Introduction
Focus on individual psychotic symptoms rather than diagnostic categories and investigating effects of one symptom on another are important when investigating complex links between psychosis and violence (Swanson et al. Reference Swanson, Swartz, Van Dorn, Elbogen, Wagner and Rosenheck2006; Douglas et al. Reference Douglas, Guy and Hart2009). Violence is more common when psychotic symptoms are acute (Nielssen & Large, Reference Nielsson and Large2010; Large & Nielssen, Reference Large and Nielsson2011; Van Dorn et al. Reference Van Dorn, Volavka and Johnson2012; Coid et al. Reference Coid, Ullrich, Kallis, Keers, Barker and Cowden2013; Ullrich et al. Reference Ullrich, Keers and Coid2013; Keers et al. Reference Keers, Ullrich, DeStavola and Coid2014), and during acute episodes, symptoms can fluctuate (Bebbington et al. Reference Bebbington, Craig, Garety, Fowler, Dunn and Colbert2006; Odgers et al. Reference Odgers, Mulvey, Skeem, Gardner, Lidz and Schubert2009). Symptom shifts and fluctuations may be as important as or even more important than the presence of static symptoms typically measured in studies of psychosis and violence. It has been shown that symptom change itself may be a key driver in pathways to violence (Odgers et al. Reference Odgers, Mulvey, Skeem, Gardner, Lidz and Schubert2009) and that elevated levels of anger increase risk of violence when measured in the following week (Skeem et al. Reference Skeem, Schubert, Odgers, Mulvey, Gardner and Lidz2006). It is therefore important to conduct prospective studies measuring symptom change whilst simultaneously ensuring temporal ordering and proximity between symptoms and violent outcome (Odgers et al. Reference Odgers, Mulvey, Skeem, Gardner, Lidz and Schubert2009; Van Dorn et al. Reference Van Dorn, Volavka and Johnson2012; Ullrich et al. Reference Ullrich, Keers and Coid2013; Keers et al. Reference Keers, Ullrich, DeStavola and Coid2014). Cross-sectional methods, case register studies and meta-analyses including categorical diagnoses have shown little or no association (Coid et al. Reference Coid, Yang, Roberts, Ullrich, Moran and Bebbington2006; Elbogen & Johnson, Reference Elbogen and Johnson2009; Fazel et al. Reference Fazel, Gulati, Linsell, Geddes and Grann2009, Reference Fazel, Buxrud, Ruchkin and Grann2010) or concluded that violence is due to substance misuse (Fazel et al. Reference Fazel, Gulati, Linsell, Geddes and Grann2009, Reference Fazel, Buxrud, Ruchkin and Grann2010), criminological factors (Bonta et al. Reference Bonta, Law and Hanson1998) and social and environmental stress (Elbogen & Johnson, Reference Elbogen and Johnson2009). These factors do indeed increase the risk of both psychosis and violence and are good statistical predictors of future violence, but causal links have not been established (Coid et al. Reference Coid, Kallis, Doyle, Shaw and Ullrich2015). These factors may be more important in their effects on symptoms shift leading to intensification and violence during acute psychotic episodes. More recently, meta-analysis concluded that, among risk factors, positive but not negative symptoms are associated with violence (Witt et al. Reference Witt, Van Dorn and Fazel2013). No specific symptom associations were observed except excitement and hostility. By contrast, interaction analysis previously found high levels of suspiciousness/persecutory ideation and delusional thinking associated with serious violence (Swanson et al. Reference Swanson, Swartz, Van Dorn, Elbogen, Wagner and Rosenheck2006). Specific effects of paranoid delusions have also been found in the pathway, but these were mediated by angry affect due to content and meaning of the delusions (Coid et al. Reference Coid, Ullrich, Kallis, Keers, Barker and Cowden2013; Ullrich et al. Reference Ullrich, Keers and Coid2013). However, relationships between changes in anger and simultaneous changes in positive and negative psychotic symptoms have not been investigated.
