Odd behaviour | 0.44 | 0.86 | 0.61 | 0.18 | 0.98 |
| Total of all four SIS factors | 2.24 | 0.86 | 0.96 | 0.67 | 0.99 |
DISCUSSION
The three main aims of the study were to examine the factor structure of schizotypy, to compare four groups of subjects on schizotypal symptoms and signs and to see whether future psychotic illness might be predicted from any aspects of schizotypy.
Factor structure of schizotypy
Factor analysis of the SIS within these heterogeneous groups of patients with schizophrenia, high-risk subjects and controls requires justification. It was hoped that the structure found would still show similarities to those in other studies, thus demonstrating robustness within different populations. Furthermore, it was thought that data reduction was desirable both to clarify the findings and to reduce the possibilities of chance findings. As demonstrated by the high intercorrelations of the factor loadings, the factor structures obtained are similar when the analysis is carried out on all subjects or just on the high-risk group.
The structure discovered may be compared with that found in other studies, particularly that of Kendler et al (Reference Kendler, McGuire and Gruenberg1995). The methods of the current study differ from the latter in several important respects (e.g. in using 34 items from the SIS, which are sometimes different from the 25 items assessed by Kendler et al) but there are considerable similarities in the factor structure found. The social withdrawal component here is very similar to the avoidant factor identified by Kendler et al. The component that we labelled ‘psychotic symptoms’ appears to be very close to Kendler et al's positive schizotypy and might have been so termed had it not also contained some of their borderline symptoms. Their components of negative schizotypy, odd speech and suspicious behaviour are similar to our odd behaviour component. Finally, their social dysfunction contains an item loading on our socio-emotional dysfunction, namely poor occupational functioning. In our analysis we also looked briefly at the nine-component solution using eigenvalues greater than unity. When this is done, components very similar to Kendler et al's positive schizotypy and avoidant symptoms are still evident. Again, there are other somewhat less compelling similarities.
The SIS psychotic symptoms on entry to the study and the development of schizophrenia
Almost all of the SIS items yielded significant mean differences between the groups of subjects but the patterns seem clearest when individual items are combined into the four principal components. Unsurprisingly, the results show that at recruitment the SIS components largely reflect psychotic symptoms as measured by the PSE.
It is possible to draw some interesting conclusions from the results in Tables 2 and 3 but before doing so there are some important caveats. The patients with schizophrenia were chosen to have no known family history of schizophrenia. This was to facilitate ultimate comparisons between the nature of psychoses developed where there was a known familial risk and where there was no such risk. Different findings might have been obtained had this patient group also been from families at high risk. Second, the results on predicting illness at this stage necessarily refer only to half of the high-risk group. Numbers falling ill so far have been small and the time period in which illness might be expected is by no means past.
On predicting illness, despite the small numbers ill and the relatively short time period, there are some highly significant results. The best all-round predictor of onset appears to be social withdrawal. Overall, within the group of subjects in these analyses 7/78 (9%) of the subjects fell ill. On social withdrawal the positive predictive power shows that 5/12 (42%) of the subjects above the cut-off point develop illness. In contrast, 64/66 (97%) of those below the cut-off point remain well. Despite the high mean value of the seven onset cases on odd behaviour, the positive predictive power is much lower at only 0.18. In other words, although odd behaviour picks out 6/7 of the onset cases, it has a lower specificity — 28/71 of the subjects who are well also score above the cut-off point. Although each component predicts to some extent, there is little evidence that any one of them is specific for schizophrenia. A combination of all four is the best predictor, with 6/9 (66.7%) of the subjects who score above the cut-off point falling ill and 68/69 (99%) below it remaining well.
The results on odd behaviour are interesting in that those who become ill show higher scores than all other subjects, whereas the patients with schizophrenia have the lowest scores of all. One possibility is that all four components are indicators of a subclinical psychotic state likely to develop into psychosis. As this ‘prodromal’ state worsens into clinical schizophrenia, the odd behaviour may give way to frank psychotic symptoms while social functioning deteriorates further. An alternative possibility is that antipsychotic and other treatment (given to the patients with first-episode schizophrenia but not, at the time of testing, to the high-risk subjects) may reduce odd behaviour preferentially.
Thus, it appears that schizotypy is heterogeneous. In common with other studies, it proved possible to extract several principal components from the original SIS item scores and, in the case of the current study, there were four distinct components. Although numbers are small, the indications are that a subject scoring high on any one of these may be in a subclinical or prodromal stage and has a somewhat increased risk of schizophrenia onset. When high scores occur in combination, there is a stronger risk of illness. The current study can, at present, throw little light on the duration of such a prodromal state, whether it inevitably develops into clinical illness or whether there are other factors involved in triggering psychosis proper. Opportunities exist, however, within the project for pursuing these matters further.
Clinical Implications and Limitations
CLINICAL IMPLICATIONS
-
• Schizotypy as measured by the Structured Interview for Schizotypy (SIS) may be divided reasonably into at least four components, these being social withdrawal, psychotic symptoms, socio-emotional dysfunction and odd behaviour.
-
• Isolated schizotypal symptoms and signs are seldom precursors of an impending onset of schizophrenia.
-
• The risk of early onset of schizophrenia in young people at high risk is greatest when a combination of SIS symptoms and signs is present, spanning social withdrawal, psychotic symptoms, socio-emotional dysfunction and odd behaviour. No more specific predictor of a first onset of schizophrenia was identified.
LIMITATIONS
-
• The factor structure described may have been influenced slightly by the heterogeneous nature of the sample.
-
• The predictions of schizophrenia onset are based on small numbers and a limited follow-up period.
-
• The patients with schizophrenia included in the cross-sectional group comparisons had no known relatives with schizophrenia and might not be representative of all such patients.
Acknowledgements
This study was conducted with the approval of the ethics committees of areas in Scotland from which the subjects came. We thank many general practitioners and psychiatrists for access to patients and are deeply grateful to the subjects and their families for their generous assistance. The project was funded by the Medical Research Council.








eLetters
No eLetters have been published for this article.