The promotion of physical activity in primary health care settings is considered an effective intervention for high-income countries (Orrow et al., Reference Orrow, Kinmonth, Sanderson and Sutton2012) and physical activity counseling is valuable in improving physical activity (The Activity Counseling Trial Research Group, 2001). However, a review published in 2012 showed that the mean effect size of interventions based on physical activity counseling given by professionals in primary health care settings is low (Heath et al., Reference Heath, Parra, Sarmiento, Andersen, Owen, Goenka, Montes and Brownson2012). Nevertheless, in countries with universal public health systems, this type of action can obtain good results for physical activity promotion, particularly given that such interventions have the potential to reach large proportions of the population.
In Brazil, the Unified Health System (or Sistema Único de Saúde, SUS in Portuguese) is public, universal, integral, decentralized and incorporates family health teams in over 85% of Brazilian cities (Paim et al., Reference Paim, Travassos, Almeida, Bahia and Macinko2011). The encouragement to undertake physical activity comprises one of the actions of the SUS for health promotion. Since 2006, the Brazilian Policy for Health Promotion and the health promotion network has worked closely with SUS in encouraging physical activity. Through a number of initiatives supported the Ministry of Health, such as the implementation of Family Health Support Units in 2008, and the ‘Health Gym Program’ in 2011 (or ‘Academia da Saúde’ in Portuguese) (Malta and Barbosa da Silva, Reference Malta and Barbosa da Silva2012), physical activity promotion within the SUS has been encouraged in primary health care. However, a recent survey involving a nationally representative sample of primary health care units showed that only 39.5% provided physical activity interventions or promotions (Ramos et al., Reference Ramos, Malta, Gomes, Bracco, Florindo, Mielke, Parra, Lobelo, Simoes and Hallal2014). However, despite those findings, it is interesting to note that a large proportion of physicians and nurses practicing at these primary care units have reported delivering regular physical activity counseling to their patients (Florindo et al., Reference Florindo, Brownson, Mielke, Gomes, Parra, Siqueira, Lobelo, Simoes, Ramos, Bracco and Hallal2013).
This disparity between physical activity promotion interventions and counseling in practice reveals both a discrepancy and an opportunity for development of a more strategic approach to physical activity promotion in these settings. Moreover, the majority of these professionals lack knowledge in the physical activity field, such as on the global recommendations for physical activity promotion (Florindo et al., Reference Florindo, Brownson, Mielke, Gomes, Parra, Siqueira, Lobelo, Simoes, Ramos, Bracco and Hallal2013). Therefore, tailored professional development training focused on health professionals is an unmet goal to improve physical activity counseling to attain greater population effect sizes to increase physical activity among the SUS users.
Since the 1900s a number of training programs for physical activity promotion counseling have been implemented and made available in range of countries. These include ‘Patient-Centered Assessment and Counseling for Exercise (PACE)’ in the Unites States (Calfas et al., Reference Calfas, Long, Sallis, Wooten, Pratt and Patrick1996; Long et al., Reference Long, Calfas, Wooten, Sallis, Patrick, Goldstein, Marcus, Schwenk, Chenoweth, Carter, Torres, Palinkas and Heath1996), as well as programs in other countries such as Japan (Miura et al., Reference Miura, Yamaguchi, Urata, Himeshima, Otsuka, Tomita, Yamatsu, Nishida and Saku2004), the Netherlands (van Sluijs et al., Reference van Sluijs, van Poppel, Stalman and van Mechelen2004), the ‘Green Prescription’ in New Zealand (Swinburn et al., Reference Schmid, Egli, Martin and Bauer1998; Elley et al., Reference Elley, Kerse, Arroll and Robinson2003). Noticably, the ‘Exercise is Medicine,’ initiative was launched in 2007 as a counseling strategy in the United States, and was also adopted elsewhere in other countries (Sallis, Reference Sallis2011; Blair et al., Reference Blair, Sallis, Hutber and Archer2012; Lobelo et al., Reference Lobelo, Stoutenberg and Hutber2014).
