Nutrient deficiencies and stunting are among the primary childhood health concerns in developing countries( 1 ). As low- and middle-income countries undergo the nutrition transition, these populations experience increases in overweight, obesity and associated non-communicable disease simultaneously with persistent undernutrition. Children are among the most vulnerable to the dual burden of malnutrition. Efforts to prevent this emerging epidemic in the early stages are critical.
The nutrition transition is defined as a shift from high prevalence of undernutrition and its related health consequences to increasing predominance of diet-related non-communicable disease( Reference Popkin 2 , Reference Rivera, Barquera and González-Cossío 3 ). Nutrition transition and related increases in the prevalence of obesity are largely driven by rapid urbanization and globalization processes that result from technology distribution, transportation, marketing, mass media, and flow of capital and services( Reference Popkin, Adair and Ng 4 ). Although these changes bring about benefits, such as improved food access, they also result in an abundance of inexpensive, processed, high-energy and high-sodium items in the countries’ food environments, as well as increased sedentary time, which lead to rises in obesity( Reference Popkin, Adair and Ng 4 ). Childhood obesity is a serious public health problem which tracks into adulthood and leads to increased morbidity and mortality later in life( Reference Serdula, Ivery and Coates 5 – Reference Daniels 8 ), with increased risk faced by children who experience early undernutrition followed by rapid weight gain in childhood or adolescence( Reference Victora, Adair and Fall 9 ). Globally, obesity has more than doubled in the last 35 years( 10 , 11 ). Among school-aged children (5–19 years) in low- and middle-income countries, the global prevalence of overweight and obesity is 10 %, but varies widely between countries depending on their stage in the nutrition transition( Reference Gupta, Goel and Shah 12 ).
Haiti is a country at an early stage of nutrition transition. It has experienced gross domestic product increases following the disruption from the 2010 earthquake( 13 ), increased urbanization, increased vaccination rates, and decreases in child undernutrition and morbidity( Reference Cayemittes, Busangu and Bizimana 14 , Reference Cayemittes, Placide and Mariko 15 ). Haiti is also experiencing an increasing prevalence of overweight and obesity among women, particularly in urban areas and higher socio-economic status groups( Reference Cayemittes, Busangu and Bizimana 14 , Reference Cayemittes, Placide and Mariko 15 ), and decreasing national supply of fruits and vegetables( 16 ). Haiti’s age-standardized overweight prevalence in children (7·7 % of boys, 9·5 % of girls) is still well below the average for the Caribbean region (13·4 % of boys, 19·9 % of girls) and the prevalence in other culturally and economically similar countries, such as the Dominican Republic, Cuba and Brazil( Reference Ng, Fleming and Robinson 17 ). In fact, Haiti’s childhood overweight prevalence is closer to the 1980 estimate for the world’s developing countries (8·1 % of boys, 8·4 % of girls), indicating that Haiti is just at the beginning of the nutrition transition( Reference Ng, Fleming and Robinson 17 ).
Predictors of childhood obesity are well characterized. These include high consumption of energy-dense foods and low consumption of fibre, fruits and vegetables, and other nutrient-rich foods; decreased physical activity; and obesogenic food and physical activity environments( Reference Gupta, Goel and Shah 12 , Reference Popkin 18 – Reference Swinburn, Sacks and Hall 21 ). However, in the developing world, most nutrition transition research has been carried out in countries that are experiencing higher obesity rates (e.g. India, Mexico, South Africa) than the rest of the low- and middle-income countries( Reference Popkin, Adair and Ng 4 ). This dearth of research in early transitioning countries means that there is a missed opportunity for prevention of the rise in childhood obesity associated with nutrition transition. Haiti is a novel setting for characterization of factors associated with obesity, which would inform the initiation and study of efforts to adapt and implement evidence-based obesity prevention interventions, with the aim of disrupting the negative consequences of the nutrition transition. We hypothesize that, being early in the nutrition transition, overweight and obesity in Haiti will be associated with a higher consumption of processed and high-energy foods (e.g. animal fat); lower consumption of fruits, vegetables and other sources of fibre; and higher socio-economic status( Reference Popkin 22 ).
