The task of assessing and managing risks associated with people with mental disorder is nothing new. Mental health professionals have been engaged in this task for many years as part of routine practice. However, recently there has been a greater awareness of the need to be more explicit about how mental health service providers, and the people who work for them, actually assess and manage the risks. This interest appears to be in response to a number of factors. These include: perceived failings in the policy of community care; criticisms of current practice following inquiries into tragedies involving people with serious mental illness; government initiatives to reduce suicide and improve community management of people with mental disorder; and the need for mental health providers to reduce the increasing costs associated with litigation and complaints (Reference Doyle and RyanDoyle, 1999).
The need to prepare staff to assess and manage risk in mental health services is now well established and it would seem logical to develop education and training which is open to all health care professionals engaged in clinical risk management. Interprofessional training initiatives have the potential to reduce friction between different professional groups and offer the opportunity to enhance communication, mutual understanding and collaborative practice development (Reference Roberts and PriestRoberts & Priest, 1997). However, problems have been highlighted resulting from rigid role demarcation, tradition, vested professional interest and poor communication, and these have led to confusion and misunderstanding about responsibilities (National Health Service Executive, 1993). To overcome these problems, a number of authors have suggested that joint inter-disciplinary educational initiatives should be developed, based on users' needs (e.g. Department of Health 1994; Centre for the Advancement of Interprofessional Education (CAIPE), 1996; Department of Health, 1996; Reference DuggenDuggen, 1997).
In response to the need for training resources in risk assessment and management, the University of Manchester (1996) produced Learning Materials on Mental Health Risk Assessment. More recently, Morgan (Reference Morgan1998) developed a training pack aimed at assisting mental health services in the preparation of their staff to undertake risk assessment and management. Despite these efforts and the continuing interest and concern in this area, there is little evidence of any cohesive, uniform approach to training clinicians to assess and manage risk in mental health services. This is highlighted by a recent survey aimed at establishing the proportion of hospital trusts in England and Wales in which risk training takes place. This found that many hospital trusts did not provide their staff with relevant training and that there was a considerable variation in the training that was provided (Reference Davies, Amos and ApplebyDavies et al, 2001).
This paper attempts to provide a clear example of how the rhetoric of closer interprofessional education has been turned into reality in Salford and Manchester since 1998. It will cover the stages of development from convening the inaugural steering group, carrying out the training-needs analysis, planning and delivering the training and, finally, evaluating outcome data from a series of training workshops. The impact on clinical practice will be discussed.
Getting started
The first step in developing the training was to establish a commitment from two local mental health trusts, North Manchester and Salford, and the local social services department in Salford. Key people with knowledge, skills and experience in the area of risk were then identified from each organisation and a service user was involved at an early stage of planning. Following an initial meeting, a steering group with clear terms of reference was established and provisional dates and targets were set.
Training needs analysis and development of workshop format
One of the first tasks was to carry out a training-needs analysis in each of the three principal organisations to examine staff requirements before developing the aim and objectives of the training. A questionnaire was used to survey 106 staff spread evenly over the three organisations. In summary, the findings revealed that the majority were confident of their skills in assessing and managing risk but that there was an overwhelming need for systematic frameworks. The training received was unsatisfactory, there was uncertainty about the impact of attitudes and beliefs and, on average, they could not realistically spend more than 2 days' training in this area.
In response to these findings and as recommended by Harris (Reference Harris1997), a seminar teaching approach was adopted and the overall aim of training was agreed. This was to provide the participants with knowledge, skills and systematic frameworks to assist in assessing and managing clinical risk. Four overall key objectives were agreed: (1) introduce risk management as a systematic, dynamic process; (2) outline the link between people with mental disorder and risk; (3) identify key risk factors; and (4) provide knowledge of risk assessment tools and practice in their use. A 2-day training format was agreed with 4 half-day sessions covering an introduction to clinical risk management, self-harm and suicide, risk to others and self-neglect. The aim was to achieve four objectives related to the overall key objectives in each of the three risk areas: self-harm and suicide, risk to others and self-neglect (Table 1). Accreditation was obtained from the Royal College of Psychiatrists and the Royal College of Nursing and places on the course were divided equally between each of the three organisations.
Table 1. Clinical risk training objectives

