Introduction
Information is needed in the mental health system by all stakeholders. Clinicians are interested in evaluating treatment outcomes; managers are interested in analysing the effectiveness of the services they lead; while decision-makers want to learn the outcomes of their policies. Other stakeholders such as users, families and advocacy NGOs (non-governmental organisations) that are keen to monitor the quality of care and respect for human rights also have an interest in information. Finally, information is needed to verify system infrastructure and the responsible and transparent utilisation of scarce resources. There is a consensus that rational planning aimed at achieving a well-functioning system is hardly possible in the absence of sound monitoring and evaluation, based on good quality information (Thornicroft & Tansella Reference Thornicroft and Tansella1999; Lora et al. Reference Lora, Lesage, Pathare and Levav2016).
Reliable and timely health information is the foundation for effective health services management and public health action (WHO, 2011). Persuaded that what ‘gets measured gets done,’ World Health Organization (WHO) included ‘monitoring community mental health,’ through strengthening information systems, as one of the ten recommendations that can make a difference in mental health care (WHO, 2001a). Consequently WHO developed long-term strategies and tools designed for mental health information gathering in all Member States, not only in high income countries but also in low and middle income countries where information are more difficult to collect.
WHO first produced an Atlas of Mental Health Resources around the world in 2001, with updates produced in 2005 and 2011 (http://www.who.int/mental_health/evidence/atlasmnh) (WHO, 2001b, 2005a & 2011). The Atlas project has become a valuable resource on global information on mental health and an important tool for developing and planning mental health services within countries.
The new edition of Mental Health Atlas (WHO, 2015), carried out in 2014, assumes new importance as a repository of mental health information in WHO Member States because it is providing much of the baseline data against which progress towards the objectives and targets of the Comprehensive Mental Health Action Plan 2013–2020 (WHO, 2013) is to be measured. For example, Atlas data can be used to estimate the proportion of countries globally that have developed or updated their policies, plans and laws for mental health in line with international and regional human rights instruments, or are routinely collecting and reporting on a core set of mental health indicators. In collecting this information, the Mental Health Atlas 2014 questionnaire covers critical areas of mental health system development, including governance and financing, human resources, service availability and delivery, promotion and prevention, and surveillance.
The goal of this paper is to describe the availability and delivery of mental health services in the WHO's Member States, focussing on the differences related to the countries’ income level.
Methods
The Mental Health Atlas project 2014 required a number of administrative and methodological steps, starting from the development of a questionnaire and ending with statistical analyses and presentation of data.
The selection of indicators to be included in the questionnaire was based on consultations with Member States, and developed in collaboration with WHO regional offices as well as experts in the area of mental health care measurement. The questionnaire was modified based on this feedback. The final version sent to countries for completion can be found at the Mental Health Atlas website (http://www.who.int/mental_health/evidence/atlasmnh). Alongside the questionnaire itself, a completion guide was developed to help standardise terms and to ensure that the conceptualisation and definition of services or resources were clearly and consistently understood by all respondents. A glossary of terms was also developed and shared with respondents. The data contained in this paper are mainly derived from questions relating to mental health service availability and uptake, as well as on financial and human resources for mental health. Other sections of the survey covered mental health system governance (policy, legislation and stakeholder involvement) and mental health promotion and prevention.
WHO headquarters staff, together with WHO regional and country office counterparts, requested ministries of health or other responsible ministries to appoint a focal point to complete the Atlas questionnaire. The focal point was encouraged to contact other experts in the field to obtain information relevant to answering the survey questions. Close contact with the focal points was maintained during the course of their nomination and through questionnaire submission. Staff members at WHO headquarters and regional offices were available to respond to enquiries, to provide additional guidance, and to assist focal points in filling out the Atlas questionnaire.
Once a completed questionnaire was received, it was screened for incomplete and inconsistent answers. To ensure good-quality data, respondents were contacted again and were asked to respond to the requests for clarification and to correct their responses. The data presented in this paper refer to the year 2014 and were collected and analysed in 2015.