From 2012 to 2013, the Mamba School Feeding study (the Mamba study) was carried out among school-aged children in Cap-Haitien, Haiti, to examine the effects of a fortified snack on nutrition outcomes. The present study used baseline data of that study to accomplish two aims. The primary aim was to examine the association of socio-economic factors and diet with overweight (including obesity) in this population. In order to begin to contextualize the school environment, the present study’s secondary aim was to describe food availability and the physical activity built environment in the participating schools.
Methods
Design and study participants
The sample was comprised of the Mamba study baseline data. The design and methods of the Mamba study have previously been described in detail( Reference Iannotti, Henretty and Delnatus 23 ). Briefly, the study was a group-randomized controlled trial carried out in six primary schools in Cap-Haitien, the second largest city in Haiti, during the 2012/13 school year. Two schools were assigned to each of three conditions: (i) fortified food provided as part of the school’s feeding programme; (ii) unfortified food provided as part of the school’s feeding programme; and (iii) no snack provided (comparison group). Children were included in the study if they: (i) were 3–13 years old; (ii) had no siblings enrolled in the study; (iii) were in good health (e.g. absence of fever, congenital health condition); (iv) were not severely malnourished (i.e. weight-for-height Z-score less than −2); (v) did not have a peanut or soya allergy; and (iv) were enrolled in a participating school for the 2012/13 school year.
Contacts were made with all families of eligible children, and parents or non-parent caregivers of all but two eligible children agreed to participate. Written informed consent was obtained from parents or non-parent caregivers of the children in French and Creole, and verbal assent was obtained from children. Longitudinal measures were taken at baseline (December 2012 to January 2013), midline (March 2013) and endline (June 2013). Children were assessed for weight and height, blood Hb concentration, body composition via bioelectrical impedance, educational outcomes and acceptability of the school snack if given. Additional information regarding socio-economic and demographic characteristics, child diet and health, and parent anthropometry was collected from children’s parents or non-parent caregivers.
The present study used the baseline data from the Mamba study (n 1084), because these data were not influenced by the Mamba intervention. After children with missing values for BMI were removed, data on 968 participants remained and were used in the analysis.
Measures
Anthropometric measures of the children and caregivers were performed by trained study personnel( Reference Iannotti, Henretty and Delnatus 23 ). Weight was measured to the nearest 0·1 kg using a Seca model 874 (digital) scale (440 lb×0·1 lb resolution (~200 kg×~45 g resolution)). Height was measured to the nearest 1 mm using the ShorrBoard measuring board. For children’s height and weight, two independent measures were taken, with a third measure taken if the difference between the first measures was outside the acceptable range. The averages of the height and weight measures were used to calculate BMI Z-scores using the WHO Growth Standards for children 3–5 years of age( 24 ) and WHO Growth References for children 6–13 years of age( 25 ). Child overweight was defined as BMI Z-score greater than +1 and includes obese children. A dichotomous variable for child overweight (0=normal or underweight, 1=overweight or obese) was used in analyses.
Dietary, child morbidity, socio-economic and demographic variables were assessed using the caregiver interview. Children’s dietary intake was assessed using the 24 h FFQ from the Demographic and Health Surveys Program that is used to measure dietary intake in low- and middle-income countries around the world( 26 ). The questionnaire was adapted to the Haiti context based on formative research to reflect foods commonly consumed by the target population. Caregivers were asked how many times the child ate the following food items in the previous 24 h: bread; cereals, porridge or other grains; roots and tubers; beans and other legumes; eggs; milk; fermented milk or yoghurt; cheese and other dairy products; poultry; other meat; fish and shellfish; fruits; vegetables; oils, butter and other fats; crackers; and cookies.
These food items were also combined into food groups based on their energy and nutrient density( Reference Drewnowski 27 ) and standardly applied food categories: fruits and vegetables; meat, fish, dairy and eggs; processed foods; and starchy foods. In addition, two approaches were used to characterize other aspects of the diet. First, the dietary diversity score( Reference Swindale and Bilinsky 28 ) was calculated to represent overall diet quality. Second, dietary patterns were derived using principal components analysis by grouping food items to reflect patterns of dietary intake.
