Introduction
There is a large body of published research relating to depression in residential homes for older people (also called long-term-care homes, and including both nursing homes and hostels) (Ames Reference Ames1990; 1993; Seitz et al., Reference Seitz, Purandare and Conn2010; Snowdon and Purandare, Reference Snowdon, Purandare, Ames, Burns and O'Brien2010; Snowdon, Reference Snowdon2010). However, despite increased detection and more frequent treatment in recent years, depression remains a significant problem for many older people living in such settings. This guest editorial summarizes current knowledge about prevalence, etiology, detection and screening, treatment and outcomes of depression in residential homes and concludes with a summary of key issues requiring urgent future action.
Residential care homes for older people
The provision of residential homes for older people varies markedly around the world and there is no universal agreed definition for these facilities, which include both hostels and nursing homes (also known in some places as low-level and high-level care) and are sometimes referred to as long-term care facilities (Ribbe et al., Reference Ribbe1997; Snowdon and Purandare, Reference Snowdon, Purandare, Ames, Burns and O'Brien2010). Nursing homes can be defined as residential facilities offering 24-hour nursing care, while hostels can be considered as facilities that offer personal care and social involvement for people who can no longer manage at home, but need no more nursing care than could be provided by visiting nurses (Ribbe et al., Reference Ribbe1997). Using these definitions, 3.63% of Americans aged over 65 years were in nursing homes in 2004 (National Nursing Homes Survey, 2004), while the UK provision of all residential home beds was 450,000 in 2000, but is expected to rise to 1.1 million by 2051 (Wittenberg et al., Reference Wittenberg, Comas-Herrera, Pickard and Hancock2004). Australia has a total population of 22 million (just over one-third that of the UK and less than two-thirds of the US state of California) with a lower percentage aged over 65 than most European countries, but 162,300 Australians were living in mainstream residential care services in mid-2009, an increase of 2050 residents over the previous year (Australian Institute of Health and Welfare, 2010).
Depression: definitions and diagnosis
The term “depression” can refer to both depressive disorders and depressive symptoms. In modern research and clinical practice, diagnoses of depressive disorders are made most often using either the criteria of the World Health Organization's International Classification of Diseases, 10th revision (ICD-10; World Health Organization, 1992) or the American Psychiatric Association's Diagnostic and Statistical Manual, 4th edition (DSM-IV; American Psychiatric Association, 1994).
The ICD-10 mandates diagnosis of a depressive episode when four or more of the following ten symptoms are present most of the day, most days for at least two weeks in the absence of another disorder (e.g. hypothyroidism, schizophrenia, dementia, etc.) that could better account for the symptoms: low mood, loss of interest and enjoyment (anhedonia), disturbed sleep, decreased or increased weight or appetite, loss of energy, psychomotor slowing, poor concentration, feelings of guilt or self reproach, recurrent thoughts of death or suicide, and loss of confidence (World Health Organization, 1992). In the DSM-IV, five of nine of the above symptoms (excluding loss of confidence) must be present for the same two-week period for a diagnosis of major depressive disorder to be confirmed (American Psychiatric Association, 1994). Both systems require that the symptoms cause clinically significant stress or impairment in social, occupational or other important areas of functioning.
Milder forms of depression that do not fulfill criteria for ICD-10 depressive episode or DSM-IV major depression are common, often comorbid with other illnesses or recent bereavement, and frequently are of substantial clinical significance. These are sometimes referred to as minor depression, dysthymic disorder (if present chronically for two years) or depressive symptoms (Ames, Reference Ames1993).
Prevalence and incidence of depression in residential care homes for older people
Prevalence of depression in residential care homes is high, ranging from 4% to 25% for major depressive disorder and 29% to 82% for minor depression or the presence of depressive symptoms (Seitz et al., Reference Seitz, Purandare and Conn2010). A recent review by Seitz and colleagues (2010), published in this journal, examined 74 studies on prevalence of psychiatric disorders in nursing homes, including 26 on depression. Dementia, depression and anxiety were the most common psychiatric disorders affecting older people in long-term care. A range of instruments was used to assess depression in the 26 studies cited, making it difficult to determine prevalence more precisely than the wide ranges cited above. The Geriatric Depression Scale (GDS) was used in 12 studies but three different versions were used with a range of cut-off points (Seitz et al., Reference Seitz, Purandare and Conn2010). See Table 1 for a summary of selected prevalence studies.
Table 1. Selected studies on prevalence of depression in residential homes

AGECAT = Automated Geriatric Examination for Computer Assisted Taxonomy; CES-D = Centre for Epidemiological Studies Depression; CSDD = Cornell Scale for Depression in Dementia; DRS = Depression Rating Scale; GDS = Geriatric Depressive Scale; GDS-SF = Geriatric Depressive Scale-Short Edition; GMS = Geriatric Mental State; HDRS = Hamilton Depression Rating Scale; MDS = Minimum Data Set; MMSE = Mini-Mental State Examination; SCID = Structured Clinical Interview for DSM-III
In most countries prevalence of depression in residential homes is substantially higher than among community-dwelling older people, particularly in the case of major depression. Junginger and colleagues (Reference Junginger, Phelan, Cherry and Levy1993) found that 21% of their sample living in nursing homes in the USA had major depression compared with 10% of community-dwelling older people. Similarly, a British study found a 9.3% prevalence of major depression in community-dwelling older people, compared with 27.1% in nursing homes (McDougall et al., Reference McDougall, Matthews, Kvaal, Dewey and Brayne2007). However, in the latter study, there was a similar prevalence of minor depression in community–dwelling and nursing home residents (26.7% compared with 22.6%).