Emergence of positive symptoms may be driven by fluctuations in affect among persons vulnerable to psychosis (Myin-Germeys & van Os, Reference Myin-Germeys and van Os2007; Thewissen et al. Reference Thewissen, Bentall, Oorschot, Van Lierop, van Os and Myin-Germeys2011). Because anger shows a strong (Reagu et al. Reference Reagu, Jones, Kumari and Taylor2013) and possible causal association in the pathway to violence (Coid et al. Reference Coid, Ullrich, Kallis, Keers, Barker and Cowden2013; Ullrich et al. Reference Ullrich, Keers and Coid2013), it is important to test whether changes in affective states of anger are primary or secondary in their effects on violence when associated with psychotic symptoms. Negative and positive symptoms are strongly correlated (Czobar & Volavka, Reference Czobor and Volavka1996). Although meta-analysis failed to show associations (Witt et al. Reference Witt, Van Dorn and Fazel2013), a previous study found independent protective effects from certain negative symptoms (Swanson et al. Reference Swanson, Swartz, Van Dorn, Elbogen, Wagner and Rosenheck2006). It is therefore important to re-examine the relationship between positive and negative symptoms during fluctuations in their intensity in view of inconsistency of previous findings.
We carried out a prospective longitudinal study over a 12-month follow-up period of patients discharged from medium secure services in England and Wales designed to investigate relationships between shifts in positive and negative symptoms and fluctuations in the intensity of angry affect. Our aims were to determine (1) independent associations between changes in total positive and negative scores, and individual symptoms, with violent behaviour; (2) whether co-occurring changes in negative symptoms have protective effects against violence during positive symptom shifts; and (3) whether changes in angry affect result in or are due to changes in positive and negative symptoms.
Method
The data collection method has previously been described (Coid et al. Reference Coid, Kallis, Doyle, Shaw and Ullrich2015). In brief, a prospective cohort follow-up study was carried out on all patients discharged from 32 National Health Service (NHS) medium secure units across England and Wales between 1 September 2010 and the 31 August 2011. These patients had been detained under compulsory orders following violent and criminal behaviour. Patients discharged to the community were eligible for follow-up. ‘Community’ placements included accommodation such as independent tenancies, supported accommodation, hostels, open rehabilitation wards and open psychiatric units.
A link person was identified at each hospital site and a notification system set up so that researchers would be automatically informed when a patient was discharged. Baseline assessments were then conducted for those discharged by interviewing a member of staff who knew the patient well, and a review of clinical and criminal records. Patients were followed-up twice after release at 6 and 12 months.
The North-West England multi-site research ethics committee approved the study. To ensure a total sample of discharges, permission was sought and granted by the National Information Governance Board (NIGB) to conduct the study without patient consent under Section 251 of the UK National Health Service Act, 2006.
Measures
Demographic and diagnostic information were recorded at baseline for each patient. Measures of psychotic symptoms, affective states and violent behaviour were completed based on information from collateral interview and file review. The following assessments were conducted:
(a) The Positive and Negative Syndrome Scale (PANSS) (Kay et al. Reference Kay, Fiszbein and Opfer1987; Tueller et al. Reference Tueller, Johnson, Grimm, Desmarais, Sellers and Van Dorn2017; van Dorn et al. Reference Van Dorn, Desmarais, Grimm, Tueller, Johnson and Sellers2016) is a 30-item instrument covering positive and negative symptoms and general psychopathology. Both negative and positive scales comprise seven symptoms. Each symptom is rated on a 1–7 scale (higher ratings reflect more severe presentation); ratings can be summed to a total positive and total negative score. High ratings of hostility are based on threatening behaviour and actual physical violence. Associations with violence would be overestimated due to content overlap. The PANSS contains a Supplemental Aggression Risk profile of which a state measure of anger was included in the interview schedule. PANSS ratings were completed following review of records and interview with collateral informants based on patient behaviour and functioning in the past month. Intra-class correlation coefficients (ICCs) were calculated between four researchers based on 20 cases. Inter-rater reliability for total PANSS score was very good (ICC = 0.93).
(b) Violence was measured using the McArthur Community Violence Instrument (MCVI) (Monahan et al. Reference Monahan, Steadman, Silver, Appelbaum, Robbins and Mulvey2001) comprising 18 questions on violent incidents. Violence was defined by combining ‘violence’ and ‘other aggressive acts’, including sexual acts, assaultive acts involving weapon use or threats made with weapon in hand, and acts of battery, regardless of resulting injury. Verbal threats alone were excluded. Additionally, details of criminal convictions 12 months post-discharge were obtained from the Police National Computer (PNC). Any violent convictions or cautions fitting the definition of violence were included.