Through a European funded project titled ‘Healthy Europe Through Learning and Practice (HELP),’ a group of European researchers in 2012 developed an online training module for health professionals (Crone, Reference Crone2011). The aim of this project was to develop an online training program for physicians and nurses with the ambition to increase their confidence and knowledge in order to enable them to advise patients on healthy weight, healthy eating and the promotion of physical activity.
It is important for countries with national health systems to provide health professionals with training in promoting physical activity promotion (including counseling) that empowers them to promote physical activity in primary health care settings. In Latin American countries, there is a dearth of studies assessing physical activity interventions in primary health care (Hoehner et al., Reference Hoehner, Ribeiro, Parra, Reis, Azevedo, Hino, Soares, Hallal, Simões and Brownson2013). More specifically, in Brazil, studies proposing and assessing strategies for physical activity promotion counseling through training of health professionals are scarce. In response to this deficit, the Physical Activity Epidemiology Group at University of São Paulo developed a training model for physicians and nurses to support the provision of physical activity counseling. This was published as part of the physical activity promotion interventions in primary health care called ‘Active Environment’ (Florindo and Andrade, Reference Florindo and Andrade2015). The model developed for Brazil was based upon content from the ‘HELP’ project (Crone, Reference Crone2011). In addition, in continental countries such as Brazil, it is important that distance-learning-based educational training for health professionals can be evaluated by using online platforms. Therefore, the objective of this study was to investigate the perspectives and opinions of health professionals regarding the distance-learning physical activity training developed in a low socio-economic region of São Paulo city, Brazil.
Methods
This paper describes the perspectives and opinions of health professionals on a physical activity training called: ‘Active Environment.’ The training was part of the research project ‘Implementation of hospital integration strategies with the primary health care system in the health care outreach of M’Boi Mirim in São Paulo city.’ This project developed an educational intervention (a distance-learning course) that comprised five modules, each of eight weeks in duration. Content included the Brazilian Ambulatory Care Sensitive Conditions list: respiratory, cardiovascular, diabetes, gastroenterology and mixed infectious diseases (Alfradique et al., Reference Alfradique, Bonolo, Dourado, Lima-Costa, Macinko, Mendonça, Oliveira, Sampaio, Simoni and Turci2009), and major health risk factors including smoking, alcoholism, illegal drugs, pain, nutrition and physical inactivity.
The physical activity component was part of the risk factors module and was delivered during the last three weeks of the course. A full report of the methods is available in Bracco et al. (Reference Bracco, Mafra, Abdo, Colugnati, Dalla, Demarzo, Abrahamsohn, Rodrigues, Delgado, Dos Prazeres, Teixeira and Possa2016), but briefly, classes were delivered weekly, by specialists, through 1-h internet-based video-conferences which were followed by a discussion involving a general practitioner. All classes were transmitted online and were therefore interactive with the audience using the Adobe Connect™ interface, provided by the Hospital Israelita Albert Einstein. Health professionals could take part directly, but the recorded conferences were also made available at the course platform, which could be accessed at any time. In addition, discussion forums guided by mentors were also made available for discussions and for the provision of didactic support materials.
All staff (n=359), who included physicians, nurses and multi-professional staff, who were working at the municipal health system, involving primary care units (n=18) and Hospital Municipal Dr. Moyses Deutsch, managed by the Centro de Estudos e Pesquisas Dr. João Amorim (CEJAM), and the Hospital Israelita Albert Einstein, under a public-private partnership model. These primary care units form the regional health care network of M’Boi Mirim, a peripheral district in the southern zone of São Paulo city. Therefore, no sample size calculation was performed, but from 359 eligible health professionals, n=170 were enrolled in the course.
Physical activity training
As noted above, the physical activity component was called ‘Active Environment.’ It was based on both previous studies on physical activity promotion interventions in primary health care conducted in the eastern region of São Paulo city (Florindo and Andrade, Reference Florindo and Andrade2015) (www.each.usp.br/ambienteativo) and from the physical activity promotion content devised by the ‘Healthy Europe Through Learning and Practice’ project (http://www.help-project.com/).