| Objectives | |||
|---|---|---|---|
| Overall | Self-harm and suicide | Risk to others | Self-neglect |
| 1. Introduce risk management as a systematic, dynamic process | 1. More aware of how negative attitudes may impact on a client's response to treatment | 1. How to identify type and severity of mental disorder associated with increased risk | 1. More aware of process of risk assessment |
| 2. Outline link between people with mental disorder and risk | 2. Increased awareness of the key skills required to conduct an effective risk assessment | 2. Increased awareness of main risk factors | 2. Increased awareness of ethical dilemmas |
| 3. Identify key risk factors | 3. Increased awareness of the theory of self-harm and suicide | 3. Identify main methods of assessment | 3. Increased awareness of the process of management |
| 4. Provide knowledge of risk assessment tools and practice in their use | 4. Session will be useful in professional work | 4. Session will be useful in professional work | 4. Session will be useful in professional work |
Method of evaluating training
Each of the objectives in the three risk areas was evaluated using a post-training evaluation form. Participants were also asked to rate their satisfaction with the content, methods, materials and delivery of the training on a Likert scale from 1 — very poor — to 5 — excellent — for each of the three risk areas. Comments were invited on each of the objectives and on the training generally. Over 200 fully completed evaluation forms were received for each of the risk areas, following 12 clinical risk training workshops held between July 1998 and June 2000.
In order to evaluate the impact of the training on clinical practice, we carried out an impact monitoring exercise. This involved sampling at random 100 staff from across the three organisations who had attended the 2-day training and who had been back in practice for at least 12 months. Participants were sent a questionnaire that asked them to rate their current practice against four key objectives related to the training: (1) I am more aware of issues related to….; (2) I use a structured approach when assessing….; (3) I am more confident in making a judgement about….; (4) I feel more able to justify my risk management decisions in relation to….; and one general objective: “Overall, I feel the workshop has been useful in improving my clinical practice”. Comments were also invited.
Results
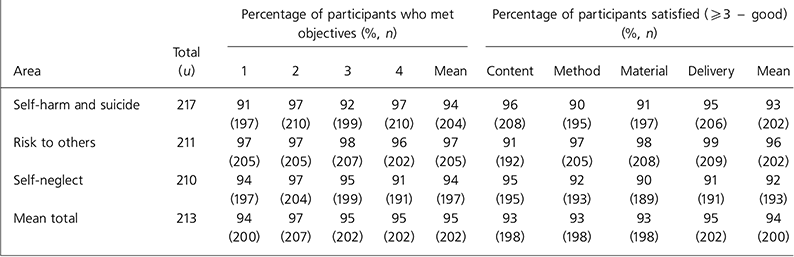
Based on fully-completed evaluation forms, approximately 70% of those attending the training workshops were from health services while 30% were from social services. Table 2 illustrates that over 90% of participants met the objectives for each risk area, ranging from an overall mean of 94% for self-harm and suicide and for self-neglect, to 97% for risk to others. Satisfaction was measured as greater than or equal to 3 (‘good’) on the satisfaction Likert scale. Using this cut-off, there was a mean 94% satisfaction rating across all risk areas. Common themes emerged from the comments made following training in relation to liability for decisions, lack of effective multi-disciplinary working, personality disorder, substance misuse, personal safety, limitations of established frameworks, risk management v. prediction and confidentiality.
Table 2. Percentage of participants who met workshop objectives and were satisfied, based on evaluation forms
| Percentage of participants who met objectives (%, n) | Percentage of participants satisfied (≥3 - good) (%, n) | ||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|
| Area | Total (u) | 1 | 2 | 3 | 4 | Mean | Content | Method | Material | Delivery | Mean |
| Self-harm and suicide | 217 | 91 (197) | 97 (210) | 92 (199) | 97 (210) | 94 (204) | 96 (208) | 90 (195) | 91 (197) | 95 (206) | 93 (202) |
| Risk to others | 211 | 97 (205) | 97 (205) | 98 (207) | 96 (202) | 97 (205) | 91 (192) | 97 (205) | 98 (208) | 99 (209) | 96 (202) |
| Self-neglect | 210 | 94 (197) | 97 (204) | 95 (199) | 91 (191) | 94 (197) | 95 (195) | 92 (193) | 90 (189) | 91 (191) | 92 (193) |
| Mean total | 213 | 94 (200) | 97 (207) | 95 (202) | 95 (202) | 95 (202) | 93 (198) | 93 (198) | 93 (198) | 95 (202) | 94 (200) |
Of the 100 staff sampled, 44 responded to the impact monitoring questionnaire (Table 3). Of these, well over 90% agreed or strongly agreed that the training had made them more aware, more structured, more confident and more capable when assessing and managing risk in their practice. All the respondents agreed or strongly agreed that the training had improved their clinical practice and impacted positively in their work.
Table 3. Impact monitoring: percentage who strongly agree/agree 12 months after training

| Key objectives | Self-harm & suicide (n) | Risk to others (n) | Self-neglect (n) | Overall mean (%) |
|---|---|---|---|---|
| I am more aware of issues related to… | 97 (39) | 95 (38) | 95 (39) | 96 |
| I am more confident in making a judgement in relation to… | 95 (36) | 92 (36) | 93 (38) | 93 |
| I use a structured approach to assessing… | 95 (37) | 93 (36) | 95 (39) | 94 |
| I feel more able to justify my risk management decisions in relation to… | 95 (37) | 95 (37) | 100 (41) | 97 |
| Overall I feel the workshop has been useful in improving my clinical practice | - | - | - | 100 (44) |
Clinical implications
The evaluation showed that the training workshop was very well received. Perhaps more importantly, of those who responded to the impact monitoring questionnaire, all felt that the training had improved their practice in assessing and managing risk of self-harm and suicide, harm to others and self-neglect. This demonstrates that a properly planned and delivered 2-day clinical risk assessment course can have a positive impact on the practice of clinicians in mental health services. However, the training was limited in its expectations and it can only reasonably be valued as an introductory course. More advanced courses in specific risk assessment instruments, and in risk formulation together with refresher workshops, are being delivered or planned as a result of the success of the original introductory course.
Declaration of interest
None.
Acknowledgements
The authors would like to thank all those involved in developing, delivering and evaluating the training, including (in alphabetical order) Lezli Boswell, Sondra Charlesworth, Janet Drinkwater, David Duffy, Paul Fallon, Dr Josanne Holloway, Dr Keith Hyde, Gail Johnson, Graham Jones, Glenn Mills, Alison Mott, Pam Neilan, Malcolm Storey and Dr Carl Wilson.






eLetters
No eLetters have been published for this article.