INTRODUCTION
Gastrointestinal infections are a major public health problem worldwide. Although most infections are self-limiting, they sometimes progress into a more serious course with the development of complications. In developed countries, mortality is low due to the high standard of living and the availability of healthcare. Children are mostly affected, although adults, especially the elderly, can also become seriously ill. In the Dutch general population, the incidence of gastroenteritis was estimated at 283/1000 person-years (py) [Reference de Wit1]. The highest incidence (900/1000 py) was reported in children aged 1–4 years. In adults, the incidence was 234/1000 py (18–64 years) and 194/1000 py (⩾65 years). In around 5% of episodes, a general practitioner (GP) was consulted [Reference de Wit2]. Although hospitalization rates due to gastroenteritis are considered to be much lower, two-thirds of the direct medical costs for gastroenteritis are attributed to hospital admissions [Reference van den Brandhof3]. The infectious causes of gastroenteritis include a wide array of bacteria, viruses, and parasites, with different capacities of causing severe illness. In a Dutch community-based study, norovirus and rotavirus were detected most often in adults, whereas in adult cases consulting their GP, Campylobacter, norovirus and Giardia lamblia were seen most frequently [Reference de Wit1, Reference de Wit4]. Systematic studies of the aetiology of gastroenteritis in patients requiring hospitalization are rare, particularly in adults, and typically they do not include a broad panel of pathogens in the microbiological analyses of stool samples. In a recent German study in adults hospitalized with gastroenteritis, Campylobacter was detected most frequently, followed by norovirus, Salmonella, and rotavirus [Reference Jansen5]. In a similar Swedish study, bacteria appeared to be the most important pathogens with the highest ranking for Clostridium (Cl.) difficile, Campylobacter and Salmonella [Reference Svenungsson6].
The objective of this study was to determine the incidence and aetiology of gastroenteritis in adults requiring hospital admission.
METHODS
Design
During about 1 year in the period between June 2008 and November 2009, adults admitted to hospital with gastroenteritis at the Gastroenterology and Hepatology, or Internal Medicine wards of five hospitals were enrolled in the study (Table 1). Four hospitals were general hospitals dispersed over The Netherlands and one hospital was a university hospital (hospital C). Gastroenteritis was defined as (1) diarrhoea (⩾3 episodes in 24 h), and/or vomiting (⩾3 episodes in 24 h), or (2) diarrhoea (<3 episodes) or vomiting (<3 episodes) and two or more other symptoms (vomiting/diarrhoea, stomach ache, abdominal cramps, nausea, fever, blood in stool, mucus in stool). An episode had to be preceded by a symptom-free period of 2 weeks. This case-definition was similar to those used in previous community- and GP-based studies to allow comparison of results [Reference de Wit1, Reference de Wit7].
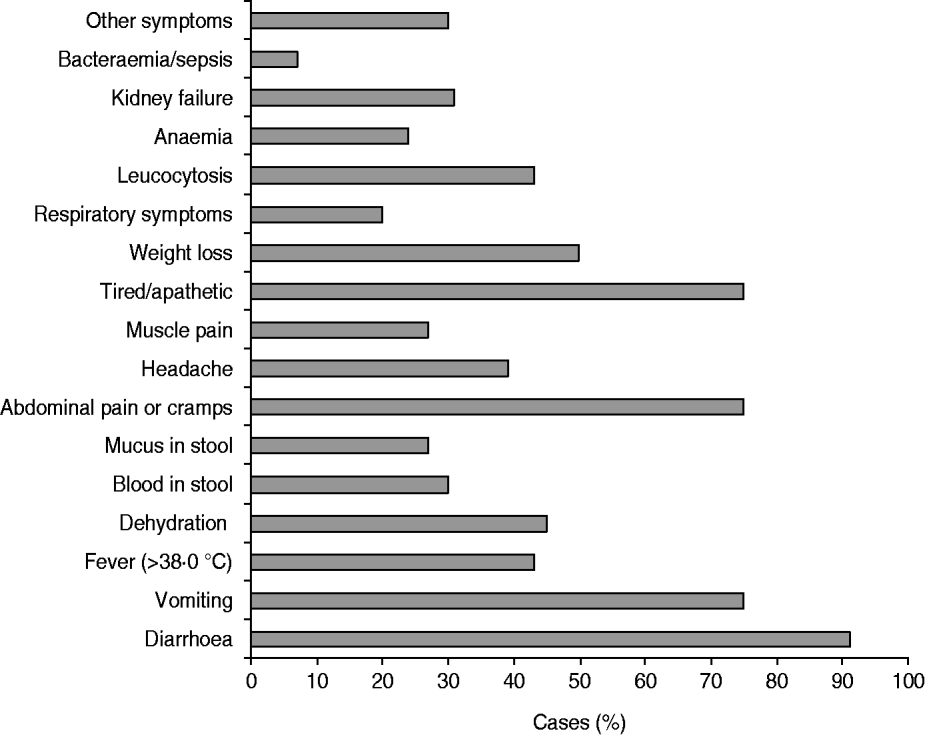
Fig. 1. Percentages of cases with gastroenteritis requiring hospitalization (n=44) per symptom.
