Background
In Australia, the number of people living with chronic health conditions is increasing. According to the 2017–2018 National Health Survey, 80% of Australians aged over 65 years had one or more chronic conditions (ie, arthritis, asthma, back pain, cancer, cardiovascular disease, chronic obstructive pulmonary disease, diabetes or mental health conditions) (Australian Bureau of Statistics, 2018a). Latest figures estimate that chronic conditions were responsible for around three-quarters of the total non-fatal burden of disease (Australian Institute of Health and Welfare, 2016), and around 9 in every 10 deaths (Australian Bureau of Statistics, 2018b).
The Chronic Disease Management (CDM) programme was introduced to the Medicare Benefits Schedule (MBS) to provide a more structured approach to managing patients with chronic conditions and complex care needs. It also recognised the important role allied health professionals play in supporting people with chronic disease to maximise their level of functioning and manage their own care safely and effectively. The programme supports general practitioners (GPs) to claim for up to one General Practice Management Plan (GPMP) for people with a chronic or terminal medical condition. It also supports, for people requiring care from a multidisciplinary team, up to one Team Care Arrangements (TCA) every year (Australian Government Department of Health, 2017). The recommendation is to prepare a new GPMP or TCA every 2 years, with review points at 6, 12 and 18 months (Royal Australian College of General Practitioners, 2018). The patient can additionally claim for up to five services provided by private allied health professionals and practice nurses (from 2007 onwards) within each calendar year.
While there may be long-term benefits from careful and thorough care planning (Burt et al., Reference Burt, Rick, Blakeman, Protheroe, Roland and Bower2014), in the short term it is possible that access to subsidised allied health services may be a major driver in commencing the care planning process for both patients and GPs. Although, as Foster et al. (Reference Foster, Mitchell, Haines, Tweedy, Cornwell and Fleming2008) highlighted, this may be suboptimal because of the limited number of allied health services allowed each year, and because optimal care is only available to those who are able to pay for the additional services required. This was reiterated by Refshauge et al. (Reference Refshauge, Dennis and Vassallo2016), who stated ‘the limited number of sessions, shared between the allied health specialities, is unlikely to be adequate to improve health outcomes because of an insufficient dose of treatment’.
While there has been evidence of a rapid uptake of CDM allied health service items over time (Cant & Foster, Reference Cant and Foster2011), and growing evidence of the impact of allied health interventions for diabetes, cardiac and respiratory health (Taylor et al., Reference Taylor, Brown, Ebrahim, Joliffe, Noorani, Rees, Skidmore, Stone, Thompson and Oldridge2004; Oldridge, Reference Oldridge2012; Smith et al., Reference Smith, Soubhi, Fortin, Hudon and O’Dowd2012; McCarthy et al., Reference McCarthy, Casey, Devane, Murphy, Murphy and Lacasse2015), there has been little evidence to date on the impact of these items on longer term patient outcomes, for example, preventing hospitalisations.
In contrast to the positive associations found by Vitry et al. (Reference Vitry, Nguyen, Ramsay, Caughey, Gilbert, Shakib, Ryan, Esterman, McDermott and Roughead2014) and Caughey et al. (Reference Caughey, Vitry, Ramsay, Gilbert, Shakib, Ryan, Esterman, McDermott and Roughead2016), who studied CDM item use among Australian war veterans, Welberry et al. (Reference Welberry, Barr, Comino, Harris-Roxas, Harris, Dutton, Donnelly, Jackson and Harris2019) and Comino et al. (Reference Comino, Islam, Tran, Jorm, Flack, Jalaludin, Haas and Harris2015) found no evidence that GPMPs or TCAs by themselves were associated with a reduction in unplanned hospital admissions. Welberry et al. (Reference Welberry, Barr, Comino, Harris-Roxas, Harris, Dutton, Donnelly, Jackson and Harris2019) by not being limited to a population of war veterans examined a more heterogeneous population in terms of mix of health status and chronic disease. However, despite controlling for various aspects of health status, it is possible that the heterogeneous nature of the population meant that CDM item use was still confounded with health status, diluting any underlying protective effect of GPMPs or TCAs.