To measure food purchasing at school, caregivers were asked how often the child buys a snack or lunch at school, with the possible answer options being ‘always’, ‘sometimes’ or ‘never’. Other measures of socio-economic status included mother’s education level (years), household monthly income (100–500, 501–800, 801–1000, 1001+ Haitian dollars), amount the household spent on food yesterday (0–20, 21–40, 41–60, 60+ Haitian dollars), whether the household receives remittances (yes, no), number of people living in the household, frequency of electricity availability in the home (always, sometimes, never), whether the household has a flush toilet (yes, no) and whether the household shares a toilet with other households (yes, no).
Child age, morbidity, micronutrient supplementation and mother’s BMI were captured and used as potential covariates. Child age (years) was measured at baseline using the child’s birthday and the date of survey administration. Caregivers were asked to recall whether the child had diarrhoea or fever in the past 2 weeks and whether the child had received vitamin A supplementation or deworming tablets in the past 6 months. Mother’s BMI was measured by trained study personnel using research grade equipment. Averages of independent measures of height and weight were used to calculate BMI, defined as weight divided by height squared.
To examine food availability and the physical activity built environment in participating schools, structured observations and interviews with school personnel were carried out. School personnel provided information regarding school policy for the length of physical activity and recreation time (min/d). The size (m2) and density (m2/student) of the outdoor space and availability of shade and green space (yes, no) were collected through direct observation and measurement of school grounds. Study team members collected exact measures of the dimensions of outdoor space at each school. These measures were then converted to density by dividing by the total student population. Food availability was defined as the presence of foods obtainable from food vendors on school grounds or in the immediate area. Study personnel carried out an inventory of food items being sold at each school. In addition, school hours of operation and the presence of electricity, latrines and water pumps were collected as descriptive characteristics of the schools.
Data analysis
Differences in participant characteristics and dietary intake between overweight (including obese) and non-overweight children were examined using Pearson’s χ 2 and Fisher’s exact test for categorical variables, and the Wilcoxon rank sum test for continuous variables, as these were not normally distributed.
Logistic regression was used to examine the association between potential predictors of overweight and child overweight status. Potential predictors of overweight were entered into the model as follows, and they were retained if they significantly predicted overweight or improved model fit based on the Akaike information criterion and −2 log likelihood statistics, while retaining model quality. Child age and sex were entered into the model first. As the relationship between child age and the dependent variable was not linear, a polynomial term for age (age squared) was added to improve model fit. Socio-economic status variables were entered next, followed by child health variables (i.e. diarrhoea or fever morbidities, vitamin A supplementation and deworming), dietary intake variables and finally mother’s BMI. In each model, the Hosmer–Lemeshow test and the c statistic were used to evaluate the quality of the model (whether the model was significantly different from the data)( Reference Hosmer and Lemeshow 29 ). Multicollinearity was examined using variance inflation factors( Reference Myers 30 ). The final model included: the constant, child’s sex, child’s age, child’s age squared, whether child purchases food at school, whether the household owns a bicycle, child’s consumption of meat (excluding fish), child’s consumption of dairy and eggs, child’s consumption of fish and mother’s BMI. Odds ratios of overweight across predictor levels and their confidence intervals were calculated to examine the association.
As a sensitivity analysis, dietary patterns were derived and along with the dietary diversity score considered for inclusion in the logistic regression models to examine the association of overall diet with child overweight. The dietary patterns were derived using principal components analysis using previously described methods( Reference Newby and Tucker 31 ). Six dietary patterns were extracted based on the eigenvalue greater than 1 cut-off point, and two dietary patterns were extracted using the scree test. The patterns were rotated using the orthogonal Varimax rotation method, which loads the food items maximally on to one dietary pattern while keeping the patterns independent, thus improving interpretability( Reference Field and Miles 32 ). The dietary diversity score and dietary patterns were included in the logistic regression model-building described above, but none were significantly predictive of overweight independently of individual food groups, nor did they improve the model fit. Therefore, they were not included in the final model.
All analyses were conducted using the statistical software package SAS version 9.4.