PANSS ratings were carried out at baseline, prior to or shortly after discharge, and at 6 and 12 months post-discharge. Measures of violence using MCVI were taken at 6 and 12 months, together with additional information obtained following study completion for violent offending in criminal records. For each 6-month follow-up period, MCVI and PNC were combined.
Statistical analysis
For descriptive purposes, absolute (n) and relative frequencies (%) were reported for dichotomous/polytomous categorical variables, means (M) and standard deviations (s.d.) for variables on interval/ratio level. In case of multilevel analyses, descriptive statistics reflected observations rather than cases.
Symptom shifts were calculated by subtracting ratings at a previous time point from ratings at subsequent time points. Negative values indicated improvement in symptom/total score; positive values indicated deterioration. We investigated symptom shifts for each PANSS symptom/total scores between baseline and 6 months and between 6 and 12 months with concurrent violence.
To take advantage of the longitudinal study design, multilevel modelling was applied. These models account for dependence of data collected longitudinally by modelling relatedness of repeated measurement within the same individual as random effects. Unlike other approaches, such as analysis of variance, mixture models do not require complete data for individuals at each time point or imputation of data which may result in bias (Gueorguieva & Krystal, Reference Gueorguieva and Krystal2004). By using all available data, multilevel models are particularly powerful in longitudinal studies where individuals are often lost to follow-up. We performed mixed-effect multilevel ordinal and logistic regression models (N = 731 observations). Analyses were run in three steps: adjustment for demographic and clinical co-variates (associated with missingness of follow-up data whereby the assumption was missingness-at-random), further adjustment for symptoms in the same domain (positive/negative), and fully adjusted where all positive and negative symptoms were included simultaneously.
Further analyses aimed to identify explanatory variables in the pathway from significantly associated symptom shifts with violence. To qualify as explanatory variable, a symptom had to be associated with both exposure and outcome. Only if both associations were significant (p < 0.05) were variables selected and entered in an adjusted model. We examined percentage reduction in baseline odds of each symptom after adding the potentially explanatory variable into the following equation:
Comparisons between baseline-adjusted and fully adjusted coefficients were used to estimate the extent to which the association between a symptom shift and violent outcome was accounted for by the explanatory variable. We performed multilevel logistic regression analyses to investigate (i) associations between exposure variables and violence and (ii) associations between explanatory variables and violent outcome. To establish associations between explanatory and exposure variables, we applied multilevel ordinal logistic regression models.
Additionally, we investigated whether there was a variation in the prevalence of violence across different combinations (stable, increase or decrease) of positive and negative symptom score shifts. We performed multilevel logistic regression models to test differences between simultaneous stability of positive and negative symptom score and each of the other combinations of positive and negative symptom shifts.
Finally, we carried out analyses at symptom level combining baseline level and symptom shift. Baseline levels of each symptom were defined according to whether baseline scores were below or equal to the median, or increased above the median. Symptom shift was divided into three categories: stable, increase or decrease of symptom score. This categorisation resulted in five groups: (1) those with low ratings at baseline who remained low (reference group); (2) those with low ratings at baseline whose ratings increased above the median; (3) those with high ratings at baseline who remained high; (4) those with high ratings at baseline whose ratings decreased below the median; (5) those with high ratings at baseline whose ratings subsequently increased.
Results
There were 788 patients discharged during the study period, 409 (52%) to the community. At 6 months post-discharge, collateral interview and case note reviews were completed for 387 (95%); at 12 months 344 (89%) patients. At 6 months post-discharge, 54 (14.0%) patients had perpetrated at least one violent act; between 6 and 12 months, 43 (12.5%) had been violent.
Mean age was 37.8 years (s.d. = 9.7), 344 (88.9%) men, 232 (60.1%) were white, 98 (25.4%) black, 24 (6.2%) South Asian, 24 (6.2%) mixed heritage and eight (2.1%) Chinese or other ethnic origin. Primary diagnoses included 313 (80.9%) schizophrenia/schizoaffective disorder, 28 (7.2%) bipolar disorder, 21 (5.4%) personality disorder, three (0.8%) anxiety disorder, five (1.3%) depression, one (0.3%) substance use and 16 (4.1%) other diagnoses.