A significant limitation of studying CDM item use within war veterans, as occurred within Vitry et al. (Reference Vitry, Nguyen, Ramsay, Caughey, Gilbert, Shakib, Ryan, Esterman, McDermott and Roughead2014) and Caughey et al. (Reference Caughey, Vitry, Ramsay, Gilbert, Shakib, Ryan, Esterman, McDermott and Roughead2016), is that the health cover provided via the Department of Veterans Affairs (DVA) is different to the cover provided under Medicare, Australia’s universal health insurance scheme. While the DVA scheme subsidises allied health services in various circumstances, Medicare only subsidises allied health via the CDM scheme (Australian Government Department of Health, 2018). For example, a DVA Gold Card holder can access as many allied health services as deemed clinically useful based on referral from their GP or specialist, and a DVA White Card holder may access these services if they are related to a war or service injury. Thus, the motivation and drivers for use of CDM items may be different for DVA clients compared to the general population.
This paper examines in more detail the allied health services claimed for up to 12 months after a GPMP or TCA claim within the Central and Eastern Sydney (CES) area. It aims to identify who is accessing which allied health service, how many services are being accessed and the differences in five-year hospitalisation rates by allied health service claims using record linkage data analysis.
Methods
Study design
The study design was a prospective longitudinal observational study of individuals aged 45 years and over who had at least one claim recorded for a GPMP (Item No. 723) or a TCA (Item No. 725) within a two-year health service utilisation baseline period (approx. 2007–2009). A prospective longitudinal observational study was undertaken in order to evaluate the impact of CDM allied health service claims on subsequent hospitalisations. Ethics approval was obtained from the NSW Population and Health Services Research Ethics Committee (2008/10/108).
Sample
The sample included all CES residents who were recruited to the 45 and Up Study and had at least one GPMP or TGA claim within a two-year baseline period centred on their study recruitment date: approximately 2007–2009 (n = 6426). Participants were excluded from the analysis if they were recruited prior to 2007 due to insufficient data for all MBS variables required (579 participants), if probable data linkage errors were identified (2 participants), if they died within a year of baseline (72 participants) or if missing/out of range data were present on key variables (2 participants) such as recruitment date or age. This resulted in a final sample of 5771.
Data sources and linkage
The research used data from the Sax Institute’s 45 and Up Study, linked by the Sax Institute using a unique identifier to MBS data provided by Department of Human Services for the period 2006–2014. It also used data from the Admitted Patient Data Collection, Emergency Department Data Collection and Death Registry, linked by the NSW Centre for Health Record Linkage using probabilistic techniques (NSW Ministry of Health, 2018).
The 45 and Up Study was based on the population of NSW, Australia. Prospective participants were selected from the Department of Human Services (formerly Medicare Australia) enrolment database using stratified random sampling, specifically stratified by age (less than 80 years and 80 years and over) and region (urban versus rural and remote). The Department of Human Services (formerly Medicare Australia) enrolment database provides near complete coverage of the population (45 and Up Collaborators, 2008). People aged 80 years and over and residents of rural and remote areas were oversampled. A total of 267 153 participants (30 645 within the CES area) joined the 45 and Up Study by completing a baseline questionnaire (between January 2006 and December 2009) and giving signed consent for follow-up and linkage of their information to routine health databases. Where possible, the questionnaire used validated questions (Sax Institute, 2018). About 18% of those invited participated, and participants included about 11% of the NSW population aged 45 years and over.
Measures
Participant characteristics using the 45 and Up Study baseline questionnaire data (Sax Institute, 2018), MBS data (Australian Government Department of Health, 2018) or Admitted Patient Data Collection data (NSW Ministry of Health, 2018) were grouped into four main categories: socio-demographic, health risk factors, health status and health care utilisation. Table 1 provides the definitions of these variables.
