The increasing prevalence( 1 , Reference Wang and Lobstein 2 ) and economic burden( Reference Wang, McPherson and Marsh 3 ) of childhood obesity in the UK, and elsewhere, have led to the UK Government’s decision to introduce policies to improve the quality of children’s diets. Research in this area has identified important dietary risk factors for obesity, which include a high proportion of energy-dense foods high in fats and sugars as well as large intakes of sugar-sweetened beverages( 1 , Reference Mendoza, Drewnowski and Cheadle 4 , Reference Malik, Schulze and Hu 5 ). In addition, low consumption of fruits and vegetables and fibre is strongly associated with a range of important health outcomes in adults including CVD and some cancers( Reference Mente, de Koning and Shannon 6 – Reference Crowe, Roddam and Key 8 ). This has resulted in a number of Western countries, including the UK, focusing on improvements in school food and introducing school meal standards( Reference Briefel, Crepinsek and Cabili 9 , Reference Harper, Wood and Mitchelle 10 ). Further changes were introduced in 2014 when free school meals were made available to all young schoolchildren (aged 4–7 years) in England( 11 ).
Food- and nutrient-based standards were introduced by law into primary schools in England between September 2006 and 2008( 12 , 13 ), and were based on recommendations from the School Meal Review Panel formed in 2005( 14 ). Before these standards, school meals had not been regulated for many years in the UK, although the Caroline Walker Trust provided recommendations in 2001 for schools to follow voluntarily( Reference Evans and Harper 15 , Reference Crawley 16 ). Information on how to implement the standards was consequently provided for schools by the School Food Trust. Nutrient-based standards included minimum or maximum standards for a school meal (averaged over a menu cycle, commonly one to three weeks) for thirteen nutrients and energy (energy alone had both a minimum and maximum recommended level)( Reference School Food 17 ). In addition to the nutrient-based standards, a number of foods were restricted such as low-quality meat, savoury snacks and confectionery products in order to exclude foods high in Na, saturated fats and sugars( Reference School Food 18 ). More nutritious foods such as fruit and vegetables and bread without spreads were made part of every school meal. When first introduced, the standards were enforced by Ofsted which inspects schools periodically; however, since the change of government in 2010, further amendments were made to the law and schools’ compliance to the standards is no longer formally assessed( 19 ).
Cross-sectional studies carried out by the School Food Trust indicate that the quality of school meals has improved since the introduction of the school meal standards, both in primary schools( Reference Golley, Pearce and Nelson 20 ) and secondary schools( Reference Pearce, Wood and Nelson 21 ). School meals are now higher in vegetables and lower in sugars and Na than they were in the past. Analysis of the Low Income Diet and Nutrition Survey( 22 ) by Stevens and Nelson( Reference Stevens and Nelson 23 ) reported that children who had a packed lunch had higher daily intakes of total fat, saturated fat and Na at lunchtime than children having a free school meal among the population of low-income children. A separate study of packed lunches only also found that sugars, saturated fat and Na were particularly high in children’s packed lunches( Reference Evans, Greenwood and Thomas 24 ). Although there is strong evidence that school meals have improved lunchtime intake for children, it is necessary to determine the impact of meal type on children’s diets over the whole day to determine whether differences at lunchtime are maintained over the rest of the day. There are few published studies comparing the nutritional intake over the whole day by school meal type that have collected data after the introduction of the school meal standards in 2006. Evans et al. reviewed cross-sectional studies comparing daily intake by school meal type carried out before the introduction of standards( Reference Evans, Cleghorn and Greenwood 25 ) and concluded that even before the improvements in school meals, packed lunches were less healthy in terms of sugars, fats and Na. A recent study on older primary-school children aged 9–10 years, published since the review and looking at consumption of specific foods by meal type, reported that children having packed lunches had more savoury snacks and importantly that lunchtime intake makes a significant contribution to overall dietary intake( Reference Harrison, Jennings and Jones 26 ).
Approximately half of primary-school children bring a packed lunch from home( 27 ) and this has remained stable in the last few years( Reference Harrison, Jennings and Jones 26 ). The quality of packed lunches therefore remains a concern, and it is important that information on both packed lunches and school meals is collected periodically in order to assess the impact of policy changes affecting school lunches( Reference Rees, Richards and Gregory 28 ). The present study uses data collected from a large number of primary-school children across England to determine the effect of meal type on important nutrients over the whole day, as well as the consumption of common children’s foods.
