INTRODUCTION
Disparities in morbidity and mortality by socioeconomic status (SES) and race/ethnicity in the United States are well established [Reference Adler1, Reference Rogers2]. The U.S. Department of Health and Human Services declared as one of the two major goals of its Healthy People 2010 health promotion agenda ‘to eliminate health disparities among different segments of the population’ [3]. Despite this public concern, the physical mechanisms underlying health disparities remain poorly understood. Likely candidates such as health behaviours and access to health care have not easily accounted for the gradient [Reference Adler1, Reference Lantz4]. Increasing evidence points to links between lifelong exposure to infectious disease and subsequent chronic disease, suggesting a potential mechanism for linking SES to health outcomes [Reference Nieto5–Reference Schmaltz7]. Low social status has been linked to increased risk of respiratory infections in humans and other primates in experimental studies [Reference Cohen8–Reference Cohen10]. Much less is known about the links between social status and susceptibility to infections in the broader US population.
Exposure to herpesviruses such as cytomegalovirus (CMV) is nearly ubiquitous in early life, and is even found in isolated aboriginal groups [Reference Soderberg-Naucler11, Reference Staras12]. Primary infection during pregnancy is a leading cause of hearing loss, vision loss, and mental retardation among congenitally infected children [Reference Colugnati13]. Although infection with CMV often passes undiagnosed because of its asymptomatic properties, the virus remains persistent in the host's cells for life. Adequate cell-mediated immunity is important for maintaining the virus in this chronic state [Reference de Jong14, Reference Sinclair and Sissons15]. Importantly, CMV has been linked to inflammatory processes, cardiovascular disease, cognitive outcomes, and Alzheimer's disease [Reference Soderberg-Naucler11, Reference Liu16–Reference Aiello20]. For these reasons, it is important to examine the prevalence of CMV at various life stages within diverse socioeconomic and racial groups.
Racial/ethnic differences in infection status for CMV have been described in the United States adjusting for SES [Reference Staras12, Reference Colugnati13]. Age-adjusted seroprevalence rates for CMV were found to be 81·7% for Mexican Americans, 75·8% for non-Hispanic blacks, and 51·2% for non-Hispanic whites [Reference Staras12]. An age-adjusted association between three categories of family income and CMV seroprevalence was found in the United States, with this relationship diminishing in a multivariate model adjusting for age, race/ethnicity, education, marital status, area of residence, census region, family size, country of birth, and type of medical insurance [Reference Staras12]. These studies did not explicitly examine the relationship between education, income and prevalence of the infection in different age groups or test pathways that might explain SES differences in infection status. This paper will examine differences in CMV seropositivity by education, income, and race/ethnicity at different ages, then test whether variables proxying for potential exposure can explain the relationship between SES, race/ethnicity, and infection status.
Although previous research has demonstrated overall socioeconomic and racial/ethnic disparities in seropositivity, it is unclear at what age social gradients in infection emerge and what factors might explain these gradients. There are no studies of which we are aware that have examined education and income gradients in CMV infection status across age in a nationally representative sample from the US population and tested the role of potential exposure pathways that might explain these differentials. These are important questions, since the later life consequences of CMV infection for cell-mediated immunity may depend on the lifetime burden of this infection, and understanding how socioeconomic and racial/ethnic groups are differentially exposed and/or susceptible to this infection can help us design effective interventions. This paper will examine the relationship between SES, as measured by household income and years of education, and race/ethnicity, and the presence of serum IgG antibodies to CMV in persons aged ⩾6 years in the United States. Looking separately at children and adults, we will test how well these disparities can be accounted for by mediating variables that have been posited as potential exposure risk factors such as the number of individuals in the household, nativity outside the United States, region of residence, daycare attendance for youth, and sexual behaviours for adults.