Table 1. Participant characteristics – definitions and data sources
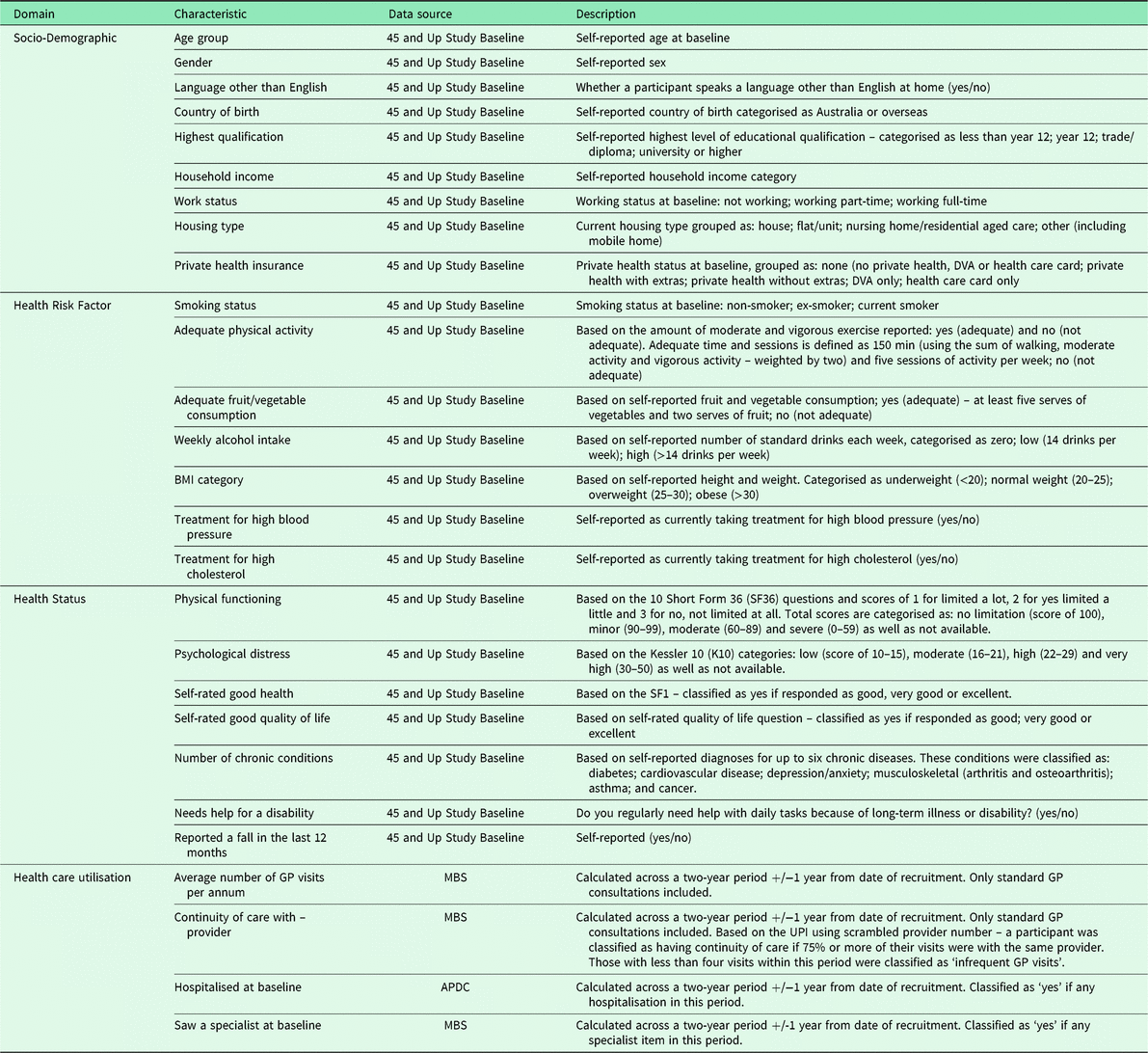
DVA = department of veterans affairs; BMI = body mass index; GP = general practitioner; MBS = medicare benefits schedule; UPI = Usual Provider Index; APDC = Admitted Patient Data Collection.
The exposure measures were claims for allied health service items, separately for the two most common allied health types, physiotherapy and podiatry, and combined for all other allied health (physiotherapy: 10960; podiatry: 10962; other allied health services: 10950, 10951, 10952, 10953, 10954, 10956, 10958, 10964, 10966, 10968,10970, 10997) in participants who had a GPMP or TCA (ie, items 723 or 725) within one year before and after recruitment to the 45 and Up Study (ie, a two-year window that mostly fell between 2007 and 2009).
The outcome measures were emergency admissions (EA) and potentially preventable hospitalisations (PPH). EA are defined as emergency department visits that led to a hospital admission. PPH are defined as admissions to hospital that could have potentially been prevented through the provision of appropriate non-hospital health services according to the preventable hospitalisation indicator in the Australian 2012 National Healthcare Agreement (Australian Institute of Health and Welfare, 2012). This indicator was composed of admissions for 21 conditions, broadly categorised as ‘chronic’, ‘acute’ and ‘vaccine-preventable’. The PPH could include people who were admitted through an emergency department.