Methods
Study design
Data were collected in 2007 from 2709 children attending fifty-four primary schools randomly selected from all state schools across England. One class from Year 2 was randomly sampled from each school. The schools reflected a wide range of social classes and ethnic backgrounds. The data analysed here are part of a cluster-randomised controlled trial and further details on sampling procedures are provided in the published trial protocol( Reference Kitchen, Ransley and Greenwood 29 ). Power calculations were based on identifying differences in daily fruit and vegetable consumption of 0·5 portions with power of 80 % and significance level of P<0·05.
Dietary data were collected using the Child and Diet Evaluation Tool (CADET), which has previously been validated in a similar age group( Reference Cade, Frear and Greenwood 30 ). CADET is a paper-based, 24 h estimated food diary with foods separated into different categories and times of the day. During the school day the trained administrators completed the diary for each child. After school, parents recorded all foods their child ate during the day by ticking the foods their child consumed at each meal or snack time. CADET uses sex- and age-appropriate portion sizes for each food category that are estimated using results on portions from the children’s National Diet and Nutrition Survey (NDNS)( Reference Gregory, Lowe and Bates 31 ). In addition to dietary data, personal information was requested including sex, education level of parents, ethnicity and postcode (on which the Index of Multiple Deprivation (IMD) was estimated) and information on aspects of diet including school meal type. This tool was chosen for being one of the few valid but simple tools that accurately reflects the diet of children.
A selection of nutrients was analysed to determine whether there was a difference in daily nutrient intakes between school meals and packed lunches. These included energy (kJ/d and kcal/d), total and saturated fat (g/d), carbohydrate (g/d), starch (g), total sugar (g/d), protein (g/d), fibre (NSP; g/d), Ca (mg/d), Fe (mg/d), Zn (mg/d), folate (mg/d), vitamin A (µg/d), vitamin C (mg/d) and Na (mg/d). These nutrients were chosen because they are included in the nutrient standards for school meals.
A range of foods was analysed to determine differences in consumption by food type. The CADET diary contains 117 food groups; however, this included individual fruits and vegetables. Vegetables were categorised into five groups: dark green, red and orange, legumes, starchy and other. Fruits were categorised into two groups: fresh or frozen (combined) or dried. After combining fruit and vegetable types there were eighty-five food groups in total. Foods consumed by at least 10 % of children are reported in the tables for ease of use.
Statistical analysis
All statistical analyses were carried out using the statistical software package STATA version 11·0 (2010). In order to compare nutrient intakes, multilevel regression modelling was used to take into account the clustering effect of children within schools. The variation in nutrients between children in a school having the same school meal may be smaller than the variation for all children and therefore multilevel regression is required. A separate regression model was performed for each nutrient. The normality of the variables was checked by generating histograms and inspecting the mean value in comparison with the standard deviation. Variables showing a skewed distribution were transformed to the natural logarithm before carrying out any statistical tests. Model fit was checked by inspecting histograms of the residuals. Results were displayed unadjusted for all children (model 1) and adjusted for age, sex, IMD in quartiles and ethnicity (model 2).
The percentage and 95 % confidence interval of children consuming each food were calculated, as well as the percentage by each lunch type. In order to test whether children having a packed lunch were more or less likely to consume a certain food or drink, logistic regression was used to generate the odd ratios of consuming each food compared with children having a school meal; 95 % confidence intervals and P values were also generated. For each food, two models are presented: model 1, which was adjusted for clustering of children within schools only, and model 2, a fully adjusted model adjusting for age, sex, IMD quartiles and ethnicity.
Children were excluded from the analysis if they had an energy intake value above 16 736 kJ/d (4000 kcal/d). If there was no information on school meal type children were excluded from the regression models but were included in the descriptive analysis. These children were compared with children having school meals and packed lunches to assess any potential response bias.
Results
Dietary data were collected from 2709 children. Thirty-seven children were excluded because of unfeasibly high daily energy intake of more than 16 736 kJ (4000 kcal), leaving 2672 children in the preliminary analysis. Background descriptive information on the total group and boys and girls is provided in Table 1. The children in the present study had BMI values similar to those in national data collected by the Health Survey for England for this age group( 32 ). There were no obvious differences between sexes in terms of anthropometric measures.