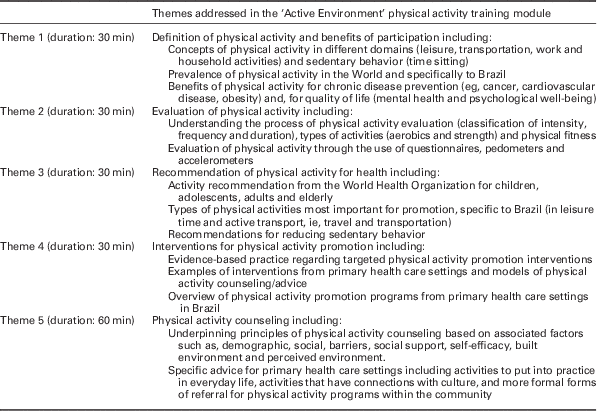
The duration of the training totaled 3 h, consisting of the five themes outlined in Table 1 applied over a three-week period. Themes 1 to 4 had duration of 30 min each, comprising 15 min of explanatory class and 15 min for discussion. Theme 5 had duration of 60 min, comprising 30 min of explanatory content and 30 min of discussion.
Table 1 Description of themes addressed in the physical activity training
Evaluation of physical activity training
To assess the opinion of health professionals about physical activity training we used two questions and to verify professional conduct for physical activity counseling we used one question (Table 2).
Table 2 Questions used for evaluation

These questions took part of the questionnaire completed by participants to evaluate the whole distance-learning course at the concluding session, held a month after the module containing the physical activity training (Bracco et al., Reference Bracco, Mafra, Abdo, Colugnati, Dalla, Demarzo, Abrahamsohn, Rodrigues, Delgado, Dos Prazeres, Teixeira and Possa2016). Questions were analyzed only in the group that accessed the fifth module (that had the physical activity training).
Discourse analysis (Bardin, Reference Bardin2011; Câmara, Reference Câmara2013) was used to analyze data from the two open questions (Table 2). We created categories from the answers about the positive points and suggestions to improve the training. We calculated how many times the responses that were contained in each category and each respondent may have cited responses for more than one category.
For the question about professional practice for physical activity counseling, the responses were analyzed using descriptive statistics (%) and thematically categorized in six options.
All data were analyzed using the Statistical Package for the Social Sciences (SPPS) version 22.0.
Ethical issues
The study was approved by the Research Ethics Committee of the Secretariat for Health of São Paulo city (permit CAAE 26981514.3.0000.0086). All professionals who took part in the study signed the Free and Informed Consent Form.
Results
Of the 170 who were enrolled in the course, 28 left their positions during the course. Of those that completed the course (n=142), 106 completed the final course evaluation after one year. Of the 106 professionals, 22.6% (n=24) accessed the fifth module (or watched some classes, or participated in the discussion forum).
The professionals who accessed the fifth module (n=24) were predominantly female (79%), nurses (67%), aged >30 years (75%), had been professionally practicing in the national health system for over five years (Table 3).
Table 3 Characteristics of health professionals that accessed the fifth module of course (major health risk factors) and answered the questions about physical activity training (n=24)

a One missing information.
b Two missing information.
We had 14 responses to positive points and 12 responses about negative points of the course (Table 4).
Table 4 Summary of positive and negative points reported by professionals who accessed the module containing the physical activity training

The professionals highlighted the course approach focused on patient’s quality of life and well-being, disease prevention and health improvements. Other important topics raised by health professionals were information about physical activity in the aging process, and treatment and rehabilitation of diseases (Table 4).
Regarding the themes for improvement, these included the need for physical activity classes for professionals to experience physical activity practice first-hand, and the need to link physical activity counseling to the local venues that provide structured physical activity programs (Table 4).
