Drivers for change
Integrated care is proposed as a more efficient client-oriented health model, building services around local populations. Drivers include a growing and ageing population with greater comorbidities, as well as workforce and financial challenges. In the UK, the NHS Long Term Plan 1 is mandating ‘integrated care systems’ (ICSs) to develop and deliver locally relevant 5-year plans. Several critical questions remain unanswered: what does ‘integration’ mean; which services ‘should’ be integrated; how to win hearts and minds of staff during integration; and how to measure its ‘success’? Evaluation cannot be an add-on to becoming an ICS, it must be integral to enable the spread of best practice and learning from failures.
Over the past decade, National Health Service (NHS) funding has grown by about 1% annually. Approximately 40% of NHS trusts are reporting deficits, up from less than 10% in 2009–10.2 The NHS Long Term Plan promises £20.5 billion more by 2023 (£2.3 billion for mental health),1 a 3.4% increase, but still below the 4% recommended to meet demand.2 Nevertheless, health has – arguably – always been proportionately better funded and supported than social care, politicians perhaps more averse to the electoral challenges of closing clinical services. Local authorities have suffered spending cuts and social care is, by and large, subject to means testing in contrast to universally free health services. The (delayed) UK governmental Green Paper on social care's long-term future will be as societally important as the NHS Long Term Plan.
By 2035 England's population will have grown by over four million, with a 50% increase in the over 65s, and a quadrupling of those with four or more illnesses. The Royal College of Psychiatrists predicts increasing demand across mental health services, most significantly for cognitive impairment and dementia.3 Those with multi-morbidities particularly risk care-fragmentation, impaired quality of life, and, unsurprisingly, impose considerably greater health costs. Concluding the gloom, there are approximately 100 000 unfilled staff posts in both the NHS and social care, which will double by 2030 given the current trend.
This supply–demand mismatch, which is mirrored internationally, needs greater funding or greater efficiency, one constant refrain being ‘more integrated care’. Existing health models largely evolved top–down tracking professional boundaries, whereas this promises a more logical patient-facing design. The emphasis is on prevention, utilising community resources and self-management, with better care for less money through greater efficiencies.
This idea is hardly new, but gained prominence from the 2014 NHS Five Year Forward View.4 Sustainability and transformation plans/partnerships (STPs) joined NHS trusts, local authorities and clinical commissioning groups to develop ‘place-based’ population plans. STPs are anticipated to evolve into ICSs that will strategically plan, commission and manage services, delivered by ‘integrated care partnerships/providers’ (ICPs) hubbed to primary care population ‘footprints’ of about 80 000. The NHS Long Term Plan has clearly laid out that ‘doing things differently’ via ICSs is the way forward. STPs and ICSs are tasked to develop and implement local 5-year integrative plans by autumn 2019. ICP contracts will be available to commissioners by April 2019, and the expectation is that ICSs will cover the UK by April 2021.
The key challenges
The acronyms are confusing, and there is a lack of clear models and robust evidence. The Royal College of Psychiatrists has expressed concern that mental health has not been sufficiently considered in ICSs, and its amalgamation with overspent acute-sector partners risks cuts to mental health services. Further, we propose there are four major challenges that need to be carefully addressed.
What does ‘integration’ mean?
Details on ICSs and ICPs are intentionally non-prescriptive: encouraging localism and adapting resources to community needs. There have been few examples incorporating mental health; the Royal College of Psychiatrists and the King's Fund noting such opportunities have not yet been maximised.Reference Naylor, Taggart and Charles5 There is an emphasis on co-location of different services, but the logistical aspects of this are enormous: a simple example is the challenge of seamless integration of different computer systems used in health and social care.
A tripartite framework is needed, covering the nature and degree of integration of: the major organisations of health and social care being integrated; the specific amalgamating teams; and support functions such as finances, information technology, etc (see the Appendix). A standardised matrix would permit organisations to both better understand and describe their model, as well as enable comparison between distinct features and performance of different integrative designs.
Which services ‘should’ be integrated?
This speaks to the ‘boundary’ of an integrated system. For example, should it integrate physical and mental health across primary and secondary settings, as well as social care across the whole local authority? Within mental health one might debate integrating working age and older persons’ mental health, child and adolescent services, substance use and so forth. Some services seem to inevitably ‘sit above’, but work into, integrated care hubs – crisis teams, wards, tertiary interventions – but for many others it is less clear. For example, consider early intervention and rehabilitation psychiatry. In one sense, integrating these with physical health services and the local authority offers considerable potential advantages for longer-term health and social inclusion. Conversely, the reason we have separate services is recognition that ‘treatment as usual’ misses out some specific needs, and such patients risk getting lost in a wider system.