Table 1 Characteristics of children aged 6–8 years and primary schools included in the analysis, England, 2007. Figures are not adjusted for clustering within schools
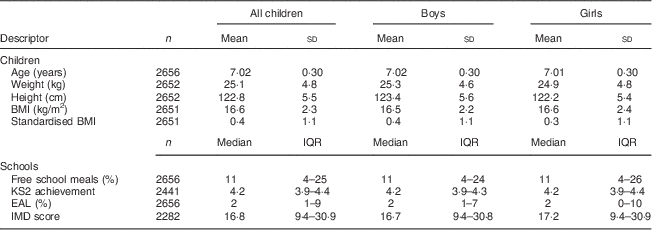
KS2, Key Stage 2 level (target is KS4 for all students by age 11 years); EAL, English as a second language; IMD, Index of Multiple Deprivation; IQR, interquartile range.
Information on school lunch type was available from 2373 children; however, this information was missing from 299 (11 %) of children. The number of boys and girls was similar, with 50 % of the total sample being boys. The proportion of boys and girls having a school meal, where information on meal type was available, was similar; 44 % of boys had a school meal and 45 % of girls had a school meal, with the remaining children reporting taking a packed lunch. Some of the children with missing lunch information may have gone home for lunch. The results from the total sample of 2373 children indicated that anthropometric measures were similar in both groups of children: those having school meals and those having packed lunches.
Adjusting only for clustering within schools and no other factors, daily energy intake for boys and girls combined was similar for those having a school meal or a packed lunch. However, daily intake of some nutrients was different when comparing school meal type. Vitamin A and vitamin C were log-transformed for analysis as they were not normally distributed. Children having a school meal had higher mean daily intakes of protein, fibre (NSP) and Zn (see Table 2). Conversely, mean daily intakes of carbohydrate, total sugars and Na were all higher in children taking a packed lunch to school. The results for boys and girls separately were broadly similar to the results from all children (data not shown). The adjusted models included fewer children due to missing data on ethnicity and IMD (see Table 2). Differences in daily nutrient intakes between meal type broadly remained the same in these models and were not attenuated for most nutrients. In the fully adjusted models children having school meals consumed higher amounts of protein, fibre and Zn and lower levels of total sugars and Na, as was seen in the unadjusted models. In addition, daily folate consumption was also significantly higher in children having a school meal. These results were similar for boys and girls separately (data not shown).
Table 2 Mean values (and standard errors) for anthropometric measures and daily nutrient intakes of children aged 6–8 years by school lunch type, adjusted for clustering within schools only (model 1) and fully adjusted (model 2) for age, sex, ethnicity and Index of Multiple DeprivationFootnote *, England, 2007. Results are for school meals compared with packed lunches
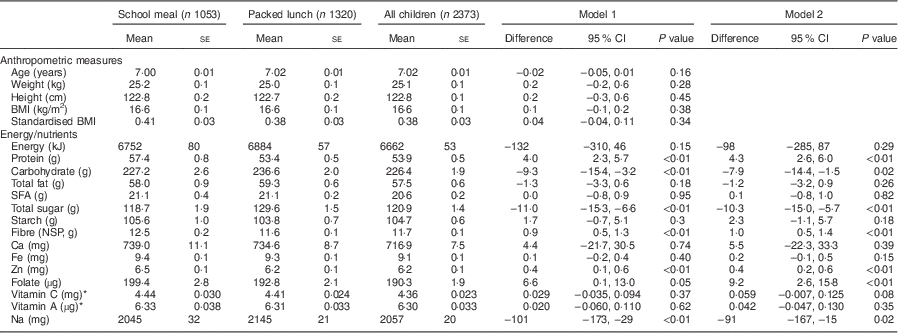
* Calculated using natural logarithm.