From baseline to first follow-up, 18.1% demonstrated stable positive symptom scores; 41.9% showed reduction, 40.0% increase. From first to second follow-up, 40.0% demonstrated stable positive symptom scores; 26.7% showed reduction, 34.3% increase. The negative symptom score remained stable from baseline to first follow-up in 15.5%; 45.3% showed decrease, 39.1% increase. From first to second follow-up, the negative symptom score remained stable in 36.6%; 35.2% showed decrease, 28.2% increase.
Associations of positive and negative symptoms with violent behaviour
Following adjustment for demographic co-variates and primary diagnosis, all positive PANSS symptoms demonstrated significant associations with violence (Table 1, model I). Significant associations among negative symptoms included emotional withdrawal, poor rapport and social withdrawal. Both total positive and negative scores were significantly associated with violence.
Table 1. Effects of symptom shift on violence

a Adjusted for age, gender, ethnicity and primary diagnosis.
b Adjusted for demography, primary diagnosis and other domain (positive/negative) symptoms.
c Adjusted for demography, primary diagnosis and simultaneous inclusion of all positive and negative symptoms.
d The total score of positive symptoms was adjusted for demography, primary diagnosis and total score of negative symptoms; the total score of negative symptoms was adjusted for demography, primary diagnosis and total score of positive symptoms.
However, following simultaneous inclusion of all items from the same domain (positive–positive/negative–negative), only anger in the positive domain and poor rapport in the negative domain remained significantly associated with violent behaviour (Table 1, model II). We then included simultaneously all positive and negative symptoms (Table 1, model III). Only anger demonstrated a positive association, suggesting that among positive and negative symptoms, anger was explanatory in the pathway towards violence. Associations between anger and other positive and negative symptoms are shown in Supplementary Table S1.
To investigate further, we ran a model where all positive and negative symptoms were included except anger. Only one positive symptom, suspiciousness/persecution (adjusted odds ratio (AOR) 1.76, 95% confidence interval (CI) 1.28–2.41, p < 0.001) remained significantly and independently associated with violence. Suspiciousness/persecution was also significantly (p < 0.05) associated with anger (Fig. 1). After inclusion in the model, suspiciousness/persecution no longer demonstrated significant association with violence; anger substantially accounted for this association.

Fig. 1. Direct and indirect pathways of symptom shift towards violence.
We reset the model to test the possibility that anger was the causal variable and suspiciousness/persecution the explanatory variable leading to violent behaviour. However, after inclusion in this second model, anger still demonstrated a significant association indicating that suspiciousness/persecution did not explain the relationship (Fig. 1).
To explain the change of direction in association between total negative score and violence after inclusion of total positive score in the model, we investigated which specific symptoms contributed to this reversion. By adding each individual symptom separately to model I (Table 1), total negative score was still a risk factor until inclusion of anger, when it was no longer associated with violent outcome (AOR 0.95, 95% CI 0.91–1.00, p = 0.061) indicating anger as the explanatory variable.
Similarly, by removing each positive symptom individually from the total positive score (model III, Table 1), the negative score was no longer a risk factor for violence after removal of suspiciousness/persecution (AOR 0.94, 95% CI 0.88–1.00, p = 0.050). This indicated that suspiciousness/persecution was the key driver of the positive association. After removing anger, the association with violence changed direction (AOR 0.94, 95% CI 0.90–1.00, p = 0.033) and became protective.
Symptom shift
Supplementary Table S2 provides descriptive statistics of changes at individual symptom level and violent behaviour.
At individual symptom level (Table 2), stable high baseline delusions were associated with significant increase in violence. Increase in severity from low baseline suspiciousness/persecution was also related to increased likelihood of violence. Compared with stable low baseline level of anger, increase in each level of anger was associated with increased prevalence of violence. In the negative domain, further increase from high baseline blunted affect was associated with significant decrease in violence.