Table 1. Enrolment period and number of included cases and controls per hospital
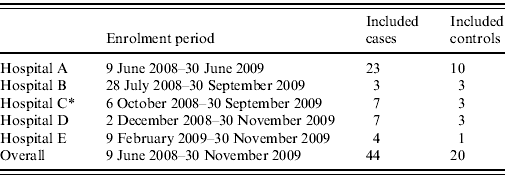
* University hospital.
The study protocol was reviewed and approved by the medical ethics review committee of the University Medical Centre Utrecht, and the local medical ethics committees of all five hospitals.
Data collection
Medical staff approached the patients hospitalized because of gastroenteritis. Inclusion consisted of obtaining written informed consent to provide epidemiological and clinical information, and supplying a faecal sample. Participants completed a questionnaire shortly after discharge from the hospital and again 3 months later. For participants with possible complications at 3 months follow-up, a second follow-up questionnaire was sent 6 months after discharge. As only four cases completed the second follow-up questionnaire, those results are not further presented in the paper. The first questionnaire included questions about demography, underlying diseases, medication use, possible risk factors, and symptoms during the episode of gastroenteritis. Follow-up questionnaires addressed questions about the development of complaints and diseases after discharge. The physician or a nurse completed a questionnaire addressing symptoms, medication use in the 3 months before admission, and treatment before and during hospitalization.
Finally, a faecal sample was collected and divided into two containers, one container with sodium acetate, acetic acid and formalin (SAF) to fix the faecal samples for microscopy for parasites, and the other container without additives. The faecal samples were checked for Campylobacter jejuni, Cl. difficile, Escherichia coli [shigatoxin producing E. coli (STEC), enteroaggregative E. coli (EAEC), typical and atypical enteropathogenic E. coli (EPEC), and enteroinvasive E. coli (EIEC)/Shigella], Salmonella enterica, Yersinia enterocolitica, adenovirus, astrovirus, norovirus, rotavirus, sapovirus, Cryptosporidium, Dientamoeba fragilis, Entamoeba histolytica, G. lamblia and helminth eggs. Faecal samples were also tested for Blastocystis hominis, which was not considered a cause of gastroenteritis and thus not included in the calculated proportion of cases with a pathogen. Tests were performed as described previously [Reference Friesema8].
Controls
For each case, a control admitted during the same period (±1 month) and within the same age range (±10 years) not hospitalized for gastroenteritis, was recruited. Similar participant questionnaires were used for comparison of follow-up health status and risk-factor analyses. As only 20 case-control pairs were available for analyses, no risk factors were found and therefore these results are not further presented in the paper.
Analyses
The adherence population of the participating hospitals was estimated by calculating the portion of hospital admissions for gastroenteritis to the participating hospitals in relation to hospital admissions of adults in all Dutch hospitals as registered in the National Hospital Discharge database, and multiplying this fraction with the total number of Dutch inhabitants. This estimation was used as denominator in the incidence estimate. The data from the university hospital was not used in the incidence estimation, as the adherence population is difficult to assess due to another, broader, working area than the general hospitals.
During the inclusion period, it became clear that not all eligible patients were included in the study. The (too low) number of included cases in the numerator causes an unavoidable underestimate of the true incidence for hospitalized cases. The electronic patient management system (Diagnosis Treatment Combination, DBC) proved to be unsuitable to provide a proxy of the total number of cases hospitalized for gastroenteritis. All statistical analyses were performed using SAS v. 9.2 for Windows (SAS Institute Inc., USA).
