Emotions are central to an understanding of the human condition, but in many countries curricula for specialist psychiatric training pay limited attention to the study of emotion. This can leave clinicians without the skills required to deal with the shame, fear, anger, disgust and humiliation associated with many clinical presentations. The concepts of emotion (affect) regulation and emotion dysregulation are not included in the standard training for the assessment and management of psychiatric disorders. Neither is there inclusion of the critical role of the autonomic nervous system in dysregulated affective responses, as described in the ‘window of tolerance’ model of the psychophysiological effects of traumatic experience (Reference Ogden, Minton and PainOgden 2006). Combining strategies from that model with insights from the biopsychosocial model of borderline personality disorder (Reference LinehanLinehan 1993) and other approaches (Reference SchwartzSchwartz 1995; Reference GreenbergGreenberg 2002; Reference FayFay 2007; Reference GermerGermer 2009; Reference Hanson and MendiusHanson 2009) allows the construction of a toolbox (presented later in this article) that may give the practising psychiatrist some useful ways of assessing and assisting patients with clinical presentations that do not fit within the standard nosological boundaries (Box 1).
BOX 1 Psychiatric disorders that may be associated with emotion dysregulation
-
• Post-traumatic stress disorder
-
• Borderline personality disorder
-
• Dissociative disorders and other complex trauma-related disorders
-
• Substance use disorders
-
• Some anxiety (e.g. generalised anxiety disorder) and dysthymic disorders
Background
The ability to regulate emotional states is a fundamental task of early life best developed within a secure attachment to an attuned caregiver in a stimulating and nourishing environment. However, it may be prevented from progressing to an ideal modulatory level by many interpersonal or environmental factors. The regulatory capacity may also be challenged in later life by personal disaster or other overwhelming experience.
Emotion regulation is the modulation, rather than the elimination, of emotions, so that the information provided by the emotional responses can be used to guide goal-directed behaviour rather than precipitate inappropriate or impulsive behaviours (Reference Gratz and RoemerGratz 2004). There is now evidence that replacing parts of standard cognitive–behavioural therapy (CBT) with emotion regulation training may improve the outcome of the psychotherapeutic intervention (Reference Berking, Wupperman and ReichardtBerking 2008).
The autonomic nervous system and emotional responses
The window of tolerance
The autonomic arousal model of trauma responses is particularly useful in assessing whether a patient is operating within a state in which information can be processed and new learning can occur, the ‘window of tolerance’ between hyperarousal and hypoarousal (Reference SiegelSiegel 1999; Reference Ogden, Minton and PainOgden 2006).
Defence responses driven by the sympathetic nervous system, such as fight and flight, can give rise to a chronic high-activation (hyperarousal) state in which vigilance, flashbacks, nightmares, and feelings of terror and panic precipitate behavioural strategies such as substance misuse, self-harm and suicidal thinking to reduce desperation and distress.
In contrast, the parasympathetically mediated hypoarousal response can be reactivated and prolonged in a state of numbness and despair in which nothing matters and life has no purpose. In this state, suicide planning is much calmer and more matter of fact than the intense urge to self-destruction of the hyperaroused state.
The window of tolerance model is helpful to traumatised patients in explaining the rapid switches of emotional state, which can feel chaotic and uncontrollable, and in understanding the destructive behaviours that are driven by urges to escape the extremes of arousal. Preliminary evidence that basic emotions of fear, anger and sadness have different patterns of autonomic activation (Reference Rainville, Bechara and NaqviRainville 2006) has been confirmed in an exhaustive review of autonomic response specificity in emotion (Reference KreibigKreibig 2010).
Theoretically, increasing exposure to antidepressants in response to low mood and expressed suicidal thinking arising from the hypoaroused state could precipitate a hyperaroused state, in which agitation increases to the point at which it is replaced by dissociation or self-harming behaviour. The reported increase in self-harm on starting selective serotonin reuptake inhibitors (SSRIs) (Reference Donovan, Madeley and ClaytonDonovan 2000) may be secondary to their use in complex trauma conditions assessed and treated as major depressive episodes. Comorbid depression is indeed common in complex trauma disorders, so antidepressants are often required. However, drug responses should be carefully monitored to avoid a slavish pursuit of more effective antidepressant therapy if the antidepressant is inducing hyperarousal. Reference Gunnell, Saperia and AshbyGunnell et al (2005) investigated an association between initiation of SSRIs and increased rates of suicide and self-harm, concluding that clinicians should warn patients of the possible risk of suicidal behaviour and monitor them closely in the early stages of treatment.