One apparently contradictory Korean study found greater prevalence of depression in older people living in their own homes, with 39.5% showing symptoms of depression compared with 24.0% of nursing home residents (Chung, Reference Chung2008). In this study, nursing home residents had significantly higher function in instrumental and personal activities of daily living (ADL), fewer children and more friends than community-dwelling older people. Functional ADL status is associated with depression (see Etiology section below) so this may explain this finding, which is out of line with most published comparative research. In addition, Korean cultural expectations of filial piety probably mean that older people with children are more likely to be cared for at home, regardless of their functional dependence.
The incidence of depression appears to be approximately 5–6% for new cases of both major and minor depression over a 6–12 month period (Parmelee et al., Reference Parmelee, Katz and Lawton1992b; Smalbrugge et al., Reference Smalbrugge, Jongenelis, Pot, Eefsting, Ribbe and Beekman2006a). Progression from minor to major depression may be higher, with one study finding 16.2% of people with minor depression progressing to major depression over a 12-month period (Parmelee et al., Reference Parmelee, Katz and Lawton1992b).
Etiology of depression
A number of factors contribute to depression in residential care homes, but no single factor can be considered the sole cause of depressive symptoms in most residents. Nor does any single factor (or combination of factors) have the same effect on different individual residents. The evidence indicates that variables including the types of homes; the education and training levels of staff; the personality, attitudes and coping strategies of residents themselves; resident health status (psychological health, physical disability/comorbidity and levels of function and dependence); social support; and length of time in care all have the potential to influence symptom expression.
Physical and mental health
In a review article one of the present authors (Ames, Reference Ames1993) noted that physical disability was strongly associated with depression, but emphasized the need for further studies to identify and define other risk factors. Medical comorbidities and functional impairment have emerged as important risk factors in a number of subsequent studies (Henderson et al., Reference Henderson, Korten, Jorm, Christensen, Mackinnon and Scott1994; Hyer et al., Reference Hyer, Carpenter, Bishmann and Wu2005; Segal, Reference Segal2005; Watson et al., Reference Watson2006). Persistent pain also has been identified as a major risk factor, affecting both mood and quality of life (Cuijpers and Lammeren, Reference Cuijpers and Lammeren1999; Asghari et al., Reference Asghari, Ghaderi and Ashory2006). Medications for a number of comorbid conditions (e.g. anti-hypertensive/cardiac drugs; treatment for Parkinson's disease, antineoplastic drugs and certain antibiotics) may also cause depression or produce depressive symptoms (Garavaglia, Reference Garavaglia2004).
The medical conditions listed by Hyer et al. (Reference Hyer, Carpenter, Bishmann and Wu2005) include those whose symptoms may overlap with those of depression, and indicate a high correlation between dementia and depression. This correlation is reported in a number of other studies (Gruber-Baldini et al., Reference Gruber-Baldini, Zimmerman, Boustani, Watson, Williams and Reed2005; Sheehan et al., Reference Sheehan, D'Souza, Nwe and O'Malley2007), though it is difficult to determine cause and effect. A history of previous depression is one of the best predictors of manifest depression in residents of care homes for older people (Payne et al., Reference Payne2002), and better cognitive functioning increases levels of risk of depression when associated with loss of physical function and capacity to live independently (Jones et al., Reference Jones, Marcantonio and Rabinowitz2003; Tsai et al., Reference Tsai, Chung, Wong and Huang2005). Jones et al. (Reference Jones, Marcantonio and Rabinowitz2003) also identified Parkinson's disease and heart disease as risk factors, although medication for these conditions may be implicated too (Garavaglia, Reference Garavaglia2004).
Other studies have noted relationships between depression and loss of perception, as in hearing loss (Eisses et al., Reference Eisses, Kluiter, Jongenelis, Pot, Beekman and Ormel2004) and uncorrected refractive error affecting vision (Owsley et al., Reference Owsley, McGwin, Scilley, Meek, Seker and Dyer2007). A further study identified a relationship between depression and malnutrition (Smoliner et al., Reference Smoliner, Norman, Wagner, Hartig, Lochs and Pirlich2009) though no clear pathway of causality was apparent.
Individual personality, social history, attitudes and coping strategies
Loss, a major factor in admission into residential care homes, is strongly associated with depression. Personal loss encompasses grief over the death of loved ones, loss of home, pets, social support and close friends; loss of function and control over the body; loss of independence and autonomy; and loss of the familiar (Hyer et al., Reference Hyer, Carpenter, Bishmann and Wu2005; Pot et al., Reference Pot, Deeg, Twisk, Beekman and Zarit2005; Zeiss, Reference Zeiss2005; Choi et al., Reference Choi, Ransom and Wyllie2008). An important factor is the loss of control over one's own destiny (Krach et al., Reference Krach, DeVaney, DeTurk and Zink1996). Personal coping styles and attitudes are important in explaining why some people are more negatively affected than others by loss and the presence of death. Cataldo (Reference Cataldo1994) found “non-hardiness and health-limiting death attitudes” to be reliable predictors of depression, and staff in another study identified social withdrawal (related to despair, loss, grief, loneliness and isolation) as a key indicator of depression (Choi et al., Reference Choi, Wyllie and Ransom2009). Lack of assertiveness is likely to lower defenses against institutional risk factors (Segal, Reference Segal2005). Higher education levels also correlate with greater likelihood of being depressed in long-term care (Eisses et al., Reference Eisses, Kluiter, Jongenelis, Pot, Beekman and Ormel2004), especially when associated with loss of mobility, function and independence.
