INTRODUCTION
Human papillomavirus (HPV) is one of the most common sexually transmitted infections in the world [1, 2]. Approximately 75%–80% of sexually active people become infected at some time in their lives. Condyloma acuminata is the classic clinical manifestation of HPV, which is caused by non-oncogenic or low-risk (LR) subtypes that lead to verrucous lesions [Reference Schiffman3]. Only a small portion of infections evolve into precursor cancer lesions and these are caused by oncogenic or high risk (HR) types, such as HPV 16 and HPV 18. Moreover, cervical cancer is considered to have a good prognosis if diagnosed and treated early. On the other hand, late diagnosis is the main reason for high mortality rates [Reference Schiffman3, Reference Ting4].
Cervical cancer is a public health burden, and Latin America is considered to have the fourth highest incidence in the world [Reference Schiffman3, Reference Murillo5]. Bolivia and Peru appear to exhibit the highest prevalence in Latin America, followed by Brazil [Reference Bosch6]. In Brazil, 16 340 new cases were expected for 2016, with an estimated risk ratio of 15·85 cases for every 100 000 women [7]. Cervical cancer is more incident in the Northern region, followed by the Northeast and Midwest regions. Southeastern and Southern regions correspond with the third and fourth highest incidences, respectively.
The Papanicolaou test was created based on spontaneous or induced exfoliation of normal or pathological cells from the cervix, and used worldwide for screening precursor lesions and cervical cancer [Reference Kulasingam8]. Furthermore, some authors have suggested complementary methods to detect cervical cancer, such as cervical inspection with 5% acetic acid [Reference Sankaranarayanan9–Reference Misra11]. This technique has been demonstrated useful in low-resource settings, with sensitivity rates ranging from 79% to 82%, and specificity rates ranging from 91% to 92% [Reference Sauvaget10, Reference Kalgong12, Reference Mustafa13], and has proven to be safe and cost-effective. Moreover, cervical inspection with 5% acetic acid helps to reduce false negative results and can be applied when resources are in short supply in health care units [Reference Sankaranarayanan9–Reference Misra11].
Taking into account the high prevalence of HPV in Brazil and its importance to public health, we investigated the prevalence and risk factors for HPV infection in the Southern region of Bahia. In addition, this study represents an opportunity to discuss complementary diagnosis through cervical inspection, since there are few studies with this approach.
METHODS
Study population
A cross-sectional study was carried out during April 2011–2012 with women attended at healthcare units in Southern Bahia, in the following cities: Itabuna, Ilhéus, Arataca, Barro Preto, Buerarema and Coaraci. Participants were invited as volunteers and cervical cell samples were collected. Women exhibiting one or more of the following criteria were excluded from the study: (1) history of hysterectomy, (2) vaginal medication use within 15 days prior to collection, (3) treatment of condyloma or intraepithelial lesions, and (4) sexual activity in last 2 days. All participants were submitted to a structured questionnaire to elicit data on demographics and practices considered risk factors for HPV infection. These data were converted to variables and tested for correlations with positive or negative results related to HPV infection.
Diagnostic criteria for visual inspection
The presence of acetowhite lesions in the transformation zone near the squamocolumnar junction (JEC), 1 min after application of 5% acetic acid, was considered as a positive result.
Cervical cytology
Smears were performed and stained by Pap test and classified according to the Bethesda System. Samples showing atypical squamous cells of undetermined significance (ASCUS), typical squamous cells, cannot rule out high-grade squamous intra-epithelial lesions (ASC-H), squamous intraepithelial lesions (SIL) and high grade squamous intraepithelial lesions (HSIL) were considered positive. The samples showing a normal pattern and inflammatory and/or reactive changes were considered negative. All cytological analysis was performed by a certified and trained Pathologist.