METHODS
Study population
The National Health and Nutrition Examination Survey (NHANES) III was conducted by the National Center for Health Statistics from 1988 to 1994 and was a complex, stratified, multistage probability cluster sample of the US population including interview, clinical examination, and laboratory tests. Persons aged <5 years or >60 years, non-Hispanic black persons, and Mexican Americans were sampled at a higher frequency than other groups to obtain adequate sample sizes to more accurately evaluate these subgroups. The complete methodology and response rates of NHANES III have been published previously [21]. Surplus sera data containing positive or negative measures for CMV IgG antibody were released in 2005 for respondents aged ⩾6 years, thus these data represent the most recent data available on CMV prevalence in the US population. Our analysis focuses on two age groups. For ages 6–16 years, 4565/6936 of interviewed respondents also had information on CMV serostatus and were included in our analysis. Those missing CMV data were more likely to be non-Hispanic white, with slightly higher family income and education of the household reference person. Another 416 observations in this age group are omitted due to missing information on one or more covariates. For ages 25–49 years, of the 8230 interview respondents, 7255 had information on CMV serostatus. Those missing CMV data were not significantly different with respect to age, sex, race, income, or education. Another 1219 observations were omitted in this age category due to missing values on one or more covariates. Compared to the non-missing observations, those omitted were more likely to be non-Hispanic black, female, and have less education. All analyses were conducted using Stata 10.0 (Stata Corp., College Station, TX, USA) survey commands to account for the complex survey design, and the sample completing the laboratory components was weighted to reflect the non-institutionalized population of the United States.
Laboratory analyses
Serum samples were tested for CMV specific IgG with a Triturus robot (Grifols, Miami, FL, USA) with SeraQuest enzyme-linked immunoabsorbent assay (ELISA) reagents by Quest International Inc. (Miami, FL, USA). Reference ranges of positive and negative controls, and standards were established by the MLE (Master Lot Entry) card for each lot. ELISA optical density index values >1·0 were considered positive.
Sera with values near the ELISA cut-off, between 0·90 and 1·05 (~7% of total), were confirmed with a second ELISA assay by bioMérieux Inc. (Durham, NC, USA). When the results from these two tests disagreed (~2% of total), an IFA from Bion Enterprises Ltd (Des Plaines, IL, USA) was used and the result of the IFA was given as the final result. This procedure resulted in 98% sensitivity and 99% specificity [Reference Staras12, 22].
Statistical analyses
Logistic regression models were used to test the relationship between CMV positivity status (0=negative, 1=positive), race/ethnicity (non-Hispanic white, Non-Hispanic black, Mexican American, and Other), years of education, and family income. For those aged <17 years, education is measured as the highest grade completed by the household reference person. For those aged ⩾25 years, education is measured as the respondent's years of completed education. Family income is coded as the midpoint of each of the 26 reported categories (using $65 000 for incomes >$50 000), adjusted for inflation between the two NHANES III phases using the consumer price index. Income was then log-transformed due to the skewness of the distribution. Variables potentially mediating exposure included in all models were age at the time of examination, housing crowdedness (persons in dwelling/number of rooms), an indicator for urban or rural residence, census region of residence, and gender. Results using alternative specifications of family and household size, including total number of persons, total number of children, and log (household size) did not significantly differ from our measure of housing crowdedness. For respondents aged <17 years, controls include an indicator for daycare attendance before the age of 4 years, an indicator for whether the child was born outside the United States, and an indicator for whether the child's mother was born outside the United States. For respondents aged 25–49 years, age at first sexual intercourse, an indicator for more than 10 total lifetime sexual partners, and whether the respondent was born outside the United States are included as potential exposure mediators. Preliminary models included continuous measures of number of lifetime sexual partners, but the dichotomous measure provided the best fit. To account for potential increased susceptibility to infections, an indicator for whether the child was born with low birthweight (<2500 g) and whether there is a smoker in the home was included for respondents aged <17 years, and an indicator for current, former or never smoking was included for adult respondents.
Sexual history questions were not asked of adults aged >49 years, and thus these adults are included in the basic analysis represented in Figure 1 but not included in models testing potential mediators. Due to concern over measurement of income and education for college-age individuals, respondents aged 18–24 years are also included in basic analysis for Figure 1 but excluded from the full models testing potential mediators of the relationship between income, education, and CMV seropositivity.