Statistical analyses
The statistical analysis included three components: (i) a descriptive analysis of the characteristics of participants claiming allied health services; (ii) logistic regression models to examine which factors were significantly related independently of the other factors; and (iii) a time to event linkage analysis using Cox proportional hazard models to examine the relationship between EA and PPH in the subsequent five years.
The descriptive analysis included information captured at baseline, either in the baseline 45 and Up Study survey or from linked health utilisation data within the baseline period (+/− 12 months from date of recruitment to the 45 and Up Study). Descriptive analyses were undertaken to examine the proportion of people with a GPMP or TCA who had at least one allied health service claim by each characteristic of interest (socio-demographic, health risk factor, health status and health service utilisation).
Logistic regression was then used to examine which factors were significantly related to having at least one allied health service claim independently the other factors. All factors were included in the model.
Time to event linkage analysis, using Cox proportional hazard models, included information captured at baseline, either in the baseline 45 and Up Study survey or within the baseline period (+/− one year from date of recruitment to the 45 and Up Study), and hospital/emergency department admissions in the five-year period starting from the end of the baseline period (+/− one year from recruitment). The outcome investigated were PPH and EA. Follow-up commenced at the end of the two-year baseline period (ie, one year after recruitment to the 45 and Up Study). Outcomes were censored at first hospitalisation, death or five years (ie, six years after recruitment to the 45 and Up Study), whichever occurred first.
Results
Descriptive analysis
Of the 5771 CES residents who had claimed for a GPMP or TCA at baseline, 43% (2460) claimed for at least one allied health service within the next 12 months. Figure 1 shows the proportion of CES residents with a GPMP or TCA at baseline who claimed for allied health services within 12 months, by type of allied health service and age group. Older age groups had higher rates for claiming allied health services within 12 months of GPMP or TCA preparation (49% for 85 years and over compared to 38% for 45–59-year-olds). Claim rates were highest for: participants in nursing homes (55.6%), without extras private health insurance (49.9%), females (48.1%), less than high school education (46.3%), not working (45.4%) and low incomes (45.1%).

Figure 1. Proportion of Central and Eastern Sydney residents with a General Practice Management Plan/Team Care Arrangement at baseline who claimed for allied health services within 12 months, by type of allied health service and age group
There were clear differences in types of services claimed across age groups. Those in the youngest age group, 45–59 years, had higher claim rates for physiotherapy only (15%) or other allied health only (15%) (including but not limited to dietetics, exercise physiology, chiropractic services) compared to podiatry (4%). Those in the oldest age group (85 years and over) had higher claim rates for podiatry only (31%) compared to physiotherapy only (9%) and other allied health only (4%). Participants across all age groups had higher claim rates for any one service type compared to a combination of services (between 4% and 6% of participants claimed for a combination of physiotherapy, podiatry and/or other allied health) and 22.7% of participants claimed all five sessions within one year.
Regression model
This difference in claiming patterns among age groups is clear when viewed in separate logistic models that relate all patient characteristics with whether a participant claimed for each allied health service in the next 12 months (Figure 2). After controlling for all other factors, increasing age was positively related to the use of podiatry, with those aged over 85 years having more than four times the odds of claiming podiatry compared to those 45–59 years of age. Conversely, increasing age was inversely related to claims for both physiotherapy and other allied health, with those aged 85 years and over having only 0.4 the odds of claiming either physiotherapy or other allied health compared to those 45–59 years of age.