Molecular diagnosis
Cervical cells were stored in saline solution (at −20 °C) for later DNA extraction with QIAamp DNA Mini Kit (Qiagen Ltd, Crawley, UK). Viral DNA was detected by nested-polymerase chain reaction (PCR) (primers MY09/MY11 followed by primers GP5+/6+), using adapted protocols previously described [Reference Levi14, Reference de Roda Husman15].
Briefly, in the first round reaction, the following reagents were used: 14·65μl of Milli-Q water; 2·5μL of 10× buffer (500 mM KCl and 100 mM Tris-HCl (pH 8·5)); 0·75 µl MgCl2 50 mM; 4 µl from the ‘pool’ of dNTP (1·25 mM); 0·3 µl of MY09 primer (10 pmol/μl); 0·3 µl of MY11 primer (10 pmol/μl); 0·5 µl Taq polymerase (Invitrogen®) (1 U/μl) and 2·0 µl of the solution containing the DNA sample (final volume of 25 µl). The cycling conditions were: 1 cycle of 1′ at 94 °C followed by 40 cycles of 1′ at 95 °C, 1′ at 55 °C and 1′ at 72 °C, followed by 10′ at 72 °C for final extension. In the second round reaction, the following reagents were used: 28·6 µl of Milli-Q water; 5 µl of 10× buffer (500 mM KCl and 100 mM Tris-HCl (pH 8·5)); 1·5 µl MgCl2 50 mM; 8 µl from the ‘pool’ of dNTP (1·25 mM); 0·70 µl of GP5+ primer (22·5 pmol/μl); 0·7 µl of GP6+ primer (18·9 pmol/μl); 0·5 µl Taq polymerase (Invitrogen®) (1 U/μl) and 5·0 µl of the solution containing the first round (final volume of 50 µl). The cycling conditions were: 1 cycle of 4′ at 94 °C followed by 40 cycles of 30″ at 94 °C, 30″ at 55 °C and 30″ at 72 °C, followed by 8′ at 72 °C for final extension. In addition, all PCR positive samples were analyzed for the presence of the following HPV types: 6 and 11 (the most prevalent low risk), and 16, 18, 31, 33, 52 and 58 (the most prevalent HR) as previously described [Reference Yamaguchi16].
Statistical analysis
A bivariate analysis was carried out using Chi-square and Fisher's exact tests with significance level of 5% (P ⩽ 0·05), to determine the association between abnormalities on clinical examination, cytology and HPV infection by nested-PCR, using EPI-INFO software version 7·2·1·0 (www.cdc.gov/epiinfo), and BioEstat version 5·0. Multivariate logistic regression analyses were performed in order to correlate independent variables with the nested-PCR. Sensitivity, specificity, positive and negative predictive values were calculated for visual inspection testing and cytological examination. The results of the nested-PCR were used as a parameter in order to assess the accuracy of the visual inspection test and the cytological examination.
Ethical considerations
This study was approved by the Research Ethics Committee of Universidade Estadual de Santa Cruz under registration number 377/14. Informed consent was obtained from all participants. In case of minors, consent was signed by parents or guardians.
RESULTS
A total of 195 healthy women were enrolled in this study. Demographic characteristics of the participants are presented in Table 1. The median age was 40·3 years (ranging from 17 to 82 years), with most participants over 30-years-old corresponding to 67·2%. The majority (89·2%) made self-reported mixed skin color. Most individuals (72·7%) live with an income of less than one minimum Brazilian wage (approximately US$220), and have an elementary school education or below (45·6%). The rate of illiteracy among the participants was 8·2%. Behavioral features such as alcohol consumption, smoking habits, and hormonal contraceptive use were reported by few women, whereas most have stable partners and multiparity history (Table 1). No statistical differences were observed when variables listed above were analyzed with positive and negative results for HPV infection.