Residential care home environments
Institutional factors that may contribute to depression include loss of privacy and frustration over shared rooms, noise, institutional furniture and odors, lack of stimulating social programs, lack of close relationships, high turnover rate of staff with little training and many cultural and educational differences, and other frustrations of living in close quarters with strangers under an institutional regime (Hyer et al., Reference Hyer, Carpenter, Bishmann and Wu2005; Choi et al., Reference Choi, Ransom and Wyllie2008). The medicalized environment of residential home settings and lack of alternative approaches to care have also been identified as depression risk factors (Garavaglia, Reference Garavaglia2004; Zeiss, Reference Zeiss2005), as has the constant presence of death (Cataldo, Reference Cataldo1994).
Length of time in care
The evidence suggests that the influence of length of time in care is different for cognitively impaired residents, and more likely to be a negative for the well-being of those without cognitive impairment (Stout et al., Reference Stout, Wilkin and Jolley1993; Pot et al., Reference Pot, Deeg, Twisk, Beekman and Zarit2005). Many residents admitted with dementia have undiagnosed depression (Sheehan et al., Reference Sheehan, D'Souza, Nwe and O'Malley2007), which is likely to improve if diagnosed and treated on and after admission (Masand, Reference Masand1995; Payne et al., Reference Payne2002). For residents with better cognitive function, the risk of becoming depressed increases with length of stay and an increased sense of hopelessness over health status and lack of autonomy (Jones et al., Reference Jones, Marcantonio and Rabinowitz2003; Hyer et al., Reference Hyer, Carpenter, Bishmann and Wu2005; Pot et al., Reference Pot, Deeg, Twisk, Beekman and Zarit2005; Tsai et al., Reference Tsai, Chung, Wong and Huang2005).
Detection of depression
Despite high prevalence, depression is still under-detected in residential care homes (Davidson et al., Reference Davidson, Koritsas, O'Connnor and Clarke2006). The Geriatric Depression Scale (GDS), the Cornell Scale for Depression in Dementia (CSDD), and, in the USA, the mood subscale of the Minimum Data Set (MDS) are the most frequently used tools for screening and detection.
Screening and detection instruments
The GDS has been widely used in residential care homes and several shorter versions have been developed, the most popular being the 15-item version. The original 30-item version (using a cut-off point of ≥11) has good psychometric properties. Gerety and colleagues (Reference Gerety1994) found moderate to substantial agreement with the DSM-III-R criterion standard for major depression and recommended its use in residential care homes, as both a case finding and severity instrument. Jongenelis and colleagues (Reference Jongenelis2005) found the GDS-30 to have sensitivity of 96.3% for major depression and 85.1% for minor depression compared with psychiatric interview and DSM-IV criteria. The 15-item version is generally preferred over the original as it is quicker to complete (6 minutes versus 12) and has good psychometric properties compared with the original version (McCurren, Reference McCurren2002) and with DSM criteria (Gerety et al., Reference Gerety1994). A five-item version of the GDS is also effective as a screening tool for depression in cognitively intact older adults, with 0.94 sensitivity and 0.81 specificity compared with an evaluation by a geriatrician (Rinaldi et al., Reference Rinaldi2003). As the GDS relies on self-report, there is debate as to whether it is suitable for use with people with mild to moderate dementia. A recent study comparing the GDS-15 with DSM-IV-TR criteria in people with and without dementia found adequate specificity and sensitivity, suggesting that it may be an appropriate instrument for use in these populations (Lach et al., Reference Lach, Chang and Edwards2010).
The CSDD has been extensively evaluated for use in residential care homes. The CSDD covers five areas: mood related signs, behavioral disturbances, physical signs, cyclic functioning and ideational disturbances. It takes approximately 30 minutes to complete: 20 minutes with a carer (or other informant) and 10 minutes with the older person. It is reliable, valid and sensitive, and can differentiate the entire range of severity, including mild to no depression (Alexopoulos et al., Reference Alexopoulos, Abrams, Young and Shamoian1988). Its limitations are that it takes 30 minutes to complete, requires trained personnel, does not correlate well with a psychiatrist's assessment, and is not always accurate in people with advanced dementia (de Bellis and Williams, Reference de Bellis and Williams2008). Despite these limitations, de Bellis and Williams concluded that it is the most comprehensive depression screening tool for older people with and without dementia, making it suitable for use in residential care homes. The main advantage of the tool is its use of multiple sources of information. Koritsas et al. (Reference Koritsas, Davidson, Clarke and O'Connor2006) suggest that routine use of the CSDD in residential care homes could improve doctor, nurse and personal carer communication, as personal care staff can be informants in the assessment of depression. Poor communication between professionals has been identified as a barrier to identification of depression in residential care homes (Brown et al., Reference Brown, Raue, Schulberg and Bruce2006).