Results
Study characteristics
Overweight children (including obese) and non-overweight children did not differ statistically by child characteristics (Table 1). Mothers of overweight children showed a significantly higher BMI than mothers of non-overweight children. As well, a significantly lower proportion of overweight child households shared a toilet with other households than did non-overweight child households. Other maternal and household health and socio-economic characteristics did not differ by group.
Table 1 Socio-economic and demographic characteristics by overweight status among children (n 968) from six primary schools in Cap-Haitien, Haiti, 2012/13 school year

† Non-overweight is defined as children with a BMI Z-score less than or equal to +1.
‡ Overweight is defined as children with a BMI Z-score greater than +1 and includes obese children.
§ 185 observations are missing from the mother’s BMI variable.
|| 212 observations are missing from the mother’s education variable.
The prevalence of children who were overweight or obese was 5·1 % in the present study. Obesity-only prevalence was 1·8 %. Similar prevalence of overweight was observed among girls (5·6 %) and boys (4·5 %). Significant differences in overweight, however, were observed by age group with the youngest (3–5 years old) and oldest (12–13 years old) children experiencing higher overweight rates than the other children.
Bivariate analysis of dietary intake
Few significant differences were observed in bivariate analyses of individual food items and food groups by overweight status. The overweight children had a significantly lower (−0·11) mean frequency of fish intake than non-overweight children (data not shown).
Association between child overweight and socio-economic and diet factors
The final logistic regression model of overweight status (Table 2) satisfied the convergence criteria and was significant (likelihood ratio (df=10)=36, P<0·0001). The Hosmer and Lemeshow goodness-of-fit statistic (H-L (df=8, n 778)=7·70, P=0·463) and the c statistic (0·721) indicated acceptable quality of the model.
Table 2 Logistic regression modelFootnote † predicting overweight statusFootnote ‡ among children (n 778) from six primary schools in Cap-Haitien, Haiti, 2012/13 school year
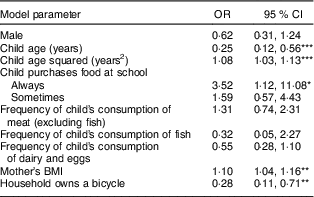
*P<0·05, **P<0·01, ***P<0·001.
† The overall model satisfies convergence criteria and is significant (likelihood ratio (df=10)=36, P<0·0001). The Hosmer and Lemeshow goodness-of-fit statistic (H-L (df=8, n 778)=7·70, P=0·463) and the c statistic at 0·721 are both acceptable.
‡ Overweight is defined as children with a BMI Z-score greater than +1 and includes obese children.
Child age, child age squared, always purchasing food at school (compared with never), household ownership of a bicycle and mother’s BMI were significantly associated with child overweight. The protective effect of child age and negative effect of child age squared on child overweight indicated that when children are in their early years, they are less likely to be overweight as they age; however in later years, the risk of overweight increases with increasing age, which suggests a curvilinear relationship between overweight and age. Children who always purchase food at school experienced significantly increased odds of being overweight than children who never purchase food at school. For every one point increase in maternal BMI, the risk of child overweight increased by 10 %. Children whose household owned a bicycle faced reduced odds of overweight by 82 % compared with children whose household did not own a bicycle.
Sex of the child and consumption of meat, fish, and dairy and eggs were retained in the model as they improved model fit based on the Akaike information criterion or −2 log likelihood statistics.
None of the measures of overall diet quality (i.e. dietary diversity score or dietary patterns) were significantly associated with overweight independently of individual food groups, nor did they improve the model fit. Therefore, they were not included in the final model.
School environment
Schools were ordered first by type (private then public) and then within these categories by size of the total student population (Table 3). Hours of operation and the proportion of recreation time were comparable across all six schools. Of the 5 h school day, 5–7 % was devoted to recreation or physical activity time. Overall, there was limited outdoor recreational space, and only two schools had shade or green space. No evident relationship between percentage overweight and outdoor space density was found, although the private schools were among the schools with higher proportions of overweight and lower outdoor space density. Across all six schools, only one had a water pump and electricity.
