Personality disorders are a category of mental illnesses characterised by persistent patterns of maladaptive behaviours and traits, with onset in adolescence or early adulthood. These disorders cause significant interpersonal difficulties, social and occupational dysfunction, and disturbance to others.Reference Tyrer, Reed and Crawford 1 Although dimensional models, which conceptualise personality disorders as maladaptive extremes of personality spectra, have been proposed, the categorical diagnostic criteria laid out in the ICD-10 and DSM-5 are most commonly applied in clinical and research settings.
Personality disorders are relatively common. Epidemiological data suggest that approximately 1 in 10 individuals has a diagnosable personality disorder.Reference Lenzenweger 2 Rates are higher in clinical settings, with approximately 25% of primary care patients and 50% of psychiatric out-patients meeting criteria for one or more personality disorders.Reference Moran 3 In studies of healthcare-related settings, more females than males present with personality disorders; however, this trend is not observed in community samples where personality disorders are found to be as, or more, common in men.Reference Tyrer, Reed and Crawford 1
When compared with other mental health conditions, treatment-seeking individuals with personality disorders have more extensive involvement with mental healthcare services, more frequent in-patient hospitalisations, more contact with out-patient clinics and more involvement in nearly all modalities of psychotherapeutic, psychopharmacological, and psychosocial interventions.Reference Bender, Dolan, Skodol, Sanislow, Dyck and McGlashan 4 Individuals with personality disorders have been associated with high frequency utilisation of emergency departments,Reference Chang, Weiss, Orav and Rauch 5 – Reference Schmoll, Boyer, Henry and Belzeaux 9 and recurrent use of emergency room psychiatric services.Reference Richard-Lepouriel, Weber, Baertschi, DiGiorigio, Sarasin and Canuto 10 A recent Canadian study found that individuals who were frequent emergency department presenters had an increased odds of having a primary or comorbid personality disorder diagnosis and that 87% of individuals with antisocial personality disorder or borderline personality disorder (BPD) presented five or more times in one year.Reference Vandyk, VanDenKerkhof, Graham and Harrison 11
Stigma further complicates the interaction between the healthcare system and individuals with personality disorders. Recent evidence suggests that, among mental health patients, those with personality disorders are the most severely stigmatisedReference Catthoor, Schrijvers, Hutsebaut, Feenstra and Sabbe 12 and that mental health professionals such as psychiatric nurses and psychiatrists have negative attitudes towards, and less empathy for, individuals with personality disorders, and particularly with BPD.Reference Bodner, Cohen-Fridel, Mashiah, Segal, Grinshphoon and Fischel 13 , Reference Sansone and Sansone 14 Provider stigma can have deleterious effects on the quality and accessibility of care for this population.Reference Lawn and Mcmahon 15 , Reference Sheehan, Nieweglowski and Corrigan 16
Although the link between a personality disorder diagnosis and high utilisation of emergency psychiatry services is well established, little else is known with regard to how personality-disorder-related presentations differ as compared with other mental health presentations in the emergency department. The aim of this study was to investigate whether factors such as mode of arrival, time and season of arrival, length of stay (LOS) and ultimate disposition decisions differ between individuals identified as having personality disorders versus individuals with other mental-health-related problems.
Based on clinical experience, we postulated the following: that individuals identified as having a personality disorder would be more likely to arrive outside the regular working hours of 09.00 to 17.00; that they would be more likely to be brought to hospital by police; and that they would be more likely to be discharged rather than admitted. We also postulated that those diagnosed with personality disorders would be younger, because prevalence of personality disorder has been found to decrease with age.Reference Balsis, Gleason and Woods 17 Finally, we hypothesised that individuals with personality disorders would have more frequent emergency department presentations and were more likely to be female.Reference Tyrer, Reed and Crawford 1
The ability to identify factors associated with emergency department presentations by individuals with personality-disorder-related diagnoses could result in improved crisis management and emergency psychiatry services for these individuals.