Without the baggage of history, would one start with specific groups (for example older adults) or services with other complementarities – in the sense that they share a common infrastructure, or some other way of working together? An economist would pose this through the lens of potential economies of scope/scale – whether it is less costly to provide things separately or together. Currently, we lack criteria and data with which to make such decisions, and most integration will be a compromise between what is considered optimal and what is achievable.
Winning hearts and minds on the frontline
We believe that integration will be won or lost by the engagement of frontline staff. It appeals to most patients and senior managers via the drivers of care and efficiencies, but an effective novel system necessitates working in new ways, not just ‘more closely with others’, with changes in practice that many may find problematic. Existing services have benefits in terms of training, development and peer support; being a smaller part of a bigger and more heterogeneous team poses the risk – speculatively at least – of encouraging generic skill sets at the cost of specialist development, and demoralising an already stretched workforce. It may feel that it is the money driving all change.
One can counter that there will be novel training and practice opportunities in an enriched work environment, and that mental health's biopsychosocial approach is a natural fit for integrative care. In our workforce crisis, new models offer both opportunities and risks.
How will we know if integration is working?
There is a lack of consensus of how we should evaluate change and know if, and for whom, an integrated model is ‘working’. A recent synthesis of measurement tools for integrated health systems identified 114 across 16 domainsReference Suter, Oelke, da Silva Lima, Stiphout, Janke and Witt6 – some agreement for ICSs is required. The Medical Research Council has provided guidance on developing and evaluating complex interventions, but there is a need for consensus in determining causal links between changes at the organisational level, and the processes and outcomes experienced by both patients and the staff.
We need to know whether integration improves clinical outcomes, real-life functioning and satisfaction. Needs vary across patients and there is a risk that ICSs emphasise the complex (and expensive) minority of patients requiring multiple inputs to the detriment of the larger number with ‘simpler’ needs. Indicators could include qualitative data, patient and clinician reported outcome measurements, and patient activation measurements that ask individuals how able they feel to manage their health. However, we lack consensus on which tools to use (including their fitness to describe outcomes in a new model), and, typically, no good ‘before’ data. At a ‘high end’ or top of a causal chain, one might explore strategic objectives such as changing suicide rates, life expectancy and employment, although these have the various challenges of (relatively) small numbers and slow change.
With complex organisational changes it is important to track effects on quality, volumes and costs, including the costs of changing the system. There are a range of existing key performance indicators from referral waits, through planned versus unplanned admissions, to delayed transfer of care; from cardiometabolic assessments to flu vaccinations; from complaints to patient experience data and so forth.
There is an absence, to the best of our knowledge, of a healthcare ‘staff activation measurement’, although demonstrating change in professionals’ perceptions of their abilities to manage care is appealing. Qualitative work might again be valuable in identifying appropriate elements of an integration scale and experiences of working in ICSs, as well as the proxy measures of staff and trainee recruitment, satisfaction, sickness and retention.
Next steps
‘Integrated care’, as a broad concept, appeals as a seemingly reasoned way for health and social services to deliver better care and manage the wider financial reality. One only has to look at physical health outcomes in those with psychosis, or the links between depression and many chronic health problems and social disadvantage to see the need to do things differently. However, it is determining the underlying detail of what this means that remains crucial, not least what ‘integration’ really means.
Integrating organisations need frameworks and tools to describe their integration model – and how it will be evaluated. Engaging staff and patients is essential to the process, and a necessary starting point for developing methodologies to evaluate organisational changes and outcomes. Appraising the outcomes of these models, both good and bad, will be necessary to inform rapid and transparent dissemination and scale-up decisions.
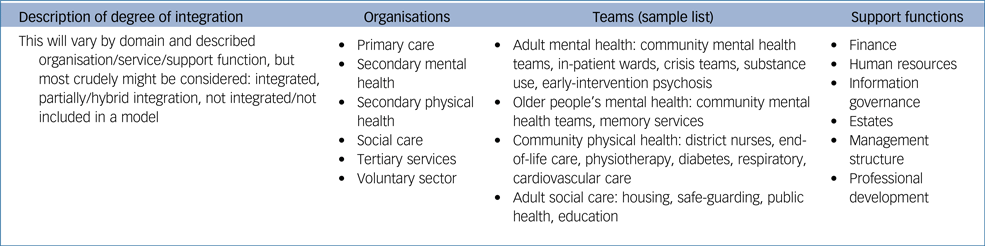
Appendix
An overview of the areas that should be considered by integrating services






eLetters
No eLetters have been published for this article.