Table 2. The effects of a shift in positive and negative symptoms on violent outcome (median split)
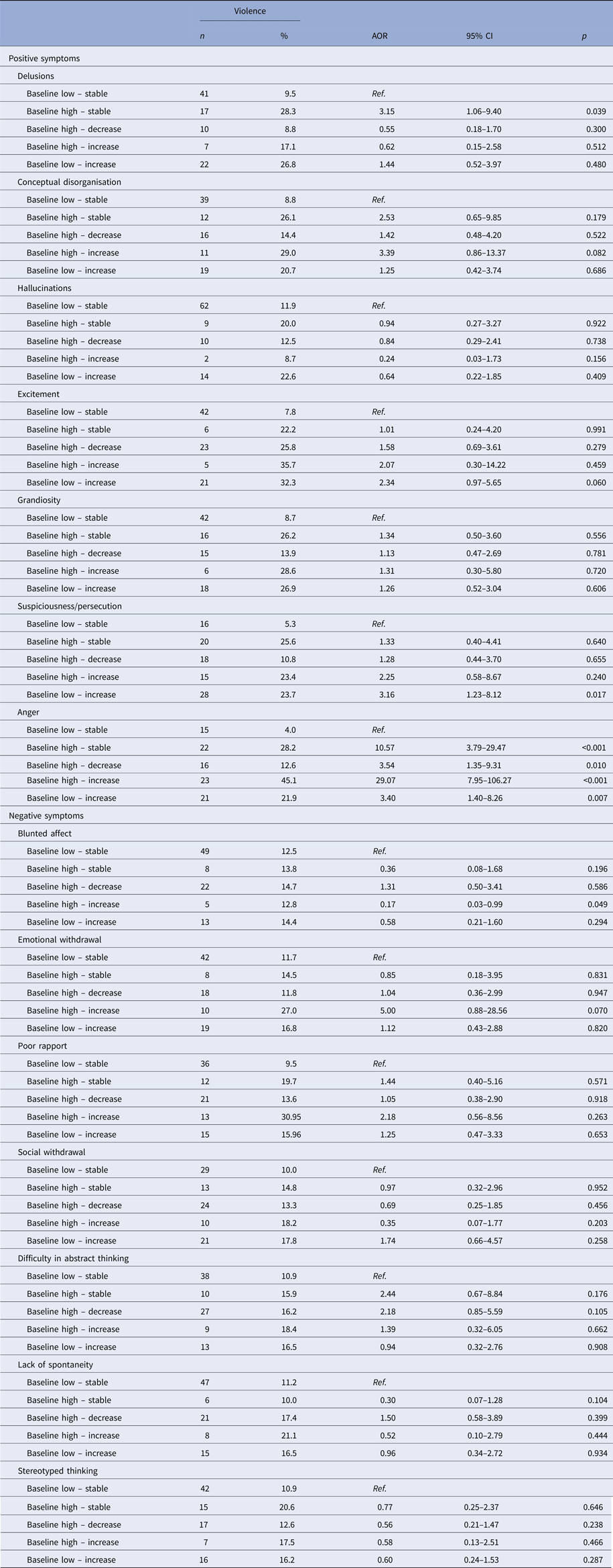
Note: Adjusted for demography, diagnostic category and other positive and negative symptoms.
Shifts in positive and negative symptom scores
Following adjustments, positive symptom scores were significantly associated with negative symptom scores (AOR 1.40, 95% CI 1.33–1.47, p < 0.001). Furthermore, shift in positive symptom scores (increase/decrease) was significantly related to shift in negative symptom scores (AOR 1.24, 95% CI 1.21–1.28, p < 0.001). Mean change in total positive symptom scores was 0.45 (s.d. 6.10) and 0.08 (s.d. 6.72) in negative total scores. This difference in size shift was not statistically significant (z = 0.42, p = 0.699).
Prevalence of violence for both stable positive and stable negative symptom scores was 6.7% (Fig. 2). Significant differences in the prevalence of violence at p < 0.05 between stable symptom scores and combinations were observed only when positive symptom scores increased; upward and downward shifts in negative symptom scores conveyed neither protective effects nor increased risk of violence. Overall, after adjustment for each other, increase in positive symptoms (AOR 1.15, 95% CI 1.10–1.20, p < 0.001) and decrease in negative symptoms (AOR 0.95, 95% CI 0.91–1.00, p = 0.035) were associated with violence.

Fig. 2. Prevalence of violence and stability/shift in positive and negative symptom scores. Note: AOR for comparison between stable both positive and negative symptom score and other combinations adjusted for demographic characteristics and diagnostic category. n.s. p ⩾ 0.05, *p < 0.05, **p < 0.01, ***p < 0.001.
