INTRODUCTION
Salmonella enterica serovar Newport (S. Newport) is an uncommon cause of gastroenteritis in Northern Ireland with on average 2–3 cases reported annually.
Investigations of S. Newport outbreaks in USA and Europe have implicated exposure to raw or undercooked ground beef, horse meat, pre-cooked pork and beef products, cheese made from unpasteurized milk, and a variety of produce including tomatoes, mango and alfalfa sprouts [1–Reference Van Beneden8]. Outbreaks in Great Britain have been linked to the consumption of cured ham and ready to eat pre-packed salad [Reference Lyytikainen9, Reference Ward10].
Routine surveillance of Salmonella in Northern Ireland is based on laboratory reporting. However, laboratories vary in their ability to fully identify less common strains of Salmonella such as S. Newport, and in their berral patterns for confirmation and subtyping. Thus some ber to the Northern Ireland Public Health Laboratory (NIPHL) or the Laboratory of Enteric Pathogens, Colindale (LEP), with others making no routine onward berral.
Initial reporting of the outbreak
On 7 September 2004, the Communicable Disease Surveillance Centre, Northern Ireland [CDSC(NI)] was notified by two health boards of 17 cases of group C Salmonella isolated over the previous week. Initial anecdotal information showed the earliest date of onset of illness to be 25 August and suggested an association with a variety of fast-food premises, but with no single food item suspected. Subsequently, the Health Protection Agency (HPA) Centre for Infections reported that S. Newport outbreaks with a similar timescale were occurring in the North East (NE) Lincolnshire and the West Midlands areas of England. During the first meeting of a Regional Outbreak Control Team on 13 September 2004, an outbreak investigation was started with the aim of describing the outbreak and identifying a common food exposure in order to guide control measures.
METHODS
Descriptive epidemiology/hypothesis generation
A case was defined as a confirmed S. Newport infection in a resident of Northern Ireland with enteric illness with onset of symptoms on or after 20 August 2004, reported by the NIPHL or LEP, Colindale.
Cases were excluded if they reported travel outside the UK in the 7 days before illness (travel-associated cases) or contact with other individuals with gastrointestinal symptoms in the 7 days before illness (secondary cases).
General practitioners were contacted with details of the outbreak and a request to report any future cases to the appropriate health board. Environmental health officers (EHOs) conducted face-to-face or telephone interviews with cases using a generic hypothesis generation questionnaire, gathering information on demographic and clinical variables, and on food exposures in the 7 days prior to illness. The questionnaire sought detail on 96 different food-type exposures under 18 broad food group categories. A master database of questionnaire data was maintained by CDSC(NI) and analyses disseminated at regular intervals to members of the outbreak control team.
Infection rates for district council (DC) areas were calculated using confirmed primary cases as the numerator and Northern Ireland Statistics Research Agency 2003 mid-year population estimates as the denominator.
Case-control study
A matched case-control study was undertaken to test the hypothesis that enteric illness due to S. Newport was associated with eating lettuce or other salad vegetables in a meal eaten outside the home. For the purposes of the case-control study, the population at risk was defined as residents of Northern Ireland who had consumed foods outside the home in the period from 20 August 2004.
Cases were asked to nominate up to three controls; a control being defined as a person who had eaten a meal with the case at a catering premises outside the home, during the 72 h prior to onset of illness in the case. Cases and controls were interviewed by questionnaire, either face-to-face or by telephone. Response rates were not collected systematically. For cases, data were collected only for meals eaten outside the home during the 72 h prior to the onset of their illness. For controls data were collected only on meals eaten outside the home with cases during this time. Where cases had eaten at more than one catering premises outside the home in the 72 h prior to illness, exposure details were amalgamated for the case. Sample size calculations based on a hypothesized exposure level of 30% in controls and, from the descriptive study, 70% in the cases suggested that 18 cases and 54 controls, or 21 cases and 42 controls, would have to be interviewed to detect an odds ratio of 5·4 with 80% power and 5% significance.