RESULTS
Inclusions
In total, 45 adults hospitalized because of gastroenteritis were included in the study. For one case, the gastrointestinal complaints were most likely nosocomial, leaving 44 cases for analysis. The median age of cases was 59·5 years (range 21–92 years), and 77% were female. Based upon the 37 cases included in the four general hospitals (Table 1), the incidence of hospitalization for gastroenteritis is 0·41/10 000 persons. Incidence was lower in the 18–64 years age group (0·29/10 000) than in the elderly (0·95/10 000). Hospital A included the most cases. Incidence in the overall adherence population for both specific age groups was 0·94, 0·56, and 2·60/10 000 persons, respectively.
Pathogens
Faecal samples of 41 cases were tested for the complete panel of pathogens, for three cases no faecal samples were available. None of the pathogens tested were found in 17 (41%) cases, 15 (37%) cases had a single infection, six (15%) cases had a double infection, and in three (7%) cases three pathogens were found (Table 2). Bacterial infections were detected in 14 (34%) samples, viruses in 13 (32%) samples, and parasitic pathogens in four (10%) samples. Rotavirus was most commonly identified (22%). The median age of the cases with rotavirus was 63 years (range 21–87 years). Cl. difficile and norovirus were detected in 20% and 13%, respectively, of the single infections and were involved in 11% and 22% of the cases with co-infections. All four cases with Cl. difficile had taken antibiotics and/or proton pump inhibitors, and were aged 44, 52, 54 and 67 years. Five cases had Crohn's disease or ulcerative colitis: in two of these cases a pathogen was detected (one with Cl. difficile 001, and one with rotavirus G1[P8]). C. jejuni was observed mainly in cases with mixed infections (3/4).
Table 2. PathogensFootnote * isolated from adults hospitalized with gastroenteritis, separate for single and co-infections, and complaints during follow-up period
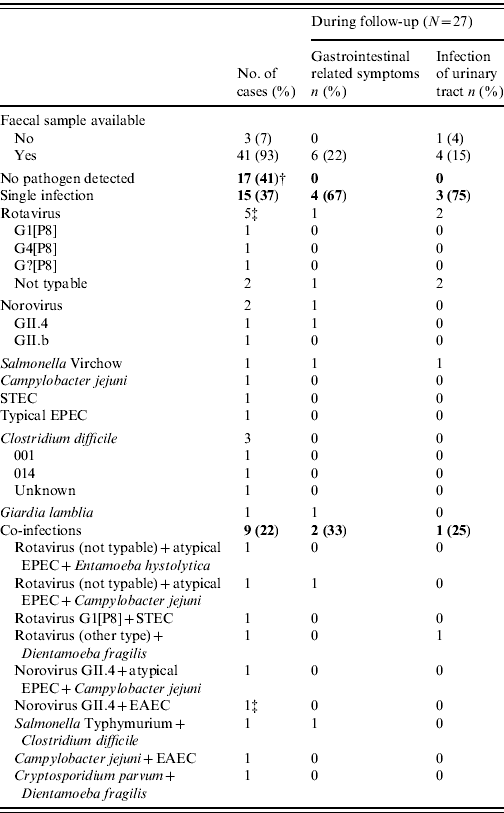
* None of the tested samples contained EIEC/Shigella, Yersinia, adenovirus, astrovirus, or sapovirus.
† Six samples contained the enteroaggregative heat-stable toxin gene (AstA); two samples contained Blastocystis hominis; one sample contained AstA and B. hominis.
‡ Three samples also contained B. hominis (two rotavirus, one norovirus and EAEC).
Episode of gastroenteritis
Five adults reported having had contact with someone with gastroenteritis symptoms before becoming ill. Almost all cases took medication (91%) and/or had underlying diseases (82%), of which diabetes was the most frequently reported. The cases had a median of 2 days of symptoms before admission to the hospital and were subsequently hospitalized for a median duration of 6 days. Of the 11 cases without a pathogen identified, but known date of onset of illness, seven (64%) were hospitalized more than 7 days after disease onset. For the cases with one or more pathogens identified, this proportion was 17% (3/18). Total duration of illness was known for only 36% of cases (median 12·5 days). One additional case still had complaints at the end of the 6-month follow-up period.
Most cases (86%) were rehydrated intravenously and 32% received antibiotics. In five (36%) of the cases receiving antibiotics a bacterial pathogen was detected. In the remaining cases, no pathogen (n=7) or rotavirus (n=2) was detected.
