INTRODUCTION
Chlamydia trachomatis is the most common bacterial sexually transmitted infection (STI) worldwide [1]. In Australia, an estimated 40% of diagnoses are in men [2]; the prevalence of rectal chlamydia is 5·6% in men who have sex with men (MSM) and infections are associated with an increased risk of HIV transmission [Reference Bernstein3].
Current guidelines for MSM from the Center for Disease Control and Prevention recommend that all positive uncomplicated chlamydia infections be treated with a single 1 g dose of azithromycin or 7 days (100 mg twice daily) of doxycycline [4]. However, there is increasing concern about rectal chlamydia treatment failure with about 22% of MSM presenting with repeat chlamydia infection following treatment with azithromycin [Reference Kong5]. In response to these concerns, European [Reference Lanjouw6] and Australian [7] guidelines have been recently revised and now recommend rectal infections be treated with 7 days doxycycline as first-line treatment. It is important to note, however, that there are only observational studies and no randomized controlled trials (RCTs) comparing azithromycin with doxycycline for the treatment of rectal chlamydia, so the level of evidence supporting this recommendation is limited.
High organism load has been associated with the failure of azithromycin to treat genital chlamydia in studies of women [Reference Walker8] and trachoma [Reference West9]. However, there are few data available regarding the association between rectal chlamydia treatment failure and organism load. What is known is that higher organism loads are reported at the rectal site compared to other genital sites [Reference Vodstrcil10] and that chlamydia isolates demonstrating heterotypic resistance to macrolides in vitro have been reported [Reference Bhengraj11] at high, but not low, levels of organism load [Reference Wang12].
This study aimed to estimate the risk of repeat rectal chlamydia infection in MSM and to investigate the association between organism load and repeat rectal infection following treatment. We also investigated rectal chlamydia genovar distribution in MSM and calculated the efficacy for those treated with 1 g azithromycin.
METHODS
Study participants, inclusion and exclusion criteria, data collection
This is a retrospective study of stored samples from asymptomatic MSM attending Melbourne Sexual Health Centre (MSHC, Australia) between July 2008 and October 2013 who had a follow-up test result within 100 days of an initial (index) rectal chlamydia infection. At MSHC, all rectal swab samples are clinician-collected without the aid of an anoscopy. All chlamydia-positive rectal swab samples were tested using the BD strand displacement amplification (SDA) test (BD ProbeTec; Becton, Dickinson and Company, USA) and were subsequently stored in BD transport medium at −80 °C for research purposes. For individuals who had multiple positive tests during the study period, only the most recent test/retest samples were included. Men diagnosed symptomatically for lymphogranuloma venereum (LGV) or proctitis was excluded as these patients would have been treated with extended treatment courses. At MSHC, LGV is treated with 3 weeks doxycycline (100 mg twice daily) and proctitis is treated with combination therapy using a single dose of 1 g azithromycin, 3 weeks doxycycline (100 mg twice daily), 500 mg ceftriaxone and 500 mg valaciclovir twice daily for 7–10 days. Any asymptomatic LGV cases detected as a result of this study were included in the analysis because these cases were originally managed as uncomplicated chlamydia infection as is clinical practice for any asymptomatic rectal chlamydia infection in the absence of genotyping. Electronic patient data were extracted for individuals. This included the patient's age, treatment received at the time of the initial diagnosis, date of drug prescription, co-infections with other STIs including HIV, past STIs, sexual risk behaviour and presence of any rectal symptoms. The time between treatment and repeat testing was estimated based on the date of the actual drug prescription.
Testing, organism load, genovar and multilocus sequence typing (MLST) testing
Stored chlamydia SDA-positive rectal samples were sent to the Department of Microbiology and Infectious Diseases, at the Royal Women's Hospital, Melbourne, Australia for chlamydial bacterial load, genovar and MLST testing.
DNA extraction
A 200 µl aliquot was extracted by using the automated system, MagNA Pure 96 (Roche Applied Science, Germany) according to the manufacturer's instructions. The total nucleic acid was then eluted in a final volume of 100 µl in MagNA Pure 96 elution buffer.