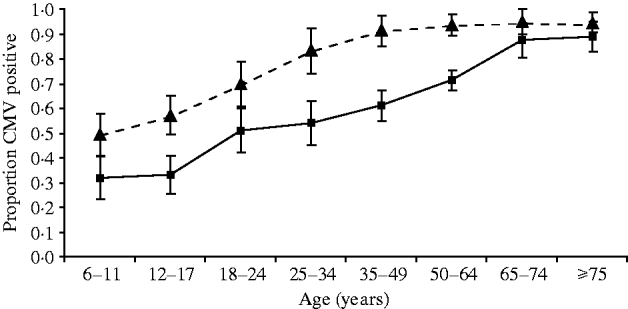
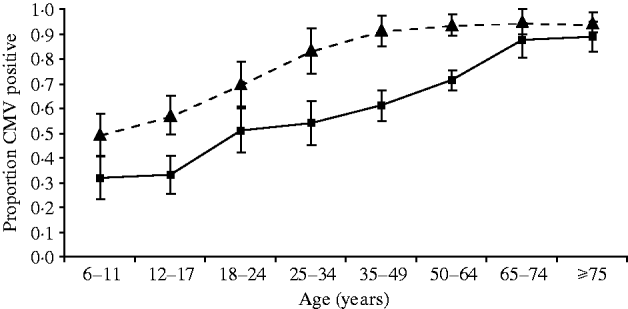
Fig. 1. Data from the Third National Health and Nutrition Examination Survey, 1988–1994, showing seroprevalence of cytomegalovirus (CMV) by age and income quartile. Results were adjusted for race/ethnicity, rural/urban residence, census region, sex, and household size. –■–, Top income quartile; –▲–, bottom income quartile.
RESULTS
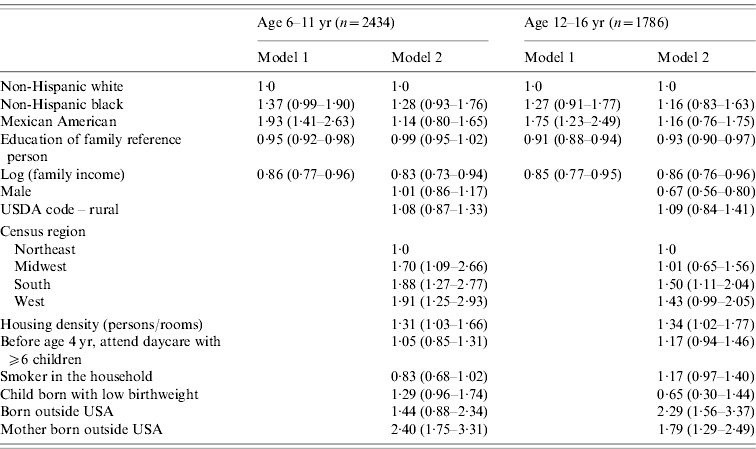
Figure 1 depicts rates of CMV seropositivity by age for the highest and lowest income quartile in NHANES III, adjusted for race/ethnicity, rural/urban residence, census region, sex, and household size. We see that cross-sectionally, income differences in seropositivity appear at early ages, widen in early and middle adulthood, then converge at older ages as almost everyone in the population is exposed. Table 1 shows descriptive statistics for our study sample. Table 2 shows the odds ratios for CMV seropositivity for ages 6–11 and 12–16 years. The first model estimates the effect of race/ethnicity and household SES on the odds of CMV seropositivity for children aged 6–11 years without adjustment for potential mediators. Adjusting for household SES, non-Hispanic black children aged 6–11 years have 37% higher odds of being infected with CMV compared to non-Hispanic whites, although the confidence interval includes the null value. Mexican American children have 93% higher odds of being infected in the 6–11 years age group compared to non-Hispanic whites. Both education of the reference person and family income are significantly related to infection status controlling for race/ethnicity, with each additional year of education of the family reference person corresponding to a 5% decrease in the odds of infection. Moving from a family income of $15 000 a year to $40 000 is associated with 14% lower odds of infection. Next we add controls for markers of potential exposures and susceptibility. Living in the northeast is associated with lower odds of infection, while household crowding and nativity of the mother outside the United States are significantly related to greater odds of infection for the 6–11 years age group. Living in a rural vs. an urban area, daycare attendance, having a smoker in the household, and being born with lowbirth weight are not significantly associated with infection status controlling for other factors. The addition of these potential mediators eliminates the racial/ethnic and parental educational differences in infection status in children aged 6–11 years, while the differences in CMV seropositivity by income remain unchanged. For children aged 12–16 years, the results are similar. Racial/ethnic differences in seropositivity are eliminated upon inclusion of mediators, but for older children the differences by both parental education and family income remain.
