Introduction
Treatment of pain and anxiety constitutes a key component of care, both in the prehospital as well as in-patient setting.Reference Gausche-Hill, Brown and Oliver 1 However, effective management of pain and anxiety is challenging in the uncontrolled prehospital environment due to concerns regarding the hemodynamic side effects and respiratory depressant effects of narcotic and benzodiazepine class medications.Reference Galinski, Ruscev and Gonzalez 2 These concerns are compounded in acutely injured patients who may have either injuries or comorbid conditions that render them particularly vulnerable to these side effects.
Ketamine hydrochloride is a potent dissociative hypnotic with both sedative as well as analgesic properties.Reference Moy and Le Clerc 3 Its use is not limited to pain control but can also be effective in the short-term management of the delirious or agitated patient.Reference Cole, Moore and Nystrom 4 , Reference Le Cong, Gynther, Hunter and Schuller 5 Although the drug was initially used widely, reports of dysphoric reactions resulted in a significant curtailment in its use, especially in the prehospital setting.Reference Strayer and Nelson 6 However, use of ketamine has become more common following recent research in the military setting, regarding its relative safety and effectiveness in managing acute pain with no significant hemodynamic and respiratory depressant side effects.Reference Shackelford, Fowler and Schultz 7 , Reference Butler, Kotwal and Buckenmaier 8
Although anecdotal evidence suggests increasing use, there are no large studies evaluating the prevalence of ketamine use, the indications for which ketamine use is permitted, and the perception of associated adverse effects among paramedics in the US. The purpose of this study was to evaluate and describe training, use, and perceptions of outcomes associated with administration of ketamine by paramedics nationally.
Methods
Study Design and Setting
A cross-sectional survey of ketamine use by nationally certified paramedics (NRPs) was performed. To determine the number of responses needed to make estimates with 95% confidence, an a priori sample size calculation was performed. Given that differences between groups are most difficult to detect when one-half of the population has the exposure of interest, a 50/50 split was used in the calculation. A conservative three percent margin of error was assumed, and it was determined that at least 1,056 responses would be needed. Given the low expected response rates common to most survey research, 64,519 NRPs with valid email addresses included in the National Registry of Emergency Medical Technicians (NREMT; Columbus, Ohio USA) database at the time of this investigation were invited to participate in the study.
Study Instrument and Variable Description
A questionnaire was designed to assess the prevalence of ketamine training, its use among different patient populations (pediatric versus adult), indications for administration of the drug, route of administration of the drug, and perceived side effects of the drug among paramedics. Before administering the questionnaire electronically, cognitive testing was conducted with eight practicing paramedics to assess readability and consistency in interpretation of the items.
The final questionnaire consisted of 29 items. Respondents were asked to indicate what type of training they had received about ketamine, whether their main Emergency Medical Services (EMS) agency’s protocols allow for the use of ketamine in the prehospital setting, and for which patient population(s) its use was permitted. Next, those whose protocols allowed for the use of ketamine were asked to indicate for which applications its use was permitted (pain management, rapid sequence intubation [RSI], chemical restraint/sedation, or procedural sedation). Permitted routes of ketamine administration were also assessed (intravenous [IV], intramuscular [IM], or intranasal [IN]). The next section of the questionnaire asked respondents to report their experience with administration of ketamine to patients, including how many times and for what reasons they had used ketamine, their perception of success of the medication, their comfort level with use, and if they would use ketamine again. Success of medication use was defined as successful (very successful or successful) or unsuccessful (neutral, unsuccessful, or very unsuccessful). Comfort in administrating ketamine was on a five-point scale dichotomized as comfortable (very comfortable or comfortable) or uncomfortable (neutral, uncomfortable, or very uncomfortable). Respondents were also asked if any patient had experienced an adverse event following the administration of ketamine, including laryngospasm, excessive salivation, emergence reactions, respiratory depression, myoclonic activity, nausea, and vomiting.
Employment characteristics assessed included: community size served; primary role of the respondent; agency type (fire-based, hospital, private, government, and tribal); primary service provided (911 with transport capability, 911 without transport capability, hazmat, medical transport [convalescent], specialty care transport, rescue, paramedic intercept, air medical, and other); agency size; and volunteer status.