Chlamydia genovar and bacterial load
Aliquots of 5 µl of the extracted nucleic acid was utilized in each qPCR assay for determination of bacterial load and chlamydial genovar as described previously [Reference Stevens13]. The chlamydial load in each tested sample was quantified by comparing the crossing threshold of each sample to the crossing threshold of a standard curve constructed by amplifying different known copy numbers of the omp1 gene. In addition, an aliquot of DNA was amplified for β-globin gene as an internal control to assess sampling adequacy. Results were calculated in copies/ml and were log-transformed for analysis.
MLST analysis
For individuals with two sequential positive samples with identical genovar, MLST was performed to help differentiate between treatment failure and reinfection by evaluating any sequence variation across five genes, i.e. CT144, CT058, CT172, pbpB and hctB [Reference Bom14] and compared to an online MLST database (http://mlstdb.bmc.uu.se/).
Outcome definition
Our primary outcome was repeat rectal chlamydia infection diagnosed by SDA test within 100 days of diagnosis and treatment for an index rectal chlamydia infection. For the secondary outcome, we further classified a repeat rectal chlamydia infection as a treatment failure or reinfection using both the genovar and reported sexual behaviour (Table 1). Our classification of treatment failure is conservative; all repeat infections of the same genovar in individuals who report condomless sex, are classified as reinfection.
Table 1. Algorithm to differentiate between reinfection and treatment failure

* Reported had male sex partners in the last 3 months.
† Reported specifically had condomless sex as a receptive partner in the last 3 months.
Statistical methods
Descriptive statistics were used to describe the characteristics of men participating. The proportion and 95% confidence intervals (CIs) of men who had a repeat positive diagnosis was calculated using exact binomial methods. Our primary outcome was analysed using univariate and multivariate logistic regression to investigate factors associated with repeat positivity including organism load, patient demographics, sexual risk behaviour, treatment received, and concurrent infections with other STIs. Variables included in our multivariate models were selected on the basis of clinical relevance and the likelihood ratio test. Our secondary outcome was analysed using univariate multinomial regression to investigate factors associated with treatment failure and reinfection. No multivariate analysis was undertaken due to the small number of treatment failures and reinfections. We also conducted a sensitivity analysis to exclude cases that were tested within 28 days of receiving treatment because of the possibility of false-positive results [4]. Box plots were generated to compare distributions in organism load between those who did or did not have a repeat infection and by their OMP classification – the difference compared using Wilcoxon rank-sum tests. Azithromycin efficacy was calculated as the proportion of individuals testing SDA negative for rectal chlamydia when retested within 100 days after receiving treatment after excluding those classified as reinfections. Analysis was performed with Stata v. 13.0 (StataCorp., USA).
Ethics statement
Ethical approval for this study was granted by the Alfred Hospital Ethics Committee (373/13).
RESULTS
A total of 227 MSM were included in the study, of whom 64 (28·2%) presented with a repeat chlamydia-positive diagnosis within 100 days, giving a total of 291 chlamydia-positive samples available for further laboratory analysis. Of these 291 samples, genovar and organism load was able to be determined for 272 (93·4%).
Characteristics of men
The median age of participants at first diagnosis was 29 (range 18–78) years (Table 2). Concurrent infections with urethral chlamydia, rectal gonorrhoea and syphilis infection were reported in about 16%, 12% and 3%, respectively; 20% were HIV positive. Overall about 65% reported ⩾2 partners in the last 3 months and 25% reported always using a condom during the last 3 months. The median time between receiving treatment and the follow-up test was 55 days, and 50% of men were retested 36–71 days after receiving treatment.
Table 2. Patient characteristics in index cases

* Only J found in this study in C complex.
† See Table 1 for classification algorithm.
Genovar and genotyping (MLST)
For index cases, genovar was determined for 218 (96·0%) men; the most commonly detected genovar was G (34·9%), followed by D (29·4%), J (16·1%), E (10·6%), B (3·7%) and F (2·3%). A total of seven (3·2%) men were found to have asymptomatic LGV-associated genotypes on their index swab that were missed during their initial diagnosis. Of men presenting with a repeat infection, 46 (71·8%) presented with an identical genovar, two (3·2%) with a different genovar and 16 (25·0%) were not assessable. Different sequence types (using MLST) were seen in 9/46 (19·6%) patients, suggesting new infections. These results show that overall 11 cases (17·2%, 95% CI 8·9–28·7) were definite reinfections on the basis of genovar analysis.