Upon receipt of the final questionnaires, data were aggregated, analysed and are reported both by WHO region and by World Bank income group. As of 1 July 2014, low-income economies are defined as those with a gross national income (GNI) per capita of US$1045 or less in 2013; middle-income economies are those with a GNI per capita of more than US$1045 but less than US$12 746; high-income economies are those with a GNI per capita of US$12 746 or more. Lower-middle-income and upper-middle-income economies are separated at a GNI per capita of US$4125. Rates per 100 000 population were calculated for certain data points, using official UN population estimates for 2013.
For each indicator, results are presented as median values. Interquartile ranges (IQRs) are also provided as measures of statistical dispersion, being equal to the difference between the upper and lower quartiles.
Results
In total, 171 out of WHO's 194 Member States were able to at least partially complete the questionnaire, a response rate approaching 90%. See Appendix for definition of mental health facilities.
Outpatient and day care
Mental health outpatient facilities
In terms of accessibility, there are very substantial differences between the population served per outpatient facility (Table 1): while in low-income countries (LIC) there are more than 2 million people, in lower-middle income countries (LMIC), upper-middle income countries (UMIC) and high-income countries (HIC) each outpatient facility serves from 250 000 to 50 000 people.
Table 1. Mental health outpatient facilities
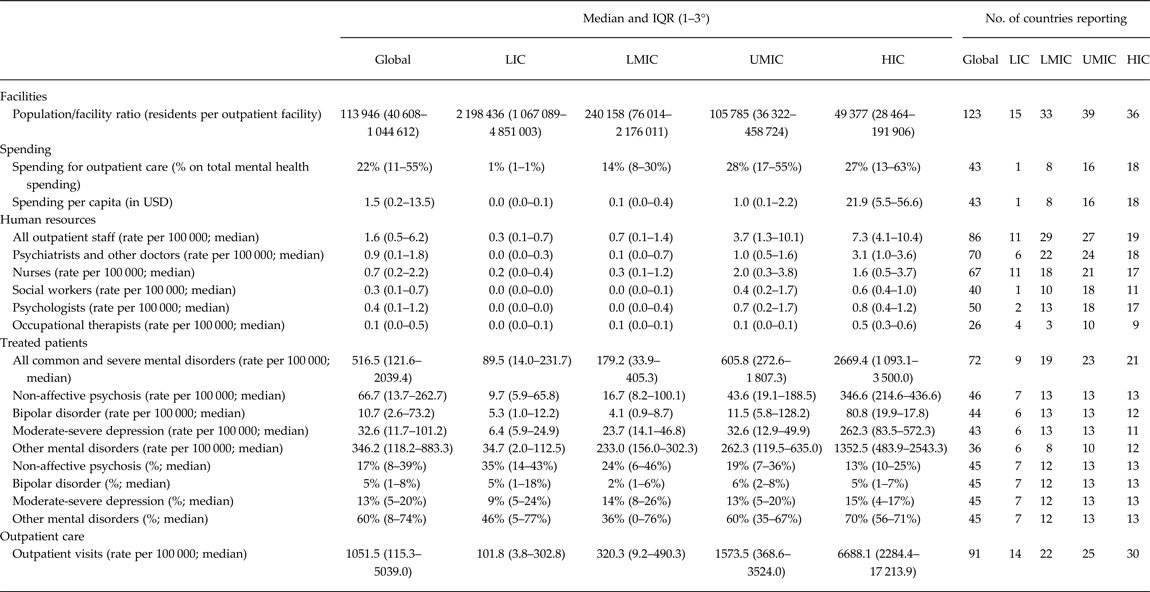
Spending is directed only partially to outpatient mental health care: the spending per capita for outpatient facilities increases dramatically from LMIC to HIC, while the percentage of funding for outpatient facilities doubles from LMIC to HIC, arriving at a quarter of total reported expenditure.