Table 1. Demographic characteristics and risk factors in women testing positive or negative by PCR for HPV infection in Southern Bahia, Brazil, 2011–2012
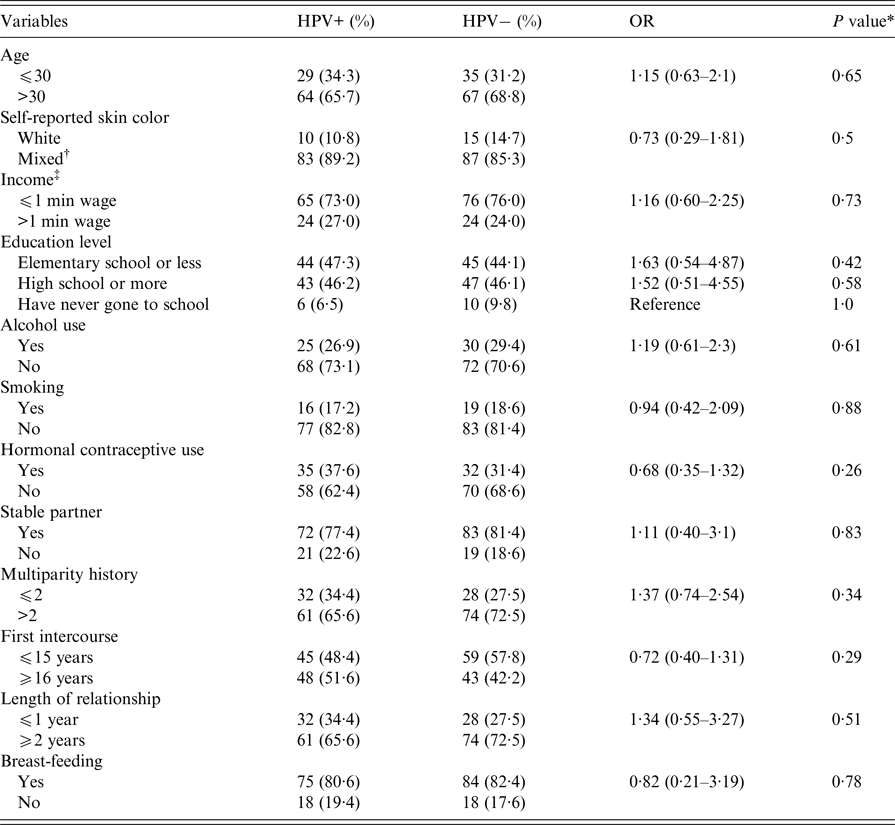
* Assessed using Pearson's χ 2 test.
† This category includes blacks, mulattos and Indians.
‡ Income value for one minimum Brazilian wage is approximately US$220.
The prevalence of HPV infection by PCR was 47·7% (95% CI 40·8–54·7). HPV 16 was the most frequent type found, with a prevalence rate of 29% (95% CI 20·7–38·9). In addition, seven patients were infected with at least two types of HPV; in all such cases, HPV 16 was present. Furthermore, some HPV 16 cases presented normal cytology and had no clinical abnormalities.
Cytological analysis revealed the presence of inflammation in 51·8%, LSIL in 17·4%, HSIL in 10·8%, ASCUS in 6·2% and ASC-H in 1·0% of participants. In addition, 18% of women with a HSIL cytology diagnosis had negative PCR results. The clinical symptoms reported were dyspareunia and bleeding (15·4% and 6·2%, respectively). A positive correlation of these symptoms was verified for positive PCR (P = 0·003; OR 2·55, CI 95% 1·35–4·8), for cervical cytology (P < 0·001, OR 3·32, 95% CI 1·75–6·31) and for positive visual inspection test (P < 0·001, OR 5·6, 95% CI 2·81–11·14) (Table 2). Hormonal contraceptive use was associated with positive visual inspection test results (Table 3).