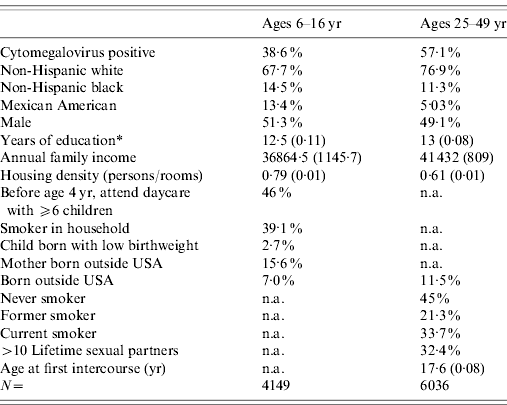
Table 1. Sample descriptive statistics (weighted) National Health and Nutrition Examination Survey III, 1988–1994
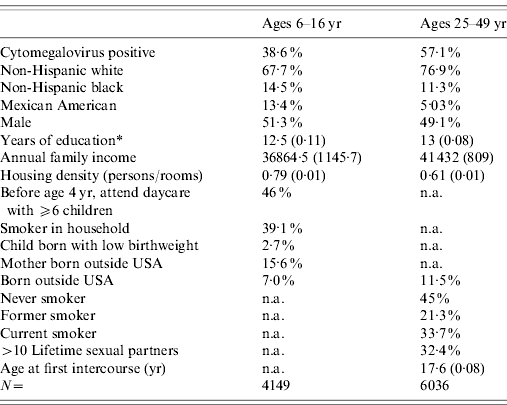
Percentage or mean and linearized standard error.
* Highest grade completed by household reference person for ages 6–16 yr.
Table 2. Risk factors for cytomegalovirus seropositivity for age <17 years, National Health and Nutrition Examination Survey III, 1988–1994

Values are odds ratio (95% confidence interval).
All models also control for age in months.