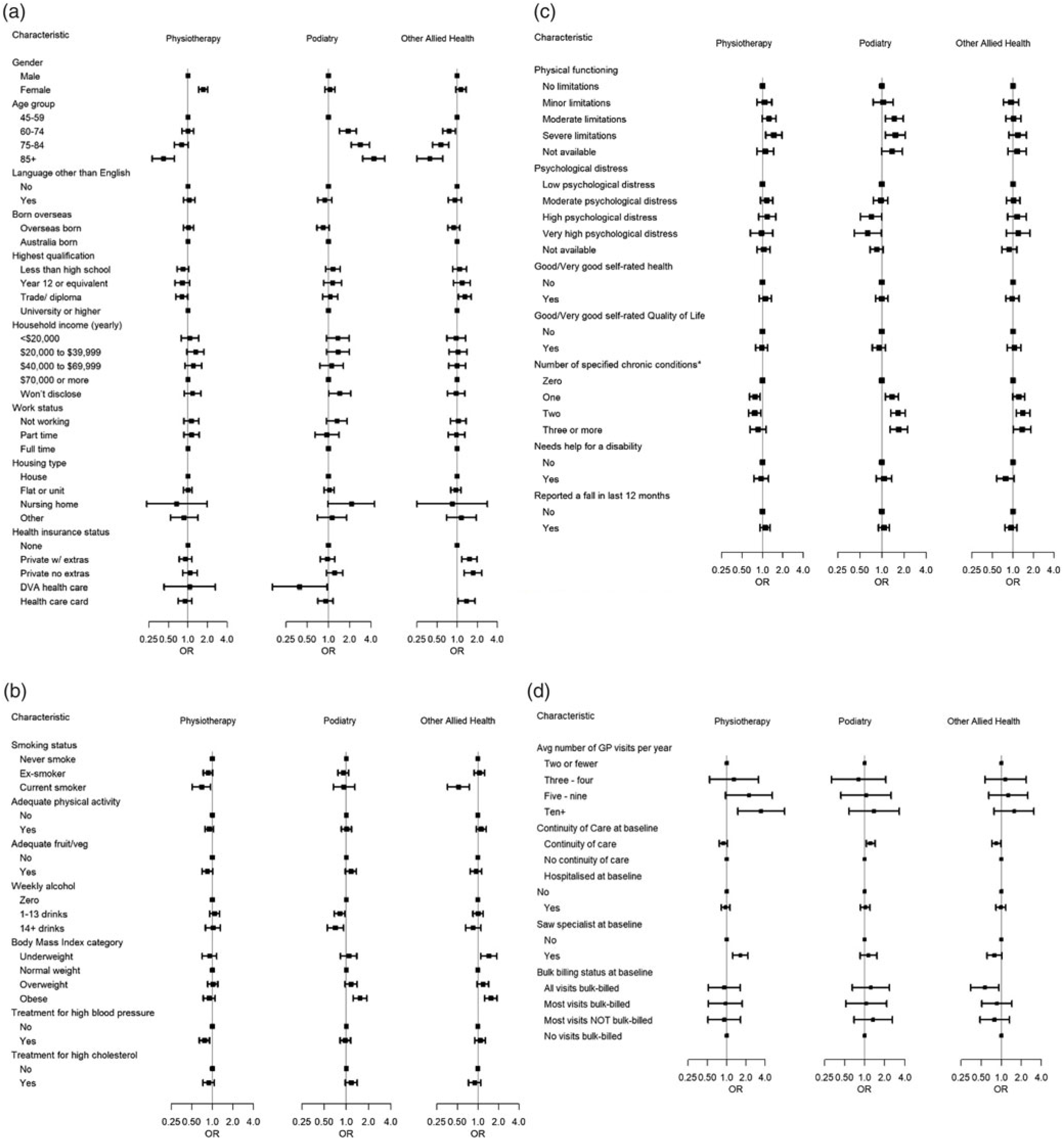
Figure 2. Adjusted Odds Ratios of claiming for Allied Health by (a) socio-demographic, (b) health risk, (c) health status and (d) health care utilisation factors adjusting for all other socio-demographic, health risk, health status and health care utilisation factors
Other characteristics associated with higher odds of claiming for allied health services, as shown in Figure 2, included: females compared to males for physiotherapy but not podiatry or other allied health; participants with a trade or diploma compared to a university degree for other allied health but not physiotherapy or podiatry; participants with private health insurance or who held a health care card compared to those who did not for other allied health but not physiotherapy or podiatry; participants who were obese compared to normal weight range for podiatry; participants who were obese or underweight for other allied health but not for physiotherapy; participants with increasingly severe physical limitations for both physiotherapy and podiatry but not for other allied health services; participants with more chronic conditions for podiatry and other allied health but not for physiotherapy; and participants who frequently saw a GP or who had seen a specialist at baseline for physiotherapy but not for podiatry or other allied health services.
Time to event linkage analysis
Table 2 provides the results of the model to examine the relationship between numbers of (i) physiotherapy claims, (ii) podiatry claims and (iii) other allied health claims, within 12 months of a GPMP or TCA, and time to first EA and first PPH, adjusting for other covariates.
Table 2. Relationship between numbers of (i) physiotherapy claims, (ii) podiatry claims and (iii) other allied health claims within 12 months of a General Practice Management Plan/Team Care Arrangement and time to (a) first subsequent emergency admission, and (b) first subsequent potentially preventable hospital admission, adjusting for other covariates

HR = hazard ratio.
a Significantly decreased hazard compared to ref category.