At a global level, there are 1.6 mental health professionals working in outpatient facilities per 100 000 population, again with marked differences between countries of different income, not only for the total number of professionals working in these facilities (the ratio between LIC and HIC is 15-fold), but also for specific professionals, e.g. doctors and nurses. Psychosocial care staff (psychologists, social workers and occupational therapists) – a key resource input providing community-based care – are particularly scarce.
The global median rate of service users treated per year in outpatient clinics is 517 per 100 000 population, with substantial variability by country income level. Accessibility, in terms of the rate of treated outpatients, is ten times greater in HIC as compared with LMIC, and 20-fold times higher than in LIC. Similarly, the utilisation of outpatient facilities, in terms of outpatient contacts, is dramatically different for countries of different income levels: the number of visits per 100 000 population in HIC is over 50 times greater than in LIC and 20 times greater than LMIC.
As far as the diagnostic breakdown of patients reported to be receiving care and treatment in outpatient facilities, all the diagnoses show an increase from LIC to HIC (higher utilisation rates), but this increase is particularly noticeable for moderate and severe depression and other mental disorders (that includes common mental disorders). At global level treated cases of non-affective psychosis represent one-sixth of the total, bipolar disorders one-twentieth, moderate and severe depression one-tenth, while most of the patients are cared in outpatient facilities present common mental disorders and other disorders. However, these figures for some diagnoses change dramatically by income level (e.g. non-affective psychoses decrease from 35% in LIC to 13% in HIC). It is also noticeable that only 46 countries were able to report the diagnostic breakdown in outpatient facilities.
Mental health day treatment facilities
Based on reported estimates from Atlas 2014 survey, mental health day care facilities are scarce in the context of lower and middle income countries. In HIC, the median value for 17 responding countries is 5.3 places per 100 000 population.
When analysed by income level, patients cared in day treatment facilities varies considerably: the median treatment rate is zero persons per 100 000 people in LIC, less than one person in middle income countries and 54 persons in HIC.
In HIC about one-fifth of the patients treated in day centres are affected by non-affective psychosis, one-twentieth by bipolar disorder, one-tenth by depression and about two-thirds by other mental disorders.
Inpatient care
Mental hospitals
Globally, there are 6.5 mental hospital beds per 100 000 population (Table 2). Despite the transition in a number of HIC towards psychiatric wards in general hospitals and the provision of community-based residential care places, HIC still have a far higher number of mental hospital beds than lower-income countries. Mental hospital beds represent 80% of total inpatient beds at the global level, with only small differences by level of country income. Globally, there is a slight decrease of 5% in the number of mental hospitals between 2011 and 2014. A more significant decrease is observed for the number of mental hospital beds, which drops by nearly 30% compared with 2011. When countries are grouped according to income level, all except LMIC, show a reduction in both the number of hospitals and the number of mental hospital beds (Tables 3–5).