Discussion
Prevalence rates of violent behaviour in the two 6-month periods of study were somewhat lower than in two previous US studies of discharged patients (Swanson et al. Reference Odgers, Mulvey, Skeem, Gardner, Lidz and Schubert2004, Reference Swanson, Swartz, Van Dorn, Elbogen, Wagner and Rosenheck2006) but are nevertheless of concern. Most patients received a diagnosis of schizophrenia, had been detained in secure hospitals for prolonged periods following criminal convictions for violence, remained subject to legal restrictions, including requirements to take medication, and subject to compulsory recall to hospital if considered a risk to others or themselves. Most were discharged to accommodation where they received daily observations from trained staff. Discharge had followed good treatment response, sustained progress in rehabilitation and mental state stability. Our findings were therefore unexpected, indicating that many were unstable following discharge, with more than a third showing profile shifts towards more positive symptoms during the first 6 months and approximately a quarter in the second.
Shifts in symptom profile, specifically those in which positive symptoms intensified, were associated with violence. The larger the positive symptom shift, the more likely violence would occur. These findings correspond to clinicians’ experience of violent psychotic patients in inpatient settings but we are not aware of any previous study which has demonstrated these effects. Negative symptoms tended to shift similarly in direction to positive. Although increase in negative symptoms was associated with protective effects against violence, this could only be observed after adjusting for positive symptoms in our statistical models. Our findings therefore suggested that when positive–negative shifts co-occurred, positive symptoms overcame protective effects of negative symptoms. Although there was no clinically observable protective effect observed from the simultaneous increase in negative symptom scores, a protective effect was observed with a single symptom. Increase in the intensity of blunted affect from a low initial level was clinically protective, but in only a small number of observations.
A key finding was that a single affective state, anger, appeared the main driving factor for positive symptom shifts associated with violence. No other positive symptom changes, except increasing suspiciousness/persecution, were associated with violence. However, this change was substantially accounted for by the shift in anger. Furthermore, a high and stable (unchanging) presentation of delusions across the two 6-month periods of observation was independently associated with violence.
Does angry affect drive the positive symptom shift resulting in violence?
We compared mean size of shifts in total negative and positive symptom scores. Our expectation was that the effect exerted on violence by positive symptoms had simply outweighed protective effects of negative symptoms. When a shift resulted in violence, the mean positive symptom shift appeared much larger than the negative. However, this difference was not statistically significant and therefore could not explain the effect of positive symptoms on violence relative to negative symptoms.
We next examined whether one or more positive symptoms exerted a particularly powerful effect. Shifts in anger appeared to exert a unique effect on violence. These findings correspond to previous studies of mediating effects of angry affect on associations between persecutory delusions and serious violence. However, the latter differed in that the specific form of anger was due to content and meaning of the delusions to the patient (Coid et al. Reference Coid, Ullrich, Kallis, Keers, Barker and Cowden2013; Ullrich et al. Reference Ullrich, Keers and Coid2013). This corresponds to the only previous study of fluctuations of symptoms on violence in a sample of depressed patients, where anger exerted a specific effect (Skeem et al. Reference Skeem, Schubert, Odgers, Mulvey, Gardner and Lidz2006).
We further established that suspiciousness/persecution did not explain the association between anger and violence. This would suggest that in our previous studies demonstrating the importance of content and meaning of delusions leading to violence perpetration (Coid et al. Reference Coid, Ullrich, Kallis, Keers, Barker and Cowden2013; Ullrich et al. Reference Ullrich, Keers and Coid2013) shifts in angry affect may have preceded either the formation of new or intensification of existing delusions, and additionally determined their content along a pathway to violence. In this context, a shift leading to increase in anger when combined with secondary anger due to the content of the delusion would greatly increase probability of violence occurring, the victim being determined then targeted due the delusional beliefs.
Are negative symptoms protective?