Table 2. Prevalence of clinical symptoms and correlations with primary clinical symptoms, pap smear, visual inspection test and PCR, in women from Southern Bahia, Brazil, 2011–2012
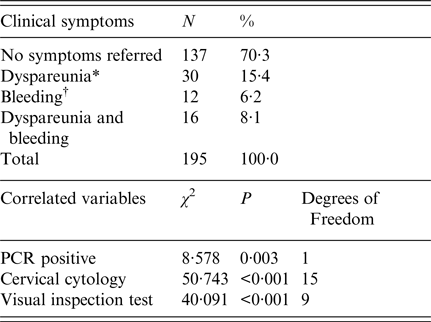
* Pain during sexual intercourse.
† Bleeding related to coitus.
Table 3. Demographic characteristics and risk factors related to the presence of acetowhite lesions in the transformation zone, in women from Southern Bahia, Brazil, 2011–2012
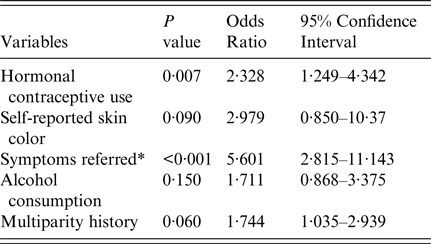
* Bleeding during sexual intercouse and dyspareunia.
Sensitivity and specificity rates were 70% and 85%, respectively for visual inspection and 83% and 40%, respectively for cytology, when compared with PCR results. There was a correlation between positive PCR and positive visual inspection (χ 2 = 35·37; P < 0·001), cervical cytology (χ 2 = 8·58; P = 0·005), and symptoms reported (χ 2 = 12·05; P = 0·01) (Table 2).
The cervical lesion screening technique performance is shown in Table 4. Positive and negative probability ratios were performed for the visual inspection test. The indexes were 4·7 and 0·38, respectively, while the technique's accuracy was 83%. The positive and negative verisimilitude ratio computations for the cervical cytological exam were 1·38 and 0·425, respectively, and this technique's accuracy was 65%.
Table 4. Performance of conventional diagnostic techniques for screening HPV infections compared with the PCR test in women from Southern Bahia, Brazil, 2011–2012
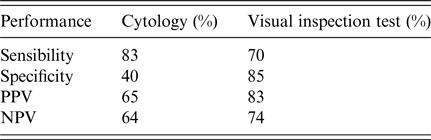
PPV, Positive Predictive Value; NPV, Negative Predictive Value.
DISCUSSION
HPV infection and cervical cancer are highly prevalent among women worldwide. The HR HPV types (16 and 18, respectively) are the main genotypes implicated in cervical cancer and pre-cancerous lesions, accounting for approximately 70% of cervical cancers and approximately 50% of high-grade lesions [17]. The rates in the Latin American population are higher compared with results of the rest of the world [1]. In a recent study, Capote Negrin reported that Bolivia exhibits a higher incidence of cervical cancer (50·73%), compared with Puerto Rico which accounts for the lowest incidence (9·73%). On the other hand, Brazil appears with an incidence rate of 24·03% [Reference Capote Negrin18].
Notwithstanding in Brazil, the risk ratio for cervical cancer was 15·85 per 100 000 women in 2016, in which Bahia is the third highest state in number of cases (1·180 new cases per 100 000 women). São Paulo and Rio de Janeiro have the highest number of cases (4·360 and 1·490 new cases, respectively) [7].
Several studies have been conducted around Brazil. The prevalence rates range from 10·5% to 48·6% [Reference de Medeiros Fernandes19–Reference Martins27]. In this study, we detected a high prevalence of HPV infection in Southern Bahia (47·7%, 95% CI 40·8–54·7), which is similar to the prevalence reported in Rio de Janeiro [Reference Martins27], and higher when compared with other regions including Salvador, the Capital of Bahia State [Reference Bruno23, Reference Oliveira28].
HPV 16 is described as responsible for the majority of HPV-associated cancers [Reference Schiffman3, Reference Ting4, Reference Bosch6, 17]. Our results demonstrated that HPV 16 was the most frequent type found in women from South Bahia (29%, 95% CI 20·7–38·9), similar with findings reported by Oliveira-Silva in Rio de Janeiro (28%).