Organism load
Median organism load was higher for repeat infection cases than for index cases (4·4 log10 copies/ml vs. 3·8 log10 copies/ml, P = 0·03) (Fig. 1).
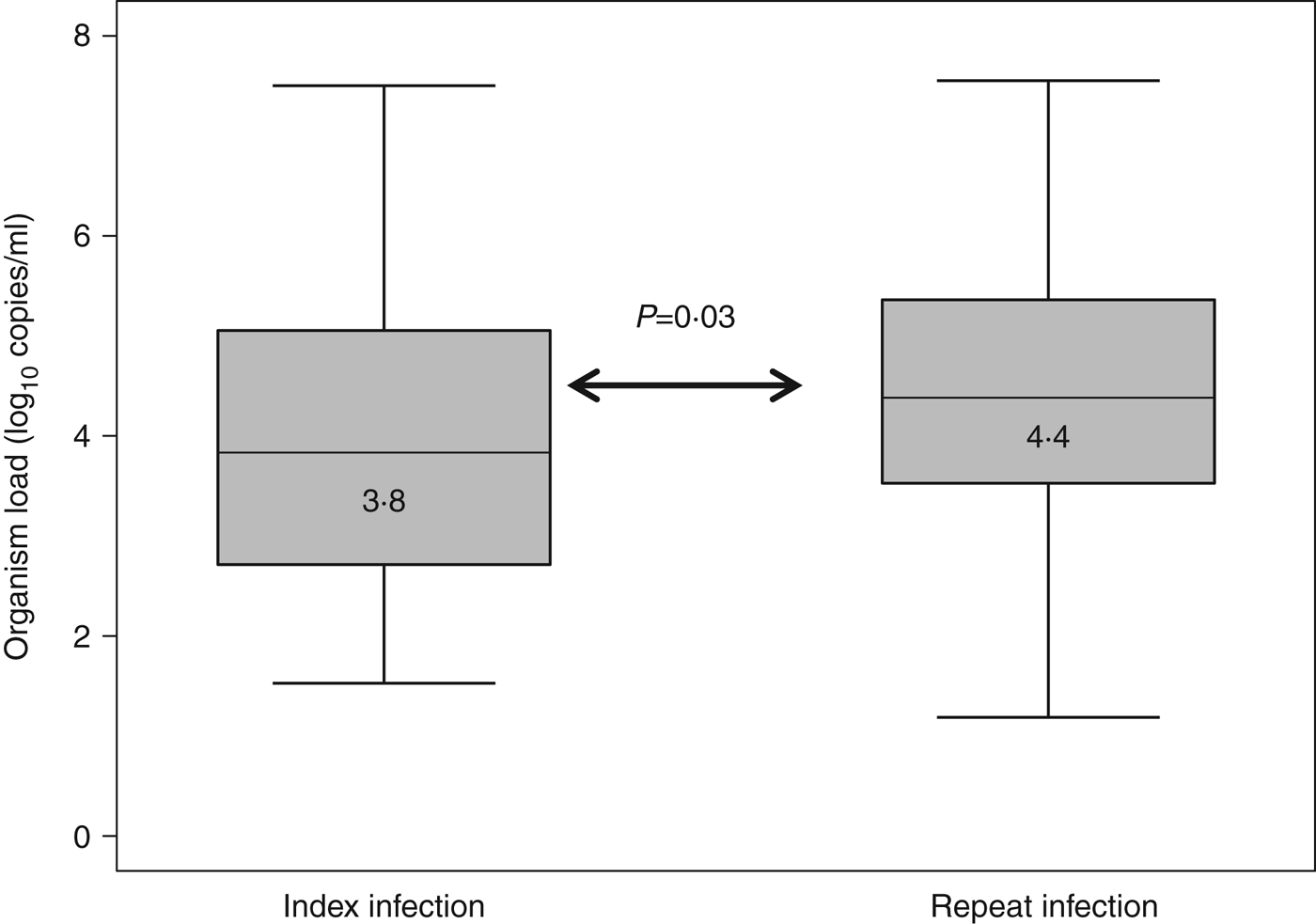
Fig. 1. Organism load/ml between index and repeat infections.