The polyvagal theory
Parasympathetic responses to trauma are thought to be mediated by components of the polyvagal system. Reference PorgesPorges (2001) argues that primitive organisms have an active sympathetic response to danger, which is only slowly turned off by gradual metabolism of adrenaline. Less primitive organisms have a dorsal vagal system which can counteract sympathetic activation by slowing the heart rate and respiratory rate. Higher animals, including humans, have a developed ventral vagal system which permits rapid adjustment of arousal level and emotional experience, for example during complex interpersonal interactions. The control of this ventral vagal system is dependent on midline structures of the prefrontal cortex (Reference Nagai, Critchley and FeatherstoneNagai 2004; Reference Tang, Ma and FanTang 2009).
Categories of emotion and their basic neurobiology
Emotion categories
Reference PankseppPanksepp (1998, Reference Panksepp, Lewis and Haviland-Jones2000, Reference Panksepp2011) divides emotions into three categories (Table 1):
TABLE 1 Categories of emotion according to Reference PankseppPanksepp (1998, Reference Panksepp, Lewis and Haviland-Jones2000, Reference Panksepp2011)

-
• category I – reflexive affects;
-
• category II – basic emotions that involve a set of brain circuits linking midline cortical areas with periaqueductal gray and hypothalamic areas;
-
• category III – higher sentiments that have become possible with the evolutionary development of the forebrain and often build on the brain structures available for the more prototypical emotions.
The appetitive motivation-seeking system (category II), which is based in the mesolimbic dopamine system, is fundamentally for searching for safety (Reference Alcaro, Huber and PankseppAlcaro 2007). Although associated with positive affect when the environment is secure, it can be associated with fearfulness when the environment is hostile (Reference Reynolds and BerridgeReynolds 2008).
Shame, although considered to be recently evolved, is evident in infants when they perceive themselves to have failed at certain tasks (Reference NathansonNathanson 1992) and is therefore considered by some authorities to be a basic emotion. However, it is not known whether the relevant circuitry includes cortical links with the periaqueductal gray area. Shame attenuates positive affects such as excitement and enjoyment, not in the way that disgust switches off hunger, but when there is still the urge towards the source of the interest or interaction. It is the change from the high sympathetic tone to the onset of the parasympathetic state that is associated with shame. Humiliation combines shame-inducing interactions with damage to the continuing relationship because the hurt is not repaired (Reference SiegelSiegel 1999).
Von Economo neurons, or spindle neurons, are specialised cells present in great apes but to a much lesser extent than in humans (Reference Watson, Jones and AllmanWatson 2006). They occur in the anterior cingulate cortex and the anterior insular cortex, the areas receptive to interoceptive feedback from the body (Reference CraigCraig 2003). Their rapid processing makes them important in the assessment of complex social situations (category III).
Basic emotions
Electrical or chemical stimulation of distinct brain regions has given information about discrete emotions (Reference PankseppPanksepp 2011), and the basic systems for fear, rage, and separation distress are clinically important. Physical pain is a sensory affect which can have a profound impact on well-being. Pain stored in emotional memory systems can be a long-term result of trauma. Also frequently encountered clinically are shame and guilt.
Basic emotions are crucial to survival when the organism is under threat. It is important to be able to use anger to drive a fight response, or fear to promote flight or freeze responses. But it is equally necessary to be able to attach to a protector, or to submit to a greater power in an unbalanced contest, if the subcortical fear response fails to identify a more effective escape route. Enforced submission may have long-term emotional consequences when the repeatedly conquered self can acquire negative valence, with feelings of rejection, devaluation and worthlessness, as is often the case following severe childhood abuse. Just as the loss of the capacity for choice and control gives helplessness, the experience of threat to future survival and well-being precipitates hopelessness: this defeat stress is a useful animal model for depression (Reference Berton, McClung and DiLeoneBerton 2006). Repeated experiences of submission fix the momentary hopelessness and helplessness into the long-term depressive outlook (Reference Corrigan, Fisher and NuttCorrigan 2011). Although painful physical stressors may recruit similar mechanisms of submission to inescapable adversity, including despairing resignation, the social defeat model relates specifically to defeat by a more aggressive opponent of the same species and is more likely to parallel human experiences of chronic bullying or abuse.
Pessimism and lack of motivation may confer an advantage in situations in which goal-directed effort will not be successful and may even be dangerous or damaging (Reference NesseNesse 2000). It has been proposed that the neurobiological origins of the susceptibility to depression lie in the capacity for shutting down unending separation distress in infants for whom continuing protest is dangerously energy-consuming. Dynorphins acting on kappa opioid systems and neuropeptides such as cholecystokinin may alter the valence of mesolimbic dopamine transmission from the ventral tegmental area to the nucleus accumbens, translating separation distress from acute protest to chronic despair (Reference Watt and PankseppWatt 2009).
Higher emotions
Reference Immordino-Yang, McColl and DamasioImmordino-Yang et al (2009) investigated the neural correlates of the higher emotions of admiration for virtue and for skill, and compassion for physical and for social/psychological pain. These higher emotions recruited the same neural pathways as the basic emotions, involving the brainstem, hypothalamus, anterior cingulate and anterior insula regions. Interestingly, however, there was also activation in the posterior medial cortices of the brain, which are involved with enhancing self-awareness.