Almost all cases had diarrhoea, whereas about three-quarters reported vomiting. Furthermore, kidney failure with onset during the episode of gastroenteritis was reported in 31% of cases. One case was newly diagnosed with ulcerative colitis when admitted to the hospital with gastrointestinal symptoms; no pathogens were detected. Three cases developed bacteraemia; one of which also developed sepsis and ruptured duodenum. Initially, she was hospitalized for 16 days and after 6 days at home rehospitalized, where she died 4 months later at the age of 54 years. Her faecal sample contained Cl. difficile (further typing failed). She was already dependent on dialysis due to kidney failure before hospitalization for gastroenteritis. Results of blood cultures were not available. However, several bacteria were found in abdominal drain fluid, namely Pseudomonas aeruginosa, Enterococcus faecium and Enterococcus faecalis, E. coli and Klebsiella pneumoniae. The faecal sample of the second case with bacteraemia contained STEC and rotavirus, and the third case's sample was negative. Results of blood cultures were not available for these two cases. Another woman died at the age of 84 years, 1 month after being hospitalized for 19 days because of gastroenteritis. The cause of death was unknown and only B. hominis was found in her faecal sample.
Twenty-seven (61%) cases responded to the first follow-up questionnaire. Four (15%) cases had been re-admitted to hospital during this follow-up period, one of them twice. Twelve (44%) cases reported one or more complaints since discharge: half of these cases reported symptoms related to the gastrointestinal tract (Table 2), followed by infection of the urinary tract (five cases). Two cases had joint complaints (one without pathogens detected during the gastroenteritis episode, one with rotavirus, atypical EPEC and E. histolytica) and one case (without pathogen being detected) developed lung embolism 2 days after discharge and was rehospitalized. One case, for whom no pathogens were detected for the gastroenteritis, was diagnosed with Staphylococcus aureus 6 days after discharge and was rehospitalized.
Of the hospital controls, 15 (75%) persons returned the first follow-up questionnaire. For four (27%) controls illness during the follow-up was reported which was related to their underlying diseases.
DISCUSSION
In the present study, aetiology of gastroenteritis requiring hospitalization was examined. One or more potential pathogens were detected in 59% of the patients. This is comparable with the 56% found by Svenungsson et al. [Reference Svenungsson6], but lower than the 82% found by Jansen et al. [Reference Jansen5]. Both studies included B. hominis in their percentages, which would increase the figure of the present study to 66%. Both studies used a broader diagnostic panel than in the present study. In the German study, Campylobacter spp. and Yersinia spp. were tested, compared to C. jejuni and Y. enterocolitica in the present study. They also found incidentally two additional pathogens: enterovirus and mycobacteria [Reference Jansen5]. In the Swedish study, just one additional pathogen, ETEC was found relatively often at 5% [Reference Svenungsson6].
The line between infectious and non-infectious gastroenteritis is often unclear. Therefore, no exclusion criteria for certain medical conditions were made beforehand as it was also of interest to study pathogens in patients with chronic intestinal diseases. In 40% of the five cases with Crohn's disease or ulcerative colitis pathogens were detected, demonstrating that individuals with such a condition can also have infectious gastroenteritis. The three remaining cases with inflammatory bowel disease that tested negative might have had a (non-infectious) flare-up of their inflammatory bowel disease. Furthermore, cytomegalovirus colitis should be considered in patients with a history of inflammatory bowel disease who are admitted with symptoms of gastroenteritis and do not respond to increases in immunosuppressive treatment.
The detection of rotavirus and norovirus in the present study and other recent studies [Reference Jansen5, Reference Podkolzin9] suggests that the role of these viruses as a pathogen in adults has long been underappreciated. Due to for example travel, new rotavirus serotypes can be introduced into susceptible adult populations and outbreaks of rotavirus have been reported in the elderly [Reference Svraka10]. The majority of norovirus infections are found to be mild and self-limiting, but since so many infections occur each year, only a small fraction developing into severe illness will contribute significantly to the number of hospitalizations. Cl. difficile and C. jejuni were detected as often as norovirus in the present study. Both were also the most common bacterial pathogens in the Swedish study, with similar percentages [Reference Svenungsson6]. In the German study, Campylobacter was the most important pathogen (35%, also including serology), followed by norovirus (23%), while Cl. difficile was only found rarely [Reference Jansen5]. Parasites were detected scarcely, in accord with other studies [Reference Jansen5, Reference Svenungsson6].