Median organism load in the index infection was significantly higher in men who had a subsequent treatment failure (n = 29, 5·2 log10 copies/ml, P < 0·01) or reinfection (n = 35, 4·7 log10 copies/ml, P < 0·01) compared to men whose infection was successfully treated (n = 163, 3·5 log10 copies/ml) (Fig. 2). There was no difference in organism load for the index case between men who had treatment failure or reinfection on retest (P = 0·35).
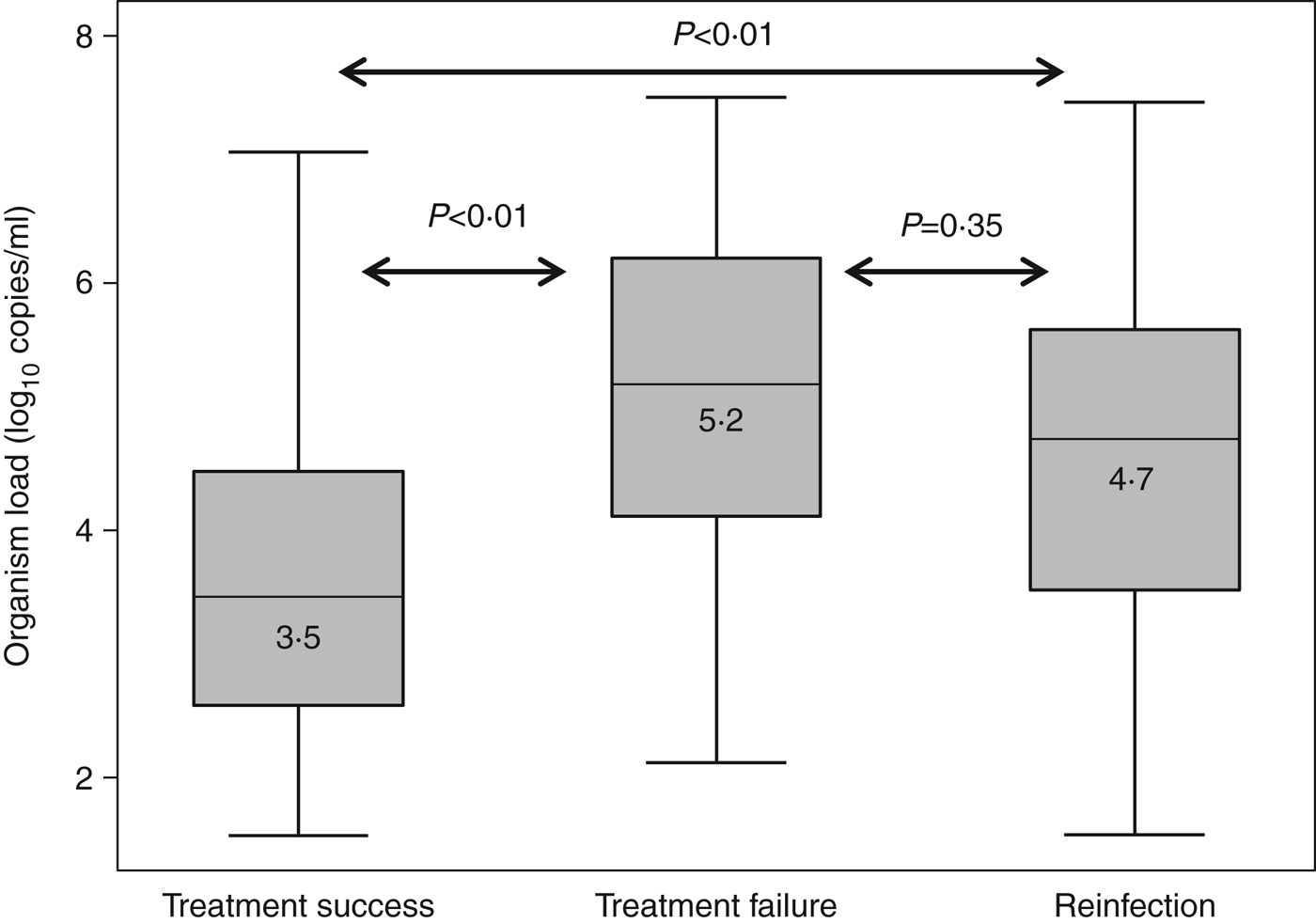
Fig. 2. Organism load/ml (in index cases) by outcome.