Data Collection and Analysis
Data collection was carried out from July-September 2015. Randomly selected paramedics in the NREMT database who held current National EMS Certification were sent an email with an invitation to complete the electronic questionnaire. The initial email contained an explanation of individuals’ rights as a participant and that participation in this study was completely voluntary with no impact to one’s National EMS Certification. Follow-up emails were sent at one and two weeks after the initial invitation. Data were collected using Snap10 survey software (Snap Surveys Ltd; Portsmouth, New Hampshire USA). No identifying information was collected by the survey software. This project was approved by the Institutional Review Board of the American Institutes of Research (Washington, DC USA) and a waiver of consent was granted.
For data analysis, inclusion criteria consisted of paramedics who held one or more state paramedic credentials, indicated “patient care provider” as their primary role, and worked in non-military settings. Only completed surveys were used for analysis. Descriptive statistics were calculated using Stata 12 (StataCorp LP; College Station, Texas USA).
Results
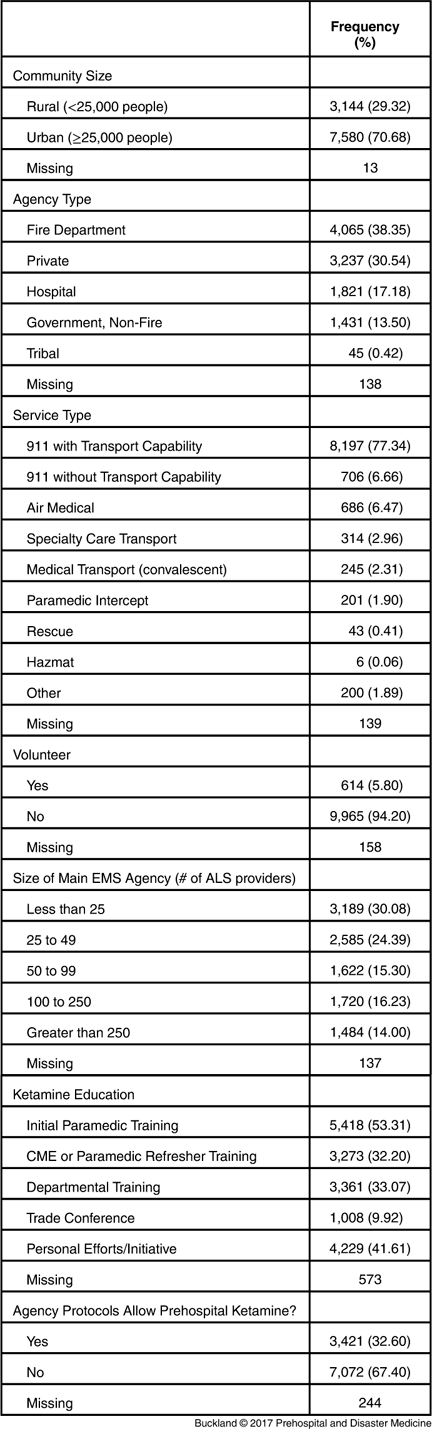
A total of 14,739 responses were obtained (response rate=23%), of which 10,737 (73%) met inclusion criteria and constituted the study cohort. The geographic distribution of respondents matched the NRP population. 9 Seventy-one percent of respondents (n=7,580) worked in an urban setting (Table 1). Thirty-eight percent (n=4,065) of respondents worked for a fire department, while 31% (n=3,237) worked for a private ambulance company. The remainder were hospital-based (17%; n=1,668), non-fire governmental agency employed (13%; n=1,309), or worked for a tribal EMS agency (0.4%; n=42). Seventy-seven percent of providers (n=8,197) responded to 911 calls and had transport capability, while seven percent (n=706) responded to 911 calls but did not have transport capability from the scene. An additional six percent (n=686) were aeromedical responders. Only six percent (n=614) were volunteers at their main EMS job. Slightly over one-half (54%; n=5,774) of respondents worked in an organization that employed less than 50 Advanced Life Support (ALS) providers.
Table 1 Demographic Profile of Respondents to the Survey (n=10,737)

Abbreviations: ALS, Advanced Life Support; CME, continuing medical education; EMS, Emergency Medical Services.
In regards to education related to ketamine, 53% (n=5,418) of respondents reported learning about ketamine during their initial paramedic program, while 32% (n=3,273) had received education on the drug as a part of a paramedic refresher or continuing medical education, and 33% (n=3,361) as a part of an intradepartmental training event. Interestingly, 42% of respondents (n=4,229) stated that they had sought education on ketamine independently. Around five percent (n=573) of respondents did not mark any of the training types listed.