Method
This is a retrospective study of all mental-health-related emergency department visits that occurred between 1 January and 31 December 2015 at the Kingston General Hospital. The Kingston General Hospital is a 440-bed, university-affiliated, tertiary care hospital in Southeastern Ontario, Canada, and serves a catchment area of approximately 500 000 residents. 18 Prior to commencement, this study underwent review for ethical compliance by the Queen's University Health Sciences and Affiliated Teaching Hospitals Research Ethics Board.
Individuals were included if their primary diagnosis on discharge from the emergency department was a psychiatric diagnosis. Diagnoses were coded according to the World Health Organization ICD-10 codes. Our study compared individuals diagnosed with personality disorders with those with all other psychiatric diagnoses (see Table 1 for included diagnoses).
Table 1 Psychiatric diagnosis included in the study

| Diagnosis cluster | ICD-10 codes |
|---|---|
| Personality disorder diagnosis | |
| Dissocial personality disorder | F60.2 |
| Emotionally unstable personality disorder | F60.3 |
| Accentuation of personality traits | Z73.1 |
| Other personality disorders: | |
| i) Paranoid personality disorder | F60.0 |
| ii) Schizoid personality disorder | F60.1 |
| iii) Histrionic personality disorder | F60.4 |
| iv) Anankastic personality disorder | F60.5 |
| v) Anxious (avoidant) personality disorder | F60.6 |
| vi) Other specific personality disorders | F60.8 |
| vii) Personality disorder, unspecified | F60.9 |
| viii) Mixed and other personality disorders | F61 |
| Other psychiatric diagnoses | |
| Organic, including symptomatic, mental disorders | F00–F09 |
| Mental and behavioural disorders because of psychoactive substance use | F10–F19 |
| Schizophrenia, schizotypal and delusional disorders | F20–F29 |
| Mood (affective) disorders | F30–F39 |
| Neurotic, stress-related and somatoform disorders | F40–F48 |
| Behavioural syndromes associated with physiological disturbances and physical factors | F50–F59 |
| Mental retardation | F70–F79 |
| Disorders of psychological development | F80–F89 |
| Behavioural and emotional disorders with onset usually occurring in childhood and adolescence | F90–F98 |
| Unspecified mental disorder | F99–F99 |
Individuals with personality disorders were further sub-grouped into four personality disorder types: (1) accentuation of personality traits; (2) emotionally unstable personality disorder; (3) dissocial personality disorder; and (4) ‘other’ personality disorders, which included paranoid, schizoid, histrionic, anankastic, anxious (avoidant), dependent, other, unspecified and mixed personality disorders.
Participant age was grouped into four categories: adolescent (12–17), young adult (18–24), adult (25–65) and senior (65+). Season of presentation was divided into Fall (September–November), Spring (March–May), Summer (June–August) and Winter (December–February). Time of presentation was coded as morning (06.01 h to 12.00 h), afternoon (12.01 h to 18.00 h), evening (18.01 h to 24.00 h) or night-time (24.01 h to 06.00 h). Information regarding LOS in the emergency departments, gender, mode of arrival (walk-in, ambulance, police, combination of ambulance services or other) and disposition/discharge arrangements (discharge home, admission to hospital, left against medical advice/left without being seen, transfer to clinic and death after arrival) was also collected.
Data were analysed using SPSS v24. Data were described using frequencies, percentages, means and standard deviations. Relationships between all other psychiatric diagnoses and all personality disorder diagnoses were assessed using Mann–Whitney U (age groups, LOS and frequency of visits) and chi-square (gender, mode of arrival, time of presentation, season and discharge disposition) analyses.
Comparisons between the different personality subgroup disorders were assessed using chi-square tests (gender, mode of arrival, time of presentation, season and discharge disposition) with post hoc testing using adjusted standardised residuals and Kruskal–Wallis H tests (age groups, LOS and frequency of visits) with Bonferroni adjustments. Missing data were treated as missing and statistical significance was set at P<0.05.