Table 2. Mental health day treatment facilities

Table 3. Mental hospital

Table 4. Psychiatric wards in general hospital
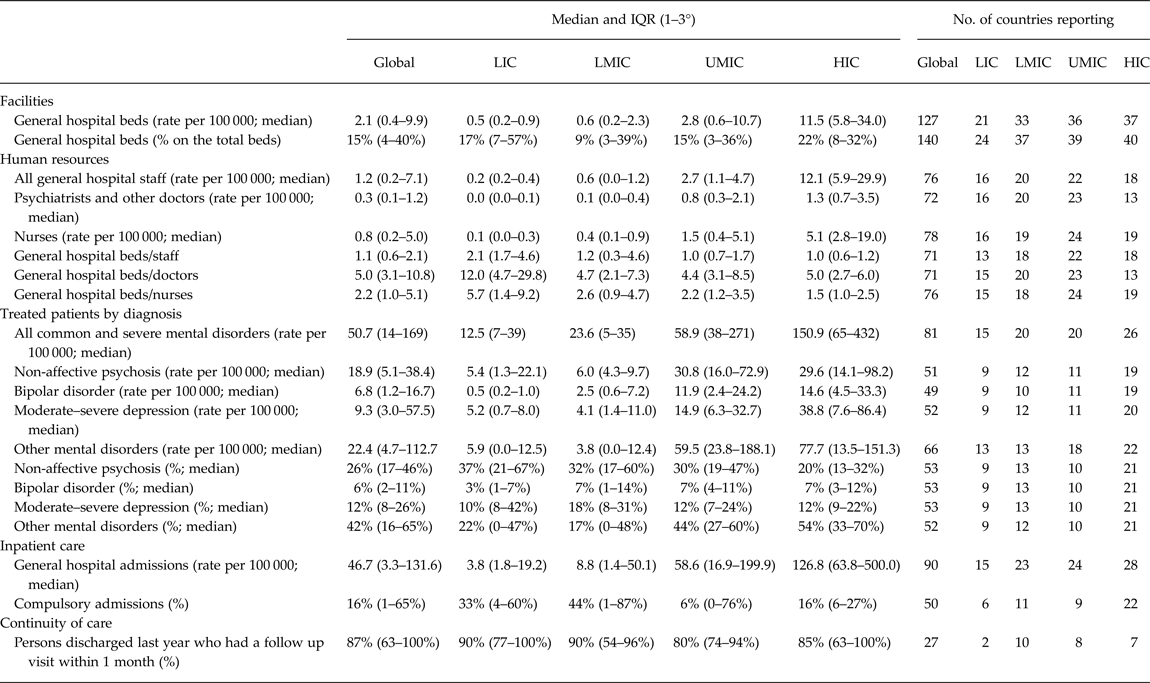
Table 5. Community-based residential care facilities

As far as funding goes, resources devoted to mental hospitals account for more than half of all reported mental health spending and, as expected, is strongly influenced by income: the spending per capita in lower and middle income countries is one-twentieth of that in HIC.
At a global level, an estimated seven professionals out of ten working in mental health are based in mental hospitals. The number of beds cared by a single doctor is three times higher in LIC compared with HIC; the same ratio holds for nurses and for staff in general.
The median rate of admissions at global level is 35.8 per 100 000 population, showing a 20-fold increase from LIC to HIC. Despite the global decrease in number of beds, between 2011 and 2014 there is an increase of over 20% in the global median of admission rate to mental hospitals, indicative of a higher turnover rate. In HIC there is a 19% decrease in admission rates to mental hospitals while there is a slight increase (of 2%) in LIC. In mental hospitals there is a decrease in the percentage of involuntary admissions from LIC to HIC, from a half to a sixth, but it is important to highlight that number of countries reporting on this is relatively low. As far as the diagnostic breakdown, the rate per 100 000 population of patients admitted to mental hospitals increases for all diagnoses from LIC to HIC (more so for bipolar disorders and other diagnoses, less so for non-affective disorders). Patients with non-affective psychosis represent about a quarter to a third of all the patients admitted to mental hospitals, those with bipolar disorder and moderate–severe depression about one-tenth, while more than half of the patients suffer from other mental disorders.
The function of mental hospitals in LIC and LMIC appears to be radically different in HIC and UMIC: in LIC and LMIC the percentage of patients staying for more than 1 year is very low, indicating that the facility works more in the mode of a an acute psychiatric ward; in UMIC and HIC, the percentage of patients staying more than 1 year is higher (about a quarter of inpatients) which signifies that the facility works more as a long term care ward.
In terms of continuity of care, at the global level about seven patients out of ten discharged from mental hospitals are followed up at outpatient level within one month: while in LIC less than half of the patients are followed, in HIC more than three quarters.