Positive emotions, the autonomic nervous system and the window of tolerance
More basic positive emotions can be differentiated into appetitive and consummatory (Reference Burgdoff and PankseppBurgdoff 2006). Dopamine activity in the nucleus accumbens is important for the appetitive positive affect associated with reward-seeking in animal models and is thought to underlie joy and laughter in humans (Reference Burgdoff and PankseppBurgdoff 2006). Consummatory positive affect derived from sensory pleasures involves the opiate and γ-aminobutyric acid (GABA) systems in the ventral striatum and orbital prefrontal cortex (Reference Burgdoff and PankseppBurgdoff 2006), and the parabrachial nucleus in the brainstem (Reference Berridge and KringelbachBerridge 2008).
In a process called reconsolidation, we can modify unpleasant, distressing and traumatic memories using complex emotions such as compassion (Reference Hanson and MendiusHanson 2009), which have significant cortical components (Reference Immordino-Yang, McColl and DamasioImmordino-Yang 2009).
Activation of the sympathetic nervous system/hypothalamus–pituitary–adrenal axis (SNS/HPAA) for good reason – such as becoming passionate and enthusiastic, handling emergencies or being forceful for a good cause – has its place in life. However, non-stop SNS/HPAA activation is unnatural, exhausting and potentially dangerous.
The parasympathetic nervous system conserves energy in our body and is responsible for ongoing, steady-state activity. In contrast to the ‘fight-or-flight’ effect of the sympathetic nervous system, the parasympathetic system produces a feeling of relaxation, followed by a sense of contentment.
The sympathetic and parasympathetic nervous systems evolved hand in hand in order to keep animals – including humans – alive in potentially dangerous environments. The combination of aliveness and centredness is the essence of the peak performance zone recognised by athletes, artists, lovers and meditators. Happiness, love and wisdom are furthered not by shutting down the sympathetic system, but through the sympathetic and parasympathetic systems working in harmony together, keeping the whole autonomic nervous system in an optimal state of balance (Reference Hanson and MendiusHanson 2009) within the window of tolerance. Extremes of arousal, outside the window of tolerance are then experienced as hyperarousal and hypoarousal.
Case vignette 1 illustrates the clinical application of the window of tolerance model of emotion dysregulation resulting from early trauma.
Case vignette 1: Borderline personality disorder and the window of tolerance
A 30-year-old woman with a history of repeated self-harm, alcohol misuse and depression is troubled by an intense need to harm herself. Sometimes this can help to clear a feeling of explosive tension inside her, which builds at times to the point of becoming unbearable. At other times, she feels a dead numbness. She says that this feeling is not distressing because she has gone beyond distress, but it is so unpleasant in a different way that she cuts herself and watches the blood flow to give her an intense feeling of being alive and present. Unfortunately, the relief she gains from self-harm is short-lived.
The patient agrees that she does not have the mental stability for any detailed discussion of her trauma history. However, she finds it less distressing to understand her present-day emotional states in terms of persisting body responses to traumatic memories and triggers.
When asked about the intense and unbearable tension she experiences, she is able to identify that her response is extreme (outside the window of tolerance). At this point it is helpful to provide a simple explanation to help the patient understand her extreme response. For example, ‘It is probable that at some point in your past you were in a situation in which the emotions accompanying your defence response – such as fear and anger – were trapped inside with no possibility of release. You had no one to go to because you had no secure attachment person who would have helped you to regulate the distress. You were unable to process the emotions accompanying the defence responses in the usual way and they were stored in your body memory.’
It is helpful to bring the patient’s attention to her body sensations: ‘What happens in your body before you cut? Tension, fast heart rate, fast breathing? OK, so that is the high arousal state in which the sympathetic nervous system is in overdrive and not being dampened by your parasympathetic brake. You have found before that alcohol, illicit substances and self-harm all help to reduce this tension. Perhaps there are other ways of self-soothing that would be appropriate for the high-activation state. Anything that would slow the breathing, reduce the heart rate and the muscle tension. Applying mindfulnessFootnote † to hobbies or when out walking – focusing moment by moment on the task without judgement – or breathing slowly with soothing statements, or seeking out someone supportive to speak to. Let’s work on expanding the list.’
Similarly, the woman’s feelings of dead numbness can be explained: ‘When you’re in the low-arousal state, you may need quite different strategies. That state is thought to be a parasympathetic-dominant state, with lower pulse rate and blood pressure. It may have arisen from a state of being frozen with fear and shame. Sometimes, the muscle tension drops when the sympathetic system is turned down by the parasympathetic brake and there are various states of defensive immobilisation which may be stored in your body’s memories. You’re telling me that then you feel numb, so dead that you might as well be dead, nothing matters. How does your body feel then? As if it doesn’t exist? In that condition, calming may be less effective than gentle activation. This can be through curiosity, interest and enjoyment or through gentle physical activity. For example, making small adjustments to your posture, a walk in the rain, going home for a shower, watching an interesting or amusing DVD. That state of belief that nothing matters was doubtless important to you at some time of extreme stress and it helped you to cope and survive, but now it’s not so helpful. Could you remind yourself that it’s an old response which has arisen in the present?