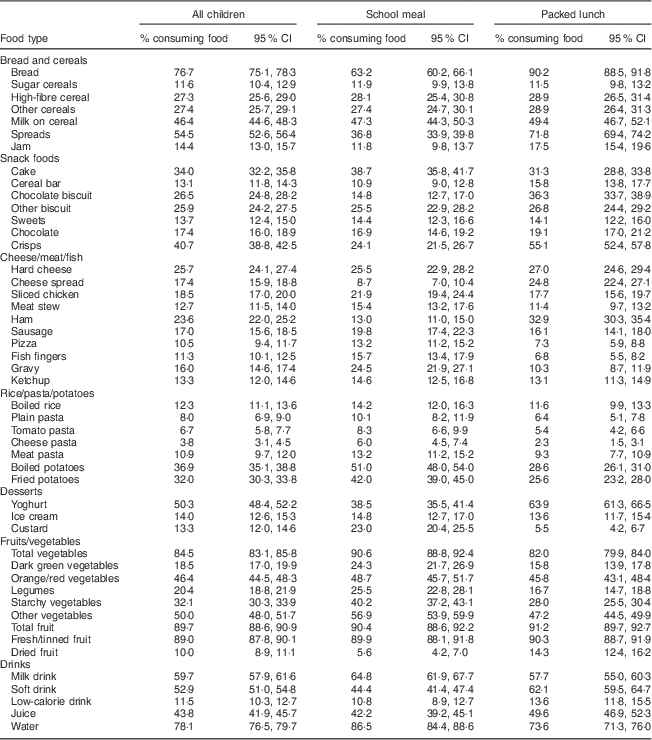
Frequencies of consumption for all children, children having a school meal and children having a packed lunch were generated for all of the food groups from the CADET assessment tool. The results showed thirty-three foods were consumed by less than 10 % of the sample and were excluded from further analysis. The frequencies and 95 % confidence intervals are displayed in Table 3 for the forty-seven remaining foods plus total vegetables and total fruit. The most commonly consumed foods in this group of children were bread, spreads, milk, yoghurts, crisps (potato chips), vegetables and potatoes. The most common drinks were sweetened drinks and juices.
Table 3 Percentage of children (and 95 % confidence interval) consuming each food type for all children aged 6–8 years (n 2672), children having a school meal (n 1053) and children having a packed lunch (n 1320), for foods consumed by more than 10 % of all children, England, 2007
Odds ratios calculated for each food indicated that there were many foods that were more likely to be consumed (over the whole day) by children having a school meal; and other foods that were more likely to be consumed (over the whole day) by children having a packed lunch (Table 4). The most popular foods more likely to be consumed by children having a packed lunch included bread, spreads, ham, cheese spread, crisps, jam, yoghurt, chocolate biscuits, cake, cereal bars and dried fruit. Popular foods more likely to be consumed by children having a school meal included hot foods such as all types of vegetables, including dark green vegetables and legumes, pasta, stew, fish fingers, pizza, sausages, rice, potatoes, gravy and custard. Children having a packed lunch were more likely to have sweetened drinks and fruit juice over the whole day while children having a school meal were more likely to drink water during the day.
Table 4 Probability of consuming each food type (odds ratios, 95 % confidence intervals and P values) for children aged 6–8 years having a school meal compared with children having a packed lunch, England, 2007
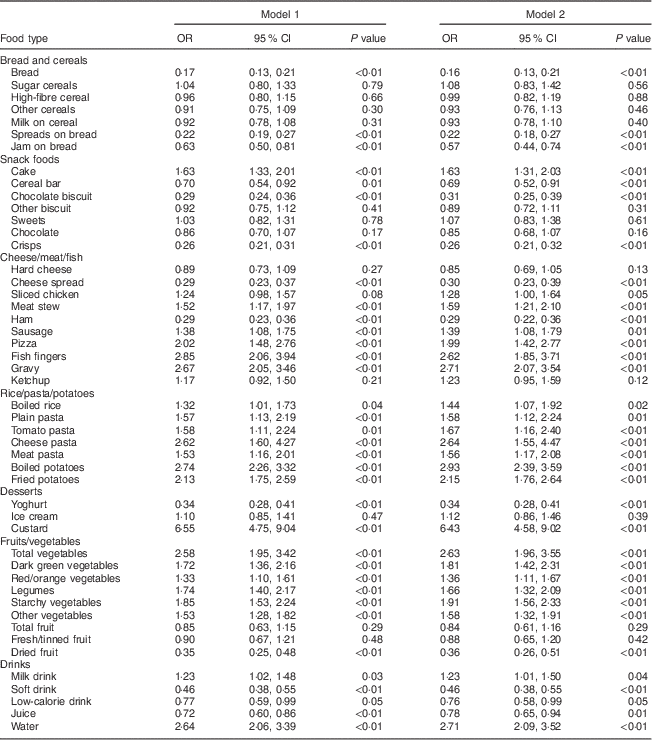
IMD, Index of Multiple Deprivation.