The observation that increase in blunted affect was associated with a protective effect on violence suggested a possible damping process on the shift towards greater intensity of positive symptoms. However, there were few cases in which this process occurred and the overall effect of blunted affect on violence was small. No other negative symptoms showed independent effects. Nevertheless, total negative score showed a significant inverse association with violence, but only after adjusting for total positive score. This suggested that protective effects of negative symptoms could not be observed clinically. Because positive symptoms and negative symptoms corresponded in their direction of shift, this could have been explained by two possibilities. We therefore firstly investigated whether, when a shift occurred, the magnitude of increase in positive symptoms outweighed that of a negative shift, i.e. there were simply more positive than negative symptoms. However, we excluded this explanation. We finally observed that any protective effects of negative symptoms were overcome by a shift in the intensity of a single symptom, anger.
Limitations
This study has several limitations. Although the method allowed prospective measurement of both symptoms and violence, PANSS ratings relied on observations of staff rather than patient interviews. This methodology permitted by the UK legislation to gather data without consent was necessary to obtain sufficient power and ensure timing of ratings. Patients were subsequently asked whether they would have been willing to co-operate in repeated interviews for the study. Only 40% responded positively.
When investigating relationships between symptoms of psychosis and violence, it is essential to account for the fact that both exposure and outcome are dynamic in nature and fluctuate over time. It has been emphasised that spatio-temporal contiguity is of utmost importance to uncover such associations (van Dorn et al. Reference Van Dorn, Volavka and Johnson2012, Reference Van Dorn, Grimm, Desmarais, Tueller, Johnson and Swartz2017; Coid et al. Reference Coid, Ullrich, Kallis, Keers, Barker and Cowden2013; Ullrich et al. Reference Ullrich, Keers and Coid2013). However, it can be argued that temporal proximity does not necessarily imply temporal ordering and, therefore, the possibility of reversed causality has to be taken into consideration. Criteria of causality were published some decades ago (Hill, Reference Hill1965) and have been guidelines in epidemiology. One of these is plausibility and (from a clinical perspective) it is more plausible that persecutory delusions lead to anger which in turn leads to violence than the reverse pathway.
Future research using sophisticated designs such as experience sampling should be considered to provide both temporal ordering of exposure and outcome and temporal proximity (Delespaul, Reference Delespaul1995; Myin-Germeys et al. Reference Myin-Germeys, Oorschot, Collip, Lataster, Delespaul and van Os2009). This method might overcome the limitation of this study where we were unable to identify temporal order.
Affective symptoms in the study were limited to anger. The PANNS includes additional symptoms of poor impulse control, tension, lack of co-operation and excitement which are combined with hostility in an excited component (PANNS-EC: Montoya et al. Reference Montoya, Valladares, Lizan, San, Escobar and Paz2011). These symptoms are likely to be strongly correlated with anger. Future investigation should therefore identify their independent effects on shifts in positive and negative symptoms and violence.
The importance of affective symptoms among psychotic patients has been demonstrated in a study which combined the PANNS with Brief Psychiatric Rating Scale (BPRS: Overall, Reference Overall and Oliver-Martin1974) using four combined datasets to identify an affective factor, or symptom cluster, associated with violence in the community (Tueller et al. Reference Tueller, Johnson, Grimm, Desmarais, Sellers and Van Dorn2017; van Dorn et al. Reference Van Dorn, Desmarais, Grimm, Tueller, Johnson and Sellers2016, Reference Van Dorn, Grimm, Desmarais, Tueller, Johnson and Swartz2017). However, combination of multiple affective variables into a single factor precluded the ability to identify which individual symptoms had strongest effects and should be targeted in future treatment interventions to prevent violence. Furthermore, omission of agitation, a key factor on the pathway to violence for a subgroup of acutely psychotic patients, requiring different treatment interventions from anger (Hankin et al. Reference Hankin, Bronstone and Koran2011), was a limitation shared by our study.
The sample was not representative of all persons with psychosis. None were in their first episode and some had remained symptomatic for several years. A sample admitted during acute psychotic episodes to general rather than secure inpatient services may have shown different patterns of symptom shift. It is therefore unclear whether two 6-month periods were sufficient to adequately capture symptom shifts. Multiple ratings would have been necessary to investigate oscillations of emotional dysregulation previously observed in a sample of high-risk patients with a primary diagnosis of depression (Odgers et al. Reference Odgers, Mulvey, Skeem, Gardner, Lidz and Schubert2009). However, psychotic symptom changes among patients with emotional dysregulation are more frequent than among those with schizophrenia (Glaser et al. Reference Glaser, van Os, Thewissen and Myin-Germeys2010).