Seven items from the mandated MDS from the Resident Assessment Instrument in the USA have been validated for use as a depression screening tool known as the MDS Depression Rating Scale (DRS) (Burrows et al., Reference Burrows, Morris, Simon, Hirdes and Phillips2000). In the original study the DRS compared favorably with the GDS-15 and the DRS has since been found to have adequate sensitivity and specificity and to be able to be reliably administered via self-report to residents with a MMSE score ≥12 (Ruckdeschel et al., Reference Ruckdeschel, Thompson, Datto, Streim and Katz2004). However, other studies have found poor correlation between the DRS and the GDS-15 (McCurren, Reference McCurren2002; Jones et al., Reference Jones2004; Meeks, Reference Meeks2004). This is probably due to the use of different information sources, as the GDS relies on self-report and the DRS is an observer-rated instrument. It may also be that the tools are measuring different elements of depression. One study found that the MDS identified greater depression among people with cognitive impairment and the GDS-15 identified more depression in people with better cognitive functioning (Jones et al., Reference Jones2004). Meeks (Reference Meeks2004) did not recommend the use of the MDS DRS as a screening tool for residential care homes because of its poor correlation and poor psychometric properties compared with the GDS.
A single screening question “Do you feel that your life is empty?” was trialed as a screening tool for depression in residential care homes in London and compared with the CSDD. A “yes” response indicated that the resident was twice as likely to have depression and a “no” response meant that there was a 75% chance that they did not have depression. Half of the study sample (n = 209) scored less than 15 on the Mini-Mental State Examination (MMSE) but there was no difference in sensitivity or specificity for the screening question for different levels of cognitive impairment. Watson et al. (Reference Watson, Zimmerman, Cohen and Dominik2009) trialed five strategies for depression screening in residential aged care. The best strategy was a two-item version of the Patient Health Questionnaire (PHQ-2) with a sensitivity of 0.80 and specificity of 0.75 as it was brief and easy to administer.
Under-detection
Nurses and personal care staff should be well placed to detect depression because of their close involvement with residents, but most are not very good at recognizing the symptoms of depression (Leo et al., Reference Leo, Sherry, DiMartino and Karuza2002; Ayalon et al., Reference Ayalon, Arean and Bornfeld2008). There is a poor relationship between resident and nurse CSDD ratings (Burrows, Reference Burrows1995). Brühl and colleagues (Reference Brühl, Hendrika and Martien2007) found the GDS detected 50% more depression than did nurses. Nurses recognized depression in only 55% of residents diagnosed via a psychiatric interview using DSM-IV criteria and they detected depression in 40% of residents not diagnosed as depressed. In the study by Watson and colleagues (2009) mentioned above, measures completed by care staff (modified version of the CSDD and a one-item screen) failed to detect depression adequately. A UK study conducted by Bagley and colleagues (Reference Bagley2000) found that only 15–27% of 308 newly admitted residents with depression were identified as depressed by staff (GDS compared with staff informant interviews). They concluded that more education was needed, as less than 2% of staff in their study had received in-service training on depression in older people. Ayalon et al. (Reference Ayalon, Arean and Bornfeld2008) found that paraprofessional staff working in residential care homes were more likely to view depression as a normal phenomenon, had less accurate beliefs about signs and symptoms and were less familiar with effectiveness of treatments for depression than nurses, social workers and activity staff. Education should be targeted to meet the needs of this group, as they provide the bulk of the care to residents.
Education
A number of studies have investigated the impact of education on detection and treatment of depression in residential care homes (McCabe et al., Reference McCabe, Russo, Mellor, Davison and George2008). In an American study investigating nursing home physicians’ beliefs about how well they can detect and treat depression, excellent training (versus good, fair, poor or none) and the use of screening tools were associated with better recognition and treatment skills, and practice guideline awareness was associated with greater self-reported treatment competency (Banazak et al., Reference Banazak, Mullan, Gardiner and Rajagopalan1999). A single education session for general practitioners (GPs) on late life depression was associated with improved GP recognition of depression in nursing home residents in an Australian study (Davidson et al., Reference Davidson, Koritsas, O'Connnor and Clarke2006). In another Australian study, staff education was one component of a successful multifactorial intervention for improving detection and treatment of depression in residential care homes (Llewellyn-Jones et al., Reference Llewellyn-Jones, Baikie, Smithers, Cohen, Snowdon and Tennant1999). Dutch nursing home staff randomized to a 4-hour training session on recognition of depression through observation of ADLs (using the Behavior Rating Scale for Psychogeriatric Inpatients) were better able to recognize depression than those in the control group. The ability to identify residents who were not depressed did not differ between groups. The use of video-based training also improves nursing staff's ability to detect mood symptoms in nursing home residents (Wood et al., Reference Wood, Cummings, Schnelle and Stephens2002). Having a mandated screening tool also improves recognition and initiation of treatment for depression in residential care homes (Boyle et al., Reference Boyle, Roychoudhury, Beniak, Cohn, Bayer and Katz2004).
Treatment and management of depression in residential homes
Assessment is an essential pre-requisite to treatment (Morris, Reference Morris2008) and may identify factors that could cause or contribute to depression, such as drug reaction, medical illness (Morris, Reference Morris2008), pain (Asghari et al., Reference Asghari, Ghaderi and Ashory2006), or environmental factors (Choi et al., Reference Choi, Ransom and Wyllie2008). Addressing such issues may alleviate depressive symptoms.
Treatment approaches
The main approaches in treatment of depression anywhere at any age can be divided into biological (e.g. antidepressants and electroconvulsive therapy (ECT)), psychological (e.g. cognitive behavior therapy) and social (e.g. recreational activities). Treatments may be used singly or in combination depending on circumstances. Table 2 displays a summary of representative treatment studies in residential care homes.