‘Sometimes you describe rapid cycling between the high and low activation states. Something triggers intense anger, which builds until you cut off and become numb and detached. Then the rage erupts again. You can go from being suicidal because of the intensely distressing tension to being suicidal because you have no feelings and nothing matters. If you stay with the feelings and body sensations and find out when the switch occurs for both changes of arousal, do you think you might get some more control? Could you try that? I’d be really interested to hear how it goes in our next session.’
Emotion regulation
The prefrontal cortex, anterior cingulate cortex and insula are cortical regions that handle abstract reasoning, planning and the ‘executive functions’ of self-monitoring, organisation and impulse control. These regions, through their connections with the amygdala, hypothalamus and periaqueductal gray area, lay the basis for the cognitive regulation of emotion (Reference Ochsner, Bunge and GrossOchsner 2002; Reference Goldin, McRae and RamelGoldin 2008).
The capacity to cope with distressing memories is promoted by the left prefrontal cortex through practising mindful acceptance of passing mental events. Negative focus on specific emotions leads to depressive rumination facilitated by activations in the subgenual anterior cingulate cortex (Reference Kross, Davidson and WeberKross 2009).
Roughly 50% of people with post-traumatic stress disorder (PTSD) do not feel better after CBT, and Reference Bryant, Felmingham and KempBryant et al (2008) have suggested that this is because they have higher levels of baseline fear. They found that higher activity in the networks involving the ventral anterior cingulate cortex and bilateral amygdala in response to fearful faces was associated with a poor response to CBT. Furthermore, cortical areas such as Brodmann area 25 in the subgenual anterior cingulate cortex have connections with areas of the hypothalamus and periaqueductal gray area that are crucial for fight and flight defence responses (Reference Price, Zald and RauchPrice 2006).
In general, the lower levels of the brain such as the brainstem, thalamus and hypothalamus stimulate and fuel the higher levels. The higher levels of the brain serve to calm and guide the lower levels. This means that the lower brain areas exert more direct control over the body, while the higher cortical areas exhibit greater neuroplasticity and can reshape their own neural network through mental activity and learning from experience (Reference Hanson and MendiusHanson 2009).
Intense negative emotions such as fear and rage lessen cortical control and this jeopardises neuroplasticity and the ability to adapt and learn from experience. Emotion regulation has a vital role in enabling meaningful cognitive restructuring and producing effective behavioural change.
Emotion dysregulation
Some psychiatric conditions, especially conditions related to trauma, are characterised by extremes of emotional responses which are difficult to regulate. These extremes are termed emotion (sometimes ‘emotional’ or ‘affect’) dysregulation. In an effort to control their distress, patients who suffer from this type of emotion dysregulation may develop behaviours that are immediately effective but unhelpful in the long term (Box 2). Self-harm is one such behaviour. It gives instant relief but prevents the development of other regulation techniques. It also leads to disfiguring and scarring, which become an embarrassment to the sufferer.
BOX 2 Unhelpful behaviours that may be associated with emotion dysregulation
-
• Self-harm
-
• Unnecessary or impulsive risk-taking
-
• Drug misuse
-
• Compulsive cleaning
-
• Binge eating
Emotion dysregulation has been brought to prominence clinically in the treatment of chronic suicidal thinking with the development of dialectical behaviour therapy (DBT) by Marsha Reference LinehanLinehan (1993). Linehan’s biopsychosocial model of borderline personality disorder proposes that a multifactorial development of a failure to adequately regulate distress during early childhood is instrumental in the development of the clinical features of the disorder.Footnote ‡ The DBT modules on mindfulness, emotion regulation, distress tolerance and interpersonal effectiveness are designed to reverse some of these deficits.
There is experimental evidence of abnormal functioning of the vagal ‘brake’ on levels of arousal and emotional experience during social engagement in individuals diagnosed with borderline personality disorder (Reference Austin, Riniolo and PorgesAustin 2007). In addition, functional magnetic resonance imaging (Reference Koenigsberg, Fan and OchsnerKoenigsberg 2009) suggests altered amygdala activation in people with borderline personality disorder responding to negative social cues. A group of patients with the disorder and a group of healthy controls were shown pictures of people in situations of loss, grief, abuse or physical threat (negative social cues). Both groups had undergone the same training in distancing themselves by adopting the perspective of a detached observer. While the healthy controls displayed activation of the dorsal anterior cingulate cortex with distancing, this area became less active in the patients (Reference Koenigsberg, Fan and OchsnerKoenigsberg 2009). The significance of the evidence is that when people with borderline personality disorder protest that, despite training in cognitive restructuring, they still cannot think the way they are expected to, it is possibly because they have not only differences in emotion regulation circuits, but also atypical neural responses to techniques that work well in other people.