Median organism load was significantly higher for B complex than C complex genovars (4·1 vs. 3·4 log10 copies/ml, P < 0·01) but not between Intermediate and C complex genovars (3·9 vs. 3·4 log10 copies/ml, P = 0·10) or between Intermediate and B complex genovars (3·9 vs. 4·1 log10 copies/ml, P = 0·11) (Fig. 3).

Fig. 3. Organism load/ml (in index cases) by OMP classification.
Repeat positive diagnosis
A total of 64 (28·2%, 95% CI 22·4–34·5) men had a rectal chlamydia diagnosis with a repeat positive result. Univariate analysis found only increased organism load [odds ratio (OR) 1·8, 95% CI 1·4–2·3] was significantly associated with a repeat positive result (Table 3).
Table 3. Factors associated with a repeat positive rectal chlamydia diagnosis, treatment failure and reinfection*
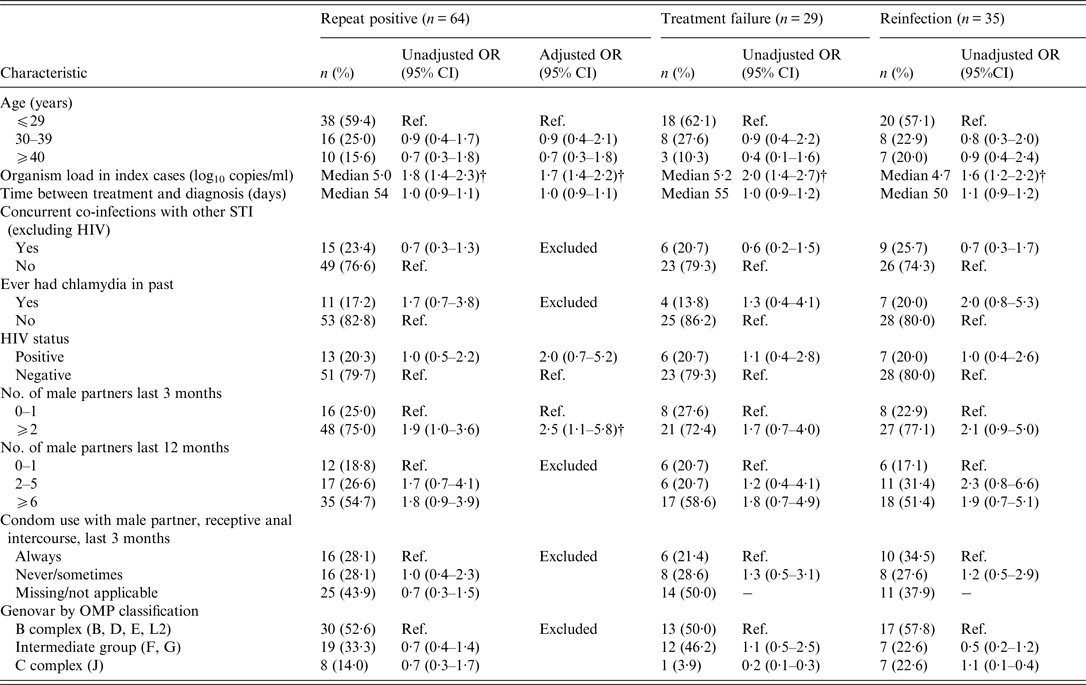
OR, Odds ratio; CI, confidence interval.
* Treatment success is the reference group (n = 163); Excluded = excluded from multivariate analysis.
† P < 0·05.