Table 2. Representative studies of treatment for depression in residential homes for the elderly
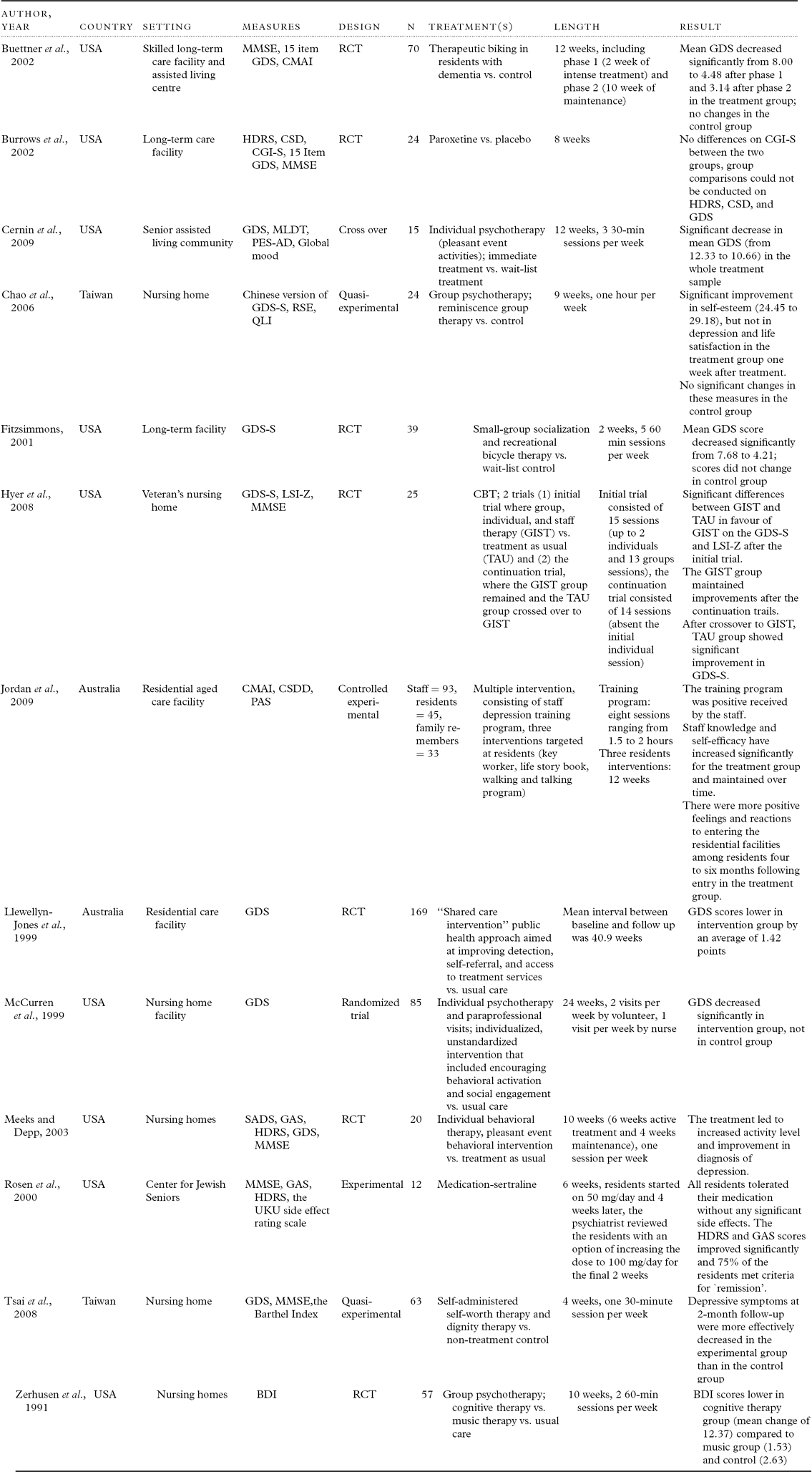
Note: BDI = Beck Depression Inventory, CGI-S = Clinical Global Impression of Severity, CMAI = Cohen-Mansfield Agitation Inventory, CSDD = Cornell Scale for Depression in Dementia, GAS = Global Assessment Scale, GDS = Geriatric Depressive Scale, GDS-S = Geriatric Depressive Scale-Short Edition, HDRS = Hamilton Depression Rating Scale, LSI-Z = Life Satisfaction Index Z, MLDT = Macneill-Lichtenberg Decision Tree, MMSE = Mini-Mental State Examination, PAS = Psycho-geriatric Assessment Scales, PES-AD = Pleasant Events Schedule For Alzheimer's Disease, QLI = Quality of Life Index, RSE = Rosenberg Self-Esteem Survey, SADS = Schedule for Affective Disorders and Schizophrenia
Antidepressants are the most common treatment for depressed residents (Brown et al., Reference Brown, Lapane and Luisi2002; Carlson and Snowden, Reference Carlson and Snowden2007). There is evidence that antidepressants are effective for treating depression, in particular, major depression in care home residents (Rovner and Katz, Reference Rovner and Katz1993; Snowden et al., Reference Snowden, Sato and Roy-Byrne2003). It is suggested that antidepressants should be included in the first-line treatment for residents with major depression (American Geriatrics Society and American Association for Geriatric Psychiatry, 2003). Several different classes of antidepressant are available (Baldwin, Reference Baldwin, Jacoby, Oppenheimer, Dening and Thomas2008) and the choice of medication should be based on the side effect profile, potential interactions with other medications and the resident's comorbid illnesses (Masand, Reference Masand1995; Rosen et al., Reference Rosen, Mulsant and Pollock2000; Kallenbach and Rigler, Reference Kallenbach and Rigler2006). Antidepressants should be started at a low dose and be increased slowly (Snowdon et al., Reference Snowdon, Burgess, Vaughan and Miller1996; Bell and Goss, Reference Bell and Goss2001; American Geriatrics Society and American Association for Geriatric Psychiatry, 2003; Kallenbach and Rigler, Reference Kallenbach and Rigler2006). ECT is usually administered in hospital and is reserved for severe depression, but because it works quickly ECT should be considered as the first-line treatment for residents at high risk of suicide (Kallenbach and Rigler, Reference Kallenbach and Rigler2006).