Basic developmental considerations of emotion regulation
The window of tolerance may be wide, when the individual is able to assimilate experiences of high arousal, such as excitement, joy and enthusiasm, and also of low arousal, such as calmness and relaxation. The window may be narrow, when any activation outwith a restricted band results in a failure to cope with the experience. Whether the window develops with sufficient width and flexibility to adapt to new experience or is established as narrow and constrained depends on critical maturation periods in an infant’s early life when the attachment relationships with the mother shape long-lasting features of personality development (Reference BowlbyBowlby 1969). A securely attached child develops a wide window of tolerance and is then able to cope with excitement, interest and activity, but also with quietness, calmness and conditions of reduced stimulation.
The orbitofrontal cortex
For the brain to develop normally, the infant must experience nurturance and affection. Reference SchoreSchore (1994) highlighted the role of emotion regulation in the emergence of a sense of a coherent self. He identified the orbitomedial prefrontal cortex as a major area in the control of the autonomic nervous system and in the generation of emotion. He posited that this region is optimally developed through a validating dyadic (mother–infant) interaction in infancy. This view is supported by imaging studies of ventral prefrontal areas during fluctuations of the autonomic system (e.g. Reference Nagai, Critchley and FeatherstoneNagai 2004), and by observation of the impact of emotional deprivation on these brain regions (e.g. Reference Chugani, Behen and MuzikChugani 2001).
Although the focus is mainly on the development of the orbitomedial prefrontal cortex for social and emotional behaviour, non-cortical structures active in the generation of emotional consciousness should not be ignored. These are the hypothalamus, colliculi and periaqueductal gray area (Reference MerkerMerker 2007), the parabrachial nucleus and the nucleus of the solitary tract (Reference DamasioDamasio 2010).
Attachment styles
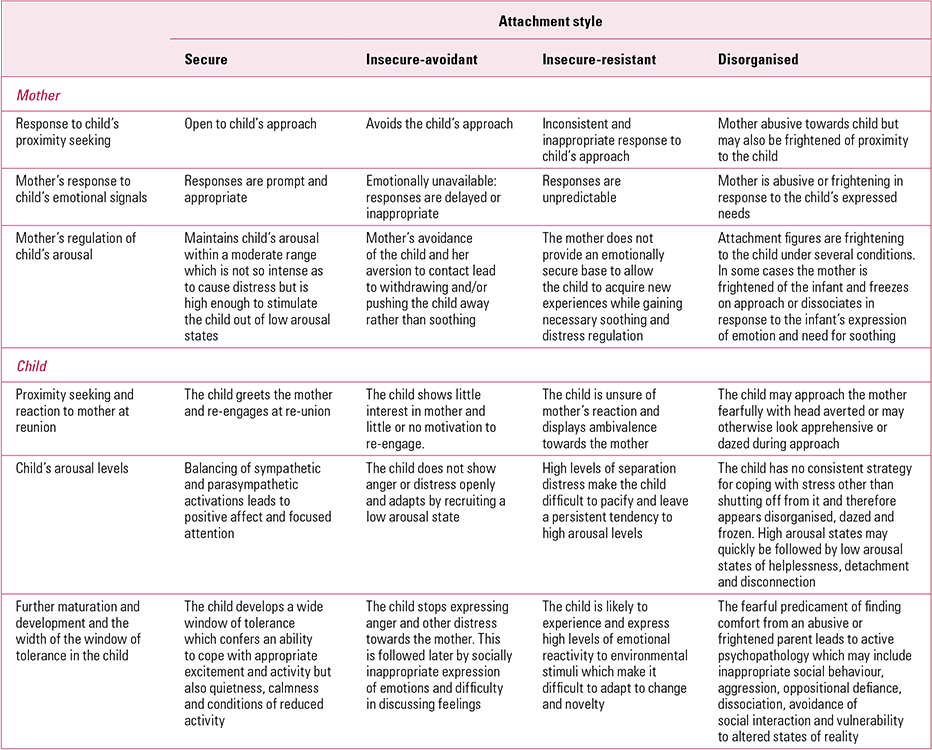
Developmental studies of individual differences in attachment, based on the observation of infants’ non-verbal behaviour towards their caregivers in the structured separation and reunion situation defined by Reference Ainsworth, Blehar and WatersAinsworth et al (1978)(Box 3), have repeatedly found three types of attachment style: one defined as secure and two designated insecure (avoidant and resistant). Some examples, constructed mainly from the work of Reference SchoreSchore (1994), of how the different attachment patterns can affect the window of tolerance, are given in Table 2.