Multivariate analysis (including age, organism load, time to next test, HIV status and number of recent partners) found repeat positivity was associated with increased organism load (OR 1·7, 95% CI 1·4–2·2) and ⩾2 sexual partners in the last 3 months (OR 2·5, 95% CI 1·1–5·8). Of the seven men found to have LGV, one (14%) was diagnosed with a repeat rectal chlamydia infection. There was no difference in the proportion with repeat positive chlamydia by index serovar (P = 0·14) (Table 3).
Of the 64 men with repeat infection, an estimated 29 (12·8%, 95% CI 8·7–17·8) were classified as treatment failure and 35 (15·4%, 95% CI 11·0–20·8) as reinfection. Univariate analysis found that increased organism load was associated with treatment failure (OR 2·0, 95% CI 1·4–2·7) or reinfection (OR 1·6, 95% CI 1·2–2·2). No other variables were associated with either outcome.
Sensitivity analysis
A total of 30 men were retested within 28 days of receiving treatment of whom seven (23·3%) were repeat positives: four (13·3%) and three (10·0%) being treatment failures or reinfection. Excluding those who were tested within 28 days of receiving treatment we found that (a) the number of partners in the past 3 months was no longer associated with repeat positive infections in multivariate analysis, and (b) there was no effect on the association of organism load on treatment failure or reinfection in univariate analysis.
Treatment efficacy
Treatment records were available for 220 (96·9%) index cases with 203 (92·3%) being prescribed a single 1 g dose of azithromycin; other treatments were prescribed for the other 17 cases. Of those treated with 1 g azithromycin and excluding those classified as reinfection (n = 32), 143 were effectively cured at follow-up corresponding to a treatment efficacy for 1 g azithromycin of 83·6% (143/171, 95% CI 77·2–88·8). Of the seven missed cases of LGV, four were successfully treated with 1 g azithromycin, two successfully treated with combination of doxycycline and azithromycin, and only one case reported as a treatment failure with 1 g azithromycin.
DISCUSSION
We found that repeat rectal chlamydia was common in MSM with >28% being diagnosed with a repeat rectal chlamydia infection within 100 days of treatment. While new infections or reinfection accounted for a significant proportion of the repeat infections, we found that 12·8% were likely to represent probable treatment failure on the basis that they were the same genovar and had either not had sex or had only protected anal sex. We also found that high rectal chlamydia organism load is associated with repeat infection with a twofold increase in the odds of treatment failure.
We found an estimated treatment efficacy of 83·6% following treatment with a single 1 g dose of azithromycin which is similar to the 85% treatment efficacy estimate from a recent meta-analysis of rectal chlamydia treatments [Reference Kong5]. An efficacy of 83·6% is less than the 95% efficacy recommended by the World Health Organization [15] and raises the question of whether 1 g azithromycin is the optimal treatment for rectal chlamydia. Guidelines for the treatment of rectal chlamydia do vary with doxycycline being the recommended first-line treatment in the EU [Reference Lanjouw6] and Australia [7], but azithromycin is the first-line treatment in the USA [4]. However, there are no RCTs comparing 7-day doxycycline and 1 g azithromycin treatments for rectal chlamydia and this higher level evidence is urgently needed given the difficultly of interpreting observational studies. Additionally, no pharmacokinetic data are available on azithromycin in rectal tissue so it remains uncertain if rectal tissue concentrations are sufficient to effectively treat chlamydia. However, available data on azithromycin concentrations in gastric tissue (a proxy for rectal tissue) report high concentrations in gastric tissue, juice and mucus [Reference Harrison, Jones and Morris16, Reference Kirchhoff17] raising the possibility that factors other than tissue concentrations may impact treatment efficacy [Reference Hocking18].
To our knowledge, these are the first available data showing the association between higher organism load and repeat rectal chlamydia infections, but this has been observed in other infection sites including the eye [Reference West9], vagina [Reference Walker8] and throat [Reference van Rooijen19]. One possible explanation for this finding is potential heterotypic resistance occurring in rectal infections whereby a chlamydia infection may comprise both treatment-susceptible and less-susceptible organisms. If the organism load is sufficiently high, the less susceptible organisms can survive treatment thereby allowing the infection to persist once treatment is complete. Heterotypic resistance has been demonstrated in vitro at high levels of chlamydial organism load, but is not evident at lower levels of organism load [Reference Wang12]. This raises the question of whether other treatments are needed or if extended doses of azithromycin are needed to effectively treat rectal chlamydia infection with a high organism load [Reference Horner20].