Results
The final data set consisted of 5626 mental-health-related emergency department visits (336 for personality disorder presentation and 5290 for all other mental health presentations).
Of the 336 visits for personality disorder presentations, there were a total of 238 unique individuals who made one or more visits during the study period and a total of 3820 unique individuals who presented with another mental health presentation. The personality disorders visit group consisted predominantly of individuals presenting with accentuation of personality traits (39%) and emotionally unstable personality disorder (40%).
Personality disorder diagnosis versus all other psychiatric diagnoses
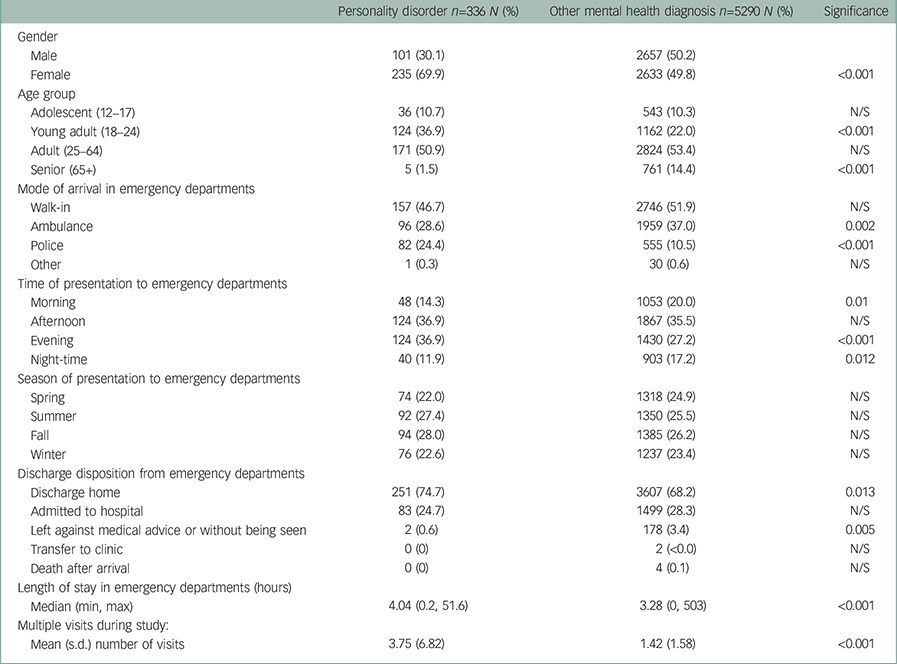
Table 2 shows the demographic information and the statistically significant differences between emergency department visits by individuals with any personality disorder diagnosis and those with any other psychiatric diagnosis.