TABLE 2 Examples of how the mother–child attachment and interaction styles can lead to different emotion regulation capacities
BOX 3 The ‘strange situation’
The child and their caregiver are taken into a room containing toys and a two-way mirror, and the child is allowed to explore while the caregiver remains uninvolved. At various points over the next 20 minutes, the child spends time in the room with the caregiver, with the caregiver and a stranger, with a stranger, and alone. An observer categorises the child’s behaviour in terms of:
-
• the amount of exploration (e.g. playing with new toys) during the test
-
• the child’s reactions to the departure of their caregiver
-
• their ‘stranger anxiety’ (when left alone with the stranger)
-
• their reunions with the caregiver
A third insecure group, with a disorganised/disoriented attachment pattern, was described by Reference Main, Solomon, Brazelton and YogmanMain & Solomon (1986). We outline it here only briefly, as it is implicated in more severe clinical manifestations of emotion dysregulation. The young human is required to attach to survive, and in the face of danger will seek a selected person for comfort and reassurance (Reference Hesse, Main, Abrams, Solomon and SiegelHesse 2003). If that caregiver is also an abuser of the child, the child is in the impossible situation of having to attach to the perpetrator of abuse, a conflict which is resolved by dissociation (Reference RossRoss 1997). The disorganised form of insecure attachment in a child is later associated with psychological problems in early adult life. Disorganised attachment may emerge indirectly in response to the frightened and distressed behaviour of a parent who was traumatised in childhood or directly through trauma to the child (Reference Hesse, Main, Abrams, Solomon and SiegelHesse 2003). As fear of the parent may lead to a disruption of normal capacity for attention and emotion (Reference Hesse, Main, Abrams, Solomon and SiegelHesse 2003), later problems with dissociation and emotion dysregulation would be expected in those with either a frightened or frightening parent.
Further developmental considerations
Protest and despair
Children who have experienced traumatic separations will respond to relatively short-lasting physical separation with anxiety, clinginess and anger on reuniting. If they are separated for longer periods, they will actively avoid the parent: the acutely distressed phase of protest converts to a phase of helplessness or despair (Reference BowlbyBowlby 1973). This may be a result of dynorphin or cholecystokinin effects on the mesolimbic dopamine system (Reference Watt and PankseppWatt 2009). Protest reactions involve agitation, distress vocalisations, crying, searching and an increased heart rate. In contrast, despair responses include social withdrawal, a facial expression of sadness and a decreased heart rate. This down-regulation of sympathetic overactivity by a parasympathetic-dominant state mirrors the peritraumatic changes described above in relation to the window of tolerance (Reference Ogden, Minton and PainOgden 2006).
An attuned bond between infant and mother can be disturbed even when they are not physically separated, if the mother is emotionally unavailable. These proximate separations can be psychologically equivalent to longer physical separations and lead to a loss of internal regulation during critical periods of maturation (Reference SchoreSchore 1994). When stress escalates beyond the child’s coping capacity and manifests as hyperaroused protest, there is a survival need for this state of high energy consumption to be transformed into hypoaroused despair, providing a neurobiological substrate for depressive states (Reference Watt and PankseppWatt 2009).
Resilience
According to Reference SiegelSiegel (1999), an infant’s behaviour at 1 year old in Ainsworth’s structured strange situation can be predicted with reasonable certainty before birth by the coherence of the mother’s narrative when asked about her own attachment history. Mothers who are secure and autonomous with respect to attachment are more likely to have infants who will display secure behaviour in an experimental strange situation than mothers who are dismissing or preoccupied.
Security of attachment is one of the factors that produce resilience to adverse events and it is seen in later life as a protective capacity for functional social relationships. By contrast, insecure attachment leaves the child more vulnerable to further invalidation, a term used by Reference LinehanLinehan (1993) to indicate a lack of supportive and consistent responses to the child’s expressions of emotion. Extreme forms of invalidation, such as sexual abuse, readily lead to problems of emotional regulation and a dysfunctional view of the self. The early failure to establish consistent and coherent emotional responses within the primary dyadic relationship, combined with the absence of an empathic protector to turn to for support at the time of major trauma, magnifies the impact of sexual abuse beyond the severe distress associated with the intrinsic pain, terror, hopelessness, helplessness and isolation.
It is more difficult to facilitate the reduction of distress and the development of positive emotions in an adult who has not had formative early experiences of joy and happiness, nor pride in achievement, and who has no ready access to feelings of compassion for the selfFootnote § in any stages of development.
Assessment of the capacity for emotion regulation
The Structured Interview for Disorders of Extreme Stress (SIDES; Reference Pelcovitz, van der Kolk and RothPelcovitz 1997) has questions designed to elicit problems in emotion regulation, alterations in attention or consciousness such as amnesia and dissociation, alterations in self-perception, alterations in relations with others, somatisation, and alterations in systems of meaning (SIDES is available from the Boston Trauma Center at www.traumacenter.org/products/instruments.php). Emotion dysregulation includes being very upset over small problems, having difficulty in self-soothing, having problems with the modulation of anger and aggressive behaviour, having self-destructive tendencies and suicidal thinking, having difficulty in modulating sexual thoughts and behaviours, and excessive risk-taking.