In the five-year period following recruitment, 2494 CES cohort participants had an EA. As shown in Table 2, after controlling for confounding factors such as socio-demographic, health risk, health status and health care utilisation, a significant difference was found between having five or more physiotherapy claims and no claims (Hazard Ratio 0.79; 95% CI 0.64–0.96), and experiencing a PPH in the subsequent five years. No statistical differences were found for podiatry claims. However, there was a difference between one to two other allied health claims and no claims (HR 0.78; 95% CI 0.65–0.94).
In the five-year period following recruitment, 1264 CES cohort participants had a PPH. As shown in Table 2, after controlling for confounding factors such as socio-demographic, health risk, health status and health care utilisation, a significant difference was found between having five or more physiotherapy visits and no visits (HR 0.79; 95% CI 0.64–0.96), and experiencing a PPH in the subsequent five years. No statistical differences were found for podiatry claims or for other allied health claims.
Discussion
We examined the allied health services claiming patterns among a cohort of CES residents who were being managed under a GPMP or TCA. Claiming patterns varied considerably by type of allied health service, which is consistent with previous findings (Cant and Foster, Reference Cant and Foster2011). For example, claiming physiotherapy was associated with being female and younger, and this was also found by Cant and Foster (Reference Cant and Foster2011). The current study had access to a much larger range of participant characteristics and found that claiming for physiotherapy was also associated independently with being a non-smoker, a frequent user of GP services and having more severe physical limitations but fewer of the six self-reported chronic conditions (cancer, diabetes, asthma, arthritis, cardiovascular disease and depression/anxiety). Those claiming for physiotherapy were also more likely to have seen a specialist at baseline – possibly as part of the TCA, although there is no way of determining whether a specialist was formally part of the TCA from the claims data alone.
The profile of those claiming podiatry was quite different. There was a strong association with age, with those aged over 85 years having more than four times the odds of claiming for podiatry compared to those aged 45–59 years. Claiming for podiatry was also associated with having more chronic conditions, being a non-drinker, being obese, having more severe physical limitations and having lower levels of psychological distress. This is consistent with older or obese people with mobility problems, as well as those with chronic conditions such as diabetes, being more likely to have significant need for help with foot care (Menz et al., Reference Menz, Gill, Taylor and Hill2008).
Claiming for other types of allied health services (including dietetics, exercise physiology and chiropractic services) was associated with being a non-smoker, being either obese or underweight, having an increasing number of chronic conditions, having some additional health cover (private or health concession card) compared to none and not being bulk-billed. While it was difficult to examine these items separately due to low numbers, this mixture of characteristics suggests there may be multiple drivers for accessing these types of allied health services that could be consistent with diet-related advice being sought for those with weight issues, but the link with health insurance status suggests there may be some patient-driven motivators that are unknown. Among those with a care plan, claiming for allied health services was not clearly related to socio-demographic disadvantage in terms of income, educational levels, ethnic background, housing type and work status. Further research may be required to better understand whether this is a patient or GP barrier in referral.
When considering the relationship between use of allied health services and subsequent EA and PPH, a possible protective effect was found with use of physiotherapy. Those with more claims for physiotherapy (five or more per year) had lower rates of EA and PPH compared to those who did not claim for physiotherapy. Physiotherapy provides a range of beneficial interventions to improve exercise capacity and quality of life and to reduce pain, while still addressing the presenting musculoskeletal, neurological or cardiothoracic conditions. In people with chronic obstructive pulmonary disease, pulmonary rehabilitation has been shown to reduce hospital admission and length of stay as well as improve participant health-related quality of life (McCarthy et al., Reference McCarthy, Casey, Devane, Murphy, Murphy and Lacasse2015). However, it is possible that accessing and completing a course of physiotherapy is a signal of some unmeasured aspect of a person’s overall health status. For example, it may reflect an underlying proactive health behaviour which also predisposes a person to lower risk of hospitalisation in addition to their age and number of chronic conditions.