Model 1 (n 2373) is adjusted for clustering within schools only and model 2 (n 2172) is the fully adjusted model adjusted for age, sex, ethnicity and IMD quartiles in addition to clustering within schools.
Discussion
This large survey of children across England investigated differences in daily consumption of important nutrients and foods, by school meal type consumed at lunchtime. The results suggest that children having a school meal consume a healthier diet over the whole day compared with children who take a packed lunch to school. Children having a school meal, on average, consumed lower levels of total sugars and Na and higher levels of protein, fibre, Zn and folate over the whole day. The differences were in the region of 5 to 10 % for all nutrients. Children having a school meal were more likely to have all types of vegetables and drink water during the day; and were less likely to consume sweet and savoury snacks and sweetened drinks. These differences in foods consumed explain why sugar and Na consumption was lower and Zn, folate and fibre intakes were higher in children who had a school meal. There were no appreciable differences in energy, total fat or saturated fat intakes over the whole day between meal types.
The data for the study were collected in the same year the food standards for school meals were introduced into primary schools. The changes may not have been fully implemented in all schools; however, it was expected that if there was no improvement in packed lunches but an improvement in school meals the gap may have widened compared with data from before 2006. A review of surveys carried out between 1990 and 2007( Reference Evans, Cleghorn and Greenwood 25 ) reported that daily energy and saturated fat intakes were higher if children had a packed lunch. However, we did not see a difference in these nutrients. This may be because food companies have made efforts to reduce saturated fat from snack foods such as crisps (potato chips) in recent years and these improvements have affected packed lunches more than school meals.
The review of studies carried out between 1990 and 2007 broadly concurred with the results from the present study regarding Na and sugar intakes. The children having packed lunches in the present study had, on average, equivalent to an extra two teaspoons (10 g) of sugar per day compared with those having a school meal. This equates to about a 10 % difference in sugar consumption over the day for an average child. The higher sugar intake of children having a packed lunch reflects the higher consumption of biscuits, yoghurts, cakes and sweetened drinks in these lunches, which has also been reported in other surveys( Reference Evans, Greenwood and Thomas 24 , Reference Rogers, Ness and Hebditch 33 , Reference Rees, Richards and Gregory 34 ). The difference in Na consumption between meal types reported in the present study is about 100 mg, a smaller difference compared with the review of studies before 2007. This attenuated difference could be due to lowered Na content of key lunchtime foods such as bread and crisps (potato chips). The food composition data were updated prior to the current analysis to reflect lower Na levels of these foods. However, the lower Na intake by children having a school meal reflects the persistent difference in dietary pattern with more meat, potatoes, gravy and vegetables consumed by children having a school meal and more bread, spreads, ham, cheese spread and crisps by children having a packed lunch.
Previous research studies looking at lunchtime intake rather than intake over the whole day generally reported larger differences in nutrient intake by lunch type compared with whole day intake. A survey of more than 10 000 primary-school children carried out by the School Food Trust in 2009( Reference Stevens and Nelson 36 ) reported differences by lunch type in many of the same nutrients that were found in the present study. We have shown that the differences in lunchtime intake of some nutrients persist over the whole day but this was not the case for all nutrients. The School Food Trust reported higher levels of total fat and saturated fat and Ca in packed lunches which we did not see in our analysis of intake over the whole day. This indicates that there may be some compensation during the rest of the day outside school for some nutrients but not others. Stevens and Nelson analysed nutrient intake from school meals and packed lunches from the Low Income Diet and Nutrition Survey over both lunchtime and the whole day, and found that although there were differences in lunchtime intake by meal type these differences rarely persisted over the whole day( Reference Stevens and Nelson 36 ). This may have been because the sample size was smaller than our analysis and therefore the study was not powered to see more modest differences. However, a previous study investigating differences in intake by lunch type in younger children aged 4–6 years reported similar findings to this research( Reference Spence, Delve and Stamp 37 ).
In the case of Fe, few differences were seen between the two types of lunch on whole day intake. In the previous review( Reference Evans, Cleghorn and Greenwood 25 ), a higher content of Fe in packed lunches was reported which may have been due to the financial restrictions of providing red meat in school meals. Compared with the recommended nutrient intake for Fe for this age group, both groups were on average consuming adequate amounts of Fe.