Discussion
This study’s objective was to report on the opinion of health professionals regarding an ‘Active Environment’ training to physical activity promotion as part of the research project ‘Implementation of hospital integration strategies with the primary health care system in the health care outreach of M’Boi Mirim in São Paulo city.’ The results showed that the positive points were the focus in well-being and quality of life and the prevention of diseases and health improvements. The training had good acceptability by the professionals who have accessed the module. However, only 24 health providers accessed the health risk factors module. Among them, a request for first-hand practical classes on physical activity and also a more specific link with counseling and local venues where activity takes place. These were the both identified as potential improvements.
This training was delivered as an internet-based distance-learning education model and had 3 h divided in three weeks (1 h/week). The main goal was to empower professionals by providing them with generalist content on physical activity and health for physical activity counseling in primary health care units.
Several interventions to empower professionals for physical activity counseling have employed a variety of strategies and contents. The ‘PACE’ intervention introduced in the United States in the 1990s (Calfas et al., Reference Calfas, Long, Sallis, Wooten, Pratt and Patrick1996; Long et al., Reference Long, Calfas, Wooten, Sallis, Patrick, Goldstein, Marcus, Schwenk, Chenoweth, Carter, Torres, Palinkas and Heath1996), a pioneering intervention for physical health promotion in primary health care, is based on 30–60 min training sessions. The sessions empower professionals to address the psychological and social factors influencing physical activity practice, such as social support of family and friends, self-efficacy or confidence, reduction of perceived barriers and raising awareness of the benefits of physical activity (Ainsworth and Youmans, Reference Ainsworth and Youmans2002; Calfas et al., Reference Calfas, Sallis, Zabinski, Wilfley, Rupp, Prochaska, Thompson, Pratt and Patrick2002; van Sluijs et al., Reference van Sluijs, van Poppel, Stalman and van Mechelen2004). The ‘Green Prescription’ intervention implemented in New Zealand recommends 4 h of training for health professionals on motivational techniques to encourage patients to practice physical activity independently, with particular emphasis on walking. Subsequently, these patients receive follow-up telephone calls from the physical activity professionals as motivational support, specific counseling on physical exercises and on local communities to practice group physical activity (Swinburn et al., Reference Schmid, Egli, Martin and Bauer1998; Elley et al., Reference Elley, Kerse, Arroll and Robinson2003). The ‘Exercise is Medicine’ intervention, established in 2007 by the American Medical Association and American College of Sports and Medicine, encompasses 6–8-h training courses based on behavioral models linked to primary health care, and also includes a clinical model for assessing, counseling and referring patients for physical activity programs at the community level (Sallis, Reference Sallis2011; Lobelo et al., Reference Lobelo, Stoutenberg and Hutber2014; Calle et al., Reference Calle, Lobelo, Jiménez, Páez, Cortés, Lima and Duperly2016).
A feature shared by some of these interventions is a scheme of counseling based on stages of change in behavior (Calfas et al., Reference Calfas, Long, Sallis, Wooten, Pratt and Patrick1996; Ainsworth and Youmans, Reference Ainsworth and Youmans2002; Lobelo et al., Reference Lobelo, Stoutenberg and Hutber2014). This was originally devised for behaviors deleterious to health such as smoking (Prochaska and Diclemente, Reference Prochaska and Diclemente1992) but later adapted to other health behaviors such as the physical activity (Dumith et al., Reference Dumith, Domingues and Gigante2008). Furthermore, physical activity counseling is based on social cognitive theory (Bandura, Reference Bandura1986), because physical activity participation includes multifactorial determinants (Bauman et al., Reference Bauman, Reis, Sallis, Wells, Loos and Martin2012).
The ‘Active Environment’ training for physicians and nurses was not based on closed, specific counseling models but seeks to empower health professionals to devise strategies according to their local practices, and to discuss and share ideas through the interactive forum. The social cognitive theory and stages of change in behavior are important because the ‘Active Environment’ works with overcoming barriers and social support to improve physical activity, as already shown in training for community health workers (Florindo et al., Reference Florindo, Costa, Sa, Santos, Velardi and Andrade2014). However, in Universal Health Systems implemented in large, culturally diverse countries like Brazil (Paim et al., Reference Paim, Travassos, Almeida, Bahia and Macinko2011), models must be adaptable to meet local conditions of health professionals. For example, Swiss-based study reported that for physicians a structured procedure could be adapted for physical activity counseling according to work conditions and realities of the primary health care units (Schmid et al., Reference Swinburn, Walter, Arroll, Tilyard and Russell2009).