Numerous psychological approaches are appropriate to treat depression in residential care homes. These include behavior therapy (Meeks and Depp, Reference Meeks and Depp2003; Meeks et al., Reference Meeks, Looney, Haitsma and Teri2008; Reference Meeks, Shah and Ramsey2009), cognitive therapy (Zerhusen et al., Reference Zerhusen, Boyle and Wilson1991; Tsai et al., Reference Tsai, Wong, Tsai and Ku2008), cognitive behavior therapy (CBT) (Hyer et al., Reference Hyer, Yeager, Hilton and Sacks2008), and life review approaches (Chao et al., Reference Chao2006; Plastow, Reference Plastow2006). Social interventions include various types of recreational activities (Snowden et al., Reference Snowden, Sato and Roy-Byrne2003), e.g. therapeutic biking programs (Fitzsimmons, Reference Fitzsimmons2001; Buettner and Fitzsimmons, Reference Buettner and Fitzsimmons2002). Most of the studies cited above reported significant beneficial effects and some review papers have concluded that psychosocial approaches are effective in treating depression, in particular minor depression, in residential care homes (Snowden et al., Reference Snowden, Sato and Roy-Byrne2003; Hyer et al., Reference Hyer, Carpenter, Bishmann and Wu2005). Consistently, it is suggested that non-pharmacological methods should be considered as first-line treatment for residents with minor depression (American Geriatrics Society and American Association for Geriatric Psychiatry, 2003). It is important to note that many of these approaches were delivered in a group format (Bharucha et al., Reference Bharucha, Dew, Miller, Borson and Reynolds2006). Group therapy is a more practical and cost-effective strategy in the residential home environment (Carlson and Snowden, Reference Carlson and Snowden2007). Individual psychotherapy is not available in most residential care homes (Snowden et al., Reference Snowden, Sato and Roy-Byrne2003) due to a shortage of trained psychotherapists, cost, and, in many countries, a lack of any tradition of psychotherapists working in residential care homes.
There is also some evidence that other approaches, such as staff training (Glaister and Blair, Reference Glaister and Blair2008), changes in health service model (Snowden et al., Reference Snowden, Sato and Roy-Byrne2003) and residential home environment (Bell and Goss, Reference Bell and Goss2001) might also be effective in reducing residents’ depressive symptoms.
It seems likely that combining medical and psychosocial approaches would be the best way to manage depression in residential care homes (McCurren et al., Reference McCurren, Dowe, Rattle and Looney1999; American Geriatrics Society and American Association for Geriatric Psychiatry, 2003; Morris, Reference Morris2008). However, no recent studies have systematically investigated the possible benefits of such a combined approach.
Over the past 12 years there has been increasing interest in multifaceted approaches to the treatment of depressed residents (Llewellyn-Jones et al., Reference Llewellyn-Jones, Baikie, Smithers, Cohen, Snowdon and Tennant1999; Reference Llewellyn-Jones2001; Brooker and Woolley, Reference Brooker and Woolley2007; Brooker et al., Reference Brooker, Woolley and Lee2007; Hyer et al., Reference Hyer, Yeager, Hilton and Sacks2008; Jordan et al., Reference Jordan, Byrne and Bushell2009). For example, the multifaceted shared care intervention used by Llewellyn-Jones et al. (Reference Llewellyn-Jones, Baikie, Smithers, Cohen, Snowdon and Tennant1999) included: (a) multidisciplinary consultation and collaboration to remove barriers to care, (b) training of GPs and carers in detection and management of depression, (c) depression-related health education and activity programs for residents. Similarly the British Enriched Opportunities program (Brooker and Woolley, Reference Brooker and Woolley2007; Brooker et al., Reference Brooker, Woolley and Lee2007) included individualized assessment of residents, case work, an activity and occupation program, staff training, management and leadership. These studies reported significant improvement in residents’ depression and suggest that integrating multiple modalities should be the focus of future research.
As discussed above, it can be difficult to identify depressed residents. It is also challenging to treat them effectively. Some antidepressants, such as selective serotonin reuptake inhibitors (SSRIs), may have limited efficacy in residents with comorbid dementia (Burrows et al., Reference Burrows, Salzman, Satlin, Noble, Pollock and Gersh2002). In addition, some residents may not be able to participate effectively in psychotherapy because of their limited cognitive function (Kallenbach and Rigler, Reference Kallenbach and Rigler2006; Carlson and Snowden, Reference Carlson and Snowden2007).
There are important methodological limitations in many treatment studies. These include small sample sizes (Bharucha et al., Reference Bharucha, Dew, Miller, Borson and Reynolds2006), variable study inclusion criteria (Snowden et al., Reference Snowden, Sato and Roy-Byrne2003; Hyer et al., Reference Hyer, Carpenter, Bishmann and Wu2005), short treatment duration (Hyer et al., Reference Hyer, Carpenter, Bishmann and Wu2005), few randomized controlled trials (Carlson and Snowden, Reference Carlson and Snowden2007) and heterogeneous outcome measures (Bharucha et al., Reference Bharucha, Dew, Miller, Borson and Reynolds2006). However, these studies do provide strong evidence that depression is treatable in nursing home residents (Hyer et al., Reference Hyer, Carpenter, Bishmann and Wu2005).