Table 3 School environment profile and student BMI category in six primary schools in Cap-Haitien, Haiti, 2012/13 school year

† Overweight is defined as children with a BMI Z-score greater than +1 and includes obese children.
All six schools had food vendors on the school property or in the immediate surrounding area; although School 3, a small public periurban school, had only one small kiosk with a limited selection of foods. The vendors sold processed foods (chips, cookies, crackers, ice cream, popcorn, sweets and sweet starch), fried foods (banana, dough, horse meat, hot dog), prepared foods (bread with peanut butter, hard-boiled eggs, boiled manioc, rice and beans/peas, sweet potatoes with milk, roasted peanuts), fruit (bananas and mangos), frozen fruit juice, sugar-sweetened beverages (fruit drinks, shaved ice with syrup) and coffee.
Discussion
Overweight was significantly associated with child age, always purchasing food at school, mother’s BMI and household ownership of a bicycle. The assessment of food availability and the physical activity environment at schools revealed limited time and space for physical activity, and high availability of unhealthy food options for purchase. Recreation time for children ranged from 15 to 20 min/d, below the Institute of Medicine’s recommendation of both 30 min of physical education daily and additional vigorous- or moderate-intensity physical activity throughout the school day( 33 ).
Children who always purchase their lunch at school experienced higher odds of being overweight than children who did not, independent of other socio-economic exposures. In this relationship, availability of high-fat or high-sugar foods may have played a role, although this was not possible to evaluate in the present study due to the number of participating schools. Several studies from South Africa and Swaziland have documented in detail the poor nutritional quality of vendor foods sold near schools, and in South Africa a positive association was observed between overweight and purchasing of those foods by students( Reference Wojcicki and Elwan 34 – Reference Wiles, Green and Veldman 37 ). The positive relationship between purchasing power and overweight observed in the present study is also consistent with past findings that the relationship between obesity and socio-economic status is modified by the country’s economic development level( Reference Monteiro, Moura and Conde 38 ), given that Haiti is one of the lower-income countries in Latin America.
A country that is transitioning to higher prevalence of chronic disease has a typical dietary profile characterized by higher consumption of fat, sugar and processed foods, and lower consumption of fibre, fruits and vegetables, although the specific dietary patterns are variable within and between countries( 11 , Reference Ng, Fleming and Robinson 17 – Reference Malik, Willett and Hu 19 ). Despite not reaching significance in the present study, inclusion of consumption of meat, fish, and dairy and eggs improved model fit and may indicate a possible role for these foods in overweight or obesity interventions. Eggs have previously been identified as a cost-effective and often overlooked component of maternal and young child nutrition, and their potential role in prevention of overweight is encouraging( Reference Iannotti, Lutter and Bunn 39 ). Dietary patterns that include foods high in monounsaturated and polyunsaturated fats (such as fish) are associated with prevention and reduction in chronic disease( Reference Willett 40 ).
A large body of evidence exists for what is effective in prevention of obesity in school-aged children( 41 – Reference Brennan, Brownson and Orleans 44 ), although few of the effectiveness studies have been conducted in Latin America( Reference Lobelo, Garcia de Quevedo and Holub 45 , Reference Holub, Elder and Arredondo 46 ), and little is available from sub-Saharan Africa and particularly countries like Benin, Ghana and Congo which have similar epidemiological trends to Haiti( Reference Naidoo, Coopoo and Lambert 47 , Reference Draper, de Villiers and Lambert 48 ). School-based interventions have been favoured in the past most likely because children spend a large amount of their time at school, school settings inherently expose children to dietary and physical activity factors, and schools allow for institutionalization and sustainment of interventions( Reference Khambalia, Dickinson and Hardy 42 ). Strong evidence exists for high-intensity, comprehensive and multi-component interventions, which often include a nutrition and physical activity curriculum, a family component and a healthy food environment, although information regarding cost of these interventions is absent( 41 – Reference Waters, de Silva Sanigorski and Hall 43 ). Evidence of effectiveness in Latin America is mostly comprised of interventions that included in-school nutrition and physical education classes and were carried out in Mexico, Chile and Brazil( Reference Lobelo, Garcia de Quevedo and Holub 45 , Reference Hoehner, Soares and Perez 49 ).