With regard to improvements suggested by the professionals, there were calls for a link between the counseling delivered and public, structured physical activity programs, such as physical exercise classes. A pilot study to test the ‘Exercise is Medicine’ intervention showed that when the counseling for physical exercise was directly linked with referral of patients to a recreation centers, the average effect of increase in moderate-to-vigorous-intensity physical activity was larger compared with a group of patients receiving counseling alone after six months of the interventions (Heath et al., Reference Heath, Kolade and Haynes2015). In a national survey involving physicians and nurses working in primary health care in Brazil, Florindo et al. (Reference Florindo, Brownson, Mielke, Gomes, Parra, Siqueira, Lobelo, Simoes, Ramos, Bracco and Hallal2013) showed that the odds ratio of counseling on physical activity was higher when structured physical activity programs were provided at the primary health care units where the professionals were working. The ‘Green Prescription’ intervention does the link between primary health care (by general practitioners or nurses) with physical exercise specialists (Elley et al., Reference Elley, Kerse, Arroll and Robinson2003; Hamlin et al., Reference Hamlin, Yule, Elliot, Stoner and Kathiravel2016). And this support was considered positive by general practitioners that working in primary health care settings in New Zealand (Patel et al., Reference Patel, Schofield, Kolt and Keogh2011).
Clearly, physical activity promotion is an interdisciplinary field and physical activity is a habit that depends on numerous factors (Bauman et al., Reference Bauman, Reis, Sallis, Wells, Loos and Martin2012). For example, although 12 h of training in a group of community health workers improved knowledge and skills for physical activity promotion in a primary health care unit in the eastern region of São Paulo (Florindo et al., Reference Florindo, Costa, Sa, Santos, Velardi and Andrade2014), this outcome did not translate to changes in the level of physical activity among the population seen by these professionals (Costa et al., Reference Costa, Andrade, Garcia, Ribeiro, Santos and Florindo2015). Therefore, besides improving the knowledge of health professionals to counsel, counseling programs should also be linked with structured physical activity programs run within the communities where these practitioners operate and work. Brazil currently has a good setting to support this, particularly after implementation of the ‘Health Gym Program’ (Malta and Barbosa da Silva, Reference Malta and Barbosa da Silva2012), which can provide environments and specialized professionals to run physical exercise classes in partnership with primary care units.
Another suggestion was the incorporation of physical activity sessions for the health professionals themselves. Because the course was 100% distance-based this approach was not possible or envisaged. However, it is believed that in universal systems with multi-professional and interdisciplinary health teams such as Brazil (Paim et al., Reference Paim, Travassos, Almeida, Bahia and Macinko2011) that including a physical activity promotion professional within this team (Florindo et al., Reference Florindo, Salvador, Reis and Guimarães2016) would be a complement to this course can and as such is recommended from this study. Many studies have shown that health professionals practicing physical activity are more likely to counsel their patients, or to provide them with more counseling, on adopting physical activity (McDowell et al., Reference McDowell, McKenna and Naylor1997; Frank et al., Reference Frank, Elon and Hertzberg2007; Florindo et al., Reference Florindo, Mielke, Gomes, Ramos, Bracco, Parra, Simoes, Lobelo and Hallal2015; Santos et al., Reference Santos, Guerra, Andrade and Florindo2015). It is therefore important to also develop physical activity promotion interventions in primary health care settings for the self-care of the health professionals in addition to training, to support them in their work–life balance and mental well-being (Sá et al., Reference Sá, Velardi and Florindo2016). An intervention involving Community Health Workers in the eastern region of São Paulo city showed that physical activity can be linked with professional training for physical activity promotion counseling in the Unified Health System (Florindo et al., Reference Florindo, Costa, Sa, Santos, Velardi and Andrade2014; Florindo and Andrade, Reference Florindo and Andrade2015).