Table 2 Demographics and analysis of differences in emergency department presentations between individuals with personality disorders versus all other psychiatric diagnoses
| Personality disorder n=336 N (%) | Other mental health diagnosis n=5290 N (%) | Significance | |
|---|---|---|---|
| Gender | |||
| Male | 101 (30.1) | 2657 (50.2) | |
| Female | 235 (69.9) | 2633 (49.8) | <0.001 |
| Age group | |||
| Adolescent (12–17) | 36 (10.7) | 543 (10.3) | N/S |
| Young adult (18–24) | 124 (36.9) | 1162 (22.0) | <0.001 |
| Adult (25–64) | 171 (50.9) | 2824 (53.4) | N/S |
| Senior (65+) | 5 (1.5) | 761 (14.4) | <0.001 |
| Mode of arrival in emergency departments | |||
| Walk-in | 157 (46.7) | 2746 (51.9) | N/S |
| Ambulance | 96 (28.6) | 1959 (37.0) | 0.002 |
| Police | 82 (24.4) | 555 (10.5) | <0.001 |
| Other | 1 (0.3) | 30 (0.6) | N/S |
| Time of presentation to emergency departments | |||
| Morning | 48 (14.3) | 1053 (20.0) | 0.01 |
| Afternoon | 124 (36.9) | 1867 (35.5) | N/S |
| Evening | 124 (36.9) | 1430 (27.2) | <0.001 |
| Night-time | 40 (11.9) | 903 (17.2) | 0.012 |
| Season of presentation to emergency departments | |||
| Spring | 74 (22.0) | 1318 (24.9) | N/S |
| Summer | 92 (27.4) | 1350 (25.5) | N/S |
| Fall | 94 (28.0) | 1385 (26.2) | N/S |
| Winter | 76 (22.6) | 1237 (23.4) | N/S |
| Discharge disposition from emergency departments | |||
| Discharge home | 251 (74.7) | 3607 (68.2) | 0.013 |
| Admitted to hospital | 83 (24.7) | 1499 (28.3) | N/S |
| Left against medical advice or without being seen | 2 (0.6) | 178 (3.4) | 0.005 |
| Transfer to clinic | 0 (0) | 2 (<0.0) | N/S |
| Death after arrival | 0 (0) | 4 (0.1) | N/S |
| Length of stay in emergency departments (hours) | |||
| Median (min, max) | 4.04 (0.2, 51.6) | 3.28 (0, 503) | <0.001 |
| Multiple visits during study: | |||
| Mean (s.d.) number of visits | 3.75 (6.82) | 1.42 (1.58) | <0.001 |
Individuals with a personality disorder diagnosis were statistically significantly more likely to be female aged between 18 and 24, more likely to be brought in by the police and less likely to be brought in by ambulance. They are also more likely to arrive between 18.00 h and 24.00 h and to be discharged home. Individuals presenting with a personality disorder diagnosis also have a significantly longer median LOS in the emergency departments and make significantly more repeat visits.
Differences between personality disorder subgroups
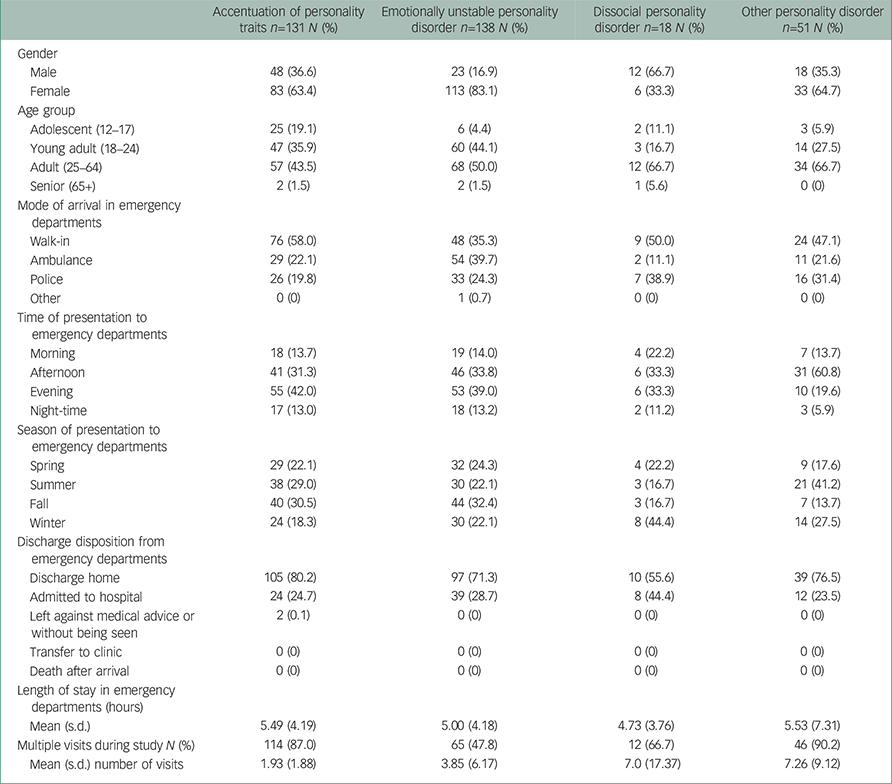
Table 3 shows the demographic information regarding the personality disorder subgroups.