HPV infection is the most important risk factor for cervical cancer development. However, HPV infection itself does not represent a sufficient cause, and several other factors increase the chances of developing cervical cancer, such as young age, co-infections, long-term oral contraceptive use, smoking, immunosuppression, multiparity, and sexual activity markers (high number of sexual partners, young age at sexual debut, and recent new sexual partner) [Reference Schiffman3, Reference Mzarico29–Reference Del Río-Ospina31]. Although it was not found to be a positive correlation with HPV infection and most of the related risk factors listed above (Table 1), the use of hormonal contraceptives was highly associated with the presence of acetowhite lesions (Table 3). Indeed, steroid hormone use (estrogen and progesterone) increase the chances for rapid progression of high-grade squamous intraepithelial lesions, as has already been shown for cervical cancer in other studies [Reference Schiffman3, Reference Chung, Franceschi and Lambert30].
Bleeding after intercourse and dyspareunia were the most reported symptoms, showing a strong correlation with HPV infection (Table 2). Positive PCR was 2·5 times more common with those women suffering from dyspareunia and bleeding (OR 2·55, 95% CI 2·48–2·84, P = 0·003). The existence of bleeding is closely related to the presence of high-grade intraepithelial lesions, which can be explained by the high degree of cellular modifications. Hence, in the poorest regions, the visual inspection test can be useful for early detection of premalignant and malignant cervical disease, helping decrease postcoital bleeding, and prompting additional evaluation and treatment [Reference Tarney and Han32, Reference Khan, Appleton and Turner33].
The incidence rates of cervical cancer have declined over the past three decades in most developing countries, due mainly to prevention programs implemented. Methods that allow early screening are extremely important for defining treatment and containing the infection [Reference Schiffman3–7]. The high prevalence found in this study could be associated with the combination of different methodologies employed, the sampling number and the sample source (public health units).
Visual inspection tests have been applied as a useful alternative method to cytology, improving cervical lesion screenings, without additional costs [Reference Sankaranarayanan9–Reference Misra11, Reference Aggarwal34]. In our survey, visual inspection showed a better performance when compared with cervical cytology, as analyzed by positive and negative probability ratios and the technique's accuracy (Table 4). Cervical cytology was more sensitive and most patients with positive cytology had high grade lesions. However, the visual inspection test proved to be twice as specific and obtained a positive predictive value greater than cytology. These data demonstrate that the visual inspection test is, in fact, more likely to point towards HPV infection. As already demonstrated in the literature, sensitivity and specificity rates for detecting HSIL lesions are similar between the colposcopy and the visual inspection test, demonstrating that this alternative method can be useful for low-income populations in poorer regions [Reference Roland35, Reference Torre36]. Furthermore, the verisimilitude ratio showed that visual inspection was almost five times more accurate than cytology, decreasing the chances of false-negative results. Additionally, we showed that PCR for detection of HPV infection was strongly related to the positive visual inspection test (OR 7·3, 95% CI 3·64–14·66, P < 0·001), and associated with cervical cytology (ASCUS, ASC-H, LSIL and HSIL; χ 2 = 12·053 and P = 0·0001).
CONCLUSION
In conclusion, we found a high prevalence of HPV infection in low-income women in Southern Bahia, with HPV 16 as the most common type. A positive correlation between HPV infection and the use of hormonal contraceptives was found. Moreover, our results corroborate the visual inspection test as a useful tool for cervical cancer screening in areas with limited financial resources. Finally, as HPV constitutes a substantial public health burden, combined alternative conventional methods could provide rapid results, enhancing early cervical cancer prevention, with rapid diagnosis and treatment.
ACKNOWLEDGEMENTS
We thank undergraduate research students Juliete Costa and João Henrique Fonseca, and also the nurses from the healthcare units for their excellent technical support. We also thank all the volunteers for taking part in this study. This research was supported by Universidade Estadual de Santa Cruz (UESC). There are no competing interests.