Another suggestion that was less cited, but equally important, was the inclusion of guides to advise on the different types of physical activities available, for differing population likes and also clinical appropriateness, to enhance take up, suitability and ultimately adherence. The inclusion of this topic can be important because this type of physical activity is varied, for example it can be undertaken in group which contributes to improvements in social support, and also type of activity related to patient preferences (Florindo et al., Reference Florindo, Nakamura, Farias Júnior, Siqueira, Reis, Cruz and Hallal2011). The focus on physical activity promotion through the social support of friends and family as well as the overcoming of barriers to practice is central part of all interventions suggested through the ‘Active Environment’ training course (Salvador et al., Reference Salvador, Ribeiro, Garcia, Andrade, Guimaraes, Aoki and Florindo2014; Costa et al., Reference Costa, Andrade, Garcia, Ribeiro, Santos and Florindo2015; Florindo and Andrade, Reference Florindo and Andrade2015).
Two positive points of the training included: (1) the focus on the relationship between physical activity and well-being/quality of life and (2) information on the prevention of disease and its role in health promotion. Beyond explanations of the biological benefits derived from physical activity practice, a focus on other variables related to well-being, such as improvement in perceived quality of life and psychological well-being related to intra- and interpersonal factors are important factor in interventions to promote physical activity within primary health care. This was deemed an important focus for physicians and nurses in physical activity counseling as the focus is often more related to the patient’s risk factors for diseases (Schmid et al., Reference Swinburn, Walter, Arroll, Tilyard and Russell2009; Patel et al., Reference Patel, Schofield, Kolt and Keogh2011) and not for prevention, health promotion and quality of life/well-being.
Other categories had less citations, but are worthy of note, for example the inclusion of additional topics such as healthy eating, and the role of physical activity in the aging process. In this case, we did not include a specific approach to these topics in the course, but they were worked in other themes of the fifth module regarding health risk factors (Bracco et al., Reference Bracco, Mafra, Abdo, Colugnati, Dalla, Demarzo, Abrahamsohn, Rodrigues, Delgado, Dos Prazeres, Teixeira and Possa2016). Other studies have adopted the training for physical activity and nutrition in the same intervention (Calfas et al., Reference Calfas, Sallis, Zabinski, Wilfley, Rupp, Prochaska, Thompson, Pratt and Patrick2002; Wilcox et al., Reference Wilcox, Parra-Medina, Felton, Poston and McClain2010) and this multidimensional focus is important for physicians in primary health care settings (Schmid et al., Reference Swinburn, Walter, Arroll, Tilyard and Russell2009).
The focus on physical activity promotion and the skills required to advise patients were however, less cited. In this case we need to improve these themes, because the main objective of the training is to develop the empowerment the health professionals for physical activity counseling, according to other interventions such as ‘PACE’ (Long et al., Reference Long, Calfas, Wooten, Sallis, Patrick, Goldstein, Marcus, Schwenk, Chenoweth, Carter, Torres, Palinkas and Heath1996; Ainsworth and Youmans, Reference Ainsworth and Youmans2002) and ‘Green Prescription’ (Elley et al., Reference Elley, Kerse, Arroll and Robinson2003; Hamlin et al., Reference Hamlin, Yule, Elliot, Stoner and Kathiravel2016). For this it is important to include practical counseling activities and examples of patients in primary health care settings during the three weeks of this training, as it is done in ‘Exercise is Medicine’ intervention (Calle et al., Reference Calle, Lobelo, Jiménez, Páez, Cortés, Lima and Duperly2016).
In addition, despite the high prevalence of physical activity counseling delivered by physicians and nurses in primary health care in Brazil (around 70%) (Florindo et al., Reference Florindo, Brownson, Mielke, Gomes, Parra, Siqueira, Lobelo, Simoes, Ramos, Bracco and Hallal2013), primary health care providers perceive that they lack adequate knowledge on physical activity and health (Hébert et al., Reference Hébert, Caughy and Shuval2012). A cross-sectional study in a sample of professionals working in primary health care in Brazil showed that knowledge on physical activity recommendations for health was generally poor, but when professionals had more interest in this area (in the case of nurses) or involved in more specific content such as assessing patients’ level of physical activity (in the case of physicians), the frequency of counseling increased (Florindo et al., Reference Florindo, Brownson, Mielke, Gomes, Parra, Siqueira, Lobelo, Simoes, Ramos, Bracco and Hallal2013).
