Lymphogranuloma venereum (LGV) is a sexually transmitted infection (STI) caused by Chlamydia trachomatis serovars L1, L2 and L3, which causes an invasive disease via lymphatic spread at the site of the infection [Reference White1]. In Europe and North America, LGV has emerged as a significant problem during the past 7 years in men who have sex with men (MSM), particularly in those who are co-infected with the human immunodeficiency virus (HIV) [Reference Fenton and Imrie2].
The increasing incidence of LGV in MSM might be partially due to the HIV epidemic. Some MSM have changed their sexual behaviour and tend to participate in certain types of practices according to their HIV status [Reference Ronn and Ward3]. For example, serosorting and strategic positioning are two methods of seroadaptive behaviour. Serosorting refers to the selection of only sero-concordant partners for unprotected anal intercourse (UAI) [Reference Mc Connell4]. Strategic positioning is a tactic in which a HIV-infected individual assumes the receptive role during UAI with a negative or unknown-status partner [Reference Mc Connell4]. Seroadaptive behaviour is a strategy perceived as a method to reduce new HIV infections, but creates dense sexual networks where co-infection with other STIs and disease propagations are high.
Barcelona is a European city with a low-level of concentrated epidemic (where high levels of infection are found in specific groups) based on data collected from populations most at risk, specifically, MSM. The incidence rate of HIV in Barcelona in 2012 was 909/105 MSM per year and 20/105 persons per year in the general population.
Most of the LGV cases have been reported in HIV-positive MSM [Reference Vargas-Leguas5]. In the present study, we reviewed the incidence rate of reported LGV in MSM in Barcelona since 2007 and described the epidemiological, clinical and sexual behaviour characteristics of LGV cases per year of diagnosis to assess seroadaptive behaviour as a risk factor for LGV transmission during 2012.
LGV epidemiological surveillance in Barcelona has been active and mandatory since 2007 and collects information about reported diagnosis in individuals who visited public health facilities. Foreigners who are registered in Spain and in the municipality in which they habitually reside, have the right to health services on the same conditions as Spanish citizens. Therefore, all those who were diagnosed and treated for LGV and were residents of Barcelona were reported. Clinicians who made the diagnosis were from the city's STI clinic (75·2%) and from third-level hospitals (24·8%). Hence, diagnosis and treatment of LGV is openly available for those who seek assistance, not just for MSM. A standard questionnaire regarding demographic, clinical and epidemiological data was completed [6]. People who were diagnosed in Barcelona and were tourists, were not included in this analysis.
All data were collected by the Barcelona STI registry and handled on a strictly confidential basis according to the requirements of Spanish Data Protection Law. Symptomatic cases with a possible diagnosis of LGV were screened on the sites of lesions and asymptomatic cases, who were in contact with LGV-positive cases, were screened on the anal and perianal region. In all cases that were declared, C. trachomatis was detected by nucleic acid amplification tests and positive samples were then confirmed by a second real-time multiplex polymerase chain reaction which differentiates LGV from non-LGV strains [Reference Chen7]. Since the beginning of the LGV epidemic, the same testing method has been used.
As part of the surveillance system, patients with a reported and confirmed LGV diagnosis were telephoned in order to follow-up treatment and to establish their sexual contacts. Authorization was established before the telephone questionnaire was administered. Questions regarding sexual behaviour and seroadaptive practices were included during 2012. The telephone questionnaire is provided as Supplementary material.
Descriptive statistics were used to analyse the epidemiological and clinical data of detected LGV cases from January 2007 to December 2012. LGV annual rate ratios in MSM aged between 15 and 69 years were compared with cases from 2007, based on data obtained from the population-based statistics registry of Barcelona [8] and from an estimation of the proportion of MSM from the city health survey (5·3%) [Public Health Agency of Barcelona, 2013 (Barcelona Health survey, 2011), unpublished observations]. Rate ratios were statistically analysed using the Poisson test, and 95% confidence intervals (CIs) were calculated.
LGV was reported in 206 cases. The incidence rate of LGV in MSM aged between 15 and 69 years old ranged from 32·1/105 MSM per year in 2007 to 182·7/105 MSM per year in 2012. Epidemiological, clinical and sexual behaviour characteristics are described in Table 1. The median age of cases was 36 years old (range 19–58 years), 76·7% had secondary or undergraduate level of education and 58·7% were Spanish. HIV co-infection was observed in 84·0% of cases, with the highest proportion found in 2011 with 92·6%. Most of the cases were symptomatic (94·2%), just 5·8% were asymptomatic. During the last 12 months, 34·1% were diagnosed with another STI. The median number of days between symptoms and diagnosis was 25 [interquartile range (IQR) 10–51. Table 2 shows the results from Poisson regression for LGV in MSM aged between 15 and 69 years. The rate ratio increased in 2011 (2·2, 95% CI 1·5–2·9) and 2012 (1·7, 95% CI 1·0–2·4), compared to cases from 2007 and was statistically significant.
Table 1. Epidemiological, clinical and sexual behaviour characteristics of lymphogranuloma venereum (LGV) cases in men who have sex with men (MSM), Barcelona 2007–2012

HIV, human immunodeficiency virus; STI, sexually transmitted infection; IQR, interquartile range.
* All cases were men who have sex with men (MSM)
† Annual incidence rates in MSM (aged between 15 and 69 years) were calculated based on data obtained from the Registry of Barcelona [8] and from an estimated proportion of MSM based on the city health survey of 5·3% [Agència de Salut Pública de Barcelona, 2013 (Barcelona Health survey, 2011), unpublished raw data].
‡ N = 105. Median was calculated from the number of men who answered this question.
Table 2. Incidence rate ratios (IRR) for LGV per year of diagnosis from Poisson regression model.
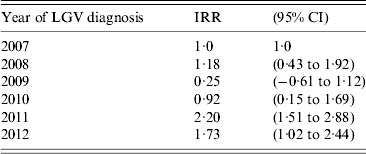
CI, Confidence interval.
Of the 206 cases, 105 (51·0%) answered the question related to the number of sexual partners during the last 12 months in the standard questionnaire; the median number was 1 (IQR 0–15·0), with the highest median of sexual partners in 2012 at 10 (IQR 0–30·0), and almost 71·8% of LGV cases (148/206) claimed to have had a new sexual partner during the last 3 months.
A total of 31/51 cases (61%) answered the telephone questionnaire in 2012. The remaining 19 did not give authorization for the survey nor could not be located. From the telephone questionnaire, a total of 84% (26/31) were HIV positive, 39% (12/31) reported having sex according to the serostatus of their partners, and 7% (2/31) used strategic positioning as a seroadaptation method. Of those who were HIV negative (5/31), just two reported using serosorting as a method of seroadaptation and all five reported having a receptive role during UAI. Of the total number of men interviewed by phone, 45% (15/31) reported that the internet was a source to search for a sexual partner, 16% (5/31) reported having sex in saunas and 19% (6/31) reported having sex in bars.
A question related to unprotected sex at the last intercourse was included in both questionnaires. In the standard questionnaire, this question was answered positively by 65·0% (134/206) of the total number of reported LGV cases, 44% (4/9) in 2007, 67% (20/30) in 2008, 58% (7/12) in 2009, 65% (15/23) in 2010, 67% (54/81) in 2011 and 67% (34/51) during 2012. The trend of unprotected sex has not changed throughout the whole period, the percentage increased slightly during the first periods but in the last two it remained the same. Of those who answered the telephone questionnaire, 81% (25/31) claimed to have had unprotected sex during their last intercourse.
In the standard questionnaire, a validation of this question was made by comparing answers from the telephone questionnaire in 2012. We found that of those who answered positively to this question in the telephone questionnaire (n = 25), two men answered negatively in the general questionnaire. Of those who answered negatively in the telephone questionnaire (n = 6), just one man admitted to having had protected sex at the last intercourse in the general questionnaire. Therefore, just 10% of the data, that was possible to compare (3/31), was different in both questionnaires, which suggests that the standard questionnaire has a high percentage of validation, providing accurate and reliable data.
LGV is an emerging STI and most of the cases are HIV positive and related to risky sexual behaviour. Our results are similar to those reported from 2003 to 2008 in the rest of Europe, in which around 97% of new LGV cases were HIV positive. In the UK, Sweden and The Netherlands, 99·5% of LGV cases were in MSM, and most were symptomatic, and primarily found in the anal/perianal regions [Reference Savage9]. Regarding the large populations of MSM who have established gay scenes, a recent study in the UK reported that 82% of cases of LGV were HIV positive, and most were involved with risky sexual behaviour and were concentrated in large cities, especially London [Reference Hughes10].
In a systematic review of 30 US studies [Reference Crepaz11], the authors found that MSM who were aware of their serostatus were more likely to engage in seroadaptive behaviours. Our results showed that less than half of MSM with LGV in Barcelona reported seroadaptive behaviours. Nevertheless, the authors believe that seroadaptation is common practice in the city, as most of the LGV cases were co-infected with HIV and were seeking unprotected sex. Seroadaptive behaviours probably contributed to increasing co-infection between HIV and LGV during the LGV epidemic in the UK [Reference Ward12].
The increase in co-infection in this study can also be explainded by dense sex networks where contacts meet through the internet, sex parties and clubs [Reference Crepaz11]. Use of the internet may assist seroadaptation, in that the anonymity it affords, can facilitate seeking HIV sero-concordant sex partners and sero-disclosure [Reference Chongyi13].
The increase in reported LGV cases may result from an increase in transmission through sexual networks, awareness of the disease in patients and clinicians, and screening of asymptomatic cases who were in contact with LGV-positive cases. Thus, there is a continued need to monitor trends in LGV diagnoses. A limitation of this study is the small number of people who answered the telephone questionnaire in 2012 and the impossibility of confirming partner HIV status. However, despite a scarcity of data and an absence of serological confirmation, the results provide useful information to direct prevention efforts. LGV prevention should encourage health information in sex venues such as saunas and bars. Moreover, the use of new technology such as internet-based interventions and mobile phone applications, can be part of a public health strategy to raise awareness of LGV and other STIs and to target complex sex networks.
APPENDIX. Barcelona STI Group
Marc Marti-Pastor, Pere Armengol, M. Jesus Barbera, Alvaro Vives, Gemma Martin-Ezquerra, Merce Alsina-Gibert, Jose Luis Blanco, Carlos Muñoz-Santos, Antonia Andreu, Pilar Gorrindo, Sonia Gil.
SUPPLEMENTARY MATERIAL
For supplementary material accompanying this paper visit http://dx.doi.org/10.1017/S0950268814000545.
ACKNOWLEDGEMENTS
The authors acknowledge the Epidemiology Service Group from the Public Health Agency of Barcelona for their collaboration throughout this project. Thanks are also due to all the doctors who reported LGV cases in the city of Barcelona.
DECLARATION OF INTEREST
None.