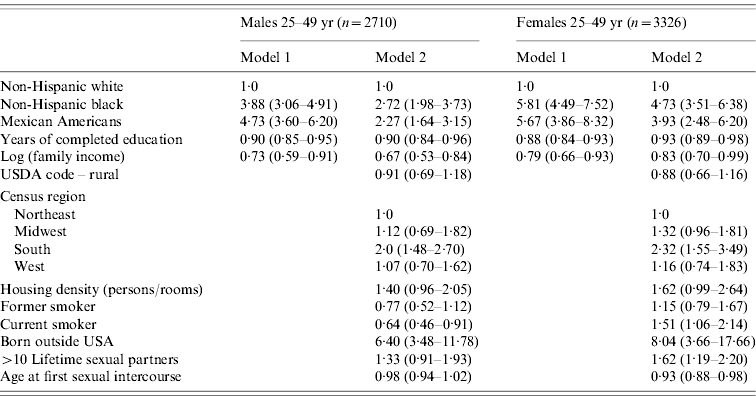
Table 3 presents results for adults aged 25–49 years separately by sex. Relative differences in seropositivity by race/ethnicity in this age range have greatly increased compared to the childhood sample, with non-Hispanic black males having almost four times the odds of infection compared to non-Hispanic white males, and Mexican American males having almost five times the odds of infection. The differences are even larger for females. Differences in infection status by education and income are also larger than the gaps at younger ages. Including controls for potential exposure, we see that being born outside the United States is a large, positive predictor of infection status in adults. Living in the south is also associated with higher odds of infection for both males and females. Population-based studies have suggested that sexual transmission is a likely risk factor for exposure to CMV [Reference Staras12, Reference Schillinger23]. Age at first intercourse and having more than ten lifetimes sexual partners are significant predictors of CMV infection status only for females. Household size and rural vs. urban residence are not associated with seropositivity in adults. Smoking is associated with a decrease in some immune markers, and thus may increase susceptibility to infection [Reference Evans24]. Interestingly, being a current smoker is significantly associated with infection status for both males and females, but in opposite directions. In fully adjusted models, smoking raises the odds of seropositivity for females, while being a current smoker is associated with a lower risk of seropositivity for males. With very little literature on the correlates of CMV infection in the general population, it is difficult to speculate as to the reasons behind these different results for smoking by gender. In models adjusted only for age, smoking remains positively associated with CMV infection for females but is not associated with CMV infection for males. Social factors related to smoking behaviour may differ by gender. If this is true, then even controlling for social factors associated with smoking such as race, income, and education, there may be residual unmeasured social factors associated with smoking that are also associated with the likelihood of CMV infection, and these factors may differ by gender. While racial/ethnic differences in positivity diminish slightly upon inclusion of controls for foreign-born status, region of residence, and sexual behaviours, they remain large. Importantly, income and education differentials were not explained by exposures commonly cited as risk factors for CMV.
Table 3. Risk factors for cytomegalovirus seropositivity ages 25–49 years, National Health and Nutrition Examination Survey III, 1988–1994
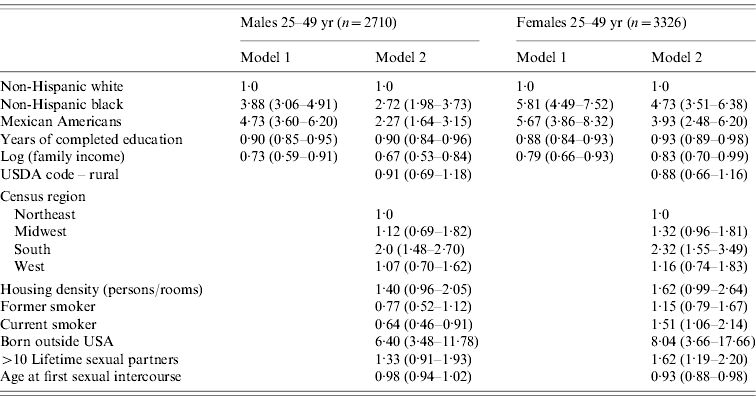
Values are odds ratio (95% confidence interval).
All models also adjusted for age in years.
DISCUSSION
This study represents a potential new direction for researchers investigating the biophysical mechanisms connecting SES and health outcomes. Numerous studies have documented an inverse association between SES and several chronic inflammation-associated conditions such as cardiovascular disease and dementia [Reference Diez Roux25–Reference Wilson28]. The biological pathways that mediate these relationships have not been thoroughly characterized. The social gradient in cardiovascular disease persists even after adjustment for health behaviours and many clinical indicators, suggesting that other processes may be involved [Reference Lantz4, Reference Lynch29]. It is possible that latent infections such as CMV may explain some of the socioeconomic gradients in cardiovascular disease and possibly other inflammatory-associated conditions. Recent research findings have shown that latent CMV infection in the elderly is an important component of a set of immunological parameters designated the ‘immunological risk phenotype’ [Reference Pawelec30]. This set of immunological markers, including latent CMV infection, high CD8 cells, low CD4 cell percentages, poor T-cell proliferation, is predictive of mortality among healthy elderly individuals [Reference Nilsson31, Reference Pawelec32]. While a definitive inference cannot be made based on cross-sectional data, the results of this study suggest that individuals with less education, lower income, and non-white race may spend a larger number of years infected with CMV on average by the time they reach older ages. Since the price paid for constant CMV immune vigilance may be high [Reference Koch33], early life disparities in CMV infection could have important implications for disparities in adult health.