About two-thirds of the 11 cases for whom no pathogens were found had suffered from symptoms for more than 1 week before being hospitalized. This indicates that pathogens can be difficult to detect in faecal samples taken more than 1 week after illness onset [Reference Svenungsson6, Reference de Wit7]. On the other hand, a non-infectious cause for the illness can not be ruled out.
Parallel to the present study, an identical study addressing children hospitalized with gastroenteritis in the same hospitals was conducted [Reference Friesema8]. In children, dehydration was an important reason for hospitalization, whereas serious symptoms during follow-up were rare as were underlying conditions and medication use before admission. In adults, almost all had underlying diseases or used medication, and development of severe disease was seen more often, including one death. Furthermore, at least four cases had serious or long-term sequelae after their infection. Moreover, kidney failure developed unexpectedly in a fairly large number of the cases, which needs to be confirmed in larger studies. These symptoms and long-term sequelae were not found to be related to specific pathogens.
As a substantial number of the eligible adults were not included in the study, selection bias can not be ruled out. Nevertheless, included patients were admitted throughout the year and patients were asked to participate within 24 h after admission when the course of the disease and the causative pathogen were still mostly unknown. It is, therefore, unlikely that the relative contribution of the different pathogens was distorted. However, the aetiology of gastroenteritis is based upon a rather small group, which will lower the chance of detecting rare pathogens and complications.
As no suitable proxy for gastroenteritis admissions was available, the overall calculated incidence as well as the incidence based upon hospital A will clearly represent an underestimation and should be considered as a minimum estimate. Using the data from this study and data from the community-based study [Reference de Wit1] it is estimated that at least 1/4000–8000 and 1/750–2000 of the adult community cases with gastroenteritis aged 18–64 years and ⩾65 years, respectively, will be hospitalized. The relatively low number of included cases hampers solid estimates of age-specific incidence. Comparison of age and sex distributions of hospitalized patient with those in other hospital-based studies is also difficult, as for most countries no valid information is available on the age and sex distribution of the community cases where the hospitalized cases originate from. Further, differences in national admission guidelines can induce difference in hospitalized populations. Nevertheless, assuming a similar distribution in community cases and hospital practice, for unknown reasons, the hospitalized cases in the Netherlands appear relatively old (mean 60 years vs. 41 and 48 years in Swedish [Reference Svenungsson6] and German studies [Reference Jansen5]) and more often are female (77%, vs. 55% in the other two studies mentioned).
In conclusion, a pathogen was detected in 59% of adults hospitalized with gastroenteritis, with rotavirus most commonly found. Adults hospitalized with gastroenteritis usually already have diseases or use medication and show clear signs of serious disease. Next to control of severe gastroenteritis by measures targeting high-risk food or specific pathogens, the focus could be on highly susceptible subgroups within the population.
ACKNOWLEDGEMENTS
The authors thank the staff of the hospitals for the participation of the patients in the present study. We thank Hein Sprong, Max Heck and Ed Kuijper for the subtyping of Cryptosporidium and Giardia lamblia, Salmonella, and Clostridium difficile, respectively. We are grateful to Carolien de Jager for her assistance in the preparation and the execution of the study. Finally the authors thank Wilfrid van Pelt for his help in calculating the incidence figures and for critically reading the manuscript. This study was financially supported by the Ministry of Health, Welfare and Sport (The Netherlands).
APPENDIX
Members of the GEops Working Group
D. Hoek1, S. Brandes1, J. Roelfsema1, B. van der Veer1, H. Vennema1, G. Wisselink2, E. van Zanten2, M. C. Scholts2, K. van Slochteren2, J. G. den Hollander3, W. D. H. Hendriks3, M. D. M. Bron-Prenen7, M. W. H. Wulf5, G. L. Homans-ter Keurs6, M. F. C. Beersma4, A. N. Reijm4, G. Pietersen4, P. B. F. Mensink4
(1 National Institute for Public Health (RIVM), Centre for Infectious Disease Control, Bilthoven; 2 Laboratory for Infectious Diseases, Department of Research & Development, Groningen; 3 Maasstad Hospital, Rotterdam; 4 Erasmus MC, Rotterdam; 5 Catharina Hospital, Eindhoven; 6 Gelderse Vallei Hospital, Ede; 7 Onze Lieve Vrouwe Gasthuis, Amsterdam)
DECLARATION OF INTEREST
None.