Statistical analyses
Univariate and multivariate analyses were performed using Stata version 10 (Stata Corporation, USA). Food-specific odds ratios (OR) and 95% confidence intervals (CI) were calculated. The χ2 test was used to compare proportions between groups and Fisher's exact test employed where expected cell values were <5. Exposure variables significant at less than the 5% level on univariate analysis were included in a conditional logistic regression model which was then simplified using backward elimination and the likelihood ratio test with a cut-off P value of 0·05.
Microbiological methods
Faecal samples from patients were submitted to a number of hospital microbiology laboratories for culture. Guidance was circulated to laboratories at the outset of this outbreak, requesting that all Salmonella isolates identified as O:6,8, O:8, O:6,7,8 or group C Salmonella were berred to the NIPHL or the HPA LEP for full identification. Such cases were reported as ‘possibles’ to CDSC(NI) by the health boards and included in the descriptive study, until their final status was determined. All isolates from Northern Ireland laboratories were berred to LEP for subtyping using pulsed field gel electrophoresis (PFGE) [Reference Peters11–Reference Fontana13].
Environmental investigation
Food premises associated with cases were inspected by EHOs. Investigation concentrated on observation of food-handling practices, the procurement of food samples for microbiological testing, and the documentation of the supply chain of salad vegetables to the premises. The distribution of salad vegetables into and within Northern Ireland was examined with particular attention paid to a comparison of arrangements in those areas with high rates of illness with those areas with no cases. Furthermore, detailed descriptive epidemiology and initial analytical investigation of the coincident cluster of cases in NE Lincolnshire, suggested strongly that lettuce was the vehicle of infection in that cluster (I. A. Gillespie, unpublished observations).
An urgent enquiry was sent to participants of the international surveillance network Enternet [Reference Fisher14] on 8 September 2004 informing them of the increase and requesting additional information from any countries that were experiencing a similar increase in S. Newport infection.
RESULTS
Descriptive epidemiology/hypothesis generation
A total of 130 confirmed cases were reported with dates of onset of illness ranging from 25 August to 14 October. Eight were classified as secondary cases, and seven as travel-associated. There was insufficient information to classify a further ten cases, leaving 105 known primary cases. The epidemic curve suggests a continuing exposure over a ~4-week period (Fig. 1).
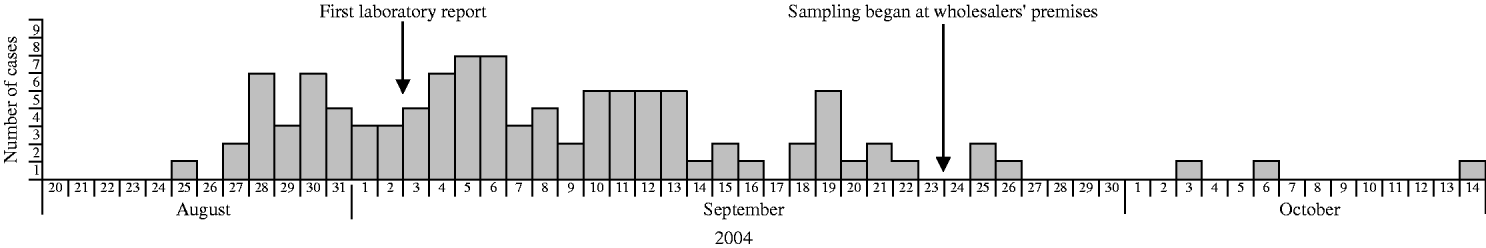
Fig. 1. Confirmed cases of Salmonella Newport, excluding travel-associated and secondary cases, by date of onset of illness, Northern Ireland, 20 August to 14 October 2004 (n=102). Date of onset of illness missing for three cases.
Forty-five per cent (47/105) of cases were male. Ages ranged from 1 to 89 years (median 33 years). Almost half (48%, 50/105) of cases were in the 20–34 years age group). Twenty-seven per cent (25/94) of cases were hospitalized. For 11 cases this information is unknown. No associated deaths were reported.
The distribution of cases by DC area of residence was not uniform (Fig. 2). The highest incidence occurred in Limavady DC at 39/100 000 population, and this region accounted for 14% (13/95) of cases where residence was known. Six DC areas had no cases. Of these, Derry in particular stands out, given its large urban population and proximity to heavily affected Limavady. Only one case was reported during the course of the outbreak to the Health Protection Surveillance Centre in the Republic of Ireland; in a resident of neighbouring County Donegal.