This detracts from the quality of counseling and, although interventions in primary health care through counseling are effective for increasing physical activity in adults (The Activity Counseling Trial Research Group, 2001), the mean effect size of this type of intervention to improve physical activity is low (Heath et al., Reference Heath, Parra, Sarmiento, Andersen, Owen, Goenka, Montes and Brownson2012). The poor quality of counseling provided by physicians and nurses can contribute to this low effect size in community interventions. Thus, counseling in itself may not enough and must be of high quality in order to be effective.
The study had some limitations. First, only 22.6% of the professionals accessed the fifth module. Therefore, we had a large dropout and a small sample to analyses the responses. Nevertheless, in the other course modules the participation was also low, suggesting that education for health providers is still challenging, as previously identified by other studies (Cervero and Gaines, Reference Cervero and Gaines2015).
Second, we did not evaluate pre- and post-intervention regarding knowledge and skills for physical activity counseling of the health professionals that participated this training. We tried applied the questionnaire before of this training, but we had a very low response rate and not was possible analyzed the data. These variables are very important to assess the results of the education process and the empowerment of professionals and has been used in studies this field (Long et al., Reference Long, Calfas, Wooten, Sallis, Patrick, Goldstein, Marcus, Schwenk, Chenoweth, Carter, Torres, Palinkas and Heath1996; Calle et al., Reference Calle, Lobelo, Jiménez, Páez, Cortés, Lima and Duperly2016).
Third, it was not possible to examine barriers to the implementation of applying this physical activity training in practice. We tried to investigate possible barriers in the follow-up questionnaire (Bracco et al., Reference Bracco, Mafra, Abdo, Colugnati, Dalla, Demarzo, Abrahamsohn, Rodrigues, Delgado, Dos Prazeres, Teixeira and Possa2016) but as this was self-reported, often incomplete with missing responses it was not possible to determine this. Understanding the barriers is critical to the development of training in respect to physical activity counseling in primary health care settings (Long et al., Reference Long, Calfas, Wooten, Sallis, Patrick, Goldstein, Marcus, Schwenk, Chenoweth, Carter, Torres, Palinkas and Heath1996; van Sluijs et al., Reference van Sluijs, van Poppel, Stalman and van Mechelen2004; Patel et al., Reference Patel, Schofield, Kolt and Keogh2011; Hébert et al., Reference Hébert, Caughy and Shuval2012; Dacey et al., Reference Dacey, Arnstein, Kennedy, Wolfe and Phillips2013; Florindo et al., Reference Florindo, Brownson, Mielke, Gomes, Parra, Siqueira, Lobelo, Simoes, Ramos, Bracco and Hallal2013).
Finally, we used only two open questions after training to verify the opinion of professionals. Other studies had used specific questionnaires to assess the course satisfaction (Calle et al., Reference Calle, Lobelo, Jiménez, Páez, Cortés, Lima and Duperly2016) and individual face-to-face interviews (Patel et al., Reference Patel, Schofield, Kolt and Keogh2011) to verify the opinions of health professionals about physical activity training.