Table 3 Demographics of the four personality disorder subgroups
| Accentuation of personality traits n=131 N (%) | Emotionally unstable personality disorder n=138 N (%) | Dissocial personality disorder n=18 N (%) | Other personality disorder n=51 N (%) | |
|---|---|---|---|---|
| Gender | ||||
| Male | 48 (36.6) | 23 (16.9) | 12 (66.7) | 18 (35.3) |
| Female | 83 (63.4) | 113 (83.1) | 6 (33.3) | 33 (64.7) |
| Age group | ||||
| Adolescent (12–17) | 25 (19.1) | 6 (4.4) | 2 (11.1) | 3 (5.9) |
| Young adult (18–24) | 47 (35.9) | 60 (44.1) | 3 (16.7) | 14 (27.5) |
| Adult (25–64) | 57 (43.5) | 68 (50.0) | 12 (66.7) | 34 (66.7) |
| Senior (65+) | 2 (1.5) | 2 (1.5) | 1 (5.6) | 0 (0) |
| Mode of arrival in emergency departments | ||||
| Walk-in | 76 (58.0) | 48 (35.3) | 9 (50.0) | 24 (47.1) |
| Ambulance | 29 (22.1) | 54 (39.7) | 2 (11.1) | 11 (21.6) |
| Police | 26 (19.8) | 33 (24.3) | 7 (38.9) | 16 (31.4) |
| Other | 0 (0) | 1 (0.7) | 0 (0) | 0 (0) |
| Time of presentation to emergency departments | ||||
| Morning | 18 (13.7) | 19 (14.0) | 4 (22.2) | 7 (13.7) |
| Afternoon | 41 (31.3) | 46 (33.8) | 6 (33.3) | 31 (60.8) |
| Evening | 55 (42.0) | 53 (39.0) | 6 (33.3) | 10 (19.6) |
| Night-time | 17 (13.0) | 18 (13.2) | 2 (11.2) | 3 (5.9) |
| Season of presentation to emergency departments | ||||
| Spring | 29 (22.1) | 32 (24.3) | 4 (22.2) | 9 (17.6) |
| Summer | 38 (29.0) | 30 (22.1) | 3 (16.7) | 21 (41.2) |
| Fall | 40 (30.5) | 44 (32.4) | 3 (16.7) | 7 (13.7) |
| Winter | 24 (18.3) | 30 (22.1) | 8 (44.4) | 14 (27.5) |
| Discharge disposition from emergency departments | ||||
| Discharge home | 105 (80.2) | 97 (71.3) | 10 (55.6) | 39 (76.5) |
| Admitted to hospital | 24 (24.7) | 39 (28.7) | 8 (44.4) | 12 (23.5) |
| Left against medical advice or without being seen | 2 (0.1) | 0 (0) | 0 (0) | 0 (0) |
| Transfer to clinic | 0 (0) | 0 (0) | 0 (0) | 0 (0) |
| Death after arrival | 0 (0) | 0 (0) | 0 (0) | 0 (0) |
| Length of stay in emergency departments (hours) | ||||
| Mean (s.d.) | 5.49 (4.19) | 5.00 (4.18) | 4.73 (3.76) | 5.53 (7.31) |
| Multiple visits during study N (%) | 114 (87.0) | 65 (47.8) | 12 (66.7) | 46 (90.2) |
| Mean (s.d.) number of visits | 1.93 (1.88) | 3.85 (6.17) | 7.0 (17.37) | 7.26 (9.12) |
Gender
There were significantly more female emergency department visits for those presenting with emotionally unstable personality disorder as compared with all other personality disorder diagnoses (χ2(3)= 26.02, P<0.001).