Thirty-three percent (n=3,421) of respondents reported that their agency allowed prehospital use of ketamine (Table 1). Of those respondents that had protocols allowing ketamine administration, approximately two-thirds (65%; n=2,184) stated that they were authorized to administer the drug to both adult and pediatric patients, while 34% (n=1,134) stated that they could only administer ketamine to adult patients (Table 2). Only one percent (n=33) of respondents stated that use of the drug was restricted to pediatric patients at their agency. Of those who were authorized to administer ketamine to adults, 66% (n=2,171) stated that they did not need online medical control approval prior to administering the drug, 13% (n=427) did need online approval, and the remaining 21% (n=712) stated that ketamine was a standing order for some uses. Of those who were authorized to administer ketamine to pediatric patients, a slightly smaller number (61%; n=1,355) stated that they did not need online medical control approval prior to administering the agent, 20% (n=445) stated that they did need medical control approval, and the remaining 19% (n=410) stated that the ketamine was a standing order for specified uses.
Table 2 Authorized Population, Clinical Application, and Administration Route of Ketamine Reported by Paramedics with Protocols to Use Ketamine in the Prehospital Setting (n=3,421)Note: Respondents were able to select multiple options; thus, item counts are not summative.

The most commonly authorized clinical uses of ketamine were RSI (72%; n=2,417) and chemical restraint/sedation (71%; n=2,377). Ketamine was also authorized for use as an analgesic agent (55%; n=1,849) and least commonly authorized for procedural sedation (31%; n=1,044). Nearly all respondents authorized to give ketamine reported being allowed to administer the drug by the IV route (94%; n=3,148), and 65% (n=2,181) were allowed to perform IM administration (Table 2). Only 18% (n=598) of respondents were allowed to administer the agent via an IN route.
Two-thirds of respondents who were authorized to use ketamine reported administering the drug at least once in their EMS career (67%; n=2,243; Table 3). Only 20% (n=651) had used ketamine more than 10 times. Respondents most frequently used ketamine for RSI (61%; n=1,366) and chemical restraint/sedation (55%; n=1,235).
Table 3 Reported Practices of Paramedics Who were Authorized to Administer Ketamine in the Prehospital Setting (n=3,421)

a Respondents were able to select multiple options; thus, item counts are not summative.
Ketamine was perceived by nearly all respondents to be successful when used (96%; n=2,156), while only 14% (n=321) of respondents reported ever experiencing an adverse patient event after administration (Table 3). The most commonly reported adverse events included emergence reactions (four percent of respondents ever administering ketamine; n=98) and respiratory depression (four percent; n=90). Only one percent (n=22) of respondents who had ever administered ketamine reported that a patient experienced laryngospasm.
While most paramedics in this study had limited experience with ketamine, 94% (n=2,106/2,245) felt comfortable administering the drug (Table 3). Ninety-five percent (n=2,132) stated they would use the drug again in a similar circumstance.
Discussion
This was the first large, national survey to assess ketamine training, use, and perceptions among paramedics in the civilian prehospital setting. Historically, paramedics have been trained to administer parenteral narcotic and benzodiazepine medications for analgesia and sedation that may have significant depressant effects on respiratory drive, airway maintenance, and blood pressure. As prehospital providers often encounter unstable patients without hemodynamic reserve, options beyond narcotics and benzodiazepine medications to manage these situations are needed. Ketamine hydrochloride is a dissociative hypnotic agent with additional analgesic properties which has been used increasingly in emergency departments.Reference Moy and Le Clerc 3 Due to its powerful analgesic and sedative properties and lower frequency of adverse effects, the use of ketamine may be advantageous in the prehospital setting.Reference Butler, Kotwal and Buckenmaier 8 , Reference Scheppke, Braghiroli, Shalaby and Chait 10 - Reference Svenson and Abernathy 13
This study demonstrated that many paramedics received training in the use of ketamine, but only one-third of respondents were authorized to use ketamine at their agency. Ketamine was perceived to be safe and effective as the vast majority of paramedics reported that they are comfortable with the use of ketamine (94%) and would, in similar situations, use it again (95%).
As ketamine use in the prehospital setting has expanded, training for prehospital providers has increased. Released in 2016, the National Continued Competency Program update included ketamine training as part of the requirements to renew National Paramedic Certification. 14 Around one-third of providers reported receiving ketamine training through paramedic refresher or departmental training. However, the most commonly reported setting for receiving ketamine education was through initial paramedic training (53%). Interestingly, nearly one-half of respondents had taken initiative on their own to learn about the drug, suggesting that there is strong interest among prehospital providers regarding ketamine.