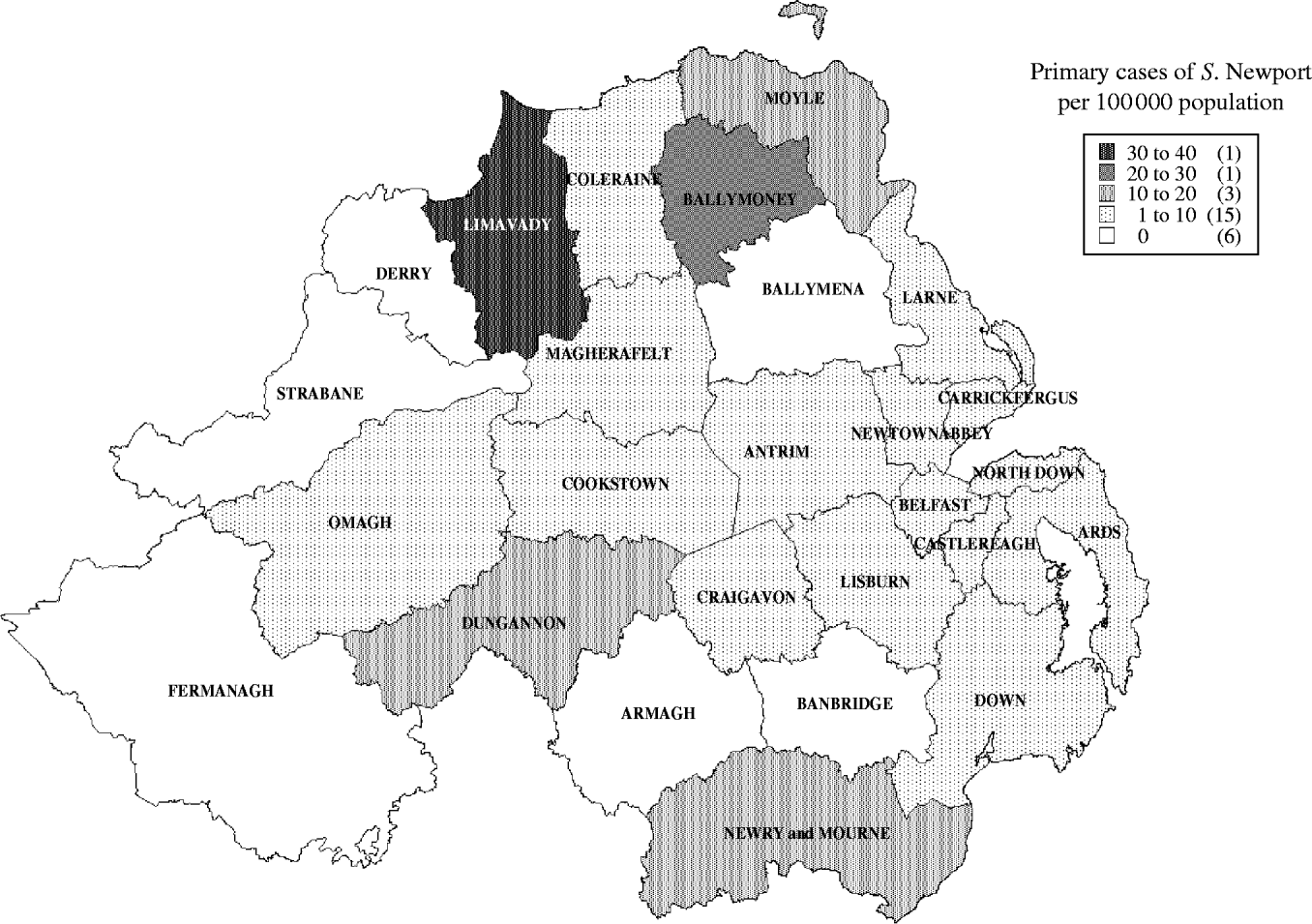
Fig. 2. Confirmed cases of Salmonella Newport, excluding travel-associated and secondary cases, with onset of illness 25 August to 14 October 2004 per 100 000 population, by Northern Ireland District Council of residence (n=95). (Based upon Ordnance Survey of Northern Ireland's data with the permission of the Controller of Her Majesty's Stationery Office, © Crown copyright and database rights NIMA ES&LA 210.4.)