Age groups
There were statistically significant differences in the adolescent age group between accentuation of personality traits and emotionally unstable personality disorder (P=0.001). Significant differences were also identified among young adults between all groups χ2(3)=8.197, P=0.042.
Mode of arrival
Significantly more individuals with accentuation of personality traits compared with those with emotionally unstable personality disorder (χ2(3)=13.927, P=0.003) were walk-ins to the emergency departments. There were significantly more individuals with an emotionally unstable personality disorder compared with accentuation of personality traits visits who arrived by ambulance (χ2(3)=14.833, P<0.002).
Time of presentation
There were significantly more visits with the diagnosis of ‘Other’ compared with those with accentuation of personality traits and emotionally unstable personality disorder in the afternoons (χ2(3)=14.911, P=0.002). Furthermore, there were significantly more emergency department visits with accentuation of personality traits compared with those with a diagnosis of ‘Other’ during the evenings (χ2(3)=8.353, P=0.039).
Frequency of emergency department visits
Statistically significantly differences in frequency of emergency department visits during the 1-year study period were identified between ‘Other’ (mean=7.26 visits) and accentuation of personality traits (mean=1.93 visits), and between ‘Other’ and emotionally unstable personality disorder (mean=3.85 visits) (χ2(3)=42.17, P<0.001).
There were no statistically significant differences found in relation to LOS, season of presentation or disposition/discharge arrangements across personality disorder diagnosis categories.
Discussion
Although a number of studies have examined the demographic factors associated with individuals with psychiatric diagnoses who present frequently in the emergency department setting,Reference Richard-Lepouriel, Weber, Baertschi, DiGiorigio, Sarasin and Canuto 10 , Reference Lim 19 this study examined factors associated with personality-disorder-related presentations as compared with other psychiatric diagnoses.
Findings regarding increased frequency of emergency department presentation, increased likelihood of recurrent emergency department visits, and age and gender of individuals with personality disorders presenting to the emergency departments were consistent with previously published studies.Reference Tyrer, Reed and Crawford 1 , Reference Chang, Weiss, Orav and Rauch 5 – Reference Vandyk, VanDenKerkhof, Graham and Harrison 11 Surprisingly, only 6% of mental-health-related presentations in the emergency departments involved individuals with a personality disorder diagnosis. Evidence suggests that personality disorder, in particular BPD, is ‘markedly under-diagnosed’.Reference Comtois and Carmel 20 A recent survey of psychiatrists practicing in the United States found that 57% had failed to disclose a diagnosis of BPD and 37% had failed to document a diagnosis of BPD at some point in their careers; the most common reasons for doing so were diagnostic uncertainty and concerns about stigma.Reference Sisti, Segal, Siegel, Johnson and Gunderson 21 It is possible that emergency department staff under-diagnose personality disorders for similar reasons. Another possibility is that emergency department staff might view the assessment and diagnosis of personality disorders as existing outside of their scope of practice.
Accentuation of personality traits
In this study, the ICD-10 code ‘accentuation of personality traits’ was the most common personality-disorder-related diagnosis assigned in the emergency department setting. Interestingly, this code is not related to personality disorders, per se, it is located under the ICD-10 heading: ‘Factors influencing health status and contact with health services’; subheading: ‘Problems related to life-management difficulty’. 22 The term is meant to be applied in cases in which ‘Type A behaviours’ such as ‘ambition, a need for high achievement, impatience, competitiveness, and a sense of urgency’ influence health status and contact with health services. 22 It seems unlikely that individuals exhibiting these ‘Type A behaviours’ would present acutely in an emergency department setting. A more likely explanation would be that emergency room staff erroneously apply this diagnostic code when personality disorder traits or personality disorder is suspected, but a formal diagnosis is not assigned. This represents an opportunity for inter-professional collaboration and education regarding the appropriate use of ICD-10 codes related to mental health.