Psychiatric wards in general hospital
There are 2.1 beds per 100 000 population at the global level, with marked differences between LIC/LMIC on one hand and UMIC/HIC on the other hand. The beds in general hospitals represent 15% of the total beds available at a global level. Between 2011 and 2014 the number of beds available in psychiatric wards in general hospital shows a marked increase of 60%.
At a global level there are 1.2 mental health professionals per 100 000 population working in General Hospital Psychiatric Wards (GHPWs), again with marked differences between countries at different income levels, not only for the total staff, but also for doctors and nurses. In general hospital wards the intensity of care is higher than in mental hospital: a single doctor has responsibility over 5 beds, a nurse 2 beds and all the staff 1 bed. The number of beds overseen by a single doctor, nurse or member of the staff is two times higher in LIC compared with HIC.
The median rate of admissions at global level is 43.8 per 100 000 population, showing a 30-fold gradient from LIC to HIC. Admission rates to general hospital facilities also increase substantially between 2011 and 2014 (by 84%). When aggregated by income group, it is apparent that these increases are largely occurring in middle-income countries; admission rates in LIC and HIC groups have actually decreased. Globally speaking, involuntary admissions in general hospitals amount to 16%, with differences between income level: they are higher in LIC/LMIC and lower in HIC.
In terms of diagnostic breakdown 1 patient out of 3–4 of those admitted to GHPWs are affected by non-affective psychosis, one out of 20 by bipolar disorders, one out of ten by moderate–severe depression, while less than half of the admissions are for other mental disorders. The rates per 100 000 population of patients admitted in GHPW for all the diagnoses increases from LIC to HIC, particularly for other diagnoses and bipolar disorders, less for non-affective disorders and depression.
In terms of continuity of care 87% of persons discharged from a general hospital units are followed up within 1 month by outpatient facilities, without marked differences between income-level groups. However, the validity of these results is questionable, because only 23 countries report this piece of information.
Community-based residential care facilities
Similar to the findings for day care, as a mode of inpatient mental health care community residential facilities are scarce in the context of low- and middle-income countries. In HIC, the median value is 10.9 beds per 100 000 population, representing a tenth of the total number of psychiatric beds.
Admissions in community residential facilities are relevant only in HIC: the median rate is 9.2 admissions per 100 000 population. Almost all of these admissions in HIC are voluntary; involuntary admissions are rare and localised in few facilities in LIC and LMIC. About a half of the patients are affected by non-affective psychosis, while the rest of the patients suffer from other mental disorders.
Discussion
The WHO Mental Health Atlas 2014 survey provides basic mental health information at the level of WHO Member States, which can inform national planning and service development, as well as reveal differences across countries when grouped by geographical region or income level.
Global comparative analysis of the type presented here reveals the extent to which mental health resources and activities in low- and middle-income countries are still scarce, inequitably distributed and inefficiently used after 10 years from the Lancet series on global mental health (Saxena et al. Reference Saxena, Thornicroft, Knapp and Whiteford2007) that highlighted these gaps.
Levels of public expenditures on mental health are very meagre in low and middle-income countries (less than US$2 per capita) (Atlas 2014). A large proportion of these funds go to inpatient care, especially mental hospitals. Globally, the median number of mental health workers is 9 per 100 000 population, but there is extreme variation (from below 1 per 100 000 population in LIC to over 50 in HIC). There is a wide gap between LIC and HIC in a number of areas: for example, mental health spending per capita is 25 times higher in HIC than in LIC, HIC have 20 times more beds in community-based inpatient units, the population served by outpatient facilities is 40 times higher, and there are 66 times more community outpatient contacts and 15 times more mental health staff at outpatient level. Without a minimum level of resources (i.e. mental health facilities and staff), it is difficult to provide community care.