Several studies have used herpesviruses, including CMV, as a marker of immune response to psychosocial stress exposures [Reference Glaser34]. Specifically, increases in herpesvirus antibody titres have been linked to academic stress in medical students and military cadets [Reference Glaser35], caregiving for a family member with Alzheimer's disease [Reference Glaser and Kiecolt-Glaser36], involvement in a poor quality marriage [Reference Herbert and Cohen37], anticipation of space flight by astronauts [Reference Mehta38], traumatic life events [Reference McDade39], as well as psychological traits of loneliness and anxiety [Reference Esterling40]. It is less clear, however, what role stress may play in initial susceptibility to CMV. Data examining respiratory infections have reported a relationship between low SES, increased levels of stress, and enhanced susceptibility to several cold and flu viruses [Reference Cohen9, Reference Cohen10, Reference Cohen41]. Low social class was associated with lower secretory immunoglobulin (sIgA), cited as a first line of defence against infection, in a large community sample in Scotland [Reference Evans24]. Taken together, these studies suggest that psychological stress associated with low SES can down-regulate various aspects of the cellular immune response, increasing susceptibility to infection. A recent study reported an association between levels of antibody to CMV and level of education in a sample of elderly Latinos [Reference Dowd42]. While measures of psychosocial stress are not available in the NHANES III data, further studies are needed to assess whether stress mediates the relationship between socioeconomic and race/ethnic differences in CMV susceptibility and antibody response.
There are several limitations to the current study. First, while our analysis has controlled for several exposure variables available in the data such as housing crowdedness, daycare attendance, and number of sexual partners, these variables are probably measured with error. For example, underreporting of the number of sexual partners is probable due to the sensitive nature of the question. Housing crowdedness and family size are imperfect measures of the transmission dynamics that actually determine an individual's risk of exposure. Being HIV positive or being otherwise immunocompromised would increase one's susceptibility to CMV infection, but this information is not available in our data. It is unlikely that these factors explain the differences in seropositivity status seen at early ages. Nonetheless, it is difficult to determine the importance of unmeasured exposures vs. susceptibility characteristics in explaining the socioeconomic and racial/ethnic differences in CMV seropositivity. Since the NHANES III data are cross-sectional, we are also not capturing new infections as we look across age groups, but are rather trying to explain differences in prevalence of this infection that could have been acquired at any age prior to measurement. Potential explanatory variables such as sexual behaviours are unlikely to explain CMV infections that were acquired in childhood. Since the seroprevalence rate for the overall 6–11 years age group is already 36·3%, there are important predictors of group differences in infection status that are potentially found in unmeasured early life exposures, especially parental or sibling risk factors. Another limitation is that while these are the most recent data available on CMV prevalence in the US population, this sample consists of respondents surveyed from 1988 to 1994, and thus might be less representative of the current social patterning of CMV infection in the United States.
In conclusion, we find socioeconomic and racial/ethnic disparities in CMV infection in the US population that are evident as early as age 6 years and persist through middle age. These differentials were not easily explained by exposures commonly cited as risk factors for CMV. Differences in lifelong exposure to persistent infections such as CMV may be one way in which lower social status contributes to poorer health outcomes. Future research should examine the exposure or susceptibility pathways responsible for these disparities in the prevalence of CMV infection.
ACKNOWLEDGEMENTS
We acknowledge the Robert Wood Johnson Health and Society Scholar Program for financial support of J.B.D. and D.E.A., and the University of Michigan – Medical School, Institute of Gerontology RCDC Fellowship support of A.E.A.
DECLARATION OF INTEREST
None.