In addition to limitations, we have some challenges. The ‘Active Environment’ training followed an online model with different strategies including classes that were recorded, didactic material, in addition to forums with health professionals following recommendations that were pointed as effective in continuing medical education (Marinopoulos et al., Reference Marinopoulos, Dorman, Ratanawongsa, Wilson, Ashar, Magaziner, Miller, Thomas, Prokopowicz, Qayyum and Bass2007; Cervero and Gaines, Reference Cervero and Gaines2015). Wilcox et al. (Reference Wilcox, Parra-Medina, Felton, Poston and McClain2010) developed a method in CD-ROM for flexible and self-paced training and showed that the most of providers and nurses adopted the physical activity counseling for patients. However, Dacey et al. (Reference Dacey, Arnstein, Kennedy, Wolfe and Phillips2013) showed that two types of face-to-face health professional training that ranged one-day to two-and-a-half-day were effective to improve knowledge and confidence and to decrease barriers to promote a healthy lifestyle and to prevent risk factors. In addition, interventions considered effective as ‘PACE’ were started and are based in face-to-face training (Calfas et al., Reference Calfas, Long, Sallis, Wooten, Pratt and Patrick1996; Long et al., Reference Long, Calfas, Wooten, Sallis, Patrick, Goldstein, Marcus, Schwenk, Chenoweth, Carter, Torres, Palinkas and Heath1996). However, online training as ‘Active Environment’ enables to achieve a large number of health professionals in a short time. In this case, we need more studies to compare online and face-to-face training and also have the support of physical education professional in primary health care units that could help in physician and nurses training (Florindo et al., Reference Florindo, Salvador, Reis and Guimarães2016).
Another challenge is to assess the skill development to advise on the effectiveness of this physical activity training in patient’s behaviors. Most of the clinical trials that assessed ‘PACE’ and ‘Green Prescription’ interventions showed significant results to improve physical activity in adults (Calfas et al., Reference Calfas, Long, Sallis, Wooten, Pratt and Patrick1996; Swinburn et al., Reference Schmid, Egli, Martin and Bauer1998; Calfas et al., Reference Calfas, Sallis, Zabinski, Wilfley, Rupp, Prochaska, Thompson, Pratt and Patrick2002; Elley et al., Reference Elley, Kerse, Arroll and Robinson2003; Miura et al., Reference Miura, Yamaguchi, Urata, Himeshima, Otsuka, Tomita, Yamatsu, Nishida and Saku2004; Hamlin et al., Reference Hamlin, Yule, Elliot, Stoner and Kathiravel2016). This is an important criterion from ‘The Community Guide’ to evaluate public health interventions (Briss et al., Reference Briss, Zaza, Pappaioanou, Fielding, Wright-De Agüero, Truman, Hopkins, Mullen, Thompson, Woolf, Carande-Kulis, Anderson, Hinman, McQueen, Teutsch and Harris2000).
All these challenges provide practical implications to be addressed for the design, content and protocol of the ‘Active Environment’ physical activity training before it being applied across primary health care within Brazil. However, few studies of the implementation of such training in physical activity with health professionals are available in Brazil. The findings of this study provide insight for the Unified Health System for physical activity promotion and for other health systems in the world, that are similar to Brazilian health system, that are searching for the development of professional training for physical activity promotion by means of motivational interviews in primary health care settings.
Acknowledgments
A.A.F. thank the Conselho Nacional de Desenvolvimento Científico e Tecnológico – CNPq for the Research Productivity Grant (303527/2013-7) and the grant received from the Santander Universities/University of São Paulo/Bid 367/2013 for internship at the University of Porto/Portugal; M.M.B. thank the Fundação de Amparo à Pesquisa do Estado de São Paulo (FAPESP) for financial support of the research project ‘Implementation of hospital integration strategies with the primary care system, in the health care network of M’Boi Mirim, São Paulo city’ within the PPSUS (12/51228-9).
The authors thank the University of Gloucestershire for their support in the adaptation of the HELP modules used as part of this study; The authors also thank the health teams and managers of the Hospital Municipal Dr. Moyses Deutsch and the 18 primary care units enrolled in the study, the Center of Studies and Research Dr. João Amorim (CEJAM), the São Paulo Municipal Health Secretary, and the Hospital Israelita Albert Einstein Research and Teaching Institute (IIEP).
Conflicts of Interest
None.
Ethical Standards
The authors assert that all procedures contributing to this work comply with the ethical standards of the relevant national and institutional guidelines on human experimentation and with the Helsinki Declaration of 1975, as revised in 2008.