Overall, in low- and middle-income countries, resources for mental health are not distributed efficiently: about 60% of financial resources and over two-thirds of all available mental health staff are concentrated in mental hospitals, which serve a small part of all the patients. Decentralisation of resources towards community-based services and care is needed to increase the coverage rate for mental disorders in low- and middle-income countries. The basic building blocks of mental health systems (e.g. policies, mental health services, human resources, information systems) (WHO, 2010) exist in most countries, though in many LIC they are rudimentary. Nevertheless, most countries, regardless of income group, have at least one of each type of facility. It is encouraging that community care is expanding in low- and middle-income countries in terms of facilities, staff and treated patients. However, progress is slow and there is still a long way to go: community-based mental health services are underdeveloped and inpatient care is still the predominant form of care. Outpatient care is the only effective means of increasing the coverage of the mental health system: there is a clear progression between LIC, LMIC and UMIC in terms of accessibility of mental health services, measured in terms of the increasing rates of outpatients. From a diagnostic point of view, this increase fosters the coverage not only of psychoses but also of severe and moderate depression cases and common mental disorders. It is important to note that inpatient mental health facilities, whether placed in general hospitals or in mental hospitals, only contribute slightly to overall service accessibility. Only community care has the potential to reduce the gap between needs in the population and supply of services.
Two elements of the network of mental health facilities are particularly scarce in low- and middle-income countries: day treatment facilities and community residential facilities. Further analyses are needed to determine whether this gap is related only to a lack of resources or to different needs of the mental health system specific to these contexts.
Between 2011 and 2014 there is a decrease in mental hospital beds and an important increase of general hospital beds and admission rates, even if there is still a scarcity of such beds in LIC and LMIC. Therefore, encouraging the development of general hospital beds in more districts should become a top priority. These beds are needed not only to supply inpatient treatments for acute cases in the population, but also in order to help the process of deinstitutionalisation. Particularly in LIC, but also in LMIC, mental hospitals often appear to function as acute wards, with a short length of stay, and it is not possible to decentralise their resources without increasing general hospital units in districts. Moreover, data on low ratio beds/staff in GHPWs and continuity of care after discharge, in comparison with mental Hospitals, may indicate a better quality of inpatient care in these facilities.
Involuntary admissions in mental hospitals and psychiatric wards in general hospital represent one-sixth of all the admissions, but the number of reporting countries is low. These results on data collection suggest that scant attention is being paid to monitoring human rights and there is a need for urgent action in this area. The poor attention to human rights is an example of how some deficiencies in mental health systems are not entirely due to a shortage of resources; frequently they may be due to organisational or legal issues that hampers the quality of care.
The reform of mental health systems is not merely a matter of resources, but also implicates cultural and scientific perceptions and practices among mental health professionals, health managers and policy-makers. Evidence indicates that, on the one hand, the majority of resources for mental health are spent in mental hospitals; on the other hand, reduction in the treatment gap necessitates an expansion of community-based care. Statistics such as these should not only stimulate scientific debate on mental health systems, but compel greater prioritisation of the global mental health agenda.
A number of limitations should be kept in mind when examining the results. While best attempts have been made to obtain information from countries on all variables, some countries could not provide data for a number of indicators. The most common reason for the missing data is that such data simply do not exist within the countries or are not collected, at least in the manner requested in the Atlas questionnaire. For instance, data on financial and human resources were particularly difficult to collect for some countries. Another reason is that Mental Health Atlas is collecting data from and through Ministry of Health, however some of the mental health data might be available at other Ministries e.g. Ministry of Social Affairs: collecting this data might require longer time and in some countries lengthy procedures. The extent of missing data can be determined in the tables from the number of countries that have or have not been able to supply details. Each individual table contains the number of countries able to respond to an item of the questionnaire. Another problem is the level of validity of the diagnoses included in administrative databases: the high percentage of ‘other diagnoses’ in mental health facilities may be related partly to misclassification. A further limitation is that most of the information provided relates to the country as a whole, thereby overlooking potentially important variability within countries concerning, for example, the availability of services.
The role of information is usually underestimated in mental health systems. High-quality information is needed to monitor and improve the quality of mental health services (WHO, 2005b). In addition, information supports accountability for services delivered and allotted funding which are key components in the public mental health system.