Compared with the recommended nutrient intakes set by the Department of Health, mean intakes of starch, fibre and Zn were lower than recommended for the whole sample and Na and sugar intakes were higher than recommended. The long-term improved health impact of a decrease in the region of 10 % in key nutrients such as sugars and Na is not clear, as the majority of the evidence available on diet and health outcomes is from research on adults not children. There is little published evidence that children who have a packed lunch are more likely to be overweight or obese or have worse health markers. Indeed, we saw no difference in daily energy intake by lunchtime meal type in the current large study. However, a study in London on markers of CVD and type 2 diabetes mellitus risk by Whincup et al. reported that adolescents having school meals had significantly lower systolic blood pressure and fasting insulin levels( Reference Whincup, Owen and Sattar 38 ), which may be linked to our results in terms of sugar and Na consumption. A US school-based study reported improvements in blood lipid profiles with the introduction of a healthier school lunch lower in total and saturated fat( Reference Arbeit, Johnson and Mott 39 ), providing some evidence of the potential importance of lunchtime meals on children’s long-term health.
There are notable strengths of the current study. It included a large number of children in more than fifty schools across the whole of England. The children were representative of the region with broadly similar levels of deprivation to the national average( 40 ) and a similar proportion of children having a school meal compared with the national average of 45 % at this time( Reference Nicholas, Wood and Nelson 41 ). Compared with the NDNS, intakes were generally higher in our survey, probably due to the difference in dietary assessment methodology( Reference Cade, Thompson and Burley 42 ). Compared with the original NDNS carried out in 1997 in the UK, daily intake was higher in energy and all nutrients with the exception of Na in our study. A further strength was the advanced statistical methods applied to these data. Multilevel regression analysis was used that took into consideration the similarity of pupils clustered within schools, and furthermore results were reported as unadjusted and adjusted for social factors. Results were similar for both models, indicating that age, sex, ethnicity and deprivation were broadly similar in both groups.
There are limitations to the study that need to be highlighted. The study is based on a cross-sectional, self-reported, one-day food diary that uses estimated portion sizes based on age and sex. This may lead to unreliable reporting of energy and nutrient intakes. The difficulties of accurately measuring dietary intake are well established( Reference Cade, Thompson and Burley 42 ). Some of the parents did not complete the non-diet data and therefore the adjusted models included fewer children, which could result in bias.
In summary, half of families in England choose to send their child to school with a packed lunch and children having a packed lunch generally consume a less healthy diet over the whole day, higher in sugars and Na and lower in fibre and Zn, even after adjusting for IMD and ethnicity. Sweet snack foods and drinks and savoury snacks are more commonly consumed by children having a packed lunch, findings which are consistent with previous studies. In order to improve children’s diets we recommend that policies are implemented that increase the proportion of schoolchildren of all ages having a school meal. The cost of school meals may be an important reason why more families do not choose a school meal and historical data indicate that as the cost of school meals increases, uptake decreases( Reference Evans and Cade 43 ). Potentially successful policies may include increasing the number of children eligible for a free school meal or subsidising the cost of school meals. The current UK government has recently introduced free school meals for all 4- to 7-year-olds in England at a cost of £600 million per year. We further suggest that high-quality prospective studies are carried out to determine the benefits of school meals to children on markers of health such as blood pressure and blood sugars in order to quantify the health benefits by school lunch type.
Acknowledgements
Acknowledgements: The authors thank the schools and children for their involvement in the project. Financial support: The current analysis was funded by the University of Leeds and received no specific grant from any funding agency in the public, commercial or not-for-profit sectors. The project was originally commissioned by the Medical Research Council (MRC) National Prevention Research Initiative (NPRI) (MRC registry code G0501297). The views and opinions expressed herein are those of the authors and do not necessarily reflect those of the NPRI programme or the MRC. Conflict of interest: C.E.L.E., V.M., M.S.C. and J.E.C. have no further financial support, no other relationships with companies that might have an interest in the submitted work and no non-financial interests that may be relevant to the submitted work. Authorship: C.E.L.E. and V.S.M. designed the research protocol and statistical analysis plan. V.S.M. and C.E.L.E. wrote the first manuscript, carried out the analysis and contributed to all versions of the manuscript. J.E.C. secured the funding for the original project and contributed to all versions of the manuscript. M.S.C. managed the data collection of the NPRI project and contributed to the final version of the manuscript. Ethics of human subject participation: This study was approved by the University of Leeds Ethics Committee. The trial registry code is G0501297.