Issues in treatment of depression
In spite of the evidence that depression is treatable in residential homes, many studies have found that depression is under-treated in this group (Masand, Reference Masand1995; Hyer et al., Reference Hyer, Carpenter, Bishmann and Wu2005). About 50%, or even up to 75% of residents with depression were receiving no treatment at all (Rovner et al., Reference Rovner, German, Brant, Clark, Burton and Folstein1991; George et al., Reference George, Davison, McCabe, Mellor and Moore2007).
Although there is evidence that the initiation of treatment for depression has improved in recent years (Boyle et al., Reference Boyle, Roychoudhury, Beniak, Cohn, Bayer and Katz2004), the treatment is often inadequate or inappropriate. First, there is a reliance on antidepressants and very few residents receive non-pharmacological treatment for depression (George et al., Reference George, Davison, McCabe, Mellor and Moore2007; Choi et al., Reference Choi, Wyllie and Ransom2009). Second, many residents receiving antidepressants are on sub-therapeutic doses (Draper et al., Reference Draper2001; Brown et al., Reference Brown, Lapane and Luisi2002). There is also evidence that antidepressants are rarely reviewed by physicians (O'Connor et al., Reference O'Connor, Griffith and McSweeney2010). Given these problems, it is not surprising that only a minority of residents on antidepressants show improvements in depressive symptoms (Draper et al., Reference Draper2001; Boyle et al., Reference Boyle, Roychoudhury, Beniak, Cohn, Bayer and Katz2004). The findings of inadequate treatment of depression in residential care homes have major implications for the management of depression in these environments. Many researchers have suggested that the management should go beyond first generation problems, such as identification and initial treatment, to include second generation problems, such as strategies for partial- and non-responders, and ongoing management through the maintenance phases (Draper et al., Reference Draper2001; Datto et al., Reference Datto, Oslin, Streim, Scheinthal, DiFilippo and Katz2002; Weintraub et al., Reference Weintraub, Datto, Streim and Katz2002; Boyle et al., Reference Boyle, Roychoudhury, Beniak, Cohn, Bayer and Katz2004; Carlson and Snowden, Reference Carlson and Snowden2007).
Outcome and prognosis of depression in residential care homes
As discussed in the etiology section, there is a bi-directional relationship between depression and risk factors for depression. Depression in residential homes is linked to poor physical health, decreased functional and cognitive abilities, pain, and poor nutrition (Parmelee et al., Reference Parmelee, Katz and Lawton1991; Reference Parmelee, Katz and Lawton1992a; Anstey et al., Reference Anstey, von Sanden, Sargent-Cox and Luszcz2007; Smoliner et al., Reference Smoliner, Norman, Wagner, Hartig, Lochs and Pirlich2009). Depressed residents also have lower levels of social engagement (Achterberg et al., Reference Achterberg, Pot, Kerkstra, Ooms, Muller and Ribbe2003; Tsai et al., Reference Tsai2009), more behavioral and vocal disturbance (Dwyer and Byrne, Reference Dwyer and Byrne2000; Brodaty et al., Reference Brodaty2001), poorer quality of life (Smoliner et al., Reference Smoliner, Norman, Wagner, Hartig, Lochs and Pirlich2009) and increased use of health care services (Smalbrugge et al., Reference Smalbrugge, Pot, Jongenelis, Gundy, Beekman and Eefsting2006b).
The most alarming outcome of depression is that it is a significant risk factor for mortality in care home residents. Rovner et al. (Reference Rovner, German, Brant, Clark, Burton and Folstein1991) examined the relationship between depression and mortality in 454 nursing homes residents. The likelihood of death at one year was increased by 59% for residents with major depression compared to those with only depressive symptoms or no depression. Ashby et al. (Reference Ashby, Ames, West, MacDonald, Graham and Mann1991) followed 973 care home residents for 8 to 16 months and found that depression was associated with increased mortality. In particular, depressed residents were three times more likely to die than those without depression or dementia. In the study by Parmelee et al. (Reference Parmelee, Katz and Lawton1992a) of 898 nursing home and congregate apartment residents, the mortality rates were 33% for residents with major depression, 28% for residents with minor depression and 16% for non-depressed residents after 18 months. This result indicates a systematic and significant increase in mortality with increasing severity of depression. In one small study, the mortality rate for depressed residents reached 59% after four years (Ames, Reference Ames1992).
These studies indicate that depression is associated with increased mortality in residential care homes for older people. However, there is controversy about the mechanism by which depression exerts its effect (Samuels and Katz, Reference Samuels and Katz1995). While some studies found that depression was an independent risk factor for mortality in residents (Rovner et al., Reference Rovner, German, Brant, Clark, Burton and Folstein1991; Shah et al., Reference Shah, Phongsathorn, George, Bielawska and Katona1993), others found no significant relationship between depression and mortality when demographic variables and correlates of depression, such as physical health, functional impairment, cognitive status, and history of depression, were taken into account (Parmelee et al., Reference Parmelee, Katz and Lawton1992a; Cuijpers, Reference Cuijpers2001). The different results might be due to methodological differences, such as the definition of depression, sampling strategies and the sample sizes, and more studies are needed for a clearer understanding of the relationship between depression and mortality among those who live in residential care homes.