Increased likelihood of presentation between 18.00 h and 24.00 h
Individuals presenting to the emergency departments in this study between 18.00 h and 24.00 h would have the following disadvantages compared with individuals presenting between, for example, 09.00 h and 17.00 h: (1) less access to social work/crisis support staff; (2) increased difficulty connecting to out-patient resources and community mental health teams outside clinic hours; and (3) logistical barriers to obtaining collateral information and to collaborating with community mental healthcare providers to assist with disposition planning.
It would be interesting to explore the reasons why personality disorder presentations were more likely to occur in the evening. Are interpersonal crises most likely to occur at this time? Do individuals feel less supported by community resources at night? Do they simply prefer to present at this time? It would be prudent to determine whether this finding is consistent in other emergency department settings, as this knowledge could assist in the development of personality-disorder-specific programming occurring outside regular clinic hours.
Personality-disorder-related presentations more likely to be brought to emergency departments by police
The increased likelihood of presenting to emergency departments with police is likely related to high rates of self-harm, para-suicidal behaviours, suicidal ideation and suicide attempts associated with BPD. Emotional dysregulation, impulsivity and anger are three core features of BPD that might also contribute to the higher likelihood of police involvement. This underscores the importance of liaison between emergency mental health services and police services.
Decreased likelihood of admission
The decreased likelihood of admission occurring with personality-disorder-related presentations may be related to the fact that acute hospitalisation has not been shown to be effective in individuals with BPD.Reference Paris 23 Both the American Psychiatric Association and the National Collaborating Centre for Mental Health (NICE) practice guidelines for the treatment of BPD suggest that hospitalisation is appropriate, as a last resort, to minimise harm for acutely suicidal individuals with BPD. 24 , 25
Strengths
This study examined a number of variables associated with personality-disorder-related presentations that have not been explored previously in the emergency department setting, thereby addressing gaps in knowledge regarding an important diagnostic group. The inclusion of a comparison group further strengthened the study design.
Limitations
In this study, diagnoses were assigned by emergency department staff, rather than by mental health personnel or using validated diagnostic tools. This may have affected diagnostic accuracy. Given the high prevalence of personality disorders, and the finding that individuals with personality disorders are high utilisers of emergency department services, we suspect that personality disorders were under-diagnosed in the comparison group and that this could have affected our results. As diagnostic coding was based on the main presenting diagnosis assigned by emergency department staff, it has not been possible to assess comorbidity between personality disorders and other psychiatric diagnosis on the basis of available data, which could be considered another limitation of the study.
Future areas of study/consideration
The findings that individuals with personality disorders are more likely to present to emergency departments outside regular clinic hours, and are more likely to be brought to emergency departments by police, warrant further study to clarify, confirm and explore these factors. Ensuring that well-trained support staff are available in the emergency departments at times when individuals with personality disorders are most likely to present may help to better address the needs of this important diagnostic group. The above findings can also be used to make a stronger case for out-of-hours availability of other evidence-based support services such as home-based treatment and crisis resolution teams, emergency mental health housing and post-discharge follow-up services, which can divert some of these emergency department presentations and potentially reduce the need for unnecessary hospital admission.
Treatment-seeking individuals with personality disorders are more likely to experience stigmaReference Sheehan, Nieweglowski and Corrigan 16 and may be further stigmatised in the emergency department setting, particularly if they are brought by police and present at times when there is limited access to mental health services. This could include more focus on educating out-of-hours emergency room staff on diagnosis and management of individuals with personality disorders including specific training on dialectical behaviour therapy and crisis management strategies. Personality-disorder-specific psychoeducation and anti-stigma programmes for front-line workers in the emergency department could potentially improve the quality of care that treatment-seeking individuals with personality disorder receive in this setting.







eLetters
No eLetters have been published for this article.