Six key areas should be examined in assessing whether emotion dysregulation in an adult might respond to treatment. These are:
-
• the security of the early attachment to the primary caregiver
-
• the spontaneous display of positive affect in early life and whether this was carefully modulated by the primary caregiver
-
• the resilience displayed in social interactions with peers
-
• the extent, nature and severity of trauma
-
• the capacity for self-soothing of distress, and the associated regulation of autonomic nervous system states of hyper- and hypoarousal
-
• the capacity to make use of opportunities for interactive regulation.
Early attachments, capacity for positive affect, and resilience
The status of the security of the early attachment can be explored in the clinical history with specific questions about the empathic presence of the primary caregiver, the caregiver’s responses to expressions of emotional distress, and reactions to separations from the caregiver in childhood. The Boston Trauma Centre’s Traumatic Antecedents Questionnaire looks at the caregiving practices experienced at different phases of the person’s life and can be adapted for clinical enquiry. The main areas for which it produces scores are listed in Box 4.
BOX 4 Traumatic Antecedents Questionnaire
Childhood experiences:
-
• Competence (being good at something and having friends)
-
• Safety (feeling safe and having someone outside the family to confide in)
-
• Neglect (not having someone care about the child’s whereabouts)
-
• Separation (family and caregiver disruption through divorce or illness)
-
• Secrets (nobody knew what was really going on)
-
• Emotional abuse (the child being told that he/she is not good enough)
-
• Physical abuse
-
• Sexual abuse
-
• Witnessing (seeing physical or sexual violence)
-
• Other traumas (serious accident or illness or involvement in natural disaster)
-
• Alcohol and drugs (child or caregiver)
(Boston Trauma Center: www.traumacenter.org/products/instruments.php)
It can be difficult to get a history of affect in the first year of life, although some individuals will have been told by their parents about their infancy, perhaps that they were placid babies or that they cried all the time and could never be comforted. Such reports can give an idea of the person’s capacity for positive affect and can be important in setting out aims and expectations in treatment. Reported sociability with peers in the early years, availability of attachment to a non-traumatising and caring adult, and continuing access to supportive relationships in later life indicate resilience to adversity, which will counteract some of the negative impact of trauma.
Trauma history
Since the time of Pierre Janet, it has been widely accepted that safety and stabilisation precede trauma reprocessing and the subsequent integration of personality (Reference Van der Hart, Nijenhuis and Steelevan der Hart 2006). Therefore, the trauma history need not be detailed at an early stage of treatment. Nevertheless, it is helpful to have some idea of whether neglect was compounded by physical or sexual abuse, and whether sexual abuse was associated with violence, penetration and an unhelpful, condemnatory response from an adult who was approached for help. The history may also be incomplete if severe dissociation with amnesia has resulted from the early trauma. The Loewenstein interview for the assessment of dissociative disorders (Reference LoewensteinLoewenstein 1991) and the Dissociative Disorders Interview Schedule (DDIS), DSM-IV version (Reference RossRoss 1997), both have formats for collection of information about abuse.
Capacities for self-soothing and interactive regulation
Self-soothing is the ability to modulate distress without recourse to another person for comfort. An impaired capacity for self-soothing is usually seen clinically as behavioural dyscontrol or dissociation in response to overwhelming emotion. Behavioural strategies for coping with distress include self-harm and suicidal thinking, misuse of alcohol and illicit drugs, aggression towards others, reckless sexuality and other risk-taking activities. Information about these can be elicited during the clinical history-taking. Dissociative defences can be less obvious at interview and the Dissociative Experiences Scale (DES; Reference Bernstein and PutnamBernstein 1986) is a routinely useful screening instrument, although false-negative responses can mislead. Self-rating scales for the five key areas of amnesia, depersonalisation, derealisation, identity confusion and identity alteration are also available (Reference Steinberg and SchnallSteinberg 2001).
Screening questions might include (Reference Paulsen, Lanius, Shapiro and NortonPaulsen 2009):
-
• Do people ever tell you that you have said things that you cannot remember? (losing time)
-
• Do any parts of your body ever go numb? (somato-form dissociation)
-
• Do you ever have out-of-body experiences, such as looking at yourself from the ceiling? (depersonalisation).
‘Grounding’ is helping a person to return from a dissociated experience to full here-and-now awareness. The following vignette demonstrates grounding to counteract a dissociative flashback which leaves the patient disconnected from the present time and place.
Case vignette 2: Grounding
A 40-year-old woman, who has had numerous diagnoses, including schizophrenia, borderline personality disorder and bipolar affective illness, was admitted after an episode of self-harm in response to voices of past abusers telling her she was vile and worthless.