Despite the high prevalence of education related to ketamine, it is interesting that only around one-third of NRPs were authorized to administer the drug. The most commonly authorized indications for ketamine use were RSI and chemical restraint or sedation. This is consistent with the recommendation from the American College of Emergency Physicians (Irving, Texas USA) Out-of-Hospital Use of Analgesia and Sedation 2015 Policy Statement suggesting the use of ketamine for both of these indications. 15
Even though one-third of respondents were authorized to administered ketamine, their providers did not use the drug frequently. Approximately one-third of providers had never given the drug, while another one-third had administered the drug fewer than five times. A potential barrier to ketamine use noted through this study was that only 18% of providers authorized to use ketamine were allowed to administer the drug IN. In the military setting, the Committee for Tactical Casualty Care has recommended the use of IN ketamine in situations where IV access is challenging.Reference Butler, Kotwal and Buckenmaier 8 In randomized controlled trials, IN ketamine has been demonstrated to result in significant pain reduction compared to placebo with few adverse events.Reference Jennings, Cameron and Bernard 16 , Reference Carr, Goudas and Denman 17 With this information in mind, the use of IN ketamine in civilian prehospital protocols should be assessed.
Interestingly, adverse events were perceived by 14% of providers who had administered ketamine, but the overall frequency of adverse events was not assessed in this study. The most severe adverse event reported, laryngospasm, was reported by only one percent of all respondents who had ever administered ketamine in the prehospital setting. A study of over 8,000 patients similarly found a very low incidence of this adverse event with no identifiable risk factors to identify a particularly vulnerable cohort.Reference Greene and Williams 18 The most commonly reported adverse event, a dysphoric emergence reaction, is a known side effect of ketamine. While these reactions can be notably difficult to manage, they are typically avoidable with the use of appropriate dosages of ketamine as well as the addition of low dose midazolam.Reference Sener, Eken, Schultz, Serinken and Ozsarac 19 , Reference Newton and Fitton 20 Despite perceived adverse events among some providers, nearly all paramedics felt comfortable with administering ketamine and 95% reported that they would administer ketamine again under similar circumstances.
Limitations
This evaluation utilized a national questionnaire to assess ketamine training, use, and perceptions among paramedics. As a survey, it suffers a common limitation of response bias. Although there were a large number of responses, the overall response rate was low, consistent with most electronic surveys in this population.Reference Hoyle, Crowe, Bentley, Beltran and Fales 21 However, based on the sample size calculation, more than enough responses were received to make estimates with 95% confidence. Further, the geographic distribution of respondents was similar to the distribution of NRPs across the United States. 22 Employment characteristics of respondents to this questionnaire were consistent with those of respondents to the 2014 National EMS Practice Analysis, a population representative of NRPs in the US. 23 For example, in this study, 29% of paramedics worked in a rural setting compared to 30% of paramedics in the 2014 practice analysis population. Similarly, 38% of these respondents worked for fire-based agencies and 31% at private agencies compared to 36% and 30% of the 2014 practice analysis population, respectively. Further, as with all studies requiring self-reflection and report, there is a potential for recall bias. Nevertheless, it is unlikely that the bias in reporting would be systematic concerning the use of ketamine.
This cross-sectional study is also unable to comment on the clinical effectiveness of ketamine, the prevalence of conditions encountered by EMS providers that would benefit from ketamine use, or the incidence of adverse events. Further, the proportion of ketamine use versus other medications (eg, midazolam, etomidate, or fentanyl) for pain management, chemical restraint/sedation, RSI, and procedural sedation was not assessed in this evaluation. A prospective study whose primary endpoint involves measuring ketamine use and adverse events in a large sample size would be required to evaluate this question.
Conclusion
This was the first large, national survey to assess ketamine training, use, and perceptions among paramedics in the civilian prehospital setting. Many paramedics received training in the use of ketamine, but only one-third of respondents were authorized to use ketamine in their agency. When used by these paramedics, ketamine was perceived to be safe and effective as the vast majority reported that they are comfortable with the use of ketamine and would, in similar situations, use it again. Future studies are needed to determine the safety and efficacy of ketamine use in the prehospital setting.
Acknowledgements
The authors would like to acknowledge the contributions of Melissa A. Bentley, PhD to the development and deployment of this project.