Reinfection was also associated with higher organism load in the index infection. Similar results were reported by Geisler et al. [Reference Geisler21] who reported higher inclusion-forming units in men who reported a previous chlamydia infection and suggested that the sampling time relative to the time of acquiring infection may be a potential bias as samples taken later in an infective cycle are likely to have higher organism loads compared to sampling early after infection.
In our study genovars G, D and J were the most prevalent in MSM and the genovar distribution was similar to the general (non-anatomically specific) distribution in Australia [Reference Twin22], Sweden, The Netherlands and United States [Reference Christerson23]. The prevalence of LGV in our study was ~3% which is similar to the prevalence of 2·4% from an Australian community setting [Reference Templeton24], but greater than that reported in Dutch STI clinics (1·2%) [Reference de Vrieze25] and lower than that reported in UK HIV/GUM clinics (14·2%) [Reference Annan26]. Our finding of seven cases of asymptomatic LGV is consistent with current evidence that symptoms can be a poor predictor of rectal LGV [Reference Lister27] and data from European countries reporting that a considerable proportion of cases of LGV may be asymptomatic at diagnosis [Reference de Vrieze25, Reference Annan26, Reference Haar28]. Therefore in the absence of genotyping at diagnosis, cases of LGV will be missed unless routine genotyping of rectal chlamydia is performed. Last, eight cases of rectal samples were found to be genovar B, the genovar normally associated with trachoma. Genovar B at the rectal site has previously been reported [Reference Geisler, Morrison and Bachmann29] and may occur as absolute tissue tropism by genovar does not exist.
The strengths of our study are that we believe this is the only study that has quantified the association between chlamydia organism load in MSM with repeat rectal chlamydial infections. We also used genotyping/MLST to aid in the differentiation between treatment failure and reinfection.
There are several potential limitations to our study. First, it is possible that false-positive diagnoses may have occurred in men retested within 4 weeks after treatment. However, our sensitivity analysis found that excluding those retested within 28 days had no effect on the association between repeat positivity and organism load. Second, MLST was only able to differentiate between 20% of repeat infections with the same genovar; and it is possible that men with the same MLST profile on repeat testing could have been reinfected with the same organism rather than this representing a treatment failure. Our classification of men as either treatment failure or reinfection was based on self-reported sexual risk behaviour data which may have been inaccurate or under-reported. However, our classification of treatment failure was conservative and the sexual behaviour data from our sample was comparable to that in a nationally representative sample of MSM, which found a similar proportion reporting ⩾6 partners in the last 3 months (26% in each case) or reporting always using a condom in the last 3 months (29% vs. 24%) [Reference Holt30]. Until a novel immunological or molecular marker of true reinfection is available, analyses similar to ours will be subject to misclassification bias. Finally, degradation of the stored frozen samples over time [Reference van Dommelen31] may have effected organism load estimates as the stored rectal samples used would have been thawed and refrozen for other studies undertaken at the clinic. We also reported organism load without taking sampling variability into consideration (i.e. not per number of eukaryotic cells present). However, it has been reported that adjusting for eukaryotic cells is inappropriate because inflammatory cells produced during an acute infection are attracted to the site of infection [Reference Moorman, Sixbey and Wyrick32].
CONCLUSION
We believe this is the first study to show that higher chlamydial load is associated with repeat rectal chlamydia infection and adds to the growing evidence that chlamydial load is important to treatment outcomes at other sites. With higher organism loads increasing the risk of repeat chlamydia positivity, it remains unknown if 1 g azithromycin remains the most effective treatment for rectal infections.
ACKNOWLEDGEMENTS
This work was supported by an Australian National Health and Medical Research Council grant (no. 568971).
DECLARATION OF INTEREST
None.