Implications
Affective symptoms, including anger, are traditionally considered peripheral or ancillary to core positive and negative symptoms of schizophrenia (Bebbington, Reference Bebbington2015). Mood instability is increasingly recognised as a prominent feature, however, and may play a key role in the genesis of psychosis (Marwaha et al. Reference Marwaha, Broome, Bebbington, Kuipers and Freeman2014). Affective symptoms and mood disturbances typically predate onset of schizophrenia and may indicate impending relapse (Häfner et al. Reference Häfner, Maurer and An Der Heiden2013). Because violence risk is greater at times when psychotic symptoms are acute (Nielssen & Large, Reference Nielsson and Large2010; Large & Nielssen, Reference Large and Nielsson2011; Van Dorn et al. Reference Van Dorn, Volavka and Johnson2012; Coid et al. Reference Coid, Ullrich, Kallis, Keers, Barker and Cowden2013; Ullrich et al. Reference Ullrich, Keers and Coid2013; Keers et al. Reference Keers, Ullrich, DeStavola and Coid2014), and serious violence in particular during prodromal phases (Nielssen & Large, Reference Nielsson and Large2010), our findings suggest that observing intensification of anger signals the need for urgent intervention to prevent violence occurring. Antipsychotic medication and nursing management of inpatients are primary interventions for psychotic patients thought to be at risk. However, our findings indicate that more attention to monitoring affect associated with positive symptoms of psychosis, and development of new pharmacological and psychological interventions (Novaco, Reference Novaco, Craig, Dixon and Ganon2013; Novaco & Whittington, Reference Novaco, Whittington and Fernandez2013) which are specific in reducing angry affect, are necessary to prevent violence. Most importantly, if fluctuations in angry affect are key drivers on the pathway to violence, then pharmacological agents which stabilise affect, with specific effects on anger, should be the primary focus.
Although cognitive behaviour therapy has been shown effective in reducing violent behaviour among psychotic patients (Novaco & Whittington., Reference Novaco, Whittington and Fernandez2013), it may be less effective in reducing their angry affect (Haddock et al. Reference Haddock, Barrowclough, Shaw, Dunn, Novaco and Tarrier2009). New psychological interventions which identify early signs of and control over shifts in anger may therefore be more effective in combination with subsequent behavioural control.
Among those vulnerable to psychosis, elevated reactivity to stress encountered in daily life is thought to result in severe affective responses (Myin-Germeys et al. Reference Myin-Germeys, van Os, Schwartz, Stone and Delespaul2001; Myin-Germeys & van Os, Reference Myin-Germeys and van Os2007). This is independent of cognitive deficits associated with schizophrenia, including those associated with negative symptoms (Lataster et al. Reference Large and Nielsson2013). Effects of stress factors in the social environment on onset and relapse of psychosis are also thought to be substantially mediated by non-psychotic, particularly mood symptoms (Bebbington, Reference Bebbington2015), and the negative effects of mood are thought to determine the content of delusional thinking (Garety & Freeman, Reference Garety and Freeman2013). Within this model, social and environmental risk factors which are changeable and have dynamic effects on violence should not be considered alternative or competing causal factors but integral, precipitating severe affective reactions which in turn trigger positive symptoms of psychosis on a pathway to violence. Alternatively, these stress factors could trigger affective reactions in individuals vulnerable to psychosis, but in the absence of positive symptoms or before their appearance. Further investigation should identify whether shifts in angry affect leading to violence can be spontaneous or are always preceded by environmental stress factors. This has key implications for managing patients during rehabilitation because mitigating their effects may prevent relapse. Specific focus on those which trigger anger (Freestone et al. Reference Freestone, Ullrich and Coid2017) may additionally prevent violence.
Acknowledgements
This article presents independent research funded by the National Institute for Health Research (NIHR) under the Programme Grants for Applied Research programme (RP-PG-0407-10500). The views expressed are those of the authors and not necessarily those of the NHS, the NIHR or the Department of Health.
Conflict of interest
None.
Ethical standards
The authors assert that all procedures contributing to this work comply with the ethical standards of the national and institutional committees on human experimentation and with the Helsinki Declaration of 1975, as revised in 2008.
Supplementary material
The supplementary material for this article can be found at https://doi.org/10.1017/S0033291718000077