During the multidisciplinary review there is a noisy disturbance in the corridor outside the consulting room: she suddenly becomes mute, looks terrified and curls up into a ball. The trainee psychiatrist suggests intramuscular lorazepam and haloperidol, but the charge nurse is aware of the patient’s trauma history and the diagnostic confusion. The nurse suspects that the woman has a dissociative disorder and suggests a more conservative approach. On this assumption he begins to reassure her: ‘Can you hear me? Are you here? If you are here and you are hearing me, can you nod your head to let us know that you can hear me? That’s good. You still look quite far away, so I’m going to talk to you for a while to help you to come back more fully. You are safe here in this hospital. This is April 2011 and you are now 40 years old. The hands that are gripped together are adult hands. Your left hand has a wedding ring that André gave you when you got married 15 years ago. You are safe here now. Just notice your breathing and notice as it gets slower. Let your breathing slow: when it’s as fast as that, you’re more likely to stay cut off from the present. That’s good, let it become slower and you become more aware. Can you feel the hard floor underneath you?’
Approaches to treatment
In people who have been severely traumatised, it is often necessary to develop accessibility to cognitive techniques by first enhancing their ability to be mindfully aware of their emotional response, including its visceral and other somatic components.
Reference LinehanLinehan (1993) regards mindfulness as the core skill in her DBT training programme,Footnote ¶ as it permits greater distress tolerance, facilitates emotion regulation and provides strategies for enhanced interpersonal effectiveness. Awareness and cognitive techniques are supplemented by many sensory-soothing exercises to reduce the unpredictability of the autonomic nervous system’s hyperactivity. In DBT, the term ‘mindfulness’ is used both for concentration-focusing exercises and for non-judgemental, observational awareness. Focused-attention meditation practices may include techniques for maintaining awareness of the breath. Open awareness encourages continuity of non-judgemental awareness of whatever arises in consciousness: thoughts, images, sensations and feelings (Reference Hanson and MendiusHanson 2009).
Combining the approaches of Linehan, Greenberg and others (e.g. Reference SchwartzSchwartz 1995; Reference FayFay 2007) with clinical experience of reprocessing trauma memories using eye movement desensitisation and reprocessing (EMDR; Reference ShapiroShapiro 1995) and the autonomic arousal model used in sensorimotor psychotherapy (Reference Ogden, Minton and PainOgden 2006), we have created a ‘toolbox’ of ways to regulate distress (Table 3). This is a basic structure for an affect-oriented, cognitively aware and neurobiologically informed approach to clinical presentations of emotion dysregulation associated with a history of trauma, neglect and problems in early attachment relationships.
TABLE 3 Toolbox of ways to regulate distress

Conclusions
‘In emotional turmoil, the upward influences of subcortical emotional circuits on the higher reaches of the brain are stronger than top-down controls. Although humans can strengthen and empower the downward controls through emotional education and self-mastery, few can ride the whirlwind of unbridled emotions with great skill’
When emotional turmoil happens in early life, the top-down controls are deficient in regulating distress arising from later events. The resulting emotional dysregulation and associated unhelpful behaviours can present as psychiatric disorders which are difficult to manage because of their inherent variability and situation-dependence. An understanding of attachment theory, basic emotional processes and the autonomic nervous system ‘window of tolerance’ can assist psychiatrists in treating individuals who have difficulties with emotion dysregulation by adding a multifactorial perspective on aetiology and management.
MCQs
Select the single best option for each question stem
-
1 The following disorders are commonly associated with emotion dysregulation:
-
a major depressive disorder
-
b PTSD
-
c schizophrenia
-
d bipolar affective disorder
-
e seasonal affective disorder.
-
-
2 In assessing whether an emotionally dysregulated adult might benefit from treatment, the following are important:
-
a resilience displayed in social interactions with peers
-
b adherence to medication regimens
-
c the capacity to ignore distress
-
d ability to complete thought diaries
-
e the age of the patient.
-
-
3 A mental state outside the window of tolerance describes:
-
a the changes in mood associated with bipolar disorder
-
b the unhelpful thoughts produced when remembering incidents of social exclusion
-
c the autonomic arousal model of trauma responses
-
d a state of well-being between the rapid switches of mood in dysregulated patients
-
e the very narrow range of emotion in which new experiences can be tolerated.
-
-
4 In Panksepp’s categories of emotions, the higher sentiments (category III) include:
-
a compassion
-
b sadness
-
c joy
-
d pain
-
e fear.
-
-
5 Steps required to enable emotion regulation include:
-
a ignoring the emotion
-
b telling yourself you are stupid to feel this way
-
c trying to describe the feeling
-
d reminding yourself that to give in to your emotions is a sign of weakness
-
e considering that only logical thoughts can help.
-
MCQ answers

| 1 | b | 2 | a | 3 | c | 4 | a | 5 | c |








eLetters
No eLetters have been published for this article.