The trawling questionnaire showed that 82% (78/95) of cases ate at least one meal outside the home in the 7 days preceding illness and 58% (55/95) ate food from a fast-food takeaway during this time. Cases had purchased or consumed food in or from 121 different premises in the 7 days prior to illness. Fifty-three of these were fast-food takeaways, the majority of which were American-style hamburger outlets and ‘fish-and-chips’ shops. Other implicated premises included cafes, restaurants and hotels. Five clusters (each with three or more primary cases associated with a particular catering premise or chain of premises) were identified accounting for a total of 19 cases. Three clusters were centred on different fast-food takeaway chains, and two centred on a café/restaurant premises within two small towns.
Of food eaten outside the home, poultry and salad were mentioned more frequently than other groups of food items [52% (49/95) and 48% (46/95), respectively], compared to pork products (24%), egg/egg products (22%), beef (25%), sauces (15%), cheese (13%) and seafood (14%). No specific proprietary brand of food item was identified as a common exposure.
The urgent enquiry through Enternet did not identify any additional cases other than those in Great Britain.
Analytical study
Between 20 September and 8 October 2004, 34 cases and 46 matched controls were interviewed as part of the case-control study. Four of the cases were found to be secondary cases or travel-associated and, together with their seven controls, excluded. An additional seven cases were excluded as they had had no controls, leaving 23 cases and 39 controls for the matched analysis. Study cases were representative of all cases with regard to age (mean 40 vs. 38 years, two-sided t test P=0·6) and gender (43% male vs. 45%, χ2P=0·9), and to area of residence when analysed at health-board level.
Exposure details were amalgamated for three cases that had eaten two meals each during the exposure period. None of the controls had eaten more than one meal with a case.
Univariate analysis showed a statistically significant association with the consumption of lettuce and the development of gastrointestinal illness (Table 1). Upon conditional logistic regression, only the consumption of lettuce was independently associated with being a case (OR 23·7, 95% CI 1·4–404·3) (Table 2).
Table 1. Demographic factors and risk exposures for cases of Salmonella Newport infection and matched controls. Northern Ireland, 20 August to 14 October 2004 (single risk variable analysis)
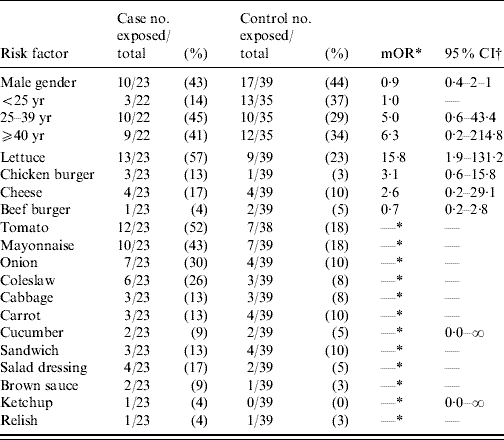
mOR, Matched odds ratio; CI, confidence interval.
* Unable to estimate as either all the cases and controls, or none of the cases and controls in the matched pairs had eaten those foods.
Table 2. Demographic factors and risk exposures for cases of Salmonella Newport infection and matched controls. Northern Ireland, 20 August to 14 October 2004 (final conditional logistic regression model)

mOR, Matched odds ratio; CI, confidence interval.
Laboratory results
S. Newport was isolated from faecal samples from 129 patients and a blood culture from one patient. Northern Ireland S. Newport isolates typed by LEP showed a PFGE pattern indistinguishable from outbreak strains in England, Scotland and the Isle of Man. They were similar but not identical to S. Newport isolates from both lettuce and humans samples obtained during the outbreak in England in 2001. No food or environmental samples submitted to laboratories in Northern Ireland or Great Britain as part of the current outbreak investigation yielded S. Newport.
Environmental results
Investigation of 87 different implicated food premises showed the majority to have purchased iceberg lettuce as whole heads rather than in pre-prepared form, and that lettuce was generally stored under brigeration until needed. However, there was greater variation in preparation, with some premises reporting washing/steeping in salt or sanitizer, and others not washing the lettuce at all. Storage was then generally at ambient temperature until use. In some premises the temperature of lettuce at point of sample was >20°C.
Given the delay between exposure and reporting of illness, no samples of leftover food from suspect meals were available for testing. In total, 308 samples of foodstuffs were submitted by EHOs for testing. These included lettuce (56 samples), onions (17), tomatoes (22), salad (46), coleslaw (10) and chicken products (32). These were taken from either retail premises mentioned by cases or wholesale premises that may have supplied food to affected individuals. The first food samples from a retail premises were submitted on 10 September, and sampling of lettuce from wholesalers' premises took place on 24 September and 22 October.
Wholesalers' investigation
In Northern Ireland lettuce is imported year round. Most lettuce comes into Northern Ireland via the wholesale market in Belfast and is distributed to both affected and unaffected areas through independent wholesalers. Agents at markets in the UK and continental Europe buy produce there with subsequent shipping to Belfast. Stock tends to be moved between wholesalers in response to demand. In addition, some local distributors import lettuce directly from UK and Republic of Ireland (and some EU) suppliers. The supply of lettuce to Northern Ireland therefore varies on a daily basis. Northern Ireland-grown lettuce is not supplied to England, Scotland or Wales.
Supply data were analysed from a number of food premises with more than one case and a link was established with ten premises having been supplied either directly or indirectly by a company in the East of England. The company used many different growers and supplies varied daily. This company supplied about 20 000 heads of lettuce to Northern Ireland each week. However, it also supplied a number of large food manufacturers who undertake extensive product testing. No problems were identified by these companies during the period of investigation.
DISCUSSION
We report the largest outbreak of salmonellosis in Northern Ireland since 1987, and the first to involve the serovar S. Newport. Its time-course mirrored those of S. Newport outbreaks in NE Lincolnshire and the West Midlands in England, Scotland and the Isle of Man. A total of 677 cases of S. Newport infection were reported in England and Wales between weeks 36 and 46, before returning to baseline levels [15]. The PFGE pattern of isolates of S. Newport from Northern Ireland were indistinguishable from human isolates of S. Newport in Great Britain suggesting illness in these regional clusters was associated with the consumption of a common foodstuff.
We conclude that this outbreak was associated with eating lettuce in a meal outside the home. Concurrently conducted case-control studies in NE Lincolnshire focusing on the two fast-food premises accounting for most of the cases there, found that the consumption of lettuce was associated with being a case of S. Newport infection (OR 11·4, 95% CI 1·9–70·3; OR 12·8, 95% CI 3·34–49·12) [16]. A similar case-control study in the West Midlands failed to identify an association, possibly due to the small number of controls recruited into the study [15]. It is unlikely that transmission within this outbreak was limited to the outside catering sector. Indeed, almost a fifth of cases in our investigation reported consumption of lettuce only within the home. However, most cases reported consumption of lettuce outside the home, justifying the focus for this investigation and highlighting the role of appropriate storage of salad items throughout the supply chain and especially in the catering environment.
Salad vegetables and fruit are increasingly recognized as the vehicle of foodborne outbreaks, being implicated in 6% (83/1518) of foodborne outbreaks of infectious intestinal disease in England and Wales between 1992 and 2000 [Reference Long17]. Similar figures have been reported from Australia and the USA [Reference Dalton18, Reference Sivapalasingham19]. While many of the outbreaks in England and Wales apparently had their origins in commercial catering premises or private households three major outbreaks were attributed to lettuce contaminated at source [Reference Long17]. Two of these outbreaks caused concurrent illness in a number of other European countries.
Notably, our investigation failed to provide microbiological evidence of a link with contaminated lettuce, a common finding with other outbreaks associated with salad vegetables and fruit [Reference Long17]. The short shelf life of lettuce, the inherent delays in laboratory reporting and the time taken to develop this hypothesis and to commence sampling will have contributed to this. In this study sampling of lettuce from wholesalers' premises took place on 24 September and 22 October by which time contaminated product was unlikely to still be in circulation. This highlights the importance of analytical epidemiology in the detection of outbreaks due to salad vegetables.
Investigation of the supply chain of lettuce into and within Northern Ireland provided little useful information, other than establishing the likelihood that the contaminated product originated from outside Northern Ireland, given that the outbreak strain was indistinguishable from that seen in Great Britain, and that no lettuce is supplied to Great Britain from Northern Ireland.
Initially we had hoped that variation in DC area infection rates would allow us to identify potential differences in the supply chain. However, while four of the six DC areas with no cases reported abut the border with the Republic of Ireland, Belfast wholesalers' records showed supply to clients in these areas also. Nevertheless, it is likely that some salad supplies to these areas came from the Republic of Ireland and this may go some way to explaining their absence of cases.
Ultimately, however, due to the complexity of the supply chain and limited traceability we were unable to find the source of the implicated product. Similar experience has been reported by other investigators where contaminated lettuce has been implicated by epidemiological studies [Reference Horby20]. Since this outbreak, there is now a statutory requirement for all food businesses to have a reliable traceability system in operation whereby they can identify suppliers and customers (one up/one down) [21]. Although untested as yet in Northern Ireland, it is hoped this legislation will prove to be of significant benefit in possible future outbreaks of this nature.
Control measures during this outbreak were limited to public media messages around the safe preparation and storage of food, and in particular salad vegetables. A leaflet specifically directed at caterers was produced with this same message. The inability of the Outbreak Control Team to direct effective control measures at the product source, and to develop preventive measures for the future, remains the central area of concern. While it is important that education continues around the need to wash salad vegetables and fruit before consumption, simple washing will only reduce bacterial levels by a factor of 0·8 log [Reference Smith22]. Prevention of contamination at source therefore remains of paramount importance [Reference Dalton18].
Our analytical study included cases that had eaten at more than one premises within the 72-h period before onset of illness. As it would not be possible to determine at which premises exposure to the contaminated food occurred, case exposure details were amalgamated for the different premises visited by the case. As a consequence, therefore, cases may have become more likely than controls to report a particular exposure since their exposure assessment bers to more than one premises, and not only one as for controls. However, there is no reason why this potential bias should apply preferentially to lettuce.
Cases were asked to nominate up to three controls that had eaten a meal outside the home with the case. Controls, therefore, were matched to cases on the type of premises visited, making it impossible to examine the role of premise type in disease risk. Furthermore, case-nominated controls increase the potential for over-matching due to friends' similarities [Reference McCarthy23], and this might be exacerbated by the relatively limited menu choices available in fast-food premises. This might explain why we were unable to estimate matched odds ratios for a number of exposures due to all positive or all negative outcomes.
CONCLUSIONS
Our findings add to the growing weight of evidence linking salad vegetables to human gastrointestinal illness. Despite closely controlled production using the principles of Hazard Analysis Critical Control Point (HACCP), salad vegetables are often produced in close proximity to the external environment. Given the international nature of the supply of such produce on a year-round basis, the opportunity for disseminated national and international outbreaks exists. The identification of such outbreaks relies on the routine application of discriminatory molecular typing techniques and the sharing of these data across borders. The use of a standardiszed epidemiological tool for all salmonellas will also assist in outbreak identification. Analytical epidemiology is especially important in this context as microbiological confirmation of pathogens in short shelf-life products may not be forthcoming. Its application in outbreaks linked to takeaway premises, whilst conceptually problematic, is possible.
APPENDIX
Members of the Outbreak Control Team: L. Dargan, E. Davies, M. Devine, P. Donaghy, S. Feeney, W. N. Irvine, M. McCarthy, A. McClenaghan, A. McClune, J. McKee, O. McWilliams, I. Maginnis, P. Rooney, R. Smithson, B. Smyth, V. K. Tohani.
ACKNOWLEDGEMENTS
The Outbreak Control Team gratefully acknowledges the contribution of Environmental Health staff across Northern Ireland.
DECLARATION OF INTEREST
None.