Limited evidence exists for policy and environmental strategies for prevention of childhood obesity( Reference Khambalia, Dickinson and Hardy 42 , Reference Brennan, Brownson and Orleans 44 ), even though these tend to be more affordable and sustainable than promoting individual behavioural changes( Reference Swinburn, Sacks and Hall 21 ). School nutrition guidelines and reduced pricing for healthy foods sold at school have been shown to improve children’s dietary intake( Reference Jaime and Lock 50 ). In addition, a novel method recently used for assessing evidence of effectiveness found that strategies targeting school food, beverage and physical activity policies and environments, food pricing, availability of parks and recreational facilities, and point-of-decision prompts were effective in prevention of childhood obesity( Reference Brennan, Brownson and Orleans 44 ). As recent governmental obesity prevention policies enacted in Mexico, Brazil and Chile( Reference Kain, Cordero and Pineda 51 ) undergo evaluation in the future, these may serve as examples for what is possible in the Haiti context.
Study limitations
We were able to draw on multiple dietary and socio-economic data from a large nutrition intervention study to examine an emerging public health nutrition issue in Haiti. However, secondary analysis of existing data potentially presents some limitations. We used baseline data and a cross-sectional analysis, and therefore no conclusions regarding causality can be made. Further, we were not able to examine the full set of factors that could potentially be influencing overweight and obesity in the country. There may also have been limitations arising from assessment of children’s dietary intake using a short-recall FFQ, such as daily variation in food intake, selective misreporting of results, caregiver recall bias, absence of sufficient data to calculate total energy intake, and other factors.
Conclusion
To our knowledge, the present study is the first to examine the covariates of childhood overweight or describe food availability and the physical activity built environment in Haiti schools. The increasing prevalence of overweight among children and adults has been extensively documented in other Latin American countries as they underwent their own nutrition transitions( Reference Popkin, Adair and Ng 4 , Reference Hoehner, Soares and Perez 49 , Reference Uauy and Kain 52 – Reference Tzioumis and Adair 56 ). As the public health nutrition programmes of Haiti and similar countries face the new complexities of the dual burden of overweight and undernutrition, there is an opportunity to draw on previous experiences and evidence in order to intervene early and in a targeted manner. The early nutrition transition period is a particularly important time for action, because of the opportunity to prevent the rises in overweight and obesity associated with this phenomenon before they become entrenched. However, limited research from early nutrition transition settings exists. Further studies are needed to adapt and implement effective and cost-effective interventions, such as changes to the food environment, for urban communities in Haiti and other similar contexts. Surveillance of the urban built environments and policies is needed before further increases in overweight prevalence occur. Lessons from Haiti may eventually be applied to other very early transition countries in the future.
Acknowledgements
Acknowledgements: The authors thank the study participants for generously offering their time; members of the study team; Summer Program for Research in Global Health (SPRINGH) fellow Charmayne Cooley of the Institute for Public Health at Washington University in St. Louis; and Brown School graduate student, Teresa Tufte. Financial support: This research was supported by the US Department of Agriculture (USDA) Foreign Agricultural Service’s Micronutrient Fortified Food Aid Products programme (grant number FFE-521-2012/034-00). The USDA Foreign Agricultural Service had no role in the design, analysis or writing of this article. This publication was also supported by Washington University in St. Louis Global Health Center of the Institute for Public Health. Conflict of interest: The authors have no conflict of interest to report. Authorship: L.L.I. and P.B.W. designed and L.L.I., J.R.D. and P.B.W. conducted the Mamba study. A.B.M., H.V.B. and L.L.I. designed the present study. A.B.M. carried out the data analysis. A.B.M., L.L.I. and H.V.B. made analytic decisions and interpreted data. A.B.M., H.V.B. and L.L.I. wrote the manuscript. All authors read and approved the final manuscript. Ethics of human subject participation: This study was conducted according to the guidelines laid down in the Declaration of Helsinki and all procedures involving human subjects were approved by the National Bioethics Committee of Haiti and the Human Research Protection Office of Washington University in St. Louis. Written informed consent was obtained from all participants.