Unfortunately mental health services trail behind the general health system in collecting and analysing standard information, not only in low and middle income countries but also in high-income countries. (Institute of Medicine, 2006; Pincus et al. Reference Pincus, Spaeth-Rublee and Watkins2011; OECD, 2014). There are several reasons for this discrepancy (Ryan et al. Reference Ryan, De Silva, Terver, Ochi and Eaton2015); for instance, insufficiencies in staff training, poor information infrastructure and lack of common performance standards. Other two reasons should be added: the lack of a tradition of accountability in mental health services and inadequate training for clinical managers that have rarely been exposed to epidemiological and mental health services research.
Improving completeness of data collection and coverage is imperative for outpatient facilities that are particularly vulnerable in terms of gaps in data collection. Moreover, much has been done to improve the quality of information collected at facility level. In most countries however, facility-based recording and reporting systems have continued to lag behind due to data quality problems. The introduction of Information and Communications Technology (ICT) is useful, but it is not sufficient enough to solve these problems on its own; rather, to improve quality of data collection, a mandatory policy with regulations, clear rules for data collection, adequate equipment and ICT is necessary (WHO, 2003).
To bridge the gaps in the use of information, certainly more attention needs to be paid to completeness and quality of the data collection, where data are lacking, but also it is necessary to shift attention of relevant stakeholders from data collection to the analysis, use and dissemination of information. Information systems for example still tend to be ‘data driven’ and focused on data collection, instead of being ‘action driven’ to change the mental health system (WHO, 2000). Resources are needed to improve the information infrastructure, but the first challenge on the way forward is to tackle the cultural obstacles. The role of information should be made better known in order to shift the attitudes of mental health staff from resistance to a seemingly hitherto alien one of genuine interest in the data analysed (Lora et al. Reference Lora, Lesage, Pathare and Levav2016).
As articulated through its Comprehensive Mental Health Action Plan 2013–2020 (WHO, 2013), WHO places considerable emphasis on the use of information as a means towards reducing the mental health treatment gap, for developing community care, and for strengthening mental health systems.
Disclaimer
F.H. and D.C. are staff members of the World Health Organization. The authors alone are responsible for the views expressed in this publication and they do not necessarily represent the decisions, policy or views of the World Health Organization.
Financial Support
This research received no specific grant from any funding agency, commercial or not-for-profit sectors.
Conflict of Interest
None.
Ethical Standard
The authors assert that all procedures contributing to this work comply with the ethical standards of the relevant national and institutional committees on human experimentation and with the Helsinki Declaration of 1975, as revised in 2008.
Appendix
Definitions of mental health facilities
1. Mental health outpatient facility is a facility that focuses on the management of mental disorders and the clinical and social problems related to it on an outpatient basis. Outpatient care is composed of hospital outpatient departments, mental health outpatient clinics, community mental health centres, and community-based mental health care facilities.
2. Mental health day treatment facility is a facility that typically provides care for users during the day. The facilities are generally available to groups of users at the same time (rather than delivering services to individuals one at a time), expect users to stay at the facilities beyond the periods during which they have face-to-face contact with staff, and involve attendances that last half or one full day.
3. Mental hospitals are specialised hospital-based facilities that provide inpatient care and long-stay residential services for people with mental disorders. Usually these facilities are independent and stand alone, although they may have some links with the rest of the health-care system. In many countries, they remain the main provider of the mental health system.
4. A psychiatric ward in general hospital is a psychiatric unit that provides inpatient care for the management of mental disorders, usually located within general hospitals; this unit provides care to patients with acute problems, and the period of stay is usually short (weeks to months).
5. A community-based residential care facility is a non-hospital, community-based mental health facility that provides overnight residence for people with mental disorders. Usually these facilities serve users with relatively stable mental disorders not requiring intensive mental health interventions.