There was no similar significant relationship with PPH or EA for the other types of allied health services, although there was a difference between one to two other allied health claims and no claims for EA which may need further exploration. It is possible that physiotherapy is helping significantly in the management of various conditions and thus preventing complications arising. Given the distinct differences observed in the profile of participants accessing the different types of services, it is a possibility that this is the case, although we attempted to address this by controlling for as many aspects of health status as possible. Also, we have no way of knowing whether the participants required additional allied health services but either went without, accessed them through outpatient clinics or paid for them themselves or via their private health insurance. Skinner et al. (Reference Skinner, Foster, Mitchell, Haynes, O’Flaherty and Haines2013), in their meta-analysis, found that having health insurance was generally associated with increased utilisation of allied health services; however, they found that the observed effects varied depending on the patient population, allied health provider and type of insurance product. Further research is required to establish whether the relationship we found is more or less protective when patient (eg, private health claims data) or local health service (eg, non-admitted patient data) funded allied health services are included via record linkage analysis.
Under the ‘Better Access to Mental Health Care Initiative’, which began in 2006, patients with mental health issues are currently eligible to receive up to 10 individual and up to 10 group allied mental health services per calendar year (Australian Government Department of Health, 2019). Evaluations of the programme have shown that the expanded services have had a substantial impact on the health of people with mental health issues (Littlefield, Reference Littlefield2017). Prior to 2006, all mental health services were included in the ‘up to five allied health services’ provided for in the TCA. The dose response observed for physiotherapy highlights that there may still be unmet needs, and so establishing a separate initiative for physiotherapy services which would not impact on other allied health needs may produce better outcomes as is the case for mental health services. Our findings are in line with what Foster et al. (Reference Foster, Mitchell, Haines, Tweedy, Cornwell and Fleming2008) predicted when they stated that ‘five subsidised sessions may not be adequate to facilitate improvement for some people, and will, we believe, often prevent allied health professionals providing care in line with recommended clinical guidelines’. The cost of the additional physiotherapy services could be met by expanding the CDM programme, through a specific initiative as was the case for mental health, or through local health services. Although allowing additional claims under the CDM programme has the potential to substantially increase the cost of this programme, it also has the potential to substantially decrease the need for subsequent hospitalisations and the associated costs.
The major strengths of the current study are the large community-dwelling population that reflects local users of the health system in the CES area of NSW, and the breadth of linked data that allow investigation of a wide range of participant characteristics with health service utilisation patterns Mealing et al. (Reference Mealing, Banks, Jorm, Steel, Clements and Rogers2010). The main limitations include the absence of clinically detailed data regarding a participant’s health state, and the lack of detail regarding the care plan, including the main purpose and conditions for which it has been put in place. Although informative, the results obtained from the cohort cannot be generalised to the CES population who are aged 45 years and over.
Conclusion
Use of allied health service CDM items in CES was well targeted towards those with chronic and complex care needs. Additionally, use of physiotherapy services was associated with less EA and less PPH. Expansion of the CDM programme so that GPs and patients do not have to choose between allied health services may improve outcomes.
Acknowledgements
This research was completed using data collected through the 45 and Up Study (www.saxinstitute.org.au). The 45 and Up Study is managed by the Sax Institute in collaboration with major partner Cancer Council NSW; and partners: the National Heart Foundation of Australia (NSW Division); NSW Ministry of Health; NSW Government Family and Community Services – Ageing, Carers and the Disability Council NSW; and the Australian Red Cross Blood Service. We thank the many thousands of people participating in the 45 and Up Study. We also wish to thank the staff at Centre for Health Record Linkage and all the data custodians for their assistance with data linkage.
Financial Support
This project was jointly funded by the Sydney Local Health District, the South Eastern Sydney Local Health District, and the Central and Eastern Sydney Primary Health Network.
Conflict(s) of Interest
None.
Authors’ Contributions
The project and analysis plan were developed by authors HW, EC, BH-R, EH, JL and MH as MB, JH, SW and CO’C joined the team later. The analysis was undertaken by HW. The first draft of the paper was written by MB and HW. All of the other authors (EC, BH-R, EH, JL, MH, JH, SW and CO’C) made comments on that draft and any further versions. MH also provided overall guidance and direction. All authors have read and approved the manuscript.
Ethical Standards
The authors assert that all procedures contributing to this work comply with the ethical standards of the relevant national and institutional guidelines on human experimentation (National Health and Medical Research) and with the Helsinki Declaration of 1975, as revised in 2008. Ethical Approval was granted for this research project by the NSW Population and Health Services Research Ethics Committee (Ref # 2016/06/642) and from the University of NSW Human Research Ethics Committee for the 45 and Up Study overall. Written (or Verbal) informed consent was obtained from all subjects/patients. Verbal consent was formally recorded for each participant by the Sax Institute who are the custodians of the 45 and Up Study.