There is evidence that much depression in residential care homes is chronic, with persistence rates ranging from 44% to 63%. Sutcliffe et al. (Reference Sutcliffe2007) followed 308 newly admitted UK residents for nine months. Of the residents who were depressed at baseline, 44% were still depressed after five and nine months. Similarly, Barca et al. (Reference Barca, Engedal, Laks and Selbaek2010) reported a persistence rate of 45% after 12 months. Smalbrugge et al. (Reference Smalbrugge, Jongenelis, Pot, Eefsting, Ribbe and Beekman2006a) followed 350 Dutch nursing home residents for six months and reported a persistence rate of 63%. This figure is similar to Ames et al. (Reference Ames, Ashby, Mann and Graham1988), who found that of residents surviving after four years, 63% of previously depressed residents were still depressed and only 17% had recovered. Weyerer et al. (Reference Weyerer, Häfner, Mann, Ames and Graham1995) followed 120 newly admitted residents (60 from residential care homes in the city of Mannheim Germany, and 60 from care homes in London, UK) for eight months. The prevalence of depression was high in both cities at admission (35% in Mannheim and 48% in London) and did not change significantly over eight months. In both places, depression at baseline was the best predictor for depression three months and eight months later; sex, age, social isolation, ADLs, and cognitive impairment at the time of admission were not significantly associated with depression either three or eight months later.
The persistence rate seems to be lower for depressed residents with dementia. Payne et al. (Reference Payne2002) followed 201 residents with cognitive impairment. They found that at six months, only 15% of the depressed residents were still depressed, and at 12 months only 7.5% were depressed. The study suggested that the decline in depression over the year after admission likely reflects appropriate diagnosis and treatment of depression in residential care homes.
Depression might also be a risk factor for suicide in residents (Reiss and Tishler, Reference Reiss and Tishler2008). A study in Finland found that 12 nursing home residents died by suicide in a 12-month period, accounting for 0.9% of all suicides in Finland in that year. Nine (75%) of them were diagnosed with a depressive syndrome, although only three (33%) were recognized by staff as having depressive symptoms before their death (Suominen et al., Reference Suominen, Henriksson, Isometsä, Conwell, Heilä and Lönnqvist2003).
It is important to point out that there are as yet relatively few outcome studies of depression in residential homes and most of those studies have short follow-up periods (Llewellyn-Jones and Snowdon, Reference Llewellyn-Jones and Snowdon2007). More longitudinal studies are needed for a better understanding of the outcomes of depression in residential care homes.
Conclusion and recommendations for action
Despite increased detection and treatment of depression in recent years (Boyle et al., Reference Boyle, Roychoudhury, Beniak, Cohn, Bayer and Katz2004), depression remains a significant problem for older people living in residential homes (Snowdon, Reference Snowdon2010). Prevalence remains high and the few longitudinal studies that have been conducted show high persistence of depression over time. Care staff still lack knowledge and understanding of depression with many seeing depression as a normal phenomenon for older people (Ayalon et al., Reference Ayalon, Arean and Bornfeld2008). Depression is therefore often not detected or treated. This lack of detection and treatment may have serious consequences, as depression does not often remit spontaneously in these home residents (Smalbrugge et al., Reference Smalbrugge, Jongenelis, Pot, Eefsting, Ribbe and Beekman2006a; Barca et al., Reference Barca, Engedal, Laks and Selbaek2010) and is a significant risk factor for mortality (Ashby et al., Reference Ashby, Ames, West, MacDonald, Graham and Mann1991; Rovner et al., Reference Rovner, German, Brant, Clark, Burton and Folstein1991; Shah et al., Reference Shah, Phongsathorn, George, Bielawska and Katona1993), and suicide (Suominen et al., Reference Suominen, Henriksson, Isometsä, Conwell, Heilä and Lönnqvist2003). Detection is the essential first step in initiating assessment and treatment for depression.
Further research is needed to investigate those treatment approaches that appear promising, particularly multifaceted (Llewellyn-Jones et al., Reference Llewellyn-Jones, Baikie, Smithers, Cohen, Snowdon and Tennant1999) and psychosocial approaches (Snowden et al., Reference Snowden, Sato and Roy-Byrne2003; Hyer et al., Reference Hyer, Carpenter, Bishmann and Wu2005). There is also a need for more longitudinal studies to inform us about incidence, persistence and outcomes of depression.
In clinical practice, there is a need for education of care staff (particularly personal carers) to ensure they understand that depression is a serious and treatable condition and that they recognize depressive symptoms and signs. Screening for depression should be mandatory in all residential care homes and linked to a process for referral and initiation of assessment and treatment. Finally, residential care homes could address environmental factors associated with depression, such as lack of privacy, and institute interventions known to benefit people with depression, such as recreational activities, for all residents as preventive measures for depression.
The devotion of an entire issue of International Psychogeriatrics (volume 22, issue 7) to the topic of mental health issues in long-term care homes, and the existence of the International Psychogeriatric Association's Task Force on Mental Health Services in Long-term Care Homes (Conn and Snowdon, Reference Conn and Snowdon2010) indicate both the importance of depression in this setting as well as a determination to do something about it. However, a quarter of a century after one of us commenced a doctoral project which focused on the treatment of depression in residential care (Ames, Reference Ames1990), the situation for many depressed residents around the world is still far from satisfactory and much work remains to be done, not least in ensuring the translation of existing knowledge into routine practice.
Conflict of interest
None.
Description of authors' roles
All five authors collaborated closely in reviewing the literature, and writing and revising this guest